-
Original Article07-26-2024
Maternal deaths caused by eclampsia in Brazil: a descriptive study from 2000 to 2021
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo65
Abstract
Original ArticleMaternal deaths caused by eclampsia in Brazil: a descriptive study from 2000 to 2021
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo65
Views232See moreAbstract
Objective
Eclampsia is a hypertensive disorder that occurs during pregnancy and can lead to death. The literature has gaps by not providing comprehensive data on the epidemiology of the disease, restricting analysis to limited temporal intervals and geographical locations. This study aims to characterize the epidemiological profile of women who died from eclampsia in Brazil from 2000 to 2021.
Methods
The maternal mortality data were obtained from the Sistema de Informações sobre Mortalidade, with the following variables of interest selected: “Federative Unit,” “Year,” “Age Range,” “Race/Color,” and “Education Level.” The collection of the number of live births for data normalization was conducted in the Sistema de Informações sobre Nascidos Vivos. Statistical analyses were performed using GraphPad Prism, calculating odds ratio for variables and fixing number of deaths per 100,000 live births for calculating maternal mortality ratio (MMR).
Results
There was a downward trend in maternal mortality rate during the study period. Maranhão stood out as the federative unit with the highest MMR (17 deaths per 100.000 live births). Mothers aged between 40 and 49 years (OR = 3.55, CI: 3.11–4.05) presents higher MMR. Additionally, black women showed the highest MMR (OR = 4.67, CI: 4.18–5.22), as well as mothers with no educational background (OR = 5.83, CI: 4.82–7.06).
Conclusion
The epidemiological profile studied is predominantly composed of mothers with little or no formal education, self-declared as Black, residing in needy states and with advanced aged. These data are useful for formulating public policies aimed at combating the issue.
-
Review Article06-27-2024
Monkeypox infection and pregnancy in lower and middle-income countries: Precautions & recommendations
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo54
Abstract
Review ArticleMonkeypox infection and pregnancy in lower and middle-income countries: Precautions & recommendations
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo54
Views198See moreAbstract
Monkeypox (MPX), an orthopoxviral disease endemic in Africa, is now a public health emergency of international concern (PHEIC) as declared by the World Health Organization in July 2023. Although it is generally mild, the overall case fatality rate was reported to be 3%, and the basic reproduction number (R0) is > 1 in men who have sex with men (MSM, i.e., Portugal (1.4), the United Kingdom (1.6), and Spain (1.8)). However, R0 is < 1 in other settings. In concordance with the smallpox virus, it is also expected to increase the risk of adverse outcomes for both the mother and the fetus. The outcomes of the disease in an immunocompromised state of pregnancy are scary, showing high mortality and morbidity of both mother and fetus, with up to a 75% risk of fetal side effects and a 25% risk of severe maternal diseases. Therefore, it warrants timely diagnosis and intervention. The reverse transcription polymerase chain reaction (RT PCR) test is the standard approach to diagnosis. We summarized the recent findings of MPX on pregnancy, and the associated risk factors. We also give recommendations for active fetal surveillance, perinatal care, and good reporting to improve outcomes. The available vaccines have shown promise for primary disease prevention.
-
Review Article02-09-2022
Prevalence of Preeclampsia in Brazil: An Integrative Review
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(7):686-691
Abstract
Review ArticlePrevalence of Preeclampsia in Brazil: An Integrative Review
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(7):686-691
Views307See moreAbstract
Objective
To review literature and estimate the occurrence of preeclampsia and its complications in Brazil.
Methods
We performed an integrative review of the literature, and included observational studies published until August 2021 on the SciELO and PubMed databases that evaluated preeclampsia among pregnant women in Brazil. Other variables of interests were maternal death, neonatal death, hemolysis, elevated liver enzymes, and low platelet count (HELLP) syndrome, and eclampsia. Three independent reviewers evaluated all retrieved studies and selected those that met inclusion criteria. A metanalysis of the prevalence of preeclampsia and eclampsia was also performed, to estimate a pooled frequency of those conditions among the studies included.
Results
We retrieved 304 studies after the initial search; of those, 10 were included in the final analysis, with a total of 52,986 women considered. The pooled prevalence of preeclampsia was of 6.7%, with a total of 2,988 cases reported. The frequency of eclampsia ranged from 1.7% to 6.2%, while the occurrence of HELLP syndrome was underreported. Prematurity associated to hypertensive disorders ranged from 0.5% to 1.72%.
Conclusion
The frequency of preeclampsia was similar to that reported in other international studies, and it is increasing in Brazil, probably due to the adoption of new diagnostic criteria. The development of a national surveillance network would be essential to understand the problem of hypertensive disorders of pregnancy in Brazil.
-
Original Article01-19-2021
Malignant Uterine Neoplasms Attended at a Brazilian Regional Hospital: 16-years Profile and Time Elapsed for Diagnosis and Treatment
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(2):137-144
Abstract
Original ArticleMalignant Uterine Neoplasms Attended at a Brazilian Regional Hospital: 16-years Profile and Time Elapsed for Diagnosis and Treatment
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(2):137-144
Views202See moreAbstract
Objective
The present study aims to evaluate the profile of endometrial carcinomas and uterine sarcomas attended in a Brazilian cancer center in the period from 2001 to 2016 and to analyze the impact of time elapsed fromsymptoms to diagnoses or treatment in cancer stage and survival.
Methods
This observational study with 1,190 cases evaluated the year of diagnosis, age-group, cancer stage and histological type. A subgroup of 185 women with endometrioid histology attended in the period from 2012 to 2017 was selected to assess information about initial symptoms, diagnosticmethods, overall survival, and to evaluate the influence of the time elapsed from symptoms to diagnosis and treatment on staging and survival. The statistics used were descriptive, trend test, and the Kaplan- Meier method, with p-values < 0.05 for significance.
Results
A total of 1,068 (89.7%) carcinomas (77.2% endometrioid and 22.8% nonendometrioid) and 122 (10.3%) sarcomas were analyzed, with an increasing trend in the period (p < 0.05). Histologies of non-endometrioid carcinomas, G3 endometrioid, and carcinosarcomas constituted 30% of the cases. Non-endometrioid carcinomas and sarcomas weremore frequently diagnosed in patients over 70 years of age and those on stage IV (p < 0.05). The endometrioid subgroup with 185 women reported 92% of abnormal uterine bleeding and 43% diagnosis after curettage. The average time elapsed between symptoms to diagnosis was 244 days, and between symptoms to treatment was 376 days, all without association with staging (p = 0.976) and survival (p = 0.160). Only 12% of the patients started treatment up to 60 days after diagnosis.
Conclusion
The number of uterine carcinoma and sarcoma cases increased over the period of 2001 to 2016. Aggressive histology comprised 30% of the patients and, for endometrioid carcinomas, the time elapsed between symptoms and diagnosis or treatment was long, although without association with staging or survival.
-
Original Article11-07-2019
Trends Associated with Stillbirth in a Maternity Hospital School in the North Zone of São Paulo: A Cross-Sectional Study
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(10):597-606
Abstract
Original ArticleTrends Associated with Stillbirth in a Maternity Hospital School in the North Zone of São Paulo: A Cross-Sectional Study
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(10):597-606
Views171See moreAbstract
Objective
To evaluate conditions associated with stillbirth (SB), and possible trends related with it, in a maternity hospital school in the North zone of São Paulo.
Methods
An observational, cross-sectional study conducted at the Hospital Maternidade- escola de Vila Nova Cachoeirinha with 1,139 SBs in the period of 2003 to 2017. Cases of intermediate SB (ISB) (weight between 500 and 999 g) and late SB (LSB) (weight ≥ 1,000 g) were compared. We evaluated clinical data, laboratory tests, and fetal and placental studies. Data were stored in Windows Excel (Microsoft Corp., Redmond, WA, USA) worksheets, according to which graphs and tables were constructed. We used the statistical software SPSS for Windows version 18.0 (SPSS In., Chicago, IL, USA), estimating the prevalence ratio (PR) and odds ratio (OR), considering the 95% confidence interval (95% CI).
Results
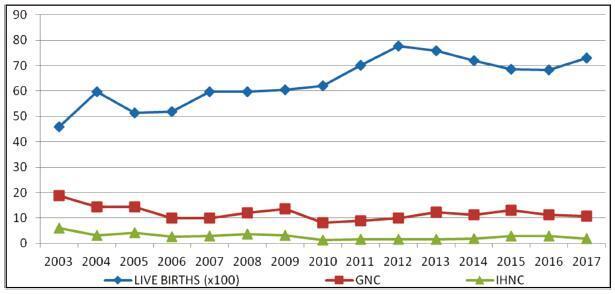
The general SB rate was 11.9%, and the in-hospital SB rate was 2.8%. Pregnant women younger than 16 years of age were more likely to have ISB (OR 0.32, 0.15- 0.76), while patients older than 40 years old had a higher chance of LSB (PR 0.85, 0.72- 0.99). A total of 25.7% of the general population did not have prenatal care, and 77.1% of the cases presented fetal death at admission. The cases of ISB had a statistically significant association with home birth (OR 0.61, 0.46-0.80). Cesarean section was performed in 16.1% of the subjects, and misoprostol was the most used method for induction. Necropsy and placental study of the fetuses were performed, respectively, in 94.2% and 97.3% of the cases. Associated causes were not identified in 22.1% of the cases, and the main causes identified were amniotic sac infections (27.9%), fetal malformations (12.5%), placental abruption (11.2%), hypertensive syndromes (8.5%), and maternal syphilis (3.9%), the latter with an increasing trend.
Conclusion
Among the factors associated to SB were: hypertensive syndromes, amniotic sac infections, fetal malformations, placental abruption and syphilis. There was a growing trend in the number of cases of syphilis, which translates an alert. Diagnostic limitations justify indeterminate causes.
-
Original Article06-01-2018
Cervical Cancer Registered in Two Developed Regions from Brazil: Upper Limit of Reachable Results from Opportunistic Screening
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(6):347-353
Abstract
Original ArticleCervical Cancer Registered in Two Developed Regions from Brazil: Upper Limit of Reachable Results from Opportunistic Screening
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(6):347-353
Views137Abstract
Objective
The aim of this study was to assess the time trends and pattern of cervical cancer diagnosed in the period from 2001 to 2012 by means of an opportunistic screening program from two developed regions in Brazil.
Methods
An observational study analyzing 3,364 cancer records (n = 1,646 from Campinas and n = 1,718 from Curitiba region) available in hospital-based cancer registries was done. An additional 1,836 records of CIN3/AIS from the region of Campinas was analyzed. The statistical analysis assessed the pooled data and the data by region considering the year of diagnosis, age-group, cancer stage, and histologic type. The Cochran-Armitage trend test was applied and p-values < 0.05 were considered significant.
Results
The total annual cervical cancer registered from2001 to 2012 showed a slight drop (273-244), with an age average of 49.5 y, 13 years over the average for CIN3/AIS (36.8 y). A total of 20.6% of the diagnoses (1.6% under 25 y) were done out of the official screening age-range. The biennial rate of diagnoses by age group for the region of Campinas showed an increase trend for the age groups under 25 y (p = 0.007) and 25 to 44 y (p = 0.003). Stage III was the most recorded for both regions, with an annual average of 43%, without any trend modification. There was an increasing trend for stage I diagnoses in the region of Campinas (p = 0.033). The proportion of glandular histologic types registered had an increased trend over time (p = 0.002), higher for the region of Campinas (21.1% versus 12.5% for the region of Curitiba).
Conclusion
The number, pattern and trends of cervical cancer cases registered had mild and slow modifications and reflect the limited effectivity of the opportunistic screening program, even in developed places.
Key-words Cervical cancerCervical intraepithelial neoplasiaEpidemiologypreventive medicinePublic healthSee more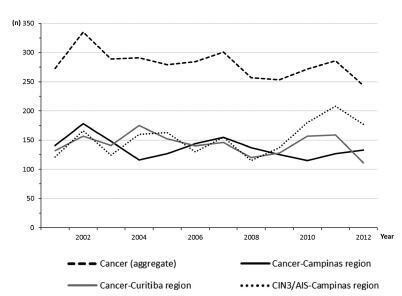
-
Original Article09-01-2017
Regional and Socioeconomic Differences in the Coverage of the Papanicolau Test in Brazil: Data from the Brazilian Health Survey 2013
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(9):480-487
Abstract
Original ArticleRegional and Socioeconomic Differences in the Coverage of the Papanicolau Test in Brazil: Data from the Brazilian Health Survey 2013
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(9):480-487
Views119Abstract
Purpose
To evaluate the coverage of the Papanicolaou test in Brazil and the associated factors.
Methods
Cross-sectional study based on data from the Brazilian Health Survey 2013 comprising the proportion of 25- to 64-year-old women who had undergone a Papanicolaou test within the previous 3 years, categorized by sociodemographic variables and access to healthcare services.
Results
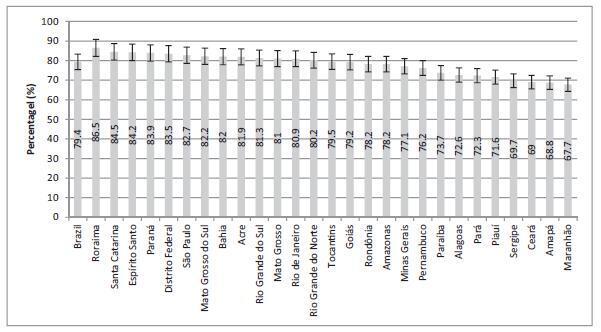
The screening coverage in Brazil was of 79.4% (95% confidence interval [95%CI]: 78.4-80.3), showing significant differences between the different states of the country, with the highest rate in the state of Roraima (86.5; 95%CI: 83.5-89.4), and the lowestone in the state ofMaranhão (67.7; 95%CI: 61.3-74.0).Undergoing the test was significantlymore frequent amongmarriedwomen (83.6%; 95%CI: 82.4-84.8), those with higher educational levels (88.7%; 95%CI: 87.0-90.5), of white ethnicity (82.6%; 95%CI: 81.3-83.9) and who reside in urban areas (80.1%; 95%CI: 79.1-81.2). Those who had undergone the test more than three years prior to the survey and the ones who had never undergone it were associated with a lower level of education, being of black or brown ethnicity, single or divorced, and rural dwellers.
Conclusions
The coverage of cervical cancer screening in Brazil is below the recommended rate and presents regional and sociodemographic disparities.
Key-words cervical neoplasmsearly detection of cancerEpidemiologyinequalities in healthPapanicolaou testWomen's healthSee more