Summary
Rev Bras Ginecol Obstet. 2023;45(3):149-159
This article aims to review the literature regarding the use of technologies to promote mental health for pregnant women. We seek to: understand the strategies that pregnant women use for mental health care. Also, we investigate the existence of scientific evidence that validates such practices.
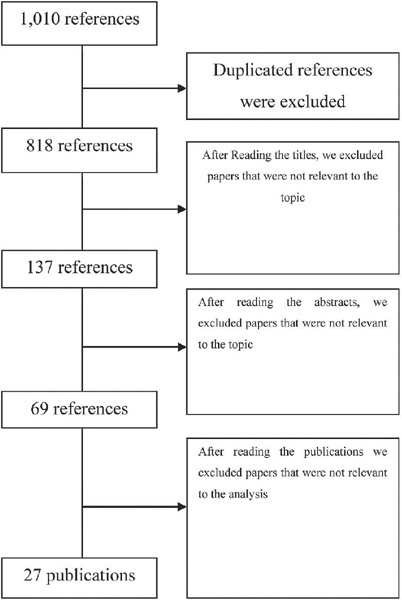
This study follows the PRISMA guidelines for systematic reviews. We analyze 27 studies published between 2012 and 2019. We include publications in Portuguese, English, and Spanish.
The results revealed several different possibilities to use technology, including the use of text messages and mobile applications on smartphones. Mobile applications are the most commonly used approaches (22.5%). Regarding the strategies used, cognitive-behavioral approaches, including mood checks, relaxation exercises, and psychoeducation comprised 44.12% of the content.
There is a need for further investigation and research and development efforts in this field to better understand the possibilities of intervention in mental health in the digital age.
Summary
Rev Bras Ginecol Obstet. 2023;45(4):192-200
To evaluate the use of different treatment options for ectopic pregnancy and the frequency of severe complications in a university hospital.
Observational study with women with ectopic pregnancy admitted at UNICAMP Womeńs Hospital, Brazil, between 01/01/2000 and 12/31/2017. The outcome variables were the type of treatment (first choice) and the presence of severe complications. Independent variables were clinical and sociodemographic data. Statistical analysis was carried out by the Cochran–Armitage test, chi-square test, Mann–Whitney test and multiple Cox regression.
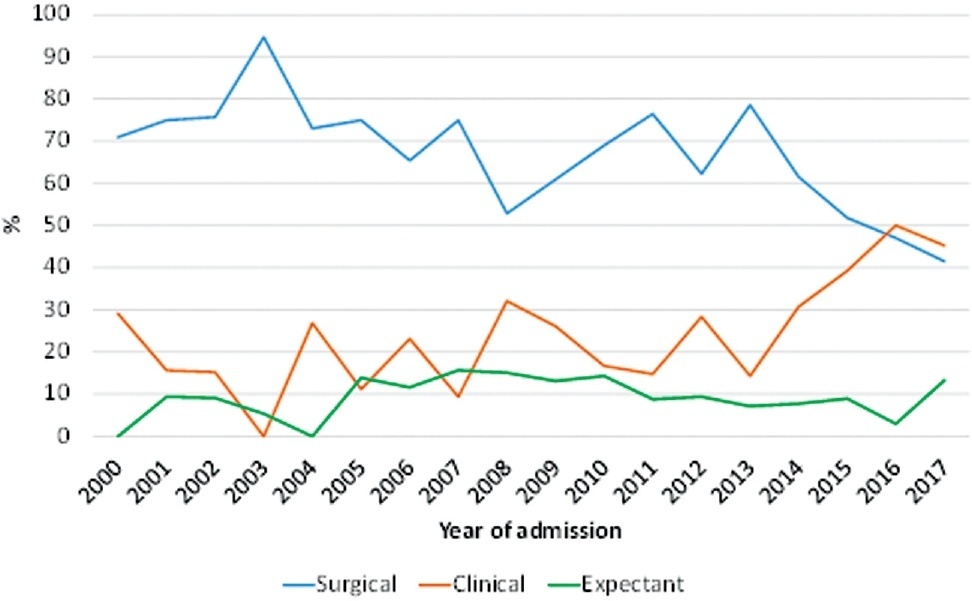
In total 673 women were included in the study. The mean age was 29.0 years (± 6.1) and the mean gestational age was 7.7 (± 2.5). The frequency of surgical treatment decreased significantly over time (z = -4.69; p < 0.001). Conversely, there was a significant increase in the frequency of methotrexate treatment (z = 4.73; p < 0.001). Seventy-one women (10.5%) developed some type of severe complication. In the final statistical model, the prevalence of severe complications was higher in women who were diagnosed with a ruptured ectopic pregnancy at admission (PR = 2.97; 95%CI: 1.61–5.46), did not present with vaginal bleeding (PR = 2.45; 95%CI: 1.41–4.25), had never undergone laparotomy/laparoscopy (PR = 6.69; 95%CI: 1.62–27.53), had a non-tubal ectopic pregnancy (PR = 4.61; 95%CI: 1.98–10.74), and do not smoke (PR = 2.41; 95%CI: 1.08–5.36).
there was a change in the first treatment option for cases of ectopic pregnancy in the hospital during the period of analysis. Factors inherent to a disease that is more difficult to treat are related to a higher frequency of severe complications.
Summary
Rev Bras Ginecol Obstet. 2021;43(5):384-394
Coronavirus disease 2019 (COVID-19) is a disease caused by a newly discovered coronavirus, severe acute respiratory syndrome coronavirus 2 (SARSCoV-2), which usually leads to non-specific respiratory symptoms. Although pregnant women are considered at risk for respiratory infections by other viruses, such as SARS and Middle East respiratory syndrome (MERS), little is known about their vulnerability to SARS-CoV-2. Therefore, this study aims to identify and present the main studies on the topic, including the postpartum period.
In this narrative review, articles were searched in various databases, organizations, and health entities using keywords compatible with medical subject headings (MeSH), such as: COVID-19, pregnancy, vertical transmission, coronavirus 2019, and SARS-CoV-2.
The review of the scientific literature on the subject revealed that pregnant women with COVID-19 did not present clinical manifestations significantly different from those of non-pregnant women; however, there are contraindicated therapies. Regarding fetuses, studies were identified that reported that infection by SARS-CoV-2 in pregnant women can cause fetal distress, breathing difficulties and premature birth, but there is no substantial evidence of vertical transmission.
Due to the lack of adequate information and the limitations of the analyzed studies, it is necessary to provide detailed clinical data on pregnant women infected with SARS-CoV-2 and on the maternal-fetal repercussions caused by this infection. Thus, this review may contribute to expand the knowledge of professionals working in the area as well as to guide more advanced studies on the risk related to pregnant women and their newborns. Meanwhile, monitoring of confirmed or suspected pregnant women with COVID-19 is essential, including in the postpartum period.
Summary
Rev Bras Ginecol Obstet. 2020;42(11):772-773
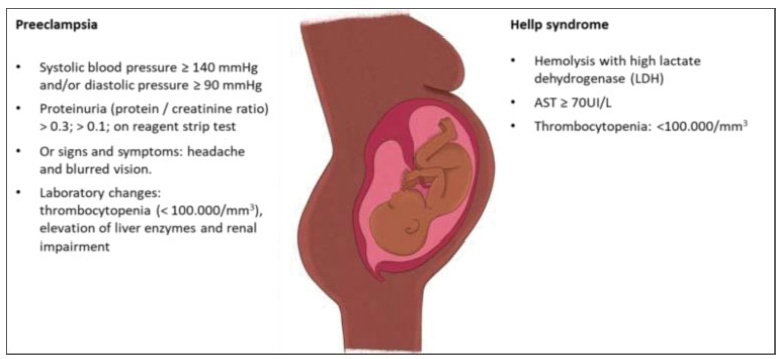
Pre-eclampsia (PE) is an obstetric disease with a multifactorial cause that affects ∼ 5% of pregnant women. Vision can be affected with varying severity, and retinal detachment is a very rare complication. It tends to be bilateral, diagnosed postpartum, and more prevalent in women who are primiparous and/or undergo caesarean delivery. The condition typically resolves completely and rarely causes total visual loss in the affected women. Fluorescence angiographic findings support the hypothesis that retinal detachment in PE is secondary to choroidal ischemia from intense arteriolar vasospasm. The present article is related to a case of a 37-year-old pregnant woman who had PE associated with a progressive blurred vision, diagnosed by ophthalmology as serous macular detachment of the retina.
Summary
Rev Bras Ginecol Obstet. 2020;42(10):659-668
To identify the most effective procedures recommended for the prevention of preeclampsia.
A systematic review was performed in the following databases: Pubmed/MEDLINE, CINAHL, Web of Science, Cochrane and LILACS via the Virtual Health Library (VHL). A manual search was also performed to find additional references. The risk of bias, the quality of the evidence, and the classification of the strength of the recommendations were evaluated using the Grading of Recommendations, Assessment, Development and Evaluations (GRADE) approach.
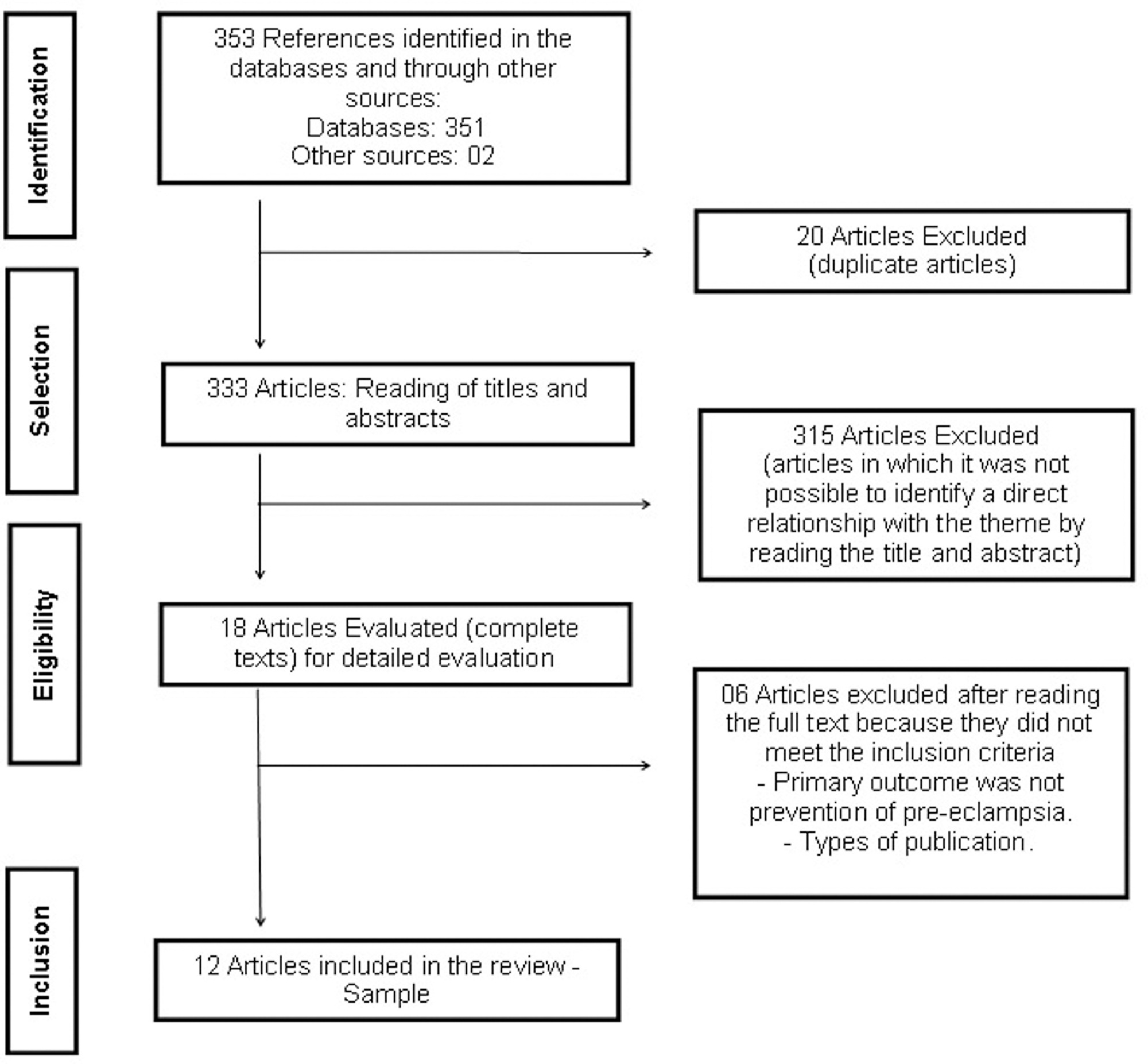
In the initial search in the databases, the total number of articles retrieved was 351, and 2 were retrieved through the manual search; after duplicate articles were removed, 333 citations remained. After a thorough review of the titles and abstracts, 315 references were excluded. Accordingly, 18 articles were maintained for selection of the complete text (phase 2). This process led to the exclusion of 6 studies. In total, 12 articles were selected for data extraction and qualitative synthesis.
The articles selected for the study were analyzed, and we inserted the synthesis of the evidence in the online software GRADEpro Guideline Development Tool (GDT) (McMaster University and Evidence Prime Inc. All right reserved. McMaster University, Hamilton, Ontário, Canada); thus, it was possible to develop a table of evidence, with the quality of the evidence and the classification of the strength of the recommendations.
In total, seven studies recommended the individual use of aspirin, or aspirin combined with calcium, heparin or dipyridamole. The use of calcium alone or in combination with phytonutrients was also highlighted. All of the studies were with women at a high risk of developing preeclampsia.
According to the studies evaluated, the administration of aspirin is still the best procedure to be used in the clinical practice to prevent preeclampsia.
Summary
Rev Bras Ginecol Obstet. 2020;42(10):669-671
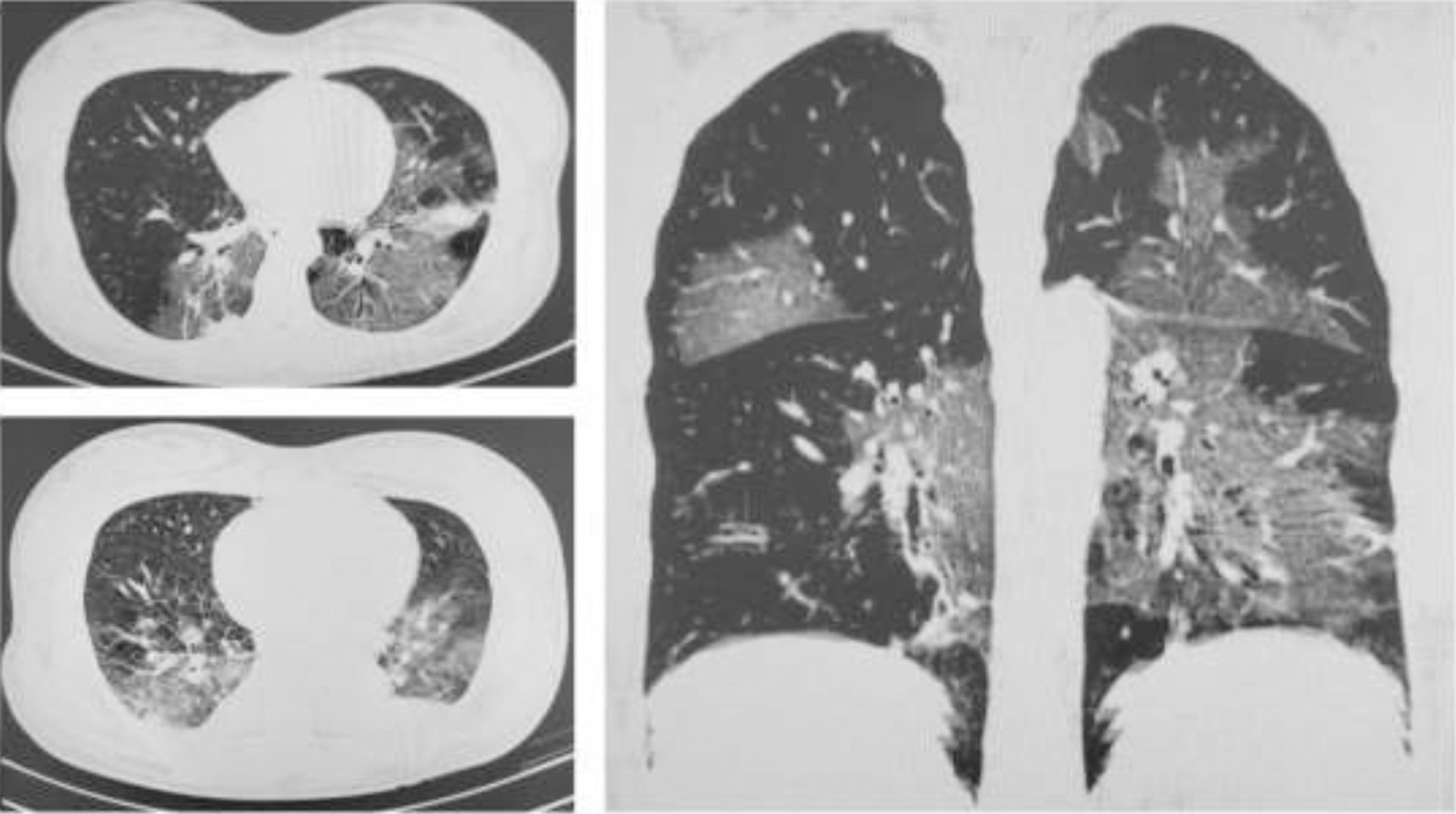
The present report describes the case of a 31-year-old primigravida, with dichorionic twins at 31 weeks. She presented with history of myalgia, jaundice, and abdominal discomfort. No flu-like symptoms as fever or cough. She was not aware of exposure to COVID-19. Normal blood pressure and O2 saturation. Laboratory tests showed platelet count of 218,000 mm3, alanine aminotransferase (ALT) 558 IU and serum creatinine 2.3 mg/dl. Doppler ultrasound in one twin was compatible with brain sparing. Partial hemolysis, elevated liver enzymes, low platelet count (HELLP) syndrome was the hypothesis, and a cesarean section was performed. On day 2, the white-cell count reached 33,730, with decreased consciousness and mild respiratory distress. Tomography revealed both lungs with ground-glass opacities. Swab for COVID-19 polymerase chain reaction (PCR) was positive. Thrombocytopenia in patients with COVID-19 appears to be multifactorial, similar to what occurs in preeclampsia and HELLP syndrome. We assume that the synergism of these pathophysiological mechanisms could accelerate the compromise of maternal conditions and could be a warning to the obstetric practice.
Summary
Rev Bras Ginecol Obstet. 2020;42(4):200-210
The present study is a systematic review of the literature to assess whether the presence of endometriosis determines or contributes to adverse obstetric outcomes.
The present work was carried out at the Hospital Israelita Albert Einstein, São Paulo, state of São Paulo, Brazil, in accordance to the PRISMA methodology for systematic reviews. A review of the literature was performed using PubMed, Web of Science and Scopus databases. The keywords used were: pregnancy outcome, pregnancy complications, obstetrical complications, obstetrics, obstetric outcomes and endometriosis. The survey was further completed by a manually executed review of cross-referenced articles, which was last performed on November 30, 2018.
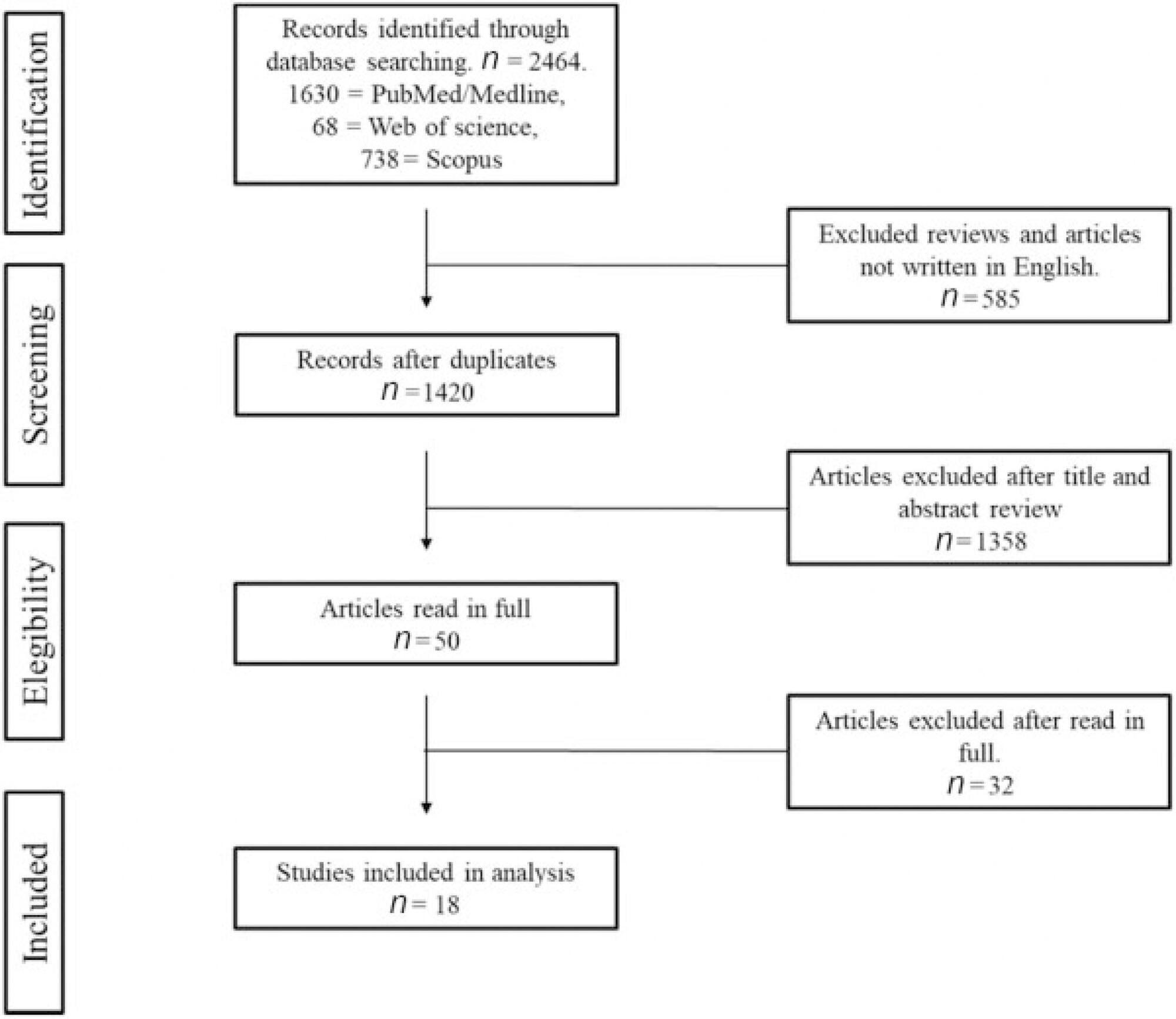
The survey disclosed a total of 2,468 articles, published from May 1946 to October 2017. A total of 18 studies were selected to be further classified according to their quality and relevance.
The Newcastle-Ottawa Quality Assessment Scale was used for classification. Five studies of greater impact and superior evidence quality and 13 studies of moderate evidence quality were selected. We analyzed the studies for the characteristics of their patients plus how endometriosis was diagnosed and their respective obstetric outcomes taking into account their statistical relevance.
Analyses of the higher impact and better quality studies have shown high incidence of preterm birth and placenta previa in patients with endometriosis.
Placenta previa and preterm birth are the most statistically significant outcomes related to endometriosis, as indicated by our systematic review. The present information is useful to alert obstetricians and patients about possible unfavorable obstetric outcomes.
Summary
Rev Bras Ginecol Obstet. 2020;42(2):74-80
To evaluate the impact of the presence of criteria for severe maternal morbidity and maternal near miss associated with hypertensive disorders on maternal and perinatal outcomes in a maternity school.
The present is a sub-analysis of a larger study involving 27 centers in Brazil that estimated the prevalence of serious maternal morbidity and near miss. It is an analytical and cross-sectional study with a quantitative approach, involving 928 women who were cared for at Maternidade Escola Assis Chateaubriand (MEAC, in Portuguese), Universidade Federal do Ceará (UFC, in Portuguese), from July 2009 to June 2010. The women were diagnosed with near miss according to the World Health Organization (WHO) criteria. The sample was divided into 2 groups: patients with (n = 827) and without hypertension (n = 101). The results were considered statistically significant when p < 0.05. The Pearson chi-squared and Fisher Exact tests were used for the categorical variables, and the Mann–Whitney U test was used for the continuous variables.
In total, 51 participants with maternal near miss criteria were identified, and 36 of them had hypertensive disorders. Of these, 5 died and were obviously excluded from the near miss final group. In contrast, we observed 867 cases with non-near miss maternal morbidity criteria. During this period, there were 4,617 live births (LBs) in the institution that was studied.
In the severe morbidity/maternal near miss population, the presence of hypertensive complications was prevalent, constituting a risk factor for both the mother and the fetus.
Search
Search in:
breast (42) breast cancer (42) breast neoplasms (95) Cesarean section (72) endometriosis (66) infertility (56) Maternal mortality (43) menopause (82) obesity (58) postpartum period (40) pregnancy (225) Pregnancy complications (99) Prenatal care (68) prenatal diagnosis (50) Prevalence (41) Quality of life (51) risk factors (94) ultrasonography (79) urinary incontinence (40) women's health (48)