-
Review Article02-09-2022
Prevalence of Preeclampsia in Brazil: An Integrative Review
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(7):686-691
Abstract
Review ArticlePrevalence of Preeclampsia in Brazil: An Integrative Review
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(7):686-691
Views323See moreAbstract
Objective
To review literature and estimate the occurrence of preeclampsia and its complications in Brazil.
Methods
We performed an integrative review of the literature, and included observational studies published until August 2021 on the SciELO and PubMed databases that evaluated preeclampsia among pregnant women in Brazil. Other variables of interests were maternal death, neonatal death, hemolysis, elevated liver enzymes, and low platelet count (HELLP) syndrome, and eclampsia. Three independent reviewers evaluated all retrieved studies and selected those that met inclusion criteria. A metanalysis of the prevalence of preeclampsia and eclampsia was also performed, to estimate a pooled frequency of those conditions among the studies included.
Results
We retrieved 304 studies after the initial search; of those, 10 were included in the final analysis, with a total of 52,986 women considered. The pooled prevalence of preeclampsia was of 6.7%, with a total of 2,988 cases reported. The frequency of eclampsia ranged from 1.7% to 6.2%, while the occurrence of HELLP syndrome was underreported. Prematurity associated to hypertensive disorders ranged from 0.5% to 1.72%.
Conclusion
The frequency of preeclampsia was similar to that reported in other international studies, and it is increasing in Brazil, probably due to the adoption of new diagnostic criteria. The development of a national surveillance network would be essential to understand the problem of hypertensive disorders of pregnancy in Brazil.
-
Original Article01-24-2021
Preeclampsia and Gestational Hypertension: Biochemical and Antioxidant Features in Vitro Might Help Understand Different Outcomes
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(12):894-903
Abstract
Original ArticlePreeclampsia and Gestational Hypertension: Biochemical and Antioxidant Features in Vitro Might Help Understand Different Outcomes
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(12):894-903
Views141See moreAbstract
Objective
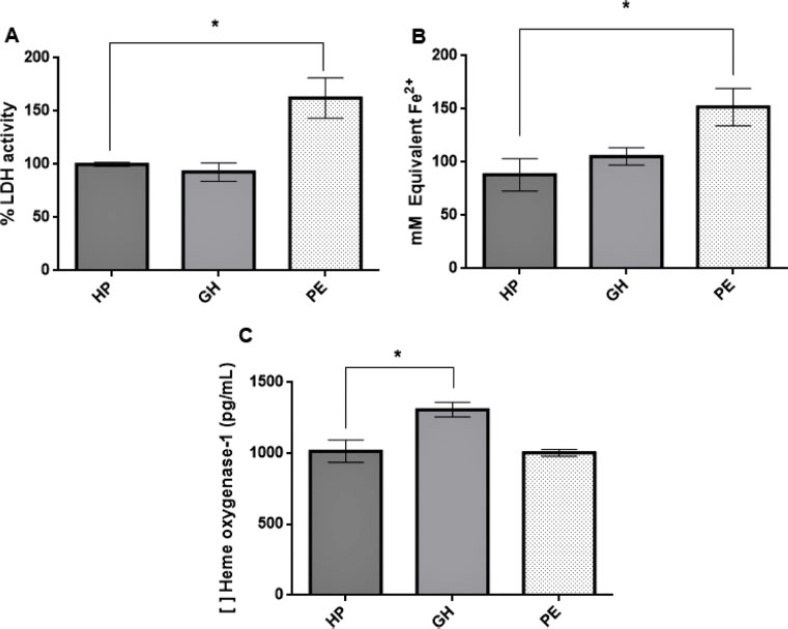
Gestational hypertension (GH) is characterized by increased blood pressure after the 20th gestational week; the presence of proteinuria and/or signs of end-organ damage indicate preeclampsia (PE). Heme oxygenase-1 (HO-1) is an antioxidant enzyme with an important role in maintaining endothelial function, and induction of HO-1 by certain molecules shows potential in attenuating the condition’s effects over endothelial tissue. HO-1 production can also be stimulated by potassium iodide (KI). Therefore, we evaluated the effects of KI over HO-1 expression in human umbilical vein endothelial cells (HUVECs) incubated with plasma from women diagnosed with GH or PE.
Methods
Human umbilical vein endothelial cells were incubated with a pool of plasma of healthy pregnant women (n = 12), pregnant women diagnosed with GH (n = 10) or preeclamptic women (n = 11)with or without the addition of KI for 24 hours to evaluate its effect on this enzyme expression. Analysis of variance was performed followed by Dunnet’s test for multiple comparisons between groups only or between groups with addition of KI (p ≤ 0.05).
Results
KI solution (1,000 µM) reduced HO-1 in the gestational hypertension group (p = 0.0018) and cytotoxicity in the preeclamptic group (p = 0.0143); treatment with KI reduced plasma cytotoxicity but did not affect the preeclamptic group’s HO-1 expression.
Conclusion
Our findings suggest that KI alleviates oxidative stress leading to decreased HO-1 expression; plasma from preeclamptic women did not induce the enzyme’s expression in HUVECs, and we hypothesize that this is possibly due to inhibitory post-transcriptional mechanisms in response to overexpression of this enzyme during early pregnancy.
-
Original Article01-24-2021
Uterine Artery Pulsatility Index as a Pre-eclampsia Predictor in the 3 Trimesters in Women with Singleton Pregnancies
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(12):904-910
Abstract
Original ArticleUterine Artery Pulsatility Index as a Pre-eclampsia Predictor in the 3 Trimesters in Women with Singleton Pregnancies
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(12):904-910
Views230See moreAbstract
Objective
To evaluate the mean uterine artery pulsatility index (UtAPI) in each trimester of pregnancy as a predictor of early or late pre-eclampsia (PE) in Colombian pregnant women.
Methods
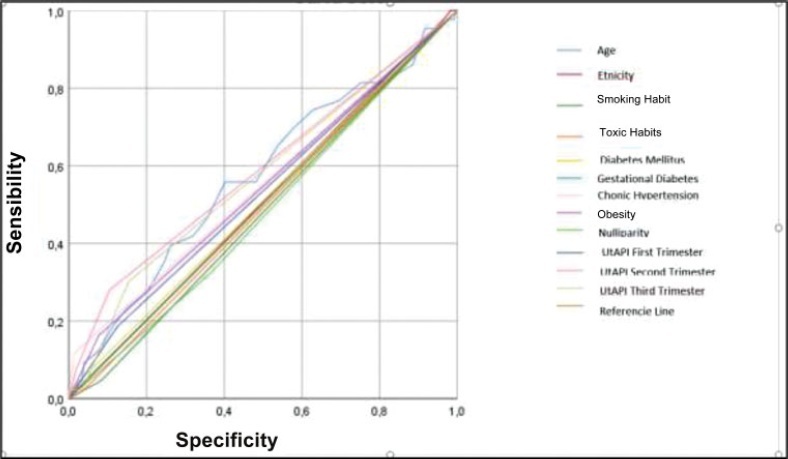
The UtAPI was measured in singleton pregnancies in each trimester. Uterine artery pulsatility index as predictor of PE was evaluated by odds ratio (OR), receiver operating characteristic (ROC) curves, and Kaplan-Meier diagram.
Results
Analysis in the 1st and 3rd trimester showed that abnormal UtAPI was associated with early PE (OR: 5.99: 95% confidence interval [CI]: 1.64–21.13; and OR: 10.32; 95%CI: 2.75–42.49, respectively). Sensitivity and specificity were 71.4 and 79.6%, respectively, for developing PE (area under the curve [AUC]: 0.922). The Kaplan-Meier curve showed that a UtAPI of 0.76 (95%CI: 0.58–1.0) in the 1st trimester was associated with early PE, and a UtAPI of 0.73 (95%CI: 0.55–0.97) in the 3rd trimester was associated with late PE.
Conclusion
Uterine arteries proved to be a useful predictor tool in the 1st and 3rd trimesters for early PE and in the 3rd trimester for late PE in a pregnant population with high prevalence of PE.
-
Review Article11-15-2021
Expectant Versus Interventionist Care in the Management of Severe Preeclampsia Remote from Term: A Systematic Review
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(8):627-637
Abstract
Review ArticleExpectant Versus Interventionist Care in the Management of Severe Preeclampsia Remote from Term: A Systematic Review
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(8):627-637
Views176See moreAbstract
Objective
To compare the effects of expectant versus interventionist care in the management of pregnant women with severe preeclampsia remote from term.
Data sources
An electronic search was conducted in the Medical Literature Analysis and Retrieval System Online (MEDLINE), Excerpta Medica Database (EMBASE), Cochrane Central Register of Controlled Trials (CENTRAL), Latin American and Caribbean Health Sciences Literature (LILACS, for its Spanish acronym), World Health Organization’s International Clinical Trials Registry Platform (WHO-ICTRP), and Open- Grey databases. The International Federation of Gynecology and Obstetrics (FIGO, for its French acronym), Royal College of Obstetricians and Gynaecologists (RCOG), American College of Obstetricians and Gynecologists (ACOG), and Colombian Journal of Obstetrics and Gynecology (CJOG) websites were searched for conference proceedings, without language restrictions, up to March 25, 2020.
Selection of studies
Randomized clinical trials (RCTs), and non-randomized controlled studies (NRSs) were included. The Grading of Recommendations, Assessment, Development and Evaluation (GRADE) approach was used to evaluate the quality of the evidence.
Data collection
Studies were independently assessed for inclusion criteria, data extraction, and risk of bias. Disagreements were resolved by consensus.
Data synthesis
Four RCTs and six NRS were included. Low-quality evidence from the RCTs showed that expectant care may result in a lower incidence of appearance, pulse, grimace, activity, and respiration (Apgar) scores<7 at 5 minutes (risk ratio [RR]: 0.48; 95% confidence interval [95%CI]: 0.23%to 0.99) and a higher average birth weight (mean difference [MD]: 254.7 g; 95%CI: 98.5 g to 410.9 g). Very low quality evidence from the NRSs suggested that expectant care might decrease the rates of neonatal death (RR: 0.42; 95%CI 0.22 to 0.80), hyalinemembrane disease (RR: 0.59; 95%CI: 0.40 to 0.87), and admission to neonatal care (RR: 0.73; 95%CI: 0.54 to 0.99). Nomaternal or fetal differences were found for other perinatal outcomes.
Conclusion
Compared with interventionist management, expectant care may improve neonatal outcomes without increasing maternal morbidity and mortality.
-
Clinical Consensus Recommendation03-08-2021
Pre-eclampsia: Universal Screening or Universal Prevention for Low andMiddle-Income Settings?
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(1):61-65
Abstract
Clinical Consensus RecommendationPre-eclampsia: Universal Screening or Universal Prevention for Low andMiddle-Income Settings?
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(1):61-65
Views301See moreAbstract
Pre-eclampsia (PE) is a severe disorder that affects up to 8% of all pregnancies and represents an important cause of maternal and perinatal morbidity and mortality. The screening of the disease is a subject of studies, but the complexity and uncertainties regarding its etiology make this objective a difficult task. In addition, the costs related to screening protocols, the heterogeneity of the most affected populations and the lack of highly effective prevention methods reduce the potential of current available algorithms for screening. Thus, the National Specialized Commission of Hypertension in Pregnancy of the Brazilian Association of Gynecology and Obstetrics Federation (Febrasgo, in the Portuguese acronym) (NSC Hypertension in Pregnancy of the Febrasgo) considers that there are no screening algorithms to be implemented in the country to date and advocates that Aspirin and calcium should be widely used.
-
Case Report01-11-2020
Preeclampsia as an Inaugural Manifestation of Primary Hyperparathyroidism: A Case Report
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):841-844
Abstract
Case ReportPreeclampsia as an Inaugural Manifestation of Primary Hyperparathyroidism: A Case Report
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):841-844
Views175See moreAbstract
Primary hyperparathyroidism is an endocrine disorder characterized by hypercalcemia and elevated or inappropriately normal levels of parathyroid hormone. The diagnosis is based on a biochemical evaluation, and a neck ultrasound is the first choice during pregnancy to access the parathyroid glands. Manifestations during pregnancy are rare and can be present with life-threatening complications, so the diagnosis is challenging. The conservative treatment is limited, and there is not enough data about its safety and efficacy during pregnancy. Surgery is the only curative treatment, and a parathyroidectomy performed during the second or third trimesters is considered safe. Recently, some authors suggested an association between primary hyperparathyroidism and preeclampsia. We describe a case of preeclampsia with severe features at 27 weeks of gestational age. The severity of the preeclampsiamotivated an early termination of the pregnancy by cesarean section. During the postpartum period, the patient presented life-threatening complications, such as severe hypercalcemia and acute pancreatitis. An ultrasound exam found two parathyroid nodules, suggestive of parathyroid adenomas. The patient recovered after the pharmacological correction of the calcemia levels.
-
Review Article01-11-2020
Update on Thrombocytopenia in Pregnancy
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):834-840
Abstract
Review ArticleUpdate on Thrombocytopenia in Pregnancy
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):834-840
Views272See moreAbstract
Thrombocytopenia, defined as platelet count < 150,000mm3, is frequently diagnosed by obstetricians since this parameter is included in routine surveillance during pregnancy, with an incidence of between 7 and 12%. Therefore, decisions regarding subsequent examination and management are primordial. While most of the cases are due to physiological changes, as gestational thrombocytopenia, other causes can be related to severe conditions that can lead to fetal or maternal death. Differentiating these conditions might be challenging: they can be pregnancy-specific (pre-eclampsia/ HELLP syndrome [hemolysis, elevated liver enzymes, low platelets]), or not (immune thrombocytopenia purpura, thrombotic thrombocytopenic purpura or hemolytic uremic syndrome). Understanding the mechanisms and recognition of symptoms and signs is essential to decide an adequate line of investigation. The severity of thrombocytopenia, its etiology and gestational age dictates different treatment regimens.
-
Case Report12-21-2020
Coronavirus 2019, Thrombocytopenia and HELLP Syndrome: Association or Coincidence?
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(10):669-671
Abstract
Case ReportCoronavirus 2019, Thrombocytopenia and HELLP Syndrome: Association or Coincidence?
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(10):669-671
Views134See moreAbstract
The present report describes the case of a 31-year-old primigravida, with dichorionic twins at 31 weeks. She presented with history of myalgia, jaundice, and abdominal discomfort. No flu-like symptoms as fever or cough. She was not aware of exposure to COVID-19. Normal blood pressure and O2 saturation. Laboratory tests showed platelet count of 218,000 mm3, alanine aminotransferase (ALT) 558 IU and serum creatinine 2.3 mg/dl. Doppler ultrasound in one twin was compatible with brain sparing. Partial hemolysis, elevated liver enzymes, low platelet count (HELLP) syndrome was the hypothesis, and a cesarean section was performed. On day 2, the white-cell count reached 33,730, with decreased consciousness and mild respiratory distress. Tomography revealed both lungs with ground-glass opacities. Swab for COVID-19 polymerase chain reaction (PCR) was positive. Thrombocytopenia in patients with COVID-19 appears to be multifactorial, similar to what occurs in preeclampsia and HELLP syndrome. We assume that the synergism of these pathophysiological mechanisms could accelerate the compromise of maternal conditions and could be a warning to the obstetric practice.


