Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(1):34-40
DOI 10.1590/S0100-72032007000100006
PURPOSE: to determine the cesarean section (CS) rate in Campinas (SP) and to identify its risk factors. METHODS: a cross-sectional study that analyzed data obtained from Live Birth Certificates in 2001. The dependent variable was the type of delivery and the independent variables were: mothers’ characteristics and those related to their pregnancies, deliveries and to newborns. The assessment of the association among variables was performed through the chi2 test, and crude and adjusted odds ratio (OR) values were calculated. RESULTS: the CS rate was 54.9%. The chances of having CS increased 1.9 times for women from 20-34 years old (adjOR-1.9; 95% CI:1.7-2.1); 3.7 times for those over 35 years old (adjOR-3.8; 95% CI:3.2-4.5); 1.5 times for those who studied from 8-11 years (adjOR-1.5; 95% CI:1.4-1.6); 2.5 times for those who studied more than 11 years (adjOR-2.6; 95% CI:2.2-2.9); 1.3 times for those who were married (adjOR-1.3; 95 % CI:1.2-1.4); 1.6 times for those who had jobs (adjOR-1.6; 95% CI:1.5-1.8); 1.2 times for who had good living conditions (adjOR-1.2; 95% CI:1.0-1.3); 2.2 times for primiparous (adjOR-2.2; 95% CI:1.9-2.5), 1.6 times for multiparous (adjOR-1.6; 95% CI:1.4-1.9) and 2.7 times in twin gestations (adjOR-2.7; 95% CI:1.9-3.9). The women who had inadequate prenatal care were protected for CS (adjOR-0.6; 95% CI:0.5-0.7). CONCLUSION: the chance of having CS was greater among women with better socio-economic conditions, with adequate prenatal care, for primiparous, for multiparous and in twin gestations, suggesting that the basis for indication of cesarean sections were not restricted to clinical factors but influenced by non-medical reasons.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(1):34-39
DOI 10.1590/S0100-72032012000100007
PURPOSE: To compare the maternal and perinatal outcomes of patients with placenta previa, after the adoption of a prolonged maternal hospital stay, to those of a 1991 series. METHODS: We performed a retrospective study comparing 108 cases of placenta previa hospitalized in the Maternity School Assis Chateaubriand, Universidade Federal do Ceará, during the period from 01/01/2006 to 12/31/2010, with those obtained in 1991, when 101 cases of the pathology were observed at our institution. The following maternal and perinatal data were collected: maternal age, parity, gestational age at delivery, mode of delivery, maternal stay length, Apgar scores at the 1st and 5th minutes, birth weight, adequacy of birth weight, neonatal length stay, maternal and neonatal morbidity and mortality rates (maternal, fetal, neonatal and perinatal). Statistical analysis was performed using the χ² and Fisher's exact tests. The results were considered significant when p<0.05. RESULTS: In 1991, placenta previa was found in 1.13% of cases (101/8900). In the present study, the prevalence was 0.43% (108/24726). No maternal death was observed in either series. Regarding the study of 1991, the current patients were significantly younger, with lower parity, were hospitalized longer, had better Apgar scores at 1st and 5th minutes, and had longer neonatal hospitalization. Also, we identified reduction of fetal, neonatal and perinatal mortality. CONCLUSIONS: Perinatal outcomes in patients with placenta previa were significantly improved between 1991 and the years 2006 and 2010. However, we can not say whether this improvement was due to the prolonged maternal hospital stay.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(7):340-347
Aerobic exercises may improve quality of life (QoL) in women with polycystic ovary syndrome (PCOS). However, there is no data on the effect of resistance exercise training (RET) programs on the QoL of women with PCOS. Thus, this study aimed to assess the effect of a 16-week RET program on QoL in PCOS women.
This 16-week case-control study enrolled 43 women with PCOS (PCOS group, PCOSG) and 51 healthy pre-menopausal controls aged 18 to 37 years (control group, CG). All women underwent a supervised RET program for 16 weeks, and were evaluated in two different occasions: week-0 (baseline), and week-16 (after RET). Quality of life was assessed using the 36-Item Short Form Health Survey (SF-36).
Testosterone reduced significantly in both groups after RET (p < 0.01). The PCOSG had improvements in functional capacity at week-16 relative to week-0 (p = 0.02). The CG had significant improvements in vitality, social aspects, and mental health at week-16 relative to week-0 (p ≤ 0.01). There was a weak correlation between social aspects of the SF-36 domain and testosterone levels in PCOS women.
A 16-week RET program modestly improved QoL in women with PCOS.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(8):340-346
DOI 10.1509/SO100-720320140005034
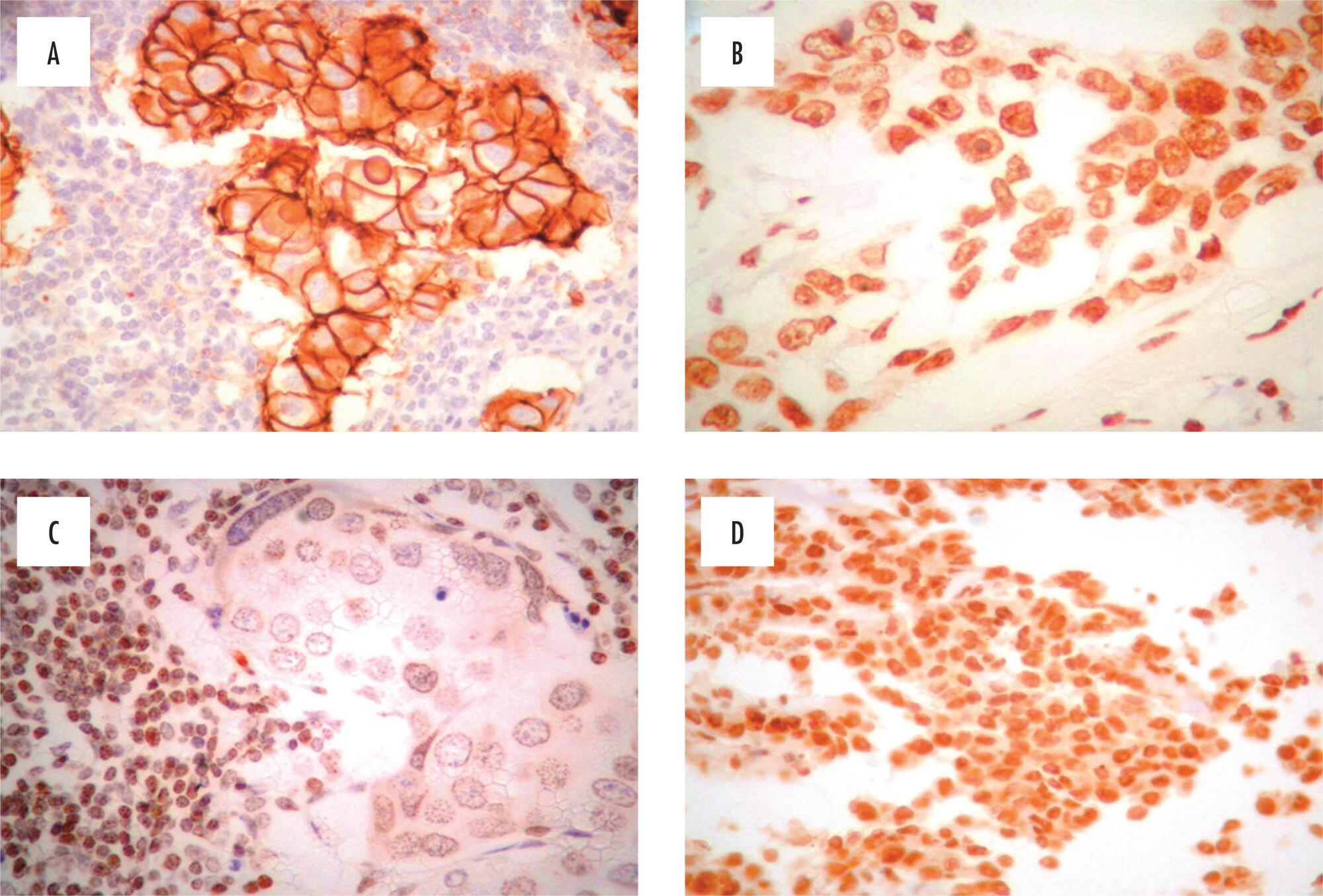
To examine the expression of AKT and PTEN in a series of HER2-positive primary invasive breast tumors using immunohistochemistry, and to associate these expression profiles with classic pathologic features such as tumor grade, hormone receptor expression, lymphatic vascular invasion, and proliferation.
A total of 104 HER2-positive breast carcinoma specimens were prepared in tissue microarrays blocks for immunohistochemical detection of PTEN and phosphorylated AKT (pAKT). Original histologic sections were reviewed to assess pathological features, including HER2 status and Ki-67 index values. The associations between categorical and numeric variables were identified using Pearson's chi-square test and the Mann-Whitney, respectively.
Co-expression of pAKT and PTEN was presented in 59 (56.7%) cases. Reduced levels of PTEN expression were detected in 20 (19.2%) cases, and these 20 tumors had a lower Ki-67 index value. In contrast, tumors positive for pAKT expression [71 (68.3%)] were associated with a higher Ki-67 index value.
A role for AKT in the proliferation of HER2-positive breast cancers was confirmed. However, immunohistochemical detection of PTEN expression did not correlate with an inhibition of cellular proliferation or control of AKT phosphorylation, suggesting other pathways in these mechanisms of control.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(7):340-345
DOI 10.1590/S0100-72032010000700006
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(7):340-345
DOI 10.1590/S0100-72032007000700003
PURPOSE: to evaluate the efficacy of in vitro fertilization (IVF) with intracytoplasmic sperm injection (ICSI) in natural cycle (NC). METHODS: retrospective clinical trial that evaluated 70 treatment cycles in 60 couples that were submitted to IVF treatment with ICSI in NC performed in private clinic from 1999 until 2003. It was performed daily ultrasound monitorization or on alternate days, and urinary LH dosage when the follicle reached 16 mm of diameter. It was scheduled egg retrieval when the follicle reached 18 mm of diameter and 36 hours after hCG administration when the LH test was negative. Embryo transfer was performed 48 to 52 hours after ICSI. RESULTS: 70 ICSI cycles in 60 patients were performed and the indications of treatment included: male factor (47.1%), tubal factor (37.1%), associated factors (8.7%), unknown infertility (7.1%). Out of 70 cycles, 18 cycles were cancelled (25.7% of cancellation rate). Out of 52 patients that were submitted to ovarian punction to oocyte retrieval we found mature oocytes in 77% of the cases (40 cycles), in four cases we collected immature oocytes and in eight cases we could not found it. We had 70% of fertilization rate and only one fertilized oocyte did not achieve the cleavage stage. So, the transfers rate per punction and per mature oocyte was 52% and 67.5%, respectively. We had 11.4% of pregnancy rate per cycle, 15.4% per punction and 29.6% per embryo transfer. CONCLUSIONS: FIV/ICSI in NC seem to be a satisfactory option of treatment, with low costs and complications (multiple gestation and Ovarian Hyperstimulation Syndrome), mainly in poor responder patients and in poor populations.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(6):340-344
DOI 10.1590/S0100-72032006000600004
PURPOSE: the study the effects of maternal cigarette smoking during pregnancy on placental maturation (calcifications) and the placental-uterine circulation, evaluated through umbilical and uterine Doppler. METHODS: prospective cohort study involving 244 pregnant women, 210 of them non-smokers and 34 smokers. Participants were submitted to four serial sonograms. The first was performed up to the 16th week of pregnancy to determine gestational age, and the other three at 28, 32 and 36 weeks for fetal biometry, evaluation of placental texture and Doppler studies of the uterine and umbilical arteries. Premature placental calcification was defined as grade III before 36 weeks. The chi2 and Fisher exact tests were used to compare placental grading, and the Mann-Whitney test to evaluate the resistance index of uterine and umbilical arteries. RESULTS: the frequency of grade III placenta and the resistance of the uterine arteries did not differ significantly between smokers and non-smokers, at all gestational ages. Umbilical artery Doppler was significantly higher in smokers than in non-smokers at 32 weeks. CONCLUSIONS: no association was found between cigarette smoking and premature placental calcification. Smoking was associated with increased umbilical artery resistance at 32 weeks.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(6):340-348
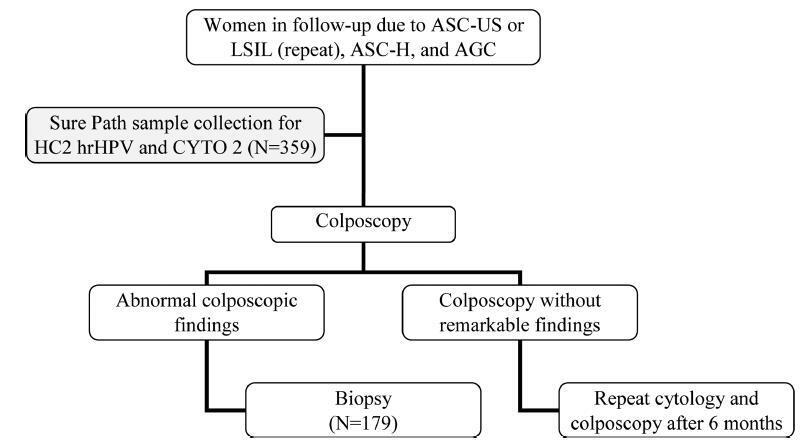
To evaluate the performance of the hybrid capture 2 (HC2) high-risk papillomavirus (hrHPV) assay and cytological test in women with previous abnormalities, to detect cervical intraepithelial neoplasia grade 2 or worse (≥ CIN 2).
A cytological test and HC2 (Qiagen, Gaithersburg, Maryland, EUA) for hrHPV were conducted in 359 liquid-based (Sure Path, Becton Dickinson, TriPath Imaging, Burlington, NC, USA) samples collected from women from the Vale do Ribeira Region, during July 2013 and September 2015 with previous cytology classified as atypical squamous cells of undetermined significance (ASC-US), low-grade squamous intraepithelial lesion (LSIL), atypical squamous cells, cannot exclude high-grade squamous intraepithelial lesions (ASC-H), and atypical glandular cells (AGC). The histopathological examination was conducted in 179 women. The performance evaluations were calculated using the “exact” Clopper-Pearson 95% confidence interval (CI) test by MEDCALC (Medcalc Software Ltd, Ostend, Belgium).
The ≥ CIN 2 frequency was 11.7% (21/179). The HC2 for hrHPV and repeat cytology to detect ≥ CIN 2 obtained, respectively, a sensitivity of 90.5% (95% CI = 69.6-98.8) and 90.5%, (95%CI = 69.6-98.8), a specificity of 65.8% (95% CI = 57.9-73.2) and 43.7% (95%CI = 35.8-51.8), a positive predictive value of 26.0% (95% CI = 21.4-31.3) and 17.6%, (95%CI = 14.9-20.6), and a negative predictive value of 98.1% (95%CI = 93.3-99.5) and 97.2% (95% CI = 90.1-99.2).
Hybrid capture 2 for hrHPV improves the performance of the detection of ≥ CIN 2, without compromising sensitivity, and provides a greater safety margin to return to the triennial screening of women undergoing follow-up due to previous abnormalities, without underlying ≥ CIN 2.