Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo87
To compare access and suitability of antenatal care between years 2020 and 2022 among postpartum individuals at a Hospital in Florianopolis, and evaluate factors associated with antenatal suitability.
Observational, cross-sectional, and quantitative study carried out in 2022. Collected data were compared with the database of a previous similar study carried out in the same setting in 2020. Data were extracted from medical records and prenatal booklets, in addition to a face-to-face questionnaire. Adequacy was measured using the Carvalho and Novaes index and health access was qualitatively evaluated. Socio-demographic and antenatal variables were analyzed. A statistical significance level of 0.05 was considered. Open-ended questions were categorized for analysis.
395 postpartum individuals were included. Antenatal care was adequate for 48.6% in 2020 and 69.1% in 2022. Among the barriers to access, 56% reported difficulty in scheduling appointments and/or exams and 23% complained of reduced healthcare staff due to strikes, COVID-19, among others. Adequate antenatal care was associated with being pregnant in 2022, being referred to high-risk units (PNAR), and not reporting difficulties in access. Also, it was associated with twice the chance of investigation for gestational diabetes (GDM) and syphilis.
The 2022 post-vaccination period showed higher antenatal adequacy. The main difficulty for postpartum individuals was scheduling appointments and/or exams. Having antenatal care in 2022, no reports of difficulty in access, and follow-up at a high-risk unit were associated with antenatal adequacy.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo72
26% of all pregnancies end in miscarriage, and up to 10% of clinically diagnosed pregnancies, and recurrent pregnancy loss is 5% among couples of childbearing ages. Although there are several known causes of pregnancy loss in the first half, including recurrent pregnancy loss, including parental chromosomal abnormalities, uterine malformations, endocrinological disorders, and immunological abnormalities, about half of the cases of pregnancy loss in its first half remain unexplained.
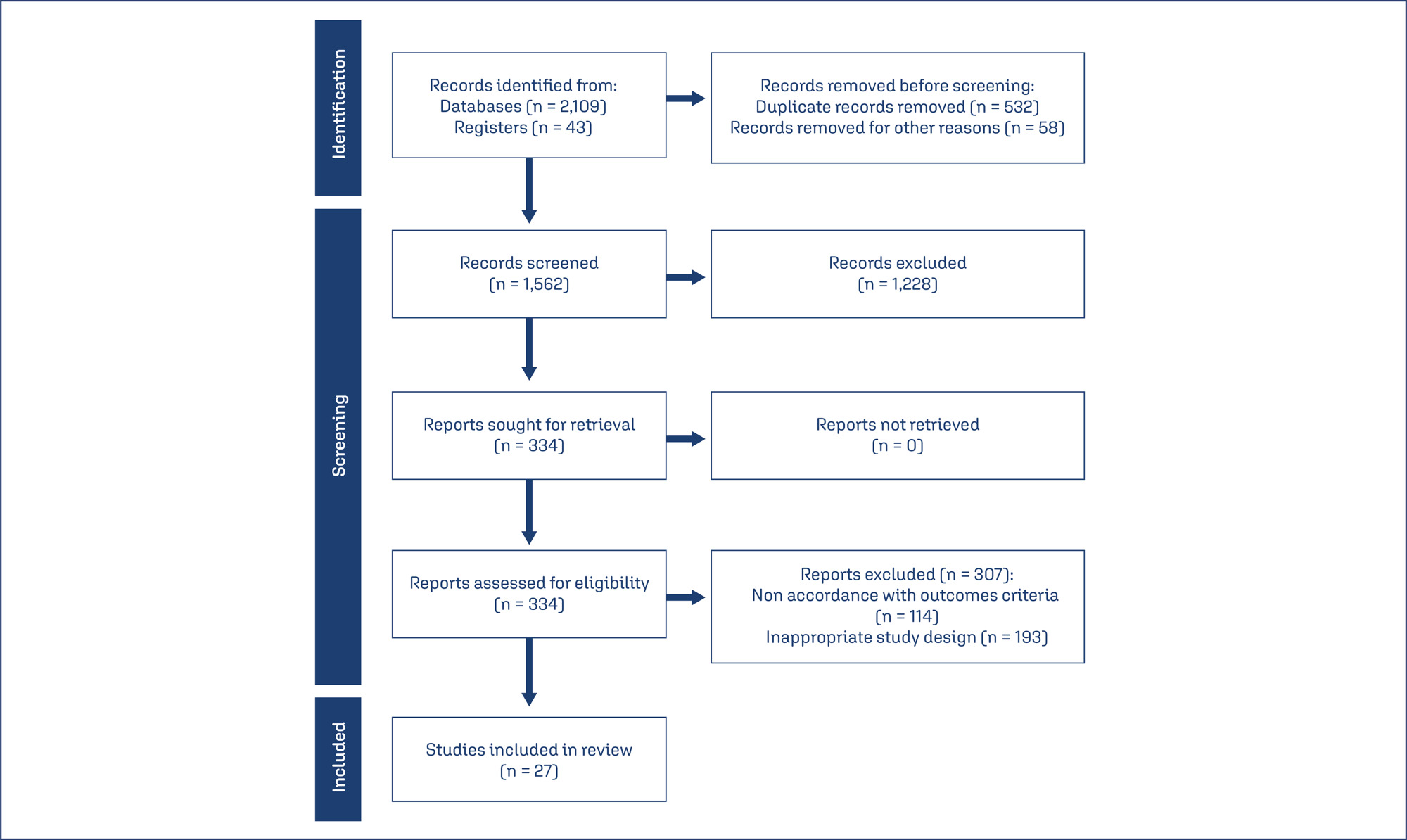
The review includes observational controlled studies (case-control or cohort, longitudinal studies, reviews, meta-analyses), which include the study of biochemical factors for predicting pregnancy losses in the first half, in singlet pregnancy. The Newcastle-Ottawa Scale (NOS) was used to assess the research quality.
Finally, 27 studies were included in the review, which has 134904 examined patients. The results of the review include estimates of β-human chorionic gonadotropin, progesterone, pregnancy-associated protein – A, angiogenic vascular factors, estradiol, α-fetoprotein, homocysteine and CA-125 as a predictors or markers of the first half pregnancy losses.
It may be concluded that to date, research data indicate the unavailability of any reliable biochemical marker for predicting pregnancy losses in its first half and require either a combination of them or comparison with clinical evidence. A fairly new model shall be considered for the assessment of α-fetoprotein in vaginal blood, which may have great prospects in predicting spontaneous miscarriages.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo22
RhD alloimmunization in pregnancy is still the main cause of hemolytic disease of the fetus and neonate (HDFN). Nevertheless, there are other antigens that may be associated with the occurrence of this phenomenon and that have been growing in proportion, given that current prevention strategies focus only on anti-RhD antibodies. Although not widespread, the screening and diagnostic management of the disease caused by these antibodies has recommendations in the literature. For this reason, the following review was carried out with the objective of listing the main red blood cell antigen groups described — such as Rh, ABO, Kell, MNS, Duffy, Kidd, among others — addressing the clinical importance of each one, prevalence in different countries, and recommended management when detecting such antibodies during pregnancy.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo58
To assess a panel of cytokines and placental insufficiency with the risk of preterm delivery (PTD).
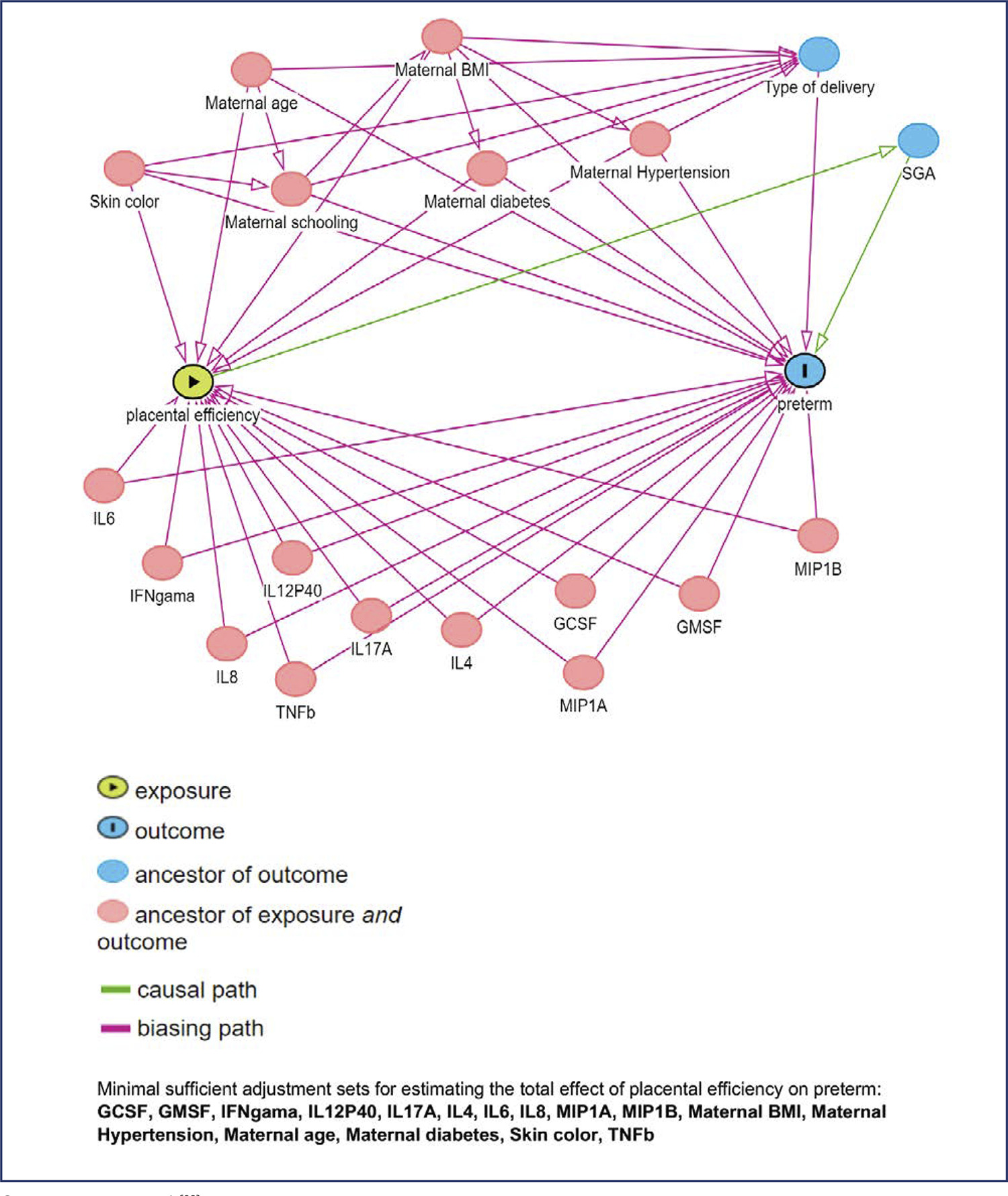
Nested case-control study into the BRISA birth cohort. Eighty-two mother-infant-placenta pairs were selected at 20+0 to 25+6 weeks. Circulating biomarker levels were performed using Luminex flowmetric xMAP technology. Cytokines classified as Th1, Th2 or Th17 and other biomarkers were selected. The ratio between birth weight and placental weight (BW/PW) was used as a proxy for placental efficiency. Spearman correlation, univariate analyses and logistic regression models were calculated. Sensitivity, specificity, positive and negative likelihood ratios were calculated using the Receiver Operating Characteristic curve.
Mean gestational age was 250 days, 14,6% were small for gestational age, 4,8% large for gestational age and 13,4% stunted. Placental efficiency was higher for term newborns (p<0,001), and 18/22 (81%) preterm biomarker values were higher than the control group. Th1 cytokines were highly correlated, while the weakest correlation was observed in other biomarkers. Less education was associated with a higher risk of PTD (p = 0.046), while there was no appreciable difference in the risk of PTD for placental insufficiency. Biomarkers showed negligible adjusted OR of PTD (0.90 to 1.02). IL-6, IL-8, IL-1β, TNFβ, IL-4, IL-13, GCSF, MIP1A, VEGF, EGF, and FGF2 presented a higher sensitivity ranging from 75.56% to 91.11%.
IL-8, IL-12p40, IL-4, IL-13, GCSF, MIP1B, and GMSF in asymptomatic pregnant women were associated with PTD. This finding suggests an activation of maternal inflammatory response.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo53
To evaluate the risk factors for postpartum hemorrhage (PPH) according to the Robson Classification in a low-risk maternity hospital.
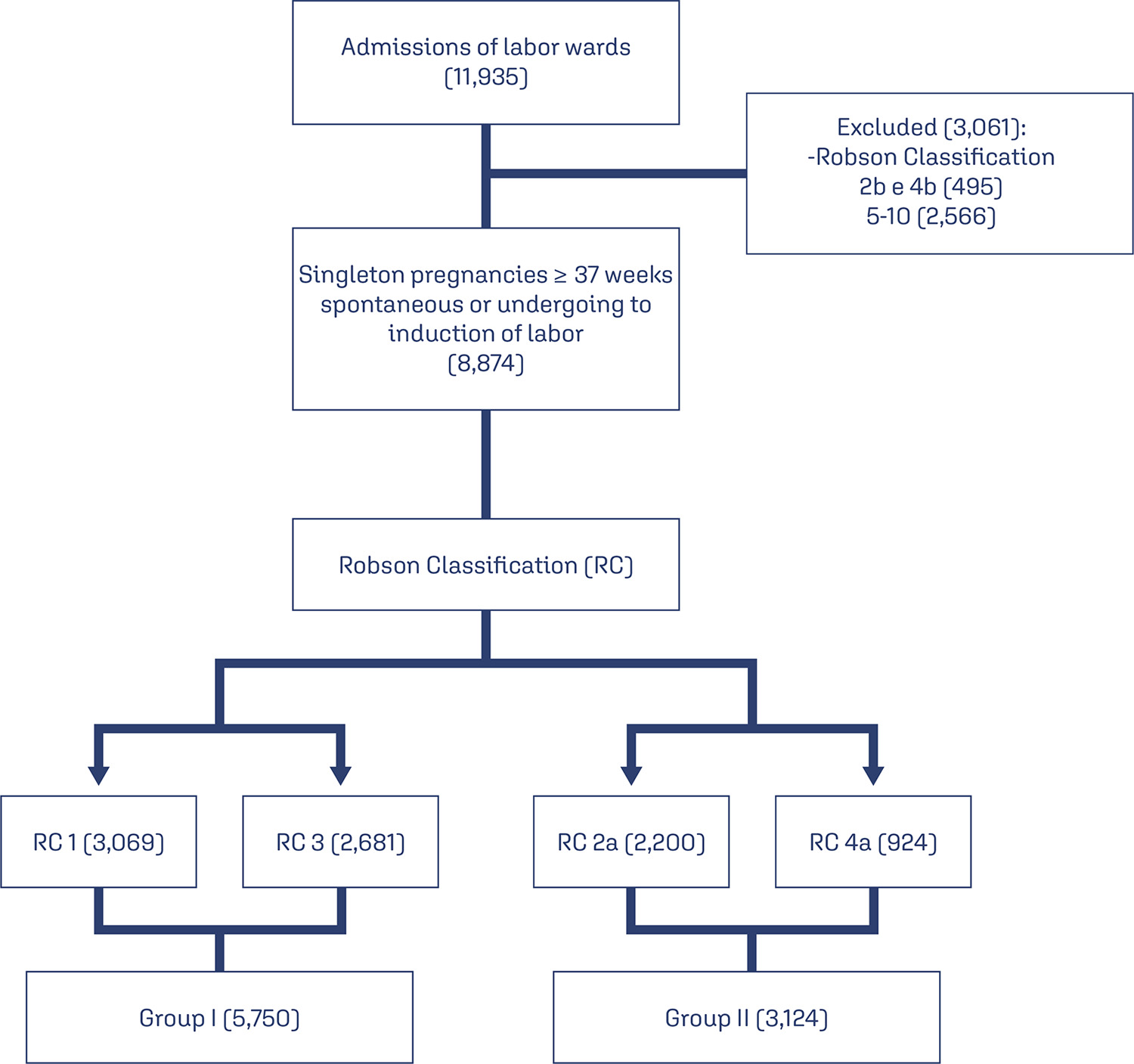
We conducted retrospective cohort study by analyzing the medical records of pregnant women attended in a low-risk maternity hospital, during from November 2019 to November 2021. Variables analyzed were: maternal age, type of delivery, birth weight, parity, Robson Classification, and causes of PPH. We compared the occurrence of PPH between pregnant women with spontaneous (Groups 1 and 3) and with induction of labor (2a and 4a). Chi-square and Student t-tests were performed. Variables were compared using binary logistic regression.
There were 11,935 deliveries during the study period. According to Robson’s Classification, 48.2% were classified as 1 and 3 (Group I: 5,750/11,935) and 26.1% as 2a and 4a (Group II: 3,124/11,935). Group II had higher prevalence of PPH than Group I (3.5 vs. 2.7%, p=0.028). Labor induction increased the occurrence of PPH by 18.8% (RR: 1.188, 95% CI: 1.02-1.36, p=0.030). Model including forceps delivery [x2(3)=10.6, OR: 7.26, 95%CI: 3.32-15.84, R2 Nagelkerke: 0.011, p<0.001] and birth weight [x2(4)=59.0, OR: 1.001, 95%CI:1.001-1.001, R2 Nagelkerke: 0.033, p<0.001] was the best for predicting PPH in patients classified as Robson 1, 3, 2a, and 4a. Birth weight was poor predictor of PPH (area under ROC curve: 0.612, p<0.001, 95%CI: 0.572-0.653).
Robson Classification 2a and 4a showed the highest rates of postpartum hemorrhage. The model including forceps delivery and birth weight was the best predictor for postpartum hemorrhage in Robson Classification 1, 3, 2a, and 4a.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo47
In Brazil, postpartum hemorrhage (PPH) is a major cause of maternal morbidity and mortality. Data on the profile of women and risk factors associated with PPH are sparse. This study aimed to describe the profile and management of patients with PPH, and the association of risk factors for PPH with severe maternal outcomes (SMO).
A cross-sectional study was conducted in Instituto de Medicina Integral Prof. Fernando Figueira (IMIP) obstetric intensive care unit (ICU) between January 2012 and March 2020, including patients who gave birth at the hospital and that were admitted with PPH to the ICU.
The study included 358 patients, of whom 245 (68.4%) delivered in the IMIP maternity, and 113 (31.6%) in other maternity. The mean age of the patients was 26.7 years, with up to eight years of education (46.1%) and a mean of six prenatal care. Uterine atony (72.9%) was the most common cause, 1.6% estimated blood loss, 2% calculated shock index (SI), 63.9% of patients received hemotransfusion, and 27% underwent hysterectomy. 136 cases of SMO were identified, 35.5% were classified as maternal near miss and 3.0% maternal deaths. Multiparity was associated with SMO as an antepartum risk factor (RR=1.83, 95% CI1.42-2.36). Regarding intrapartum risk factors, abruptio placentae abruption was associated with SMO (RR=2.2 95% CI1.75-2.81). Among those who had hypertension (49.6%) there was a lower risk of developing SMO.
The principal factors associated with poor maternal outcome were being multiparous and placental abruption.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo52
To analyze the death of Brazilian pregnant and postpartum women due to COVID-19 or unspecific cause.
This is retrospective, descriptive-exploratory, population-based study carried out with the Sistema de Informação de Vigilância Epidemiológica da Gripe (SIVEP-Gripe) database, with pregnant and postpartum women of reproductive age who died from confirmed COVID-19 between 2020 and 2021. The chosen variables were: age, gestational period, type and number of comorbidities, skin color, using the statistical software R Foundation for Statistical Computing Platform, version 4.0.3 and Statistical Package for Social Science, version 29.0 for analysis.
A total of 19,333 cases of pregnant and postpartum women aged between 10 and 55 years diagnosed with SARS were identified, whether due to confirmed COVID-19 or unspecific causes. Of these, 1,279 died, these cases were classified into two groups according to the cause of death: deaths from COVID-19 (n= 1,026) and deaths from SARS of unspecific cause (n= 253).
The risk of death increased among black and brown women, in the postpartum period and with the presence of comorbidities, mainly diabetes, cardiovascular diseases and obesity. The data presented here draw attention to the number of deaths from SARS, especially among sociodemographic profiles, precarious access to health, such as the black population. In addition, limitations in adequate access to health care are reinforced by even lower rates of ICU admissions among women who died from SARS of an unspecified cause.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo28
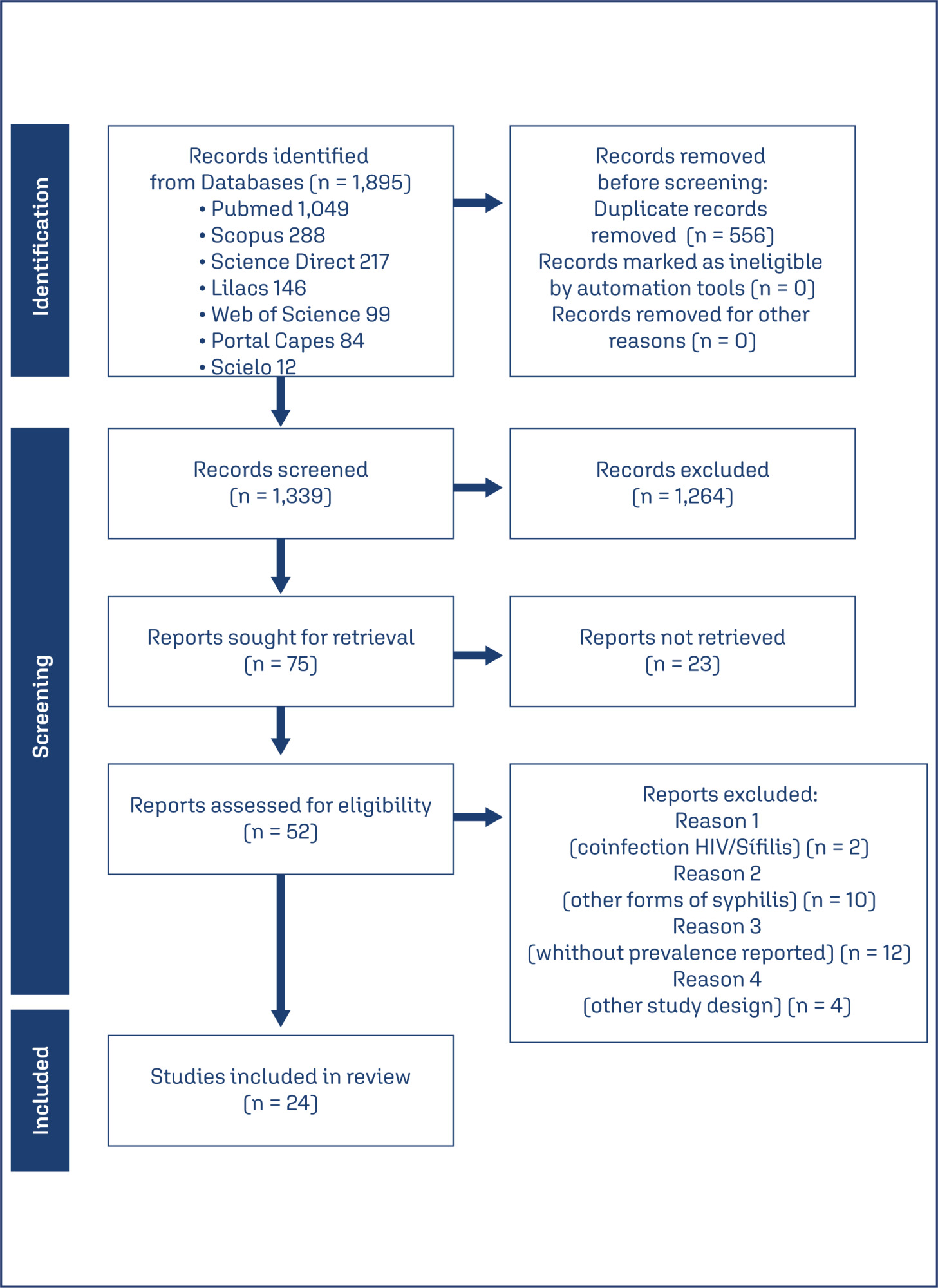
This systematic review accompanied by a meta-analysis aimed to estimate the prevalence of syphilis in pregnant women in Brazil and describe its associated factors.
Following the establishment the search strategies and the registration of the review protocol in PROSPERO, we conducted a search for relevant articles in the Pubmed, LILACS, Science Direct, SciELO and Web of Science databases. Our inclusion criteria were cross-sectional studies published between 2005 and 2023, with no language restrictions. The combined prevalence of syphilis infection was estimated using the random effects model in the R Software with a 95% confidence interval (95% CI) and p < 0.01 as statistically significant.
A total of 24 articles were recruited, which together investigated 221,884 women. The combined prevalence of syphilis in pregnant women in Brazil was 1.79% (95% CI: 1.24-2.57%), and the main factors associated with its occurrence were black and brown skin color, low education and factors related to the partner.
There was a high prevalence of syphilis in pregnancy in Brazil, mainly associated with socioeconomic factors.