Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(3):121-126
To assess the management chosen by gynecologists after atypical squamous cells (ASCs) cytology results, and to evaluate the outcomes of these cases in Brazilian women.
A prospective observational study evaluated the initial management offered by the gynecologist in the case of 2,458 ASCs cytology results collected between January of 2010 and July of 2016. The outcomes of the cytology, high-risk human papilloma virus (HR-HPV) test and histology were compared in two subgroups: atypical squamous cells of undetermined significance (ASC-US) and atypical squamous cells-cannot exclude high-grade squamous intraepithelial lesion (ASC-H).
In many cases of ASC-US (36.97%) and ASC-H (40.50%), no clinical actions were taken. Cytology was the most frequent follow-up chosen, including for cases of ASC-H, which goes against the conduct recommended in the national guideline. In women over 30 years of age, the period of time elapsed between an ASC-US result and a new cytology was in 13.03 months, in disagreement with the national guideline recommendations (p< 0.0001). Negative for intraepithelial lesions or malignancy (NILM) cytologic (p = 0.0026) and histologic (p = 0.0017) results in the follow-up were associated with prior ASC-US, while negative results for ASC-H were cytologically (p< 0.0001) and histologically associated with high-grade squamous intraepithelial lesion (HSIL) (p< 0.0001). Two invasive cervical carcinomas (ICCs) were found in the follow-up for ASC-H, and there was a statistically significant association (p = 0.0341). A positive HR-HPV test was associated with ASC-H (p = 0.0075).
The data suggest that even for a population of Brazilian women assisted at private clinics, the national guidelines recommendations for ASCs results are not followed.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(8):408-414
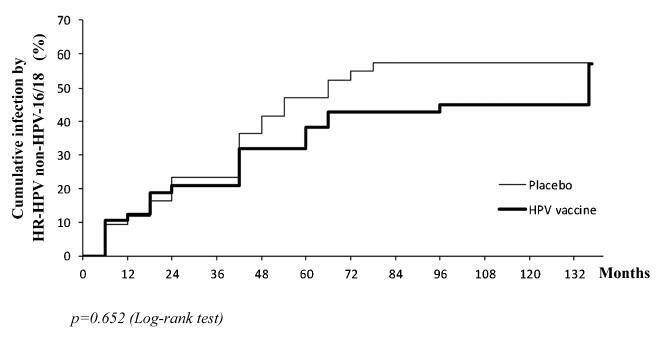
the aim of this study was to evaluate the pattern of human papillomavirus (HPV) detection in an 11.3-year post-vaccination period in a cohort of adolescent and young women vaccinated or not against HPV 16/18.
a subset of 91 women from a single center participating in a randomized clinical trial (2001-2010, NCT00689741/00120848/00518336) with HPV 16/18 AS04- adjuvanted vaccine was evaluated. All women received three doses of the HPV vaccine (n = 48) or a placebo (n = 43), and cervical samples were collected at 6-month intervals. Only in this center, one additional evaluation was performed in 2012. Up to 1,492 cervical samples were tested for HPV-DNA and genotyped with polymerase chain reaction (PCR). The vaccine group characteristics were compared by Chi-square or Fisher exact or Mann-Whitney test. The high-risk (HR)-HPV 6-month-persistent infection rate was calculated. The cumulative infection by HPV group was evaluated by the Kaplan-Meier method and the log-rank test.
the cumulative infection with any type of HPV in an 11.3-year period was 67% in the HPV vaccine group and 72% in the placebo group (p = 0.408). The longitudinal analysis showed an increase of 4% per year at risk for detection of HR-HPV (non-HPV 16/ 18) over time (p = 0.015), unrelated to vaccination. The cumulative infection with HPV 16/18 was 4% for the HPV vaccine group and 29% for the placebo group (p = 0.003). There were 43 episodes of HR-HPV 6-month persistent infection, unrelated to vaccination.
this study showed themaintenance of viral detection rate accumulating HR-HPV (non-HPV-16-18) positive tests during a long period post-vaccination, regardless of prior vaccination. This signalizes that the high number of HPV-positive testsmay be maintained after vaccination.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(9):471-476
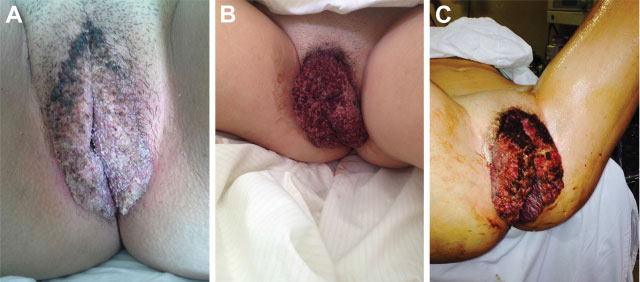
The Buschke-Loewenstein tumor is characterized by excessive growth of verrucous lesions on the genitals and/or perianal region. It is considered benign despite the high rate of recurrence and the possibility of malignant transformation. It is commonly associated with subtypes 6 and 11 of the human papillomavirus (HPV), and host 's immunity plays an important role in the development of the disease. Surgical excision is the recommended treatment in most cases. We present the case of a 16 years old female patient with extensive vulvar lesions successfully treated surgically.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(9):416-422
DOI 10.1590/SO100-720320140004995
The aim of this study was to evaluate the human papillomavirus genotypes and the frequency of multiple human papillomavirus infections, as well as to assess the association between human papillomavirus genotype, cyto-histopathological abnormalities and age range.
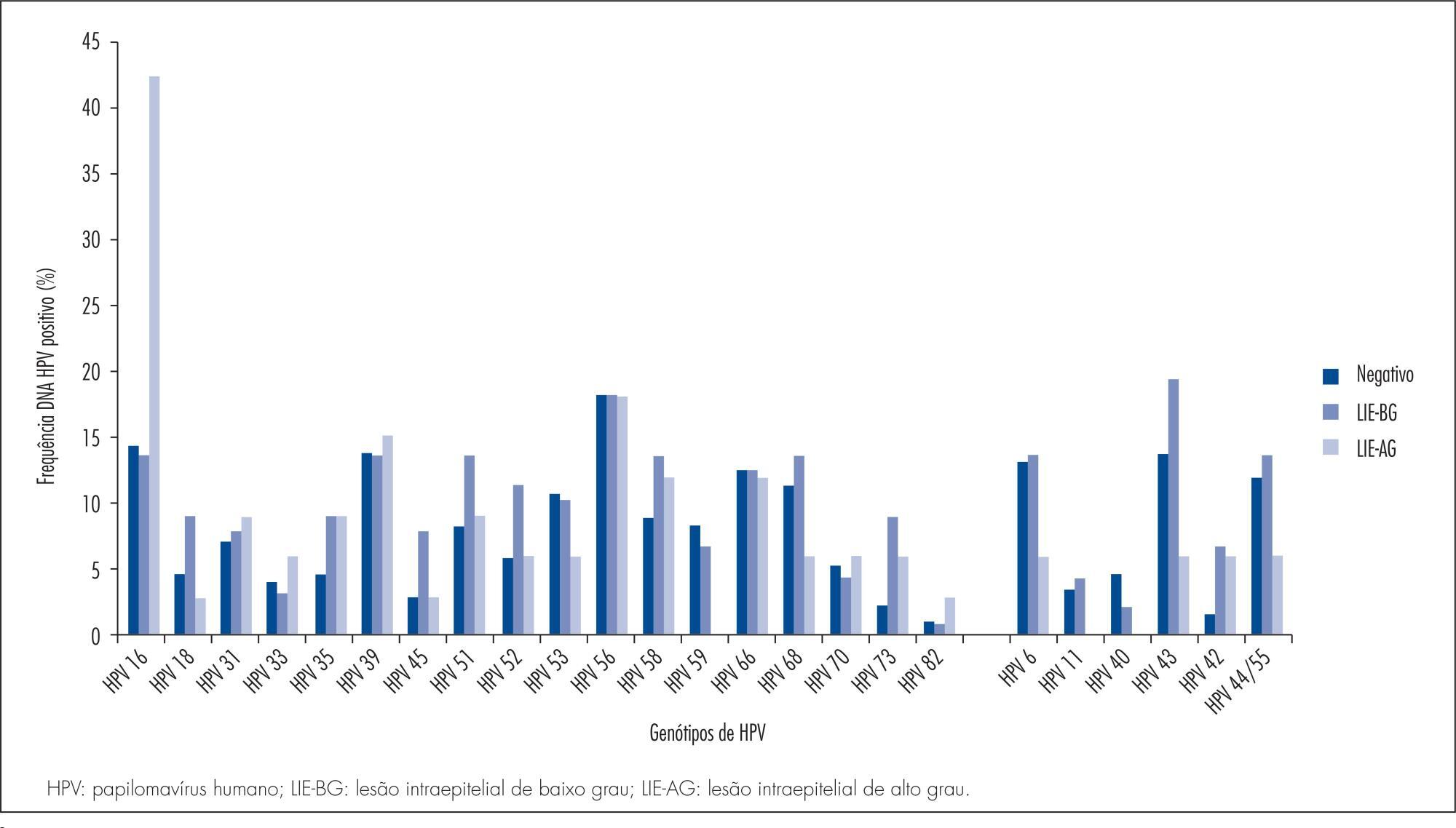
A retrospective cross-sectional study was carried out between June 2010 and October 2013 in Salvador, Bahia, Brazil. We analyzed 351 results of positive human papillomavirus genotyping performed using the PapilloCheck(r) test, designed to detect 24 human papillomavirus types. The cyto-histopathological abnormalities were classified as negative (negative cytology and histopathology), low-grade lesions (cytologic low-grade squamous intraepithelial lesion diagnosis or histopathologic cervical intraepithelial neoplasia 1 or vaginal intraepithelial neoplasia 1 diagnosis) and high-grade lesions (cytologic high-grade squamous intraepithelial lesion diagnosis or histopathologic cervical intraepithelial neoplasia 2+ or vaginal intraepithelial neoplasia 2+ diagnosis).
The most frequently detected high risk human papillomavirus genotype was HPBV 16, with 18.5%, 95% confidence interval (95%CI) 14.6-23.0, followed by HPV 56 (14%; 95%CI 10.5-18.0) and HPV 39 (13.4%; 95%CI 9.5-16.8). HPV 18 (5.4%; 95%CI 3.3-8.3) was among the least frequent types. Among the low risk types, HPV 42 (15.7%; 95%CI 12.0-20.0), HPV 6 (11.4%; 95%CI 8.3-15.2) and HPV 44/55 (11.1%; 95%CI 8.0-14.9) were the most frequent, while HPV 11 (2.8%; 95%CI 1.4-5.2) was the least common. The proportion of HPV 16-positive women increased with severity of cyto-histopathological abnormalities: 13.8% (12/87) in low-grade lesion and 42.4% (14/33) in high-grade lesion. There was association between low- or high-grade cyto-histopathological lesion and the high risk genotypes, HPV16, HPV 52, HPV 73 and HPV 82, and the low risk type, HPV 43. Women under 30 years showed a significantly higher frequency of HPV 16 (22.2 versus 12.9%, p =0.01), HPV 42 (19.7 versus 10.9%, p=0.01) and HPV 45 (6.6 versus 1.4%, p=0.01), and multiple human papillomavirus infections (58.1 versus 47.4%, p=0.04).
We observed variability of human papillomavirus genotype distribution in women from the state of Bahia. HPV 16 was the most frequently detected high risk human papillomavirus, as also reported for other geographic areas of Brazil and for the world in general. HPV 56 and HPV 39 were the second and the third most common genotypes, whereas HPV 18 was among the least frequent types. HPV 42, 6 and 44/55 were the most frequently detected low risk human papillomavirus, and HPV 11 was the least common.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):425-433
DOI 10.1590/S0100-72032005000700010
Cervical cancer is nowadays a disease amenable to secondary prevention. Methods for the detection of its precursor lesions and human papillomavirus infection, such as cervical cytology and molecular biology, achieved widespread use worldwide. However, there is still too much controversy regarding the use of these methods in gynecological practice. Which is the best examination or the best association of examinations, and the most adequate time intervals to proceed with screening, are still pending questions, generating anxiety in patients and doctors. On the other hand, the management of women who have been diagnosed with viral infection and/or cervical intraepithelial neoplasia is not yet consensual, and several factors may affect the clinical decision on how to treat them. Therapeutic options are dependent upon the type of viral infection, severity of the cervical intraepithelial neoplasia and its histological type. The aim of the present article was to review the several aspects of cervical cancer screening and its viable treatment.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(6):457-462
DOI 10.1590/S0100-72032004000600006
OBJECTIVE: to assess the ability of Pap smear and hybrid capture II (HCII) to detect clinically significant cervical lesions (CIN2/3) in women referred to hospital due to atypical squamous cells of unknown significance (ASCUS) or low-grade squamous intraepithelial lesions (LSIL). METHODS: a cross-sectional study comprising 161 women referred to the Taubaté University Hospital due to ASCUS/LSIL, between August 2000 and September 2002. All women responded to a questionnaire regarding sociodemographic and reproductive characteristics and were subjected to gynecological examination with specimen collection for Pap test and HCII, along with colposcopy and eventual cervical biopsy. The relationship between HCII results and age, use of condom, oral hormonal contraception, and smoking were evaluated by the chi-square test. The sensitivity, specificity, positive and negative predictive values of both Pap test and HCII were calculated. All calculations were performed within 95% confidence intervals. RESULTS: sixty-seven percent of the women that tested positive for HPV were less than 30 years old. Pap smear and HCII showed the same 82% sensitivity in detecting CIN2/3 when the threshold for a positive Pap result was ASCUS, LSIL or HSIL. Pap smear specificity and positive predictive values were substantially increased when only HSIL results were considered as positive (from 29 to 95% and 12 to 50%, respectively). These figures were superior to those of HCII, but at the expense of an expressive loss of sensitivity (from 82% to 41%). CONCLUSIONS: our results substantiate the potential of HCII in detecting CIN2/3 among women referred due to ASCUS/LSIL.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(4):289-294
DOI 10.1590/S0100-72032004000400004
OBJECTIVE: to study the relationship of biobehavioral factors, such as age, menarche, number of gestations, and age of first sexual intercourse, with changes in Langerhans'cells in women with negative hybrid capture for HPV. METHODS: thirty women referred due to abnormal cervical cytology or premalignant cervical lesions were studied and underwent colposcopy, guided biopsy and histopathological exams. The Langerhans' cells were identified by immunohistochemical (S100+) exams. Langerhans' cells visualized in brown color were counted using the software Cytoviewer. The nonparametric Wilcoxon rank-sum test was employed for statistical analysis. RESULTS: the number of Langerhans' cells in women who had menarche after 13 years old presented statistically significant difference (173.34 cell/mm²) compared to the group whose menarche occurred before 13 (271.41 cell/mm²). The age at the first sexual intercourse was associated with the low number of Langerhans' cells, 127.15 cell/mm² and 250.14 cell/mm², respectively, for the beginning of the sexual activity up to 17 years old and after 17 (p=0.03). Previous cauterizations of the uterine cervix have been related to a lower number of Langerhans' cells in the epithelium, with the average 120.30 cell/mm² as compared to 236.06 cell/mm² for those women who never underwent that procedure (p=0.05). Other factors such as the patient's age and the number of gestations showed no statistically significant differences in the density of Langerhans' cells. CONCLUSIONS: the present study reports the association of biobehavioral factors with decrease in the number of Langerhans' cell.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(4):277-287
DOI 10.1590/S0100-72032004000400003
OBJECTIVE: to compare the prevalence of DNA of human papillomavirus (HPV), in samples of normal endometrial tissue, and tissue with endometrial carcinoma of women submitted to surgical treatment (hysterectomy), or between endometrial carcinoma and benign disease, through the PCR technique. METHODS: this is an observational control-case study where 100 women (50 with endometrial carcinoma and 50 with normal endometrial tissue) were analyzed for the detection of HPV DNA in samples of endometrial tissue kept in paraffin blocks by the PCR technique. The cases of endometrial carcinoma with uncertain primary site of the lesion as well as the cases with previous or current history of pre-neoplasic lesions or carcinoma of the lower genital tract were excluded. Variables as age, smoking habit, endometrial trophism, squamous differentiation and degree of tumor differentiation were also evaluated. RESULTS: the estimated relative risk of the presence of HPV in the endometrial carcinoma and in the normal endometrial tissue was the same. HPV was detected in 8% of the cases of carcinoma and 10% in the normal endometrial tissue. In spite of HPV having been 3.5 times more detected in women with smoking habit in the group without carcinoma, there was no statistical difference. The presence of HPV was also not correlated with the women's age, endometrial trophism, squamous differentiation and degree of tumor differentiation. The HPV types 16 (5 cases) and 18 (4 cases) were the viruses most frequently found both in the normal endometrial tissue or in the tissue with carcinoma. No oncogenic low risk virus was detected in the samples. CONCLUSION: The same proportion of HPV is present in the endometrial tissue of women with endometrial cancer and with normal endometrium. It could not be demonstrated a possible correlation of DNA of HPV with the development of endometrial carcinoma.