Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo72
26% of all pregnancies end in miscarriage, and up to 10% of clinically diagnosed pregnancies, and recurrent pregnancy loss is 5% among couples of childbearing ages. Although there are several known causes of pregnancy loss in the first half, including recurrent pregnancy loss, including parental chromosomal abnormalities, uterine malformations, endocrinological disorders, and immunological abnormalities, about half of the cases of pregnancy loss in its first half remain unexplained.
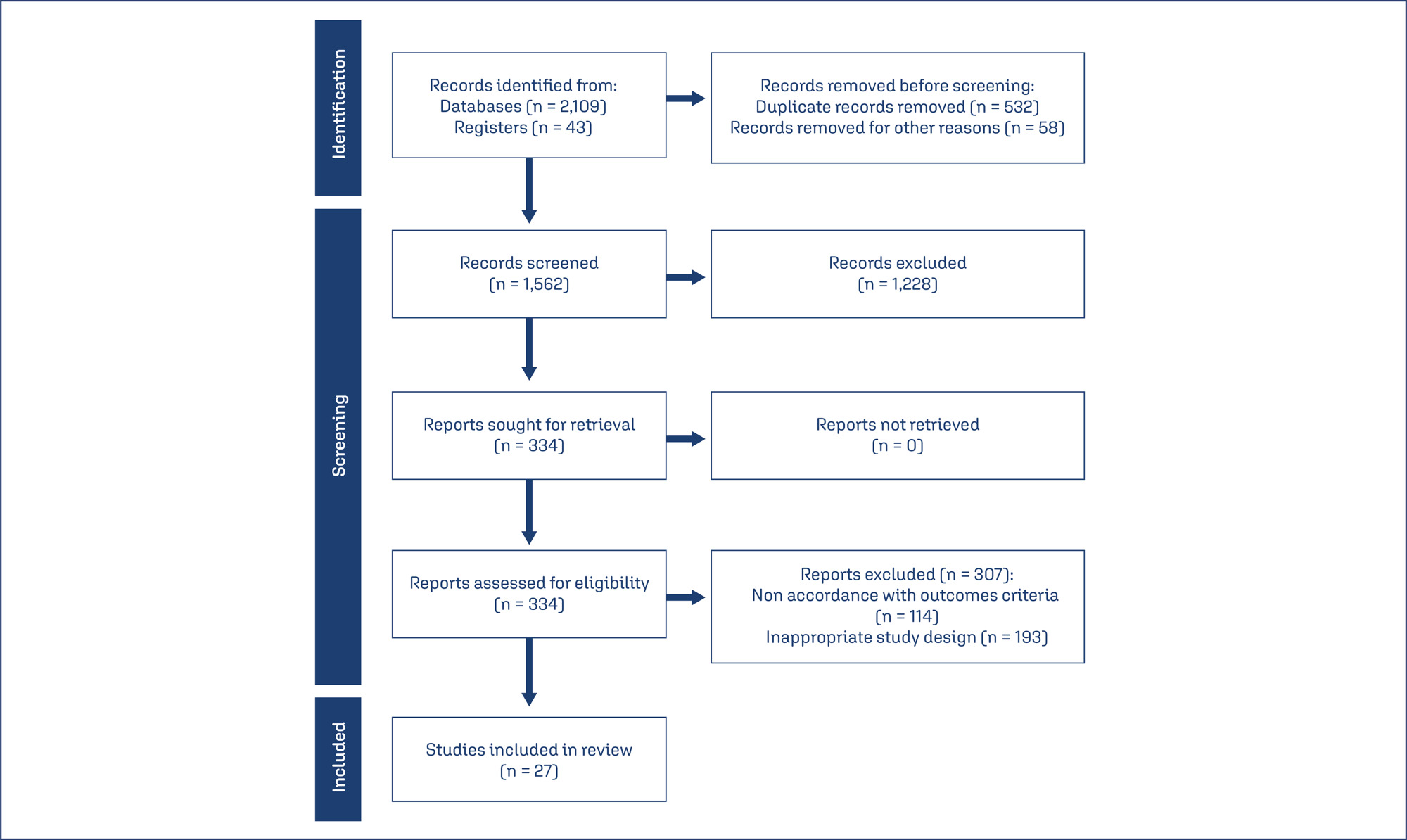
The review includes observational controlled studies (case-control or cohort, longitudinal studies, reviews, meta-analyses), which include the study of biochemical factors for predicting pregnancy losses in the first half, in singlet pregnancy. The Newcastle-Ottawa Scale (NOS) was used to assess the research quality.
Finally, 27 studies were included in the review, which has 134904 examined patients. The results of the review include estimates of β-human chorionic gonadotropin, progesterone, pregnancy-associated protein – A, angiogenic vascular factors, estradiol, α-fetoprotein, homocysteine and CA-125 as a predictors or markers of the first half pregnancy losses.
It may be concluded that to date, research data indicate the unavailability of any reliable biochemical marker for predicting pregnancy losses in its first half and require either a combination of them or comparison with clinical evidence. A fairly new model shall be considered for the assessment of α-fetoprotein in vaginal blood, which may have great prospects in predicting spontaneous miscarriages.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo74
This study aims to evaluate the clinical outcomes of surgical management for placenta accreta spectrum in a Latin American reference hospital specializing in this condition. The evaluation involves a comparison between surgeries performed on an emergent and scheduled basis.
A retrospective cohort study was conducted on patients with placenta accreta spectrum who underwent surgery between January 2011 and November 2021 at a hospital in Colombia, using data from the institutional PAS registry. The study included patients with intraoperative and/or histological confirmation of PAS, regardless of prenatal suspicion. Clinical outcomes were compared between patients who had emergent surgeries and those who had scheduled surgeries. Descriptive analysis involved summary measures and the Shapiro-Wilk test for quantitative variables, with comparisons made using Pearson’s Chi-squared test and the Wilcoxon rank sum test, applying a significance level of 5%.
A total of 113 patients were included, 84 (74.3%) of them underwent scheduled surgery, and 29 (25.6%) underwent emergency surgery. The emergency surgery group required more transfusions (72.4% vs 48.8%, p=0.047). Patients with intraoperative diagnosis of placenta accreta spectrum (21 women, 19.5%) had a greater volume of blood loss than patients taken into surgery with known presence of placenta accreta spectrum (3500 ml, IQR 1700 – 4000 vs 1700 ml, IQR 1195-2135. p <0.001).
Patients with placenta accreta spectrum undergoing emergency surgery require transfusions more frequently than those undergoing scheduled surgery
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo75
To identify the opinion of coordinators and members about the essential characteristics and to understand the research networks characteristics, to facilitate their implementation, sustainability and effectiveness so it can be replicated in low and middle-income countries.
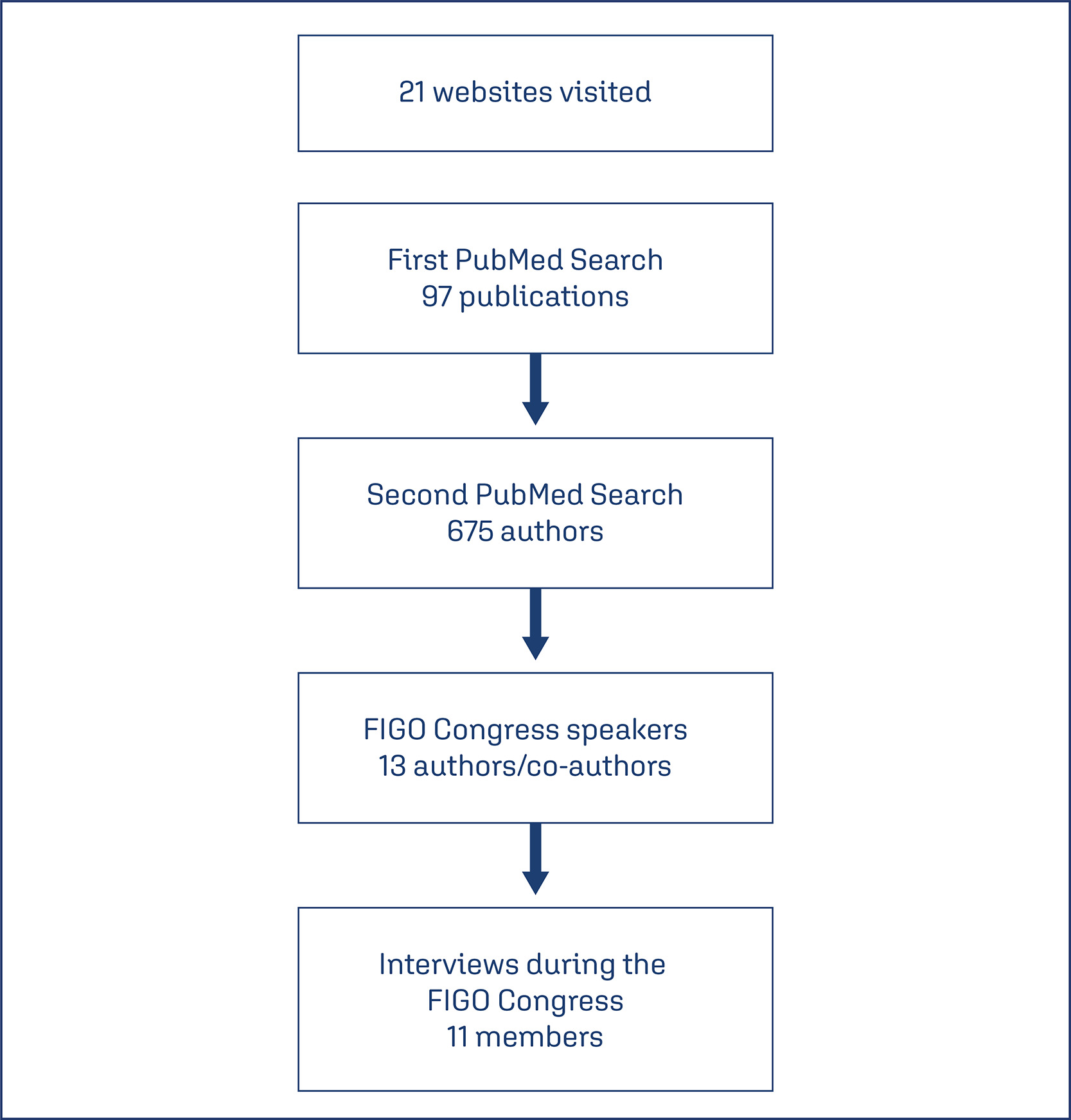
A qualitative study using a semi-structured interview technique was conducted. We selected potential members, managers and participants of networks from publications identified in PubMed. After checking the FIGO congress program, we identified authors who were assigned as speakers at the event. An invitation was sent and interviews were scheduled.
In total, eleven interviews were performed. Coordinators and members of networks have the same goal when they decide to participate in a network. In general, they cited that these individuals had to be committed, responsible and enthusiastic people. The network should be composed also of postgraduate students. A network should allow multi-leadership, co-responsibility, autonomy and empowerment of its members. Effective communication was mentioned as an important pillar for network maintenance. Another motivation is being an author or coauthor in publications. One way to maintain a network running is social or governmental commitment, after resources expire, studies continue.
Networks are different due to the social context where they are inserted, however, some characteristics are common to all of them, such as having engaged leaders. For an effective and sustainable network, commitment and motivation in a leader and members are more in need than financial resources. Ideally, to ensure the operation of the network, the institution where the leader is linked should support this network.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo76
To evaluate early complications in prepectoral breast reconstruction.
A retrospective cohort study including 180 consecutive cases of nipple-sparing mastectomy, comparing immediate breast reconstruction with subpectoral to prepectoral mammary implants in 2012-2022. Clinical and demographic characteristics and complications in the first three months following surgery were compared between the two techniques.
The prepectoral technique was used in 22 cases (12.2%) and the subpectoral in 158 (87.8%). Median age was higher in the prepectoral group (47 versus 43.8 years; p=0.038), as was body mass index (25.1 versus 23.8; p=0.002) and implant volume (447.5 versus 409 cc; p=0.001). The prepectoral technique was more associated with an inframammary fold (IMF) incision (19 cases, 86.4% versus 85, 53.8%) than with periareolar incisions (3 cases, 13.6% versus 73, 46.2%); (p=0.004). All cases in the prepectoral group underwent direct-to-implant reconstruction compared to 54 cases (34.2%) in the subpectoral group. Thirty-eight complications were recorded: 36 (22.8%) in the subpectoral group and 2 (9.1%) in the prepectoral group (p=0.24). Necrosis of the nipple-areola complex/skin flap occurred in 27 patients (17.1%) in the subpectoral group (prepectoral group: no cases; p=0.04). The groups were comparable regarding dehiscence, seroma, infection, and hematoma. Reconstruction failed in one case per group (p=0.230). In the multivariate analysis, IMF incision was associated with the prepectoral group (aOR: 34.72; 95%CI: 2.84-424.63).
The incidence of early complications was comparable between the two techniques and compatible with previous reports. The clinical and demographic characteristics differed between the techniques. Randomized clinical trials are required.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgoedt4
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo4
To classify the bibliometric indicators of online scientific research on placentophagy.
A bibliometric study was conducted to quantify the scientific production of authors and institutions with the aim of highlighting the growth and impact of these publications nationally and internationally. The Bradford Law, network maps, and textual statistics were used, with searches conducted in libraries and databases in October 2021.
The sample consisted of 64 articles, whose primary authors were associated with 49 institutions, and mostly with degrees in anthropology. The United States of America was the country that published the most papers on the theme, and most studies were reviews with individual production. Through the term analysis, it was found that the predominant themes regarding placentophagy were the following: Alternative therapy for women's health, methodologies used for research in this area, period of placenta ingestion (postpartum period), and its benefits.
The bibliometric indicators found are essential for the development of future research.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo6
BI-RADS® is a standardization system for breast imaging reports and results created by the American College of Radiology to initially address the lack of uniformity in mammography reporting. The system consists of a lexicon of descriptors, a reporting structure with final categories and recommended management, and a structure for data collection and auditing. It is accepted worldwide by all specialties involved in the care of breast diseases. Its implementation is related to the Mammography Quality Standards Act initiative in the United States (1992) and breast cancer screening. After its initial creation in 1993, four additional editions were published in 1995, 1998, 2003 and 2013. It is adopted in several countries around the world and has been translated into 6 languages. Successful breast cancer screening programs in high-income countries can be attributed in part to the widespread use of BI-RADS®. This success led to the development of similar classification systems for other organs (e.g., lung, liver, thyroid, ovaries, colon). In 1998, the structured report model was adopted in Brazil. This article highlights the pioneering and successful role of BI-RADS®, created by ACR 30 years ago, on the eve of publishing its sixth edition, which has evolved into a comprehensive quality assurance tool for multiple imaging modalities. And, especially, it contextualizes the importance of recognizing how we are using BI-RADS® in Brazil, from its implementation to the present day, with a focus on breast cancer screening.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo43
In low and middle-income countries such as Brazil, most maternal deaths are related to hypertensive complications. Preeclampsia is the leading cause of maternal mortality and morbidity. Significant proportion is associated with the following factors: lack of identification of high-risk women, lack of adequate prevention, difficulty in maintaining a high-risk prenatal follow-up, delayed diagnosis, insecurity and low use of magnesium sulphate, delayed pregnancy interruption and lack of postpartum follow-up of these high-risk cases. Four major actions are proposed to minimize this alarming clinical picture and reduce the mortality rates due to preeclampsia, called the "4 P Rule" (Adequate Prevention – Vigilant Prenatal Care – Timely Delivery (Parturition) – Safe Postpartum). From this simple "rule" we can open a range of important processes and reminders that may help in the guidance of preeclampsia management.