Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(7):315-316
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(7):315-319
DOI 10.159/S0100-720320140004977
To analyze associations between mammographic arterial mammary calcifications in menopausal women and risk factors for cardiovascular disease.
This was a cross-sectional retrospective study, in which we analyzed the mammograms and medical records of 197 patients treated between 2004 and 2005. Study variables were: breast arterial calcifications, stroke, acute coronary syndrome, age, obesity, diabetes mellitus, smoking, and hypertension. For statistical analysis, we used the Mann-Whitney, χ2 and Cochran-Armitage tests, and also evaluated the prevalence ratios between these variables and mammary artery calcifications. Data were analyzed with the SAS version 9.1 software.
In the group of 197 women, there was a prevalence of 36.6% of arterial calcifications on mammograms. Among the risk factors analyzed, the most frequent were hypertension (56.4%), obesity (31.9%), smoking (15.2%), and diabetes (14.7%). Acute coronary syndrome and stroke presented 5.6 and 2.0% of prevalence, respectively. Among the mammograms of women with diabetes, the odds ratio of mammary artery calcifications was 2.1 (95%CI 1.0-4.1), with p-value of 0.02. On the other hand, the mammograms of smokers showed the low occurrence of breast arterial calcification, with an odds ratio of 0.3 (95%CI 0.1-0.8). Hypertension, obesity, diabetes mellitus, stroke and acute coronary syndrome were not significantly associated with breast arterial calcification.
The occurrence of breast arterial calcification was associated with diabetes mellitus and was negatively associated with smoking. The presence of calcification was independent of the other risk factors for cardiovascular disease analyzed.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(7):315-316
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(6):315-321
DOI 10.1590/S0100-72031998000600004
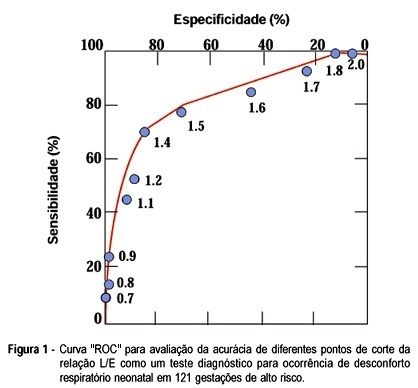
The objective was to evaluate the accuracy of the foam stability test, lecithin/sphingomyelin (LS) ratio, presence of phosphatidylglycerol (PG) and lung profile (L/S ratio > 1.7 and PG present simultaneously) in 121 consecutive high-risk gestations at the São Paulo Hospital from January 1990 to January 1995. Delivery occurred within 3 days of fetal lung maturation testing. This is a prospective study in which the sensitivity, specificity, positive (PPV) and negative predictive value (NPV) of all the tests were determined. Neonatal respiratory outcome and amniocentesis results were stratified by gestational age for comparison. The distribution of the studied population according to maternal pathology was diabetes mellitus (48), hypertensive disorders (41), Rh isoimmunization (14) and miscellaneous (18). Respiratory distress (RD) was present in 33 infants (27.2%), mainly in the diabetic group. There was no false negative using lung profile (all patients) and foam stability tests among hypertensive pregnancies (specificity 100%), but there were about 20% to 50% false positives in the other tests. Overall, all four tests had a low PPV: 23% for foam test, 51% for L/S ratio, 63% for PG, 61% for lung profile, and high NPV: 92% for foam test, 88% for L/S ratio, 89% for PG and 100% for lung profile. All tests had less accuracy in the diabetic pregnant women. This study shows that the presence of PG and L/S ratio > 1.7 in the amniotic fluid of high-risk pregnancies confirms maturity with a very low risk to develop RD and that the foam stability test was useful as a first-line test to predict the absence of surfactant-deficient respiratory distress syndrome, particularly in hypertensive pregnant women.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(5):315-320
DOI 10.1590/S0100-72032002000500005
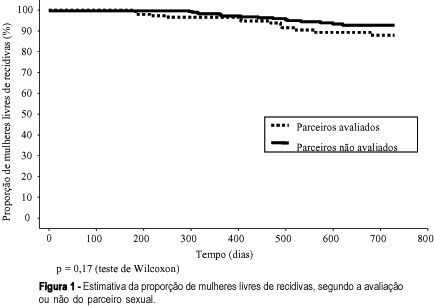
Purpose: to study the association between the evaluation or not of the male partner and relapses in women treated for HPV lesions. Methods: a reconstituted cohort study with 144 women with HPV lesions and whose partners had been evaluated, compared with 288 women whose partners had not been examined, controlled regarding date of attendance, age, lesion degree and treatment, attended between July 1993 and March 2000. We evaluated similarity between the groups, the association between the evaluation or not of the partners or the diagnosis of lesions with the occurrence and relapse lesion degree in the women and the disease-free interval (DFI). Results: the groups were similar regarding the control variables. Relapses occurred in 9.0 % of the women whose partners had been evaluated and in 5.9% of those whose partners had not been evaluated (p=0.23). When lesions were diagnosed in the men, 12.5% of their partners had relapses, against 7.3% of the women whose partners had no lesions (p=0.23), but there was no correlation with the relapse lesion degree and DFI. When the men reported a time of monogamous conjugal relationship <12 months, we observed 14.9% relapses in women, against 6.2% for the women whose partners reported a longer time (p=0.08). Conclusions: evaluation of the man did not decrease the relapse risk of HPV lesions in his partner. The presence of lesions in the male partners did not correlate with the occurrence and relapse degree in women and DFI. This study does not support the hypothesis that nonevaluated men would be an important cause of relapses in their partners.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2011;33(10):315-320
DOI 10.1590/S0100-72032011001000008
PURPOSE: to compare three methods for the detection of HPV infection and to determine the prevalence of the genotypes found. METHODS: a total of 120 cervical scrape samples from patients with cervical intraepithelial neoplasia were analyzed by the conventional polymerase chain reaction using the MY09/11 and GP05+/06+ primers, and by the Nested polymerase chain reaction. The samples were subjected to DNA amplification with the GH20 and PC04 primers (β-globin) to verify DNA quality and also by polymerase chain reaction and Nested polymerase chain reaction. The amplicons were visualized in 1.2% agarose gel stained with Blue Green Loading Dye I. Positive samples also were sequenced using the automatic DNA sequencer "MegaBACE 1000". The Χ2 and Fisher tests were used for statistical analysis with the level of significance set at 5%. RESULTS: fifteen samples were eliminated from the study because they failed to amplify the β-globin gene. Of the remaining samples, 40% (42/105) were positive using primers MY09/11, 98% (103/105) using primers GP05+/06+, and 92% (97/105) using Nested-PCR. With the MY09/11 and GP05+/06+ techniques, it was possible to obtain 100% HPV-positive samples. In this study, the prevalence of the genotypes found was 57, 23, 5, 4 and 3% for HPV genotypes 16, 18, 31, 33 and 56, respectively. HPVs 67 and 83 were present in 2%, and genotypes 6, 11, 58 and candHPV85 were present in 1% each. The prevalence of the more common genotypes (HPV 16 and 18) in this study agrees with that reported worldwide (IC95%=0.4657-0.8976). CONCLUSIONS: to obtain more reliable results, it is necessary the use of more than one primer system to detect HPV infections. We believe that the three techniques studied are important and suitable for the clinical diagnosis of HPV, when they are appropriately combined.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(7):315-320
DOI 10.1590/S0100-72032010000700002
PURPOSE: to determine the prevalence of HPV 16, 18, 31 and 45 in cervical screening samples of women with cellular changes and/or colposcopy suggestive of persistent high grade or low grade lesion who were submitted to conization. METHODS: a total of 120 women were included in the study. Histological analysis of the cervical cones revealed 7 cases of cervicitis, 22 of CIN1, 31 of CIN2, 54 of CIN3, and 6 invasive carcinomas. The cervical screening samples were analyzed before conization for the presence of HPV-DNA by PCR using the consensus primers PGMY09/11. HPV-DNA-positive samples were tested for the presence of HPV16, 18, 31 and 45 using type-specific primers for these HPV. RESULTS: HPV-DNA was detected in 67.5% of the studied women. HPV 16 (40%) was the most prevalent type in most ilesions, followed by HPV 31 (13.3%), 45 (13.3%), and 18 (4.1%). Multiple infections occurred in 15% of the cases and infections with other HPV types were detected in 14% of the sample. CONCLUSIONS: HPV 16 and 18 infections do not always occur as a single infection, and may be associated with other HPV types on different occasions.
