Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo44
To describe Top-hat results and their association with margin status and disease relapse in a referral facility in Brazil.
A retrospective study of 440 women submitted to LEEP to treat HSIL, in which 80 cases were complemented immediately by the top hat procedure (Top-hat Group - TH). TH Group was compared to women not submitted to Top-hat (NTH). The sample by convenience included all women that underwent LEEP from January 2017 to July 2020. The main outcome was the histological result. Other variables were margins, age, transformation zone (TZ), depth, and relapse. The analysis used the Chi-square test and logistic regression.
The TH Group was predominantly 40 and older (NTH 23.1% vs. TH 65.0%, p<0.001). No difference was found in having CIN2/CIN3 as the final diagnosis (NTH 17.0% vs. TH 21.3%, p=0.362), or in the prevalence of relapse (NTH 12.0% vs. TH 9.0%, p=0.482). Of the 80 patients submitted to top hat, the histological result was CIN2/CIN3 in eight. A negative top hat result was related to a negative endocervical margin of 83.3%. A CIN2/CIN3 Top-hat result was related to CIN2/CIN3 margin in 62.5% (p=0.009). The chance of obtaining a top hat negative result was 22.4 times higher (2.4-211.0) when the endocervical margin was negative and 14.5 times higher (1.5-140.7) when the ectocervical margin was negative.
The top hat procedure did not alter the final diagnosis of LEEP. No impact on relapse was observed. The procedure should be avoided in women of reproductive age.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo45
To explore women's experiences with postpartum intrauterine device (PPIUD) insertion and the decision-making process in the postpartum period.
A qualitative design was employed with face-to-face interviews using a semi-structured script of open questions. The sample was intentionally selected using the concept of theoretical information saturation.
Interviews were conducted (1) in the immediate postpartum period, and (2) in the postpartum appointment. 25 women (N = 25) over 18 years old who had a birth followed by PPIUD insertion were interviewed between October 2021 and June 2022. Three categories were constructed: (1) Choice process, (2) Relationship with the health team at the time of birth and the postpartum period, and (3) To know or not to know about contraception, that is the question.
Professionals’ communication management, popular knowledge, advantages of the PPIUD and the moment PPIUD is offered play a fundamental role in the construction of knowledge about the IUD. Choice process did not end in the insertion.

Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo38
This meta-analysis of randomized controlled trials (RCTs) aimed to update evidence on the effectiveness and safety of laser therapy for treating genitourinary syndrome of menopause (GSM).
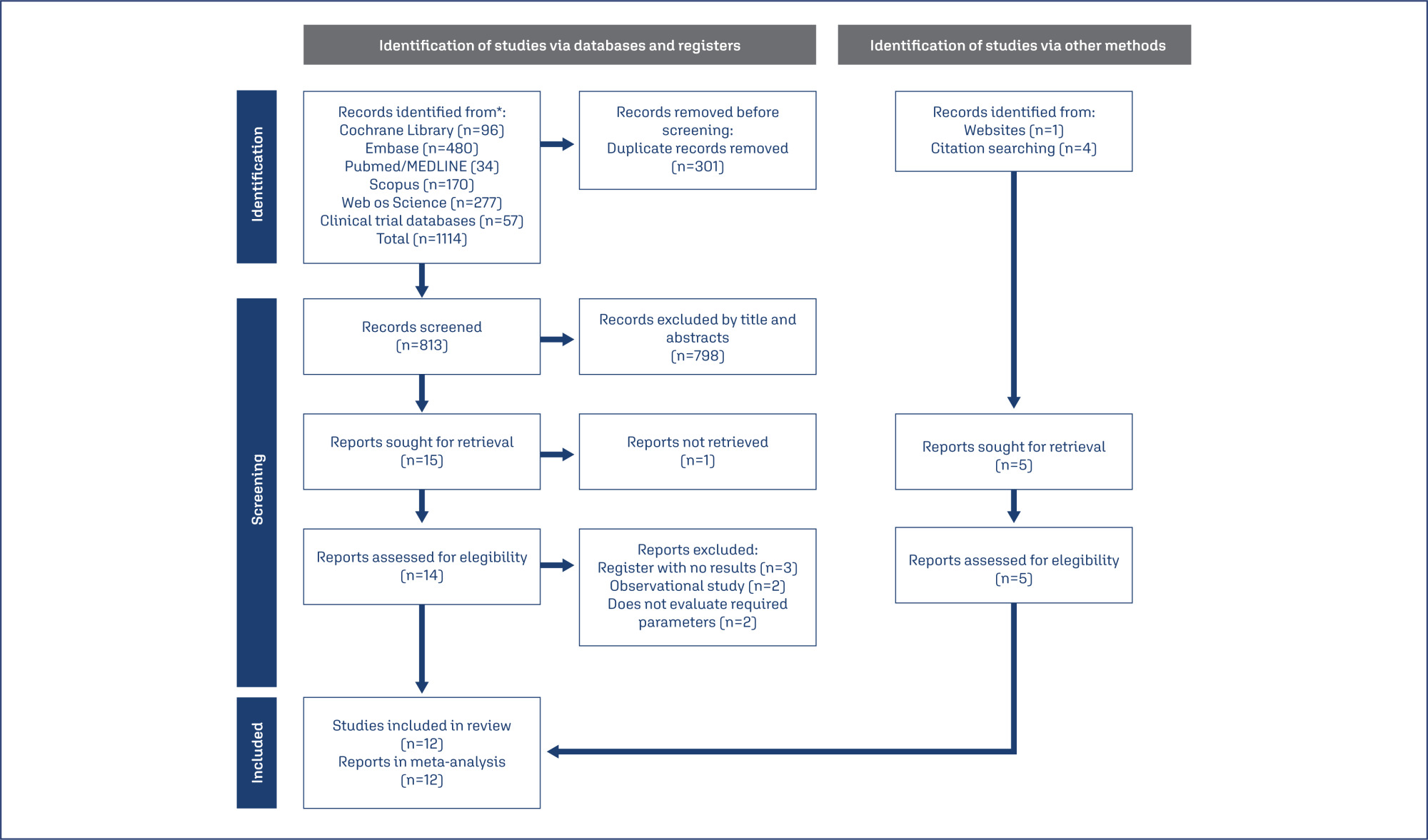
Manuscripts published until May 2023 were systematically searched in PubMed; Embase; Scopus; Web of Science; CENTRAL; CINAHL; and clinical trial databases (www.trialscentral.org, www.controlled-trials.com, and clinicaltrials.gov), with no language and year of publication restriction.
RCTs with women diagnosed with GSM, and the intervention was vaginal laser therapy (CO2-laser or Er: YAG-laser) comparing with placebo (sham therapy), no treatment or vaginal estrogen therapy.
Two authors evaluated the publications for inclusion based on the title and abstract, followed by reviewing the relevant full-text articles. Disagreements during the review process were addressed by consensus, with the involvement of a third author.
Twelve RCTs, representing a total of 5147 participants, were included in this review. Vaginal health index (VHI) significantly improved in the carbon dioxide laser (CO2-laser) therapy group (MD=2.21; 95% CI=1.25 to 3.16), while dyspareunia (MD=−0.85; 95% CI=−1.59 to −0.10), dryness (MD=−0.62; 95% CI=−1.12 to −0.12) and burning (MD= −0.64; 95% CI=−1.28 to −0.01) decreased. No serious adverse effects were reported.
CO2-laser increases VHI score and decreases dyspareunia, dryness and burning, especially when compared to sham-laser. However, the certainty of the evidence is low, thus preventing the recommendation of laser therapy for GSM management.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo40
To evaluate and compare the sexual function and pelvic floor muscles (PFM) function of women with endometriosis and chronic pelvic pain (CPP) with and without Myofascial Pelvic Pain Syndrome (MPPS).
Cross-sectional study conducted between January 2018 and December 2020. Women with deep endometriosis underwent assessments for trigger points (TP) and PFM function using the PERFECT scale. Electromyographic activity (EMG) and sexual function through Female Sexual Function Index (FSFI) were assessed. Statistical analyses included chi-square and Mann-Whitney tests.
There were 46 women. 47% had increased muscle tone and 67% related TP in levator ani muscle (LAM). Weakness in PFM, with P≤2 was noted in 82% and P≥3 in only 17%. Incomplete relaxation of PFM presented in 30%. EMG results were resting 6.0, maximal voluntary isometric contraction (MVIC) 61.9 and Endurance 14.2; FSFI mean total score 24.7. We observed an association between increased muscle tone (P<.001), difficulty in relaxation (P=.019), and lower Endurance on EMG (P=.04) in women with TP in LAM. Participants with TP presented lower total FSFI score (P=.02). TP in the right OIM presented increased muscle tone (P=.01). TP in the left OIM presented lower values to function of PFM by PERFECT (P=.005), and in MVIC (P=.03) on EMG.
Trigger points (TP) in pelvic floor muscles (PFM) and obturator internus muscle (OIM) correlates with poorer PFM and sexual function, particularly in left OIM TP cases. Endometriosis and chronic pelvic pain raise muscle tone, weaken muscles, hinder relaxation, elevate resting electrical activity, lower maximum voluntary isometric contraction, and reduce PFM endurance.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo41
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo64
To evaluate whether there were differences in the presentation of patients with tubal ectopic pregnancy (EP) during the first year of the COVID-19 pandemic.
We performed a retrospective cohort study of all cases of tubal EP between March 2019 and March 2020 (pre-pandemic) and between March 2020 and March 2021 (pandemic). We compared between these two groups the risk factors, clinical characteristics, laboratory data, sonographic aspects, treatment applied and complications.
We had 150 EP diagnoses during the two years studied, of which 135 were tubal EP. Of these, 65 were included in the pre-pandemic and 70 in the pandemic period. The prevalence of lower abdominal pain was significantly higher in the pandemic compared to the pre-pandemic period (91.4% vs. 78.1%, p=0.031). There was no significant difference in shock index, initial beta-hCG level, hemoglobin level at diagnosis, days of menstrual delay, aspect of the adnexal mass, amount of free fluid on ultrasound, and intact or ruptured presentation between the groups. Expectant management was significantly higher during the pandemic period (40.0% vs. 18.5%, p=0.008), surgical management was lower during the pandemic period (47.1% vs. 67.7%, p=0.023), and number of days hospitalized was lower in the pandemic period (1.3 vs. 2.0 days, p=0.003).
We did not observe a significant difference in patient history, laboratory and ultrasound characteristics. Abdominal pain was more common during the pandemic period. Regarding treatment, we observed a significant increase in expectant and a decrease in surgical cases during the pandemic period.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgoedt3
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo28
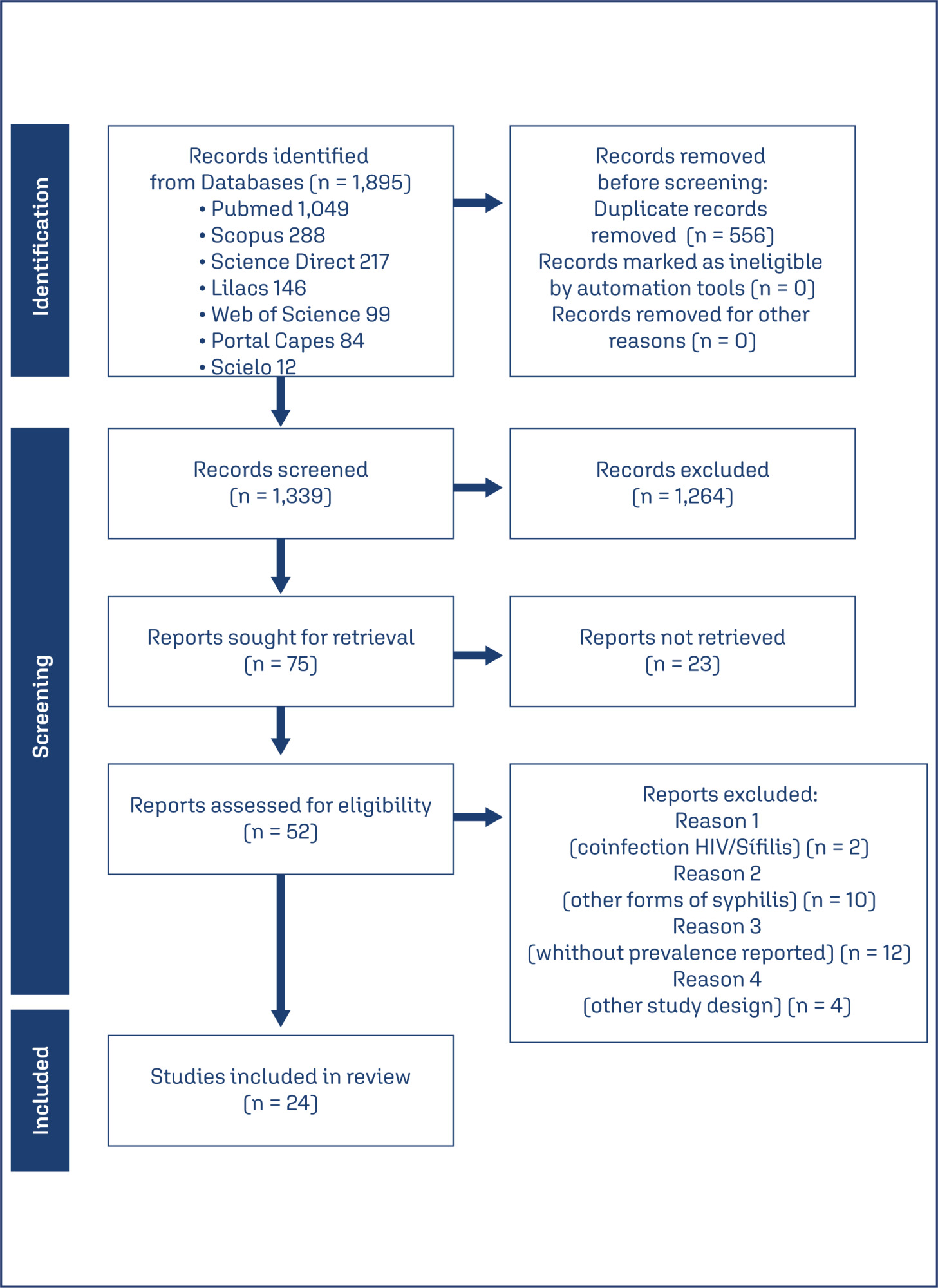
This systematic review accompanied by a meta-analysis aimed to estimate the prevalence of syphilis in pregnant women in Brazil and describe its associated factors.
Following the establishment the search strategies and the registration of the review protocol in PROSPERO, we conducted a search for relevant articles in the Pubmed, LILACS, Science Direct, SciELO and Web of Science databases. Our inclusion criteria were cross-sectional studies published between 2005 and 2023, with no language restrictions. The combined prevalence of syphilis infection was estimated using the random effects model in the R Software with a 95% confidence interval (95% CI) and p < 0.01 as statistically significant.
A total of 24 articles were recruited, which together investigated 221,884 women. The combined prevalence of syphilis in pregnant women in Brazil was 1.79% (95% CI: 1.24-2.57%), and the main factors associated with its occurrence were black and brown skin color, low education and factors related to the partner.
There was a high prevalence of syphilis in pregnancy in Brazil, mainly associated with socioeconomic factors.