You searched for:"Gustavo Arantes Rosa Maciel"
We found (9) results for your search.-
Febrasgo Position Statement
Hyperprolactinemia in women: diagnostic approach
Rev Bras Ginecol Obstet. 2024;46:e-FPS04
Summary
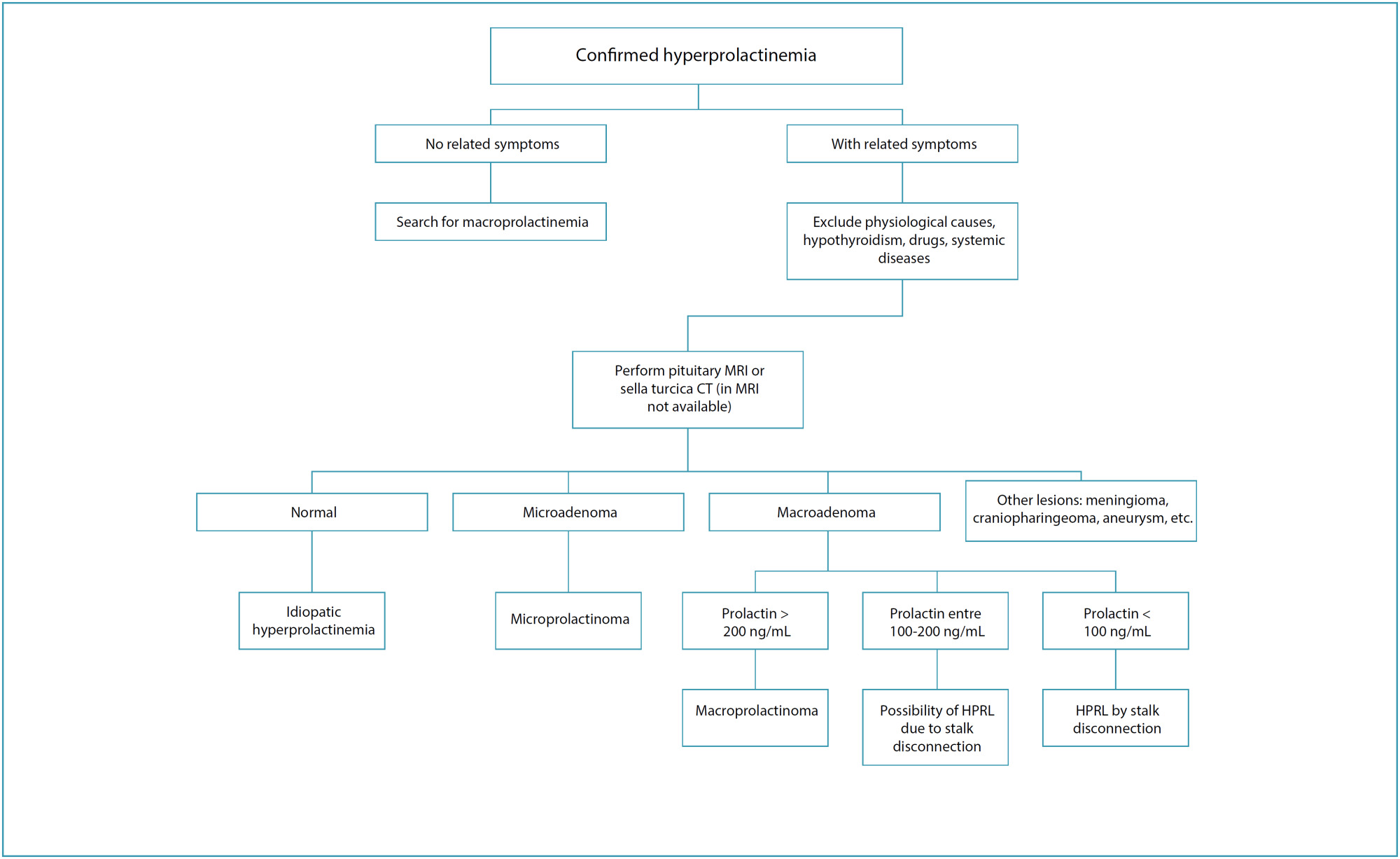
Febrasgo Position StatementHyperprolactinemia in women: diagnostic approach
Rev Bras Ginecol Obstet. 2024;46:e-FPS04
-
Febrasgo Position Statement
Hyperprolactinemia in women: treatment
Rev Bras Ginecol Obstet. 2024;46:e-FPS05
Summary
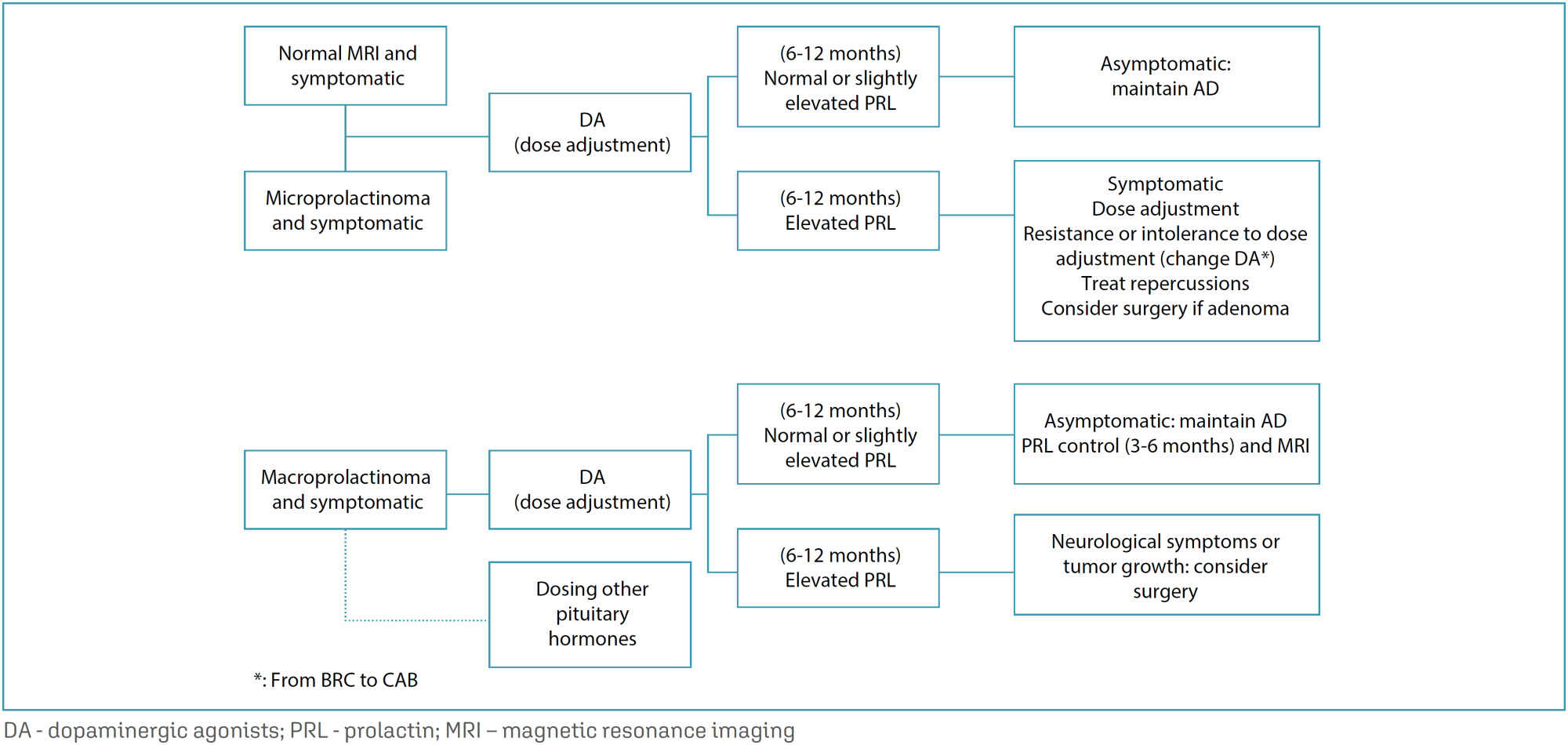
Febrasgo Position StatementHyperprolactinemia in women: treatment
Rev Bras Ginecol Obstet. 2024;46:e-FPS05
-
Febrasgo Position Statement
Use of androgens at different stages of life: climacterium – Number 1 – January 2022
Rev Bras Ginecol Obstet. 2022;44(1):83-88
Summary
Febrasgo Position StatementUse of androgens at different stages of life: climacterium – Number 1 – January 2022
Rev Bras Ginecol Obstet. 2022;44(1):83-88
-
Original Article
Use of androgens at different stages of life: reproductive period: Number 11 – December 2021
Rev Bras Ginecol Obstet. 2021;43(12):988-993
Summary
Original ArticleUse of androgens at different stages of life: reproductive period: Number 11 – December 2021
Rev Bras Ginecol Obstet. 2021;43(12):988-993
-
Review Article
Reproductive Outcomes in Cases of Subclinical Hypothyroidism and Thyroid Autoimmunity: A Narrative Review
Rev Bras Ginecol Obstet. 2020;42(12):829-833
Summary
Review ArticleReproductive Outcomes in Cases of Subclinical Hypothyroidism and Thyroid Autoimmunity: A Narrative Review
Rev Bras Ginecol Obstet. 2020;42(12):829-833
Views2Abstract
Thyroid diseases are relatively common in women in the reproductive period. It is currently understood that clinically-evident thyroid disorders may impair ovulation and, consequently, fertility. However, to date it has not been proven that high serum levels of thyroid-stimulating hormone and/or positivity for antithyroid antibodies are associated to a reduction in fertility, mainly in the absence of altered thyroxine levels. The present comprehensive review aims to present current data on the association between subclinical hypothyroidism and/or thyroid autoimmunity and reproductive outcomes.
Key-words autoimmunityfemale infertilityhypothyroidismthyroid diseasesthyroid function teststhyroid hormonesSee more -
Febrasgo Position Statement
Increasing the Chances of Natural Conception: Opinion Statement from the the Brazilian Federation of Gynecology and Obstetrics Associations – FEBRASGO Committee of Gynecological Endocrinology
Rev Bras Ginecol Obstet. 2019;41(3):183-190
Summary
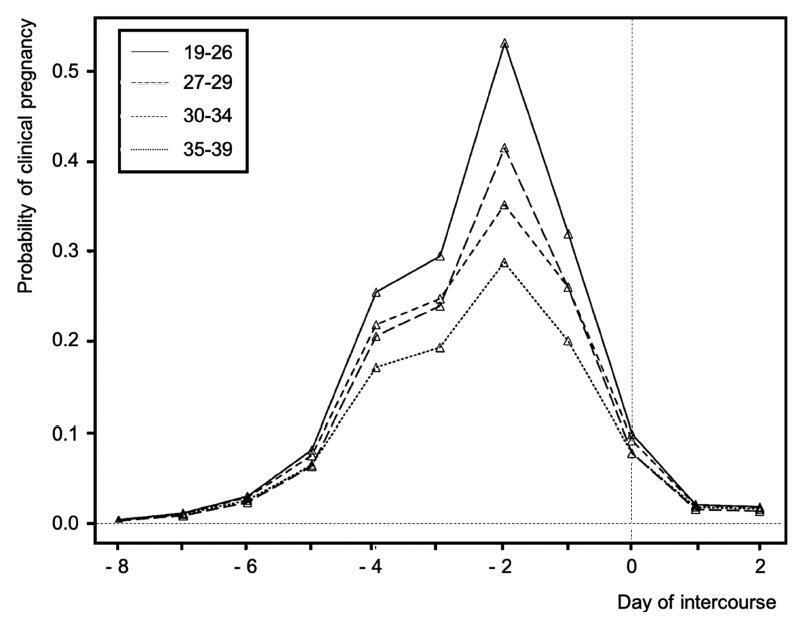
Febrasgo Position StatementIncreasing the Chances of Natural Conception: Opinion Statement from the the Brazilian Federation of Gynecology and Obstetrics Associations – FEBRASGO Committee of Gynecological Endocrinology
Rev Bras Ginecol Obstet. 2019;41(3):183-190
Views2See moreAbstract
Considering that myths and misconceptions regarding natural procreation spread rapidly in the era of easy access to information and to social networks, adequate counseling about natural fertility and spontaneous conception should be encouraged in any kind of health assistance. Despite the fact that there is no strong-powered evidence about any of the aspects related to natural fertility, literature on how to increase the chances of a spontaneous pregnancy is available. In the present article, the Brazilian Federation of Gynecology and Obstetrics Associations (FEBRASGO, in the Portuguese acronym) Committee on Endocrine Gynecology provides suggestions to optimize counseling for non-infertile people attempting spontaneous conception.
-
Editorial
About the Anti-Müllerian Hormone (AMH) Uses in the Clinical Practice
Rev Bras Ginecol Obstet. 2018;40(11):661-663
Summary
EditorialAbout the Anti-Müllerian Hormone (AMH) Uses in the Clinical Practice
Rev Bras Ginecol Obstet. 2018;40(11):661-663
Views2The anti-Müllerian hormone (AMH) is a glycoprotein that belongs to the transforming growth factor β (TGF-β) superfamily, and which has a key role in the male sexual development. It is produced by the Sertoli cells in the testis and induces the regression of Müllerian structures. In females, the roles of the AMH have been the […]See more -
Review Article
Recommendations for the Use of Testosterone in Male Transgender*
Rev Bras Ginecol Obstet. 2018;40(5):275-280
Summary
Review ArticleRecommendations for the Use of Testosterone in Male Transgender*
Rev Bras Ginecol Obstet. 2018;40(5):275-280
Views5See moreAbstract
Gender incongruence is defined as a condition in which an individual self-identifies and desires to have physical characteristics and social roles that connote the opposite biological sex. Gender dysphoria is when an individual displays the anxiety and/or depression disorders that result from the incongruity between the gender identity and the biological sex. The gender affirmation process must be performed by a multidisciplinary team. The main goal of the hormone treatment is to start the development of male physical characteristics by means of testosterone administration that may be offered to transgender men who are 18 years old or over. The use of testosterone is usually well tolerated and improves the quality of life. However, there is still lack of evidence regarding the effects and risks of the long-term use of this hormone. Many different pharmacological formulations have been used in the transsexualization process. The most commonly used formulation is the intramuscular testosterone esters in a short-term release injection, followed by testosterone cypionate or testosterone enanthate. In the majority of testosterone therapy protocols, the male physical characteristics can be seen in almost all users after 6 months of therapy, and themaximum virilization effects are usually achieved after 3 to 5 years of regular use of the hormone. To minimize risks, plasmatic testosterone levels should be kept within male physiological ranges (300 to 1,000 ng/dl) during hormonal treatment. It is recommended that transgender men under androgen therapy be monitored every 3 months during the 1st year of treatment and then, every 6 to 12 months.
Search
Search in:
Tag Cloud
breast (42) breast cancer (42) breast neoplasms (95) Cesarean section (72) endometriosis (66) infertility (56) Maternal mortality (43) menopause (82) obesity (58) postpartum period (40) pregnancy (225) Pregnancy complications (99) Prenatal care (68) prenatal diagnosis (50) Prevalence (41) Quality of life (51) risk factors (94) ultrasonography (79) urinary incontinence (40) women's health (48)