Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(3):160-164
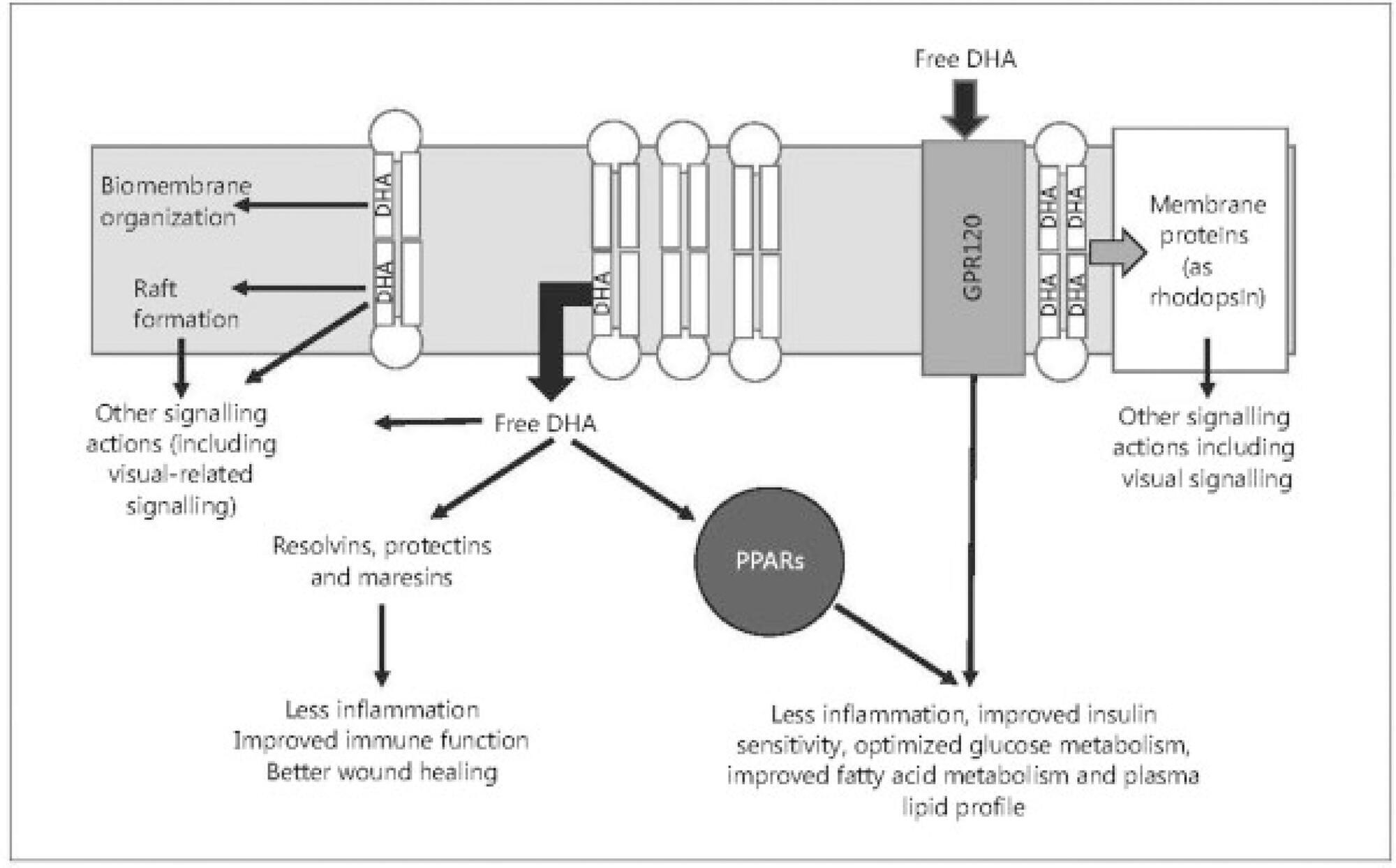
Long-chain omega-3 (n-3) polyunsaturated fatty acids (PUFAs), such as the eicosapentaenoic and docosahexaenoic acids, have been linked to human health in all stages of life, from fetal development to aging. These PUFAs act as precursors for various metabolites involved in the prevention of certain diseases. The recognizable effects of these supplements prior to pregnancy (oocyte maturation), during pregnancy (improvement in the risk of premature delivery, among others) and in the offspring (in terms of cognitive function and the approach to neurodevelopmental disorders) are described in the present narrative review. We concluded that the diffusion of these supplements may improve the prognosis of these patients in a simple, effective way, and with high safety rates.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(10):621-627
Antiphospholipid antibody syndrome (APS) is a systemic, autoimmune, prothrombotic disease characterized by persistent antiphospholipid antibodies (aPLs), thrombosis, recurrent abortion, complications during pregnancy, and occasionally thrombocytopenia. The objective of the present study was to review the pathophysiology of APS and its association with female infertility. A bibliographic review of articles of the past 20 yearswas performed at the PubMed, Scielo, and Bireme databases. Antiphospholipid antibody syndrome may be associated with primary infertility, interfering with endometrial decidualization and with decreased ovarian reserve. Antiphospholipid antibodies also have direct negative effects on placentation, when they bind to the trophoblast, reducing their capacity for invasion, and proinflammatory effects, such as complement activation and neutrophil recruitment, contributing to placental insufficiency, restricted intrauterine growth, and fetal loss. In relation to thrombosis, APS results in a diffuse thrombotic diathesis, with global and diffuse dysregulation of the homeostatic balance. Knowing the pathophysiology of APS, which is closely linked to female infertility, is essential for new therapeutic approaches, specialized in immunomodulation andinflammatory signaling pathways, to provide important advances in its treatment.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(9):564-574
To assess the efficacy of non-surgical treatment for adenomyosis.
A search was performed by two authors in the Pubmed, Scopus, and Scielo databases and in the grey literature from inception to March 2018, with no language restriction.
We have included prospective randomized studies for treating symptomaticwomen with adenomyosis (abnormal uterine bleeding and/or pelvic pain) diagnosed by ultrasound or magnetic resonance imaging.
Studies were primarily selected by title and abstract. The articles that were eligible for inclusion were evaluated in their entirety, and their data was extracted for further processing and analysis.
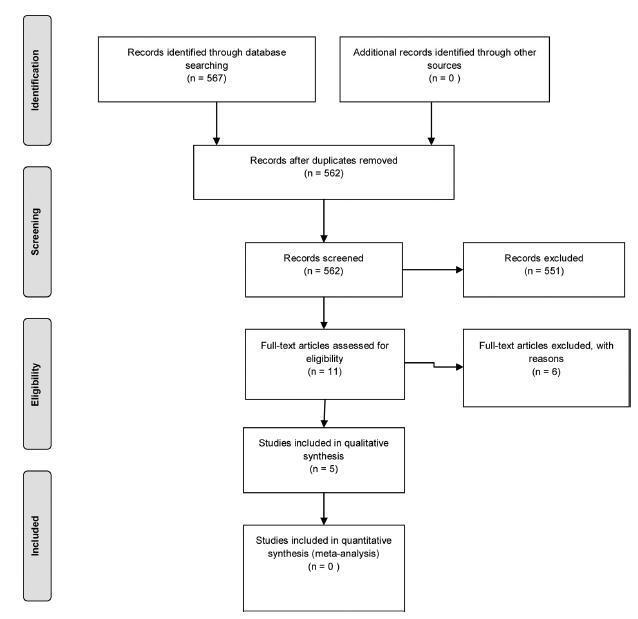
From567retrieved records only 5 remained for analysis. The intervention groups were: levonorgestrel intrauterine system (LNG-IUS)(n= 2), dienogest (n= 2), and letrozole (n= 1). Levonorgestrel intrauterine system was effective to control bleeding when compared to hysterectomy or combined oral contraceptives (COCs). One study assessed chronic pelvic pain and reported that LNG-IUS was superior to COC to reduce symptoms. Regarding dienogest, it was efficient to reduce pelvic pain when compared to placebo or goserelin, but less effective to control bleeding than gonadotropin-releasing hormone (GnRH) analog. Letrozolewas as efficient asGnRHanalog to relieve dysmenorrhea and dyspareunia, but not for chronic pelvic pain. Reduction of uterine volumewas seen with aromatase inhibitors, GnRH analog, and LGN-IUD.
Levonorgestrel intrauterine system and dienogest have significantly improved the control of bleeding and pelvic pain, respectively, in women with adenomyosis. However, there is insufficient data from the retrieved studies to endorse eachmedication for this disease. Further randomized control tests (RCTs) are needed to address pharmacological treatment of adenomyosis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(8):508-519
We sought to investigate whether women present adequate knowledge of the main pelvic floor disorders (PFDs) (urinary incontinence - UI, fecal incontinence - FI, and pelvic organ prolapse - POP).
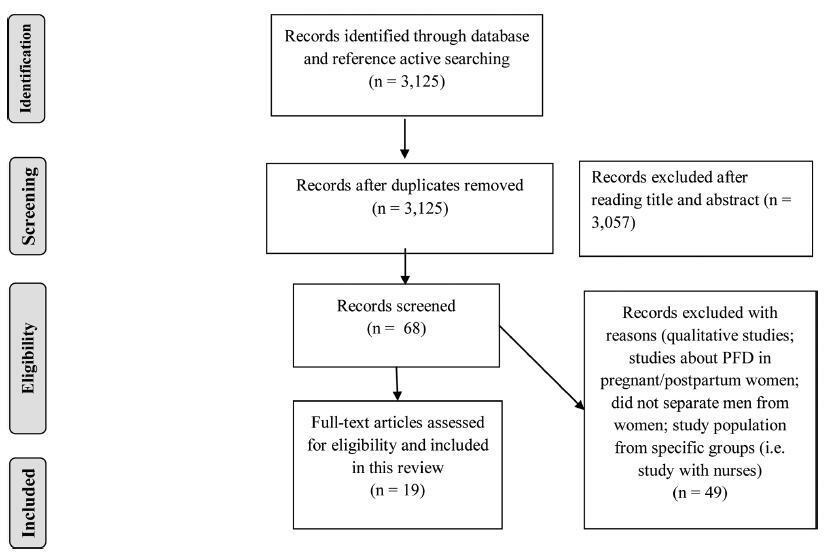
sources A systematic review was performed in the MEDLINE, PEDro, CENTRAL, and Cochrane databases for publications from inception to April 2018. Selection of studies A total of 3,125 studies were reviewed. Meta-analysis was not possible due to the heterogeneity of primary outcomes and the diversity of instruments for measuring knowledge. The quality of the articles included in the analysis was evaluated with the Newcastle-Ottawa Scale (NOS) adapted for cross-sectional studies.
Two authors performed data extraction into a standardized spreadsheet.
Nineteen studies were included, comprising 11,512 women. About the methodological quality (NOS), most of the studies (n= 11) presented a total score of 6 out of 10. Validated questionnaires and designed pilot-tested forms were the most frequently used ways of assessing knowledge. Some studies were stratified by race, age, or group minorities. The most used questionnaire was the prolapse and incontinence knowledge questionnaire (PIKQ) (n= 5). Knowledge and/or awareness regarding PFD was low to moderate among the studies. Urinary incontinence was the most prevalent PFD investigated, and the most important risk factors associated with the lack of knowledge of the pelvic floor were: African-American ethnicity (n= 3), low educational level (n= 4), low access to information (n= 5) and socioeconomic status (n= 3).
Most women have a gap in the knowledge of pelvic floor muscle dysfunctions, do not understand their treatment options, and are not able to identify risk factors for these disorders.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(4):256-263
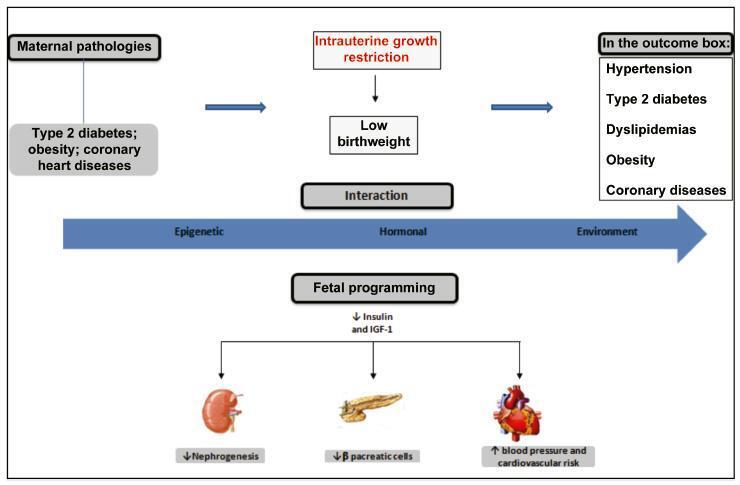
The hypothesis of fetal origins to adult diseases proposes that metabolic chronic disorders, including cardiovascular diseases, diabetes, and hypertension originate in the developmental plasticity due to intrauterine insults. These processes involve an adaptative response by the fetus to changes in the environmental signals, which can promote the reset of hormones and of the metabolism to establish a “thrifty phenotype”. Metabolic alterations during intrauterine growth restriction can modify the fetal programming. The present nonsystematic review intended to summarize historical and current references that indicated that developmental origins of health and disease (DOHaD) occur as a consequence of altered maternal and fetal metabolic pathways. The purpose is to highlight the potential implications of growth factors and adipokines in “developmental programming”, which could interfere in the development by controlling fetal growth patterns. These changes affect the structure and the functional capacity of various organs, including the brain, the kidneys, and the pancreas. These investigations may improve the approach to optimizing antenatal as well as perinatal care aimed to protect newborns against long-termchronic diseases.