-
Original Article03-01-2018
Management of Atypical Squamous Cell Cases: A Prospective Study of Women seen at a Private Health Service in Northeastern Brazil
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(3):121-126
Abstract
Original ArticleManagement of Atypical Squamous Cell Cases: A Prospective Study of Women seen at a Private Health Service in Northeastern Brazil
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(3):121-126
Views148Abstract
Objective
To assess the management chosen by gynecologists after atypical squamous cells (ASCs) cytology results, and to evaluate the outcomes of these cases in Brazilian women.
Methods
A prospective observational study evaluated the initial management offered by the gynecologist in the case of 2,458 ASCs cytology results collected between January of 2010 and July of 2016. The outcomes of the cytology, high-risk human papilloma virus (HR-HPV) test and histology were compared in two subgroups: atypical squamous cells of undetermined significance (ASC-US) and atypical squamous cells-cannot exclude high-grade squamous intraepithelial lesion (ASC-H).
Results
In many cases of ASC-US (36.97%) and ASC-H (40.50%), no clinical actions were taken. Cytology was the most frequent follow-up chosen, including for cases of ASC-H, which goes against the conduct recommended in the national guideline. In women over 30 years of age, the period of time elapsed between an ASC-US result and a new cytology was in 13.03 months, in disagreement with the national guideline recommendations (p< 0.0001). Negative for intraepithelial lesions or malignancy (NILM) cytologic (p = 0.0026) and histologic (p = 0.0017) results in the follow-up were associated with prior ASC-US, while negative results for ASC-H were cytologically (p< 0.0001) and histologically associated with high-grade squamous intraepithelial lesion (HSIL) (p< 0.0001). Two invasive cervical carcinomas (ICCs) were found in the follow-up for ASC-H, and there was a statistically significant association (p = 0.0341). A positive HR-HPV test was associated with ASC-H (p = 0.0075).
Conclusion
The data suggest that even for a population of Brazilian women assisted at private clinics, the national guidelines recommendations for ASCs results are not followed.
Key-words atypical squamous cells of the cervixdisease managementHuman papillomavirusPapanicolaou testUterine cervical neoplasmSee more -
Original Article03-01-2016
Predictive Capability of HPV and Pap Tests in Screening for Cervical Cancer over a Three-Year Follow-up
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(3):147-153
Abstract
Original ArticlePredictive Capability of HPV and Pap Tests in Screening for Cervical Cancer over a Three-Year Follow-up
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(3):147-153
Views121See morePurpose
To compare the predictive capability of HPV and Pap smear tests for screening pre-cancerous lesions of the cervix over a three-year follow-up, in a population of users of the Brazilian National Health System (SUS).
Methods
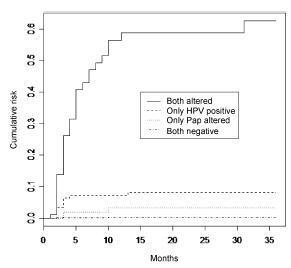
This is a retrospective cohort study of 2,032 women with satisfactory results for Pap smear and HPV tests using second-generation hybrid capture,made in a previous study. We followed them for 36 months with data obtained from medical records, the Cervix Cancer Information System (SISCOLO), and the Mortality Information System (SIM). The outcome was a histological diagnosis of cervical intraepithelial neoplasia grade 2 or more advanced lesions (CIN2ş). We constructed progression curves of the baseline test results for the period, using the Kaplan-Meier method, and estimated sensitivity, specificity, positive and negative predictive value, and positive and negative likelihood ratios for each test.
Results
A total of 1,440 women had at least one test during follow-up. Progression curves of the baseline test results indicated differences in capability to detect CIN2ş (p < 0.001) with significantly greater capability when both tests were abnormal, followed by only a positive HPV test. The HPV test was more sensitive than the Pap smear (88.7% and 73.6%, respectively; p < 0.05) and had a better negative likelihood ratio (0.13 and 0.30, respectively). Specificity and positive likelihood ratio of the tests were similar.
Conclusions
These findings corroborate the importance of HPV test as a primary cervical cancer screening.
-
Original Article06-03-2008
Immunohistochemical expression of p16 and herpes simplex virus type 2 in squamous intraepithelial lesions and cervical cancer
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(2):61-66
Abstract
Original ArticleImmunohistochemical expression of p16 and herpes simplex virus type 2 in squamous intraepithelial lesions and cervical cancer
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(2):61-66
DOI 10.1590/S0100-72032008000200003
Views88PURPOSE: to demonstrate the expression of biomarkers, detected by immunohistochemical techniques in healthy tissues, as well as in preneoplastic and neoplastic lesions of the uterine cervix. METHODS: in order to evaluate the immunohistochemical reactivity of tissues from the uterine cervix to p16 and to type 2 herpes simplex virus (HSV-2), 187 samples of low-grade intraepithelial lesions (LG-IEL) and high-grade intraepithelial lesions (HG-IEL), and of uterine cervix carcinoma were compared with a group of patients without uterine cervix lesions. Statistical analysis was done by the chi2 test for trends. The significance level was alpha=0.05. RESULTS: the reactivity to p16 was assessed showing the following distribution: group without uterine cervix lesions: 56% (24/43), LG-IEL: 92% (43/47), HG-IEL: 94% (43/46), and cancer: 98% (46/47) (p<0.001, linear trend). Concerning the HSV-2: group without uterine cervix lesions: 27% (12/45), LG-IEL: 58% (22/38), HG-IEL: 78% (35/45), and cancer: 59 % (29/49) (p<0.001, linear trend). There was an increase in the reactivity ratio for the two markers in the pathological groups (LG-IEL, HG-IEL and uterine cervix cancer, at p<0.001) compared to controls. There was no significant difference between the LG-IEL and the HG-IEL groups. CONCLUSIONS: a progressive increase of reactivity ratios of the studied immunohistochemical markers as a function of lesion severity was observed.
Key-words Cervical intraepithelial neoplasiaGenes p16Herpesvirus 2 humanImmunohistochemistryPrecancerous conditionsUterine cervical neoplasmSee more


