Summary
Rev Bras Ginecol Obstet. 2012;34(7):323-328
DOI 10.1590/S0100-72032012000700006
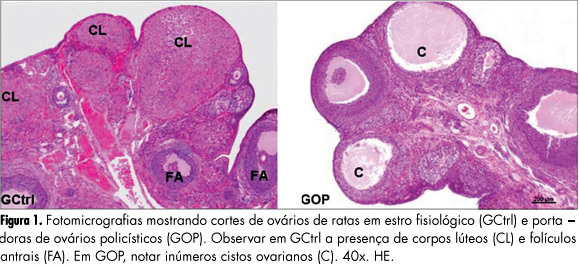
PURPOSES: To evaluate the histomorphometry of ovarian interstitial cells, as well as the blood sex steroid concentrations of female rats with polycystic ovaries induced by continuous light. METHODS: Twenty female rats were divided into two groups: Control Group - in the estrous phase (CtrlG), and a group of rats with polycystic ovaries induced by continuous illumination (POG). CtrlG animals were maintained on a light period from 07:00 a.m. to 07:00 p.m., and POG animals with continuous illumination (400 Lux) for 60 days. After this period all animals were anesthetized and blood was collected for the determination of serum estradiol (E2), progesterone (P4), and testosterone (T), followed by removal of the ovaries that were fixed in 10% formalin and processed for paraffin embedding. Five-µm histological sections were stained with hematoxylin and eosin and used for histomorphometric analysis. Morphological analyses, cyst count, determination of concentration and of the nuclear volume of interstitial cells were performed with the aid of a light microscope adapted to a high resolution camera (AxioCam), whose images were transmitted to and analyzed by the computer using AxioVision Rel 4.8 software (Carl Zeiss). Data were analyzed statistically by the Student's t-test (p<0.05). RESULTS: Morphological analysis showed the presence of ovarian cysts in POG animals and corpora lutea in CtrlG animals, as well as evidence of the origin of interstitial cells from the internal theca of these cysts. POG animals presented increased serum estradiol levels (pg/mL) compared to CtrlG animals (POG=124.9±4.2>CtrlG=73.2±6.5, p<0.05), the same occurring with testosterone levels (pg/mL) (POG=116.9±4.6>CtrlG=80.6±3.9, p<0.05). However, progesterone levels (ng/mL) were higher in CtrlG than in POG animals (CtrlG=16.3±2.0>POG=4.2±1.5, p<0.05). Morphometry showed a significant increase in nuclear volume in POG animals (POG=102.1±5.2>CtrlG=63.6±16.5, p<0.05), as well as in the area occupied (%) by interstitial cells (POG=24.4±6.9>CtrlG=6.9±3.2, p<0.05) compared to CtrlG animals. CONCLUSION: The interstitial cells of the rat polycystic ovary probably originate from ovarian cysts due to the degeneration of granulosa cells and differentiation of the internal theca cells. The elevations of serum testosterone and estradiol were probably due to the significant increase in cell activity and in the area occupied by interstitial cells.
Summary
Rev Bras Ginecol Obstet. 2012;34(7):316-322
DOI 10.1590/S0100-72032012000700005
PURPOSE: To compare the metabolic parameters, body composition and muscle strength of women with Polycystic Ovary Syndrome (PCOS) to those of women with ovulatory menstrual cycles. METHODS: A case-control study was conducted on 27 women with PCOS and 28 control women with ovulatory cycles, aged 18 to 27 years with a body mass index of 18 to 39.9 kg/m², who did not practice regular physical activity. Serum testosterone, androstenedione, prolactin, sex hormone-binding globulin (SHBG), insulin and glycemia levels were determined. Free androgen index (FAI) and resistance to insulin (by HOMA) were calculated. The volunteers were submitted to evaluation of body composition based on skin folds and DEXA and to 1-RM maximum muscle strength tests in three exercises after familiarization procedures and handgrip isometric force was determined. RESULTS: Testosterone levels were higher in the PCOS group than in the Control Group (68.07±20.18 versus 58.20±12.82 ng/dL; p=0.02), as also were the FAI (282.51±223.86 versus 127.08±77.19; p=0.01), insulin (8.41±7.06 versus 4.05±2.73 µIU/mL; p=0.01), and HOMA (2.3±2.32 versus 1.06±0.79; p=0.01), and SBHG levels were lower (52.51±43.27 versus 65.45±27.43 nmol/L; p=0.04). No significant differences in body composition were observed between groups using the proposed methods. The PCOS group showed greater muscle strength in the 1-RM test in the bench press (31.2±4.75 versus 27.79±3.63 kg; p=0.02), and leg extension exercises (27.9±6.23 versus 23.47±4.21 kg; p=0.02) as well as handgrip isometric force (5079.61±1035.77 versus 4477.38±69.66 kgf/m², p=0.04). PCOS was an independent predictor of increase muscle strength in bench press exercises (estimate (E)=2.7) (p=0.04) and leg extension (E=3.5) (p=0.04), and BMI in the exercise of isometric handgrip (E=72.2) (p<0.01), bench press (E=0.2) (p=0.02) and arm curl (E=0.3) (p<0.01). No association was found between HOMA-IR and muscle strength. CONCLUSIONS: Women with POS showed greater muscle strength, with no difference in body composition, and IR was not associated with muscle strength performance. Muscle strength may be possibly related to high levels of androgens in these women.
Summary
Rev Bras Ginecol Obstet. 2012;34(3):128-132
DOI 10.1590/S0100-72032012000300007
PURPOSE: To evaluate the importance of the oral glucose tolerance test for the diagnosis of glucose intolerance (GI) and type 2 diabetes mellitus (DM-2) in women with PCOS. METHODS: A retrospective study was conducted on 247 patients with PCOS selected at random. The diagnosis of GI was obtained from the two-hour oral glucose tolerance test with 75 g of glucose according to the criteria of the World Health Organization (WHO) (GI: 120 minutes for plasma glucose >140 mg/dL and <200 mg/dL), and the diagnosis of DM-2 was obtained by both the oral glucose tolerance test (DM: 120 minutes for plasma glucose >200 mg/dL) and fasting glucose using the criteria of the American Diabetes Association (impaired fasting glucose: fasting plasma glucose >100 and <126 mg/dL; DM: fasting glucose >126 mg/dL). A logistic regression model for repeated measures was applied to compare the oral glucose tolerance test with fasting plasma glucose. ANOVA followed by the Tukey test was used for the analysis of the clinical and biochemical characteristics of patients with and without GI and/or DM-2. A p<0.05 was considered statistically significant. RESULTS: PCOS patients had a mean age of 24.8±6.3, and body mass index (BMI) of 18.3 to 54.9 kg/m² (32.5±7.6). The percentage of obese patients was 64%, the percentage of overweight patients was 18.6% and 17.4% had healthy weight. The oral glucose tolerance test identified 14 cases of DM-2 (5.7%), while fasting glucose detected only three cases (1.2%), and the frequency of these disorders was higher with increasing age and BMI. CONCLUSIONS: The results of this study demonstrate the superiority of the oral glucose tolerance test in relation to fasting glucose in diagnosing DM-2 in young women with PCOS and should be performed in these patients.
Summary
Rev Bras Ginecol Obstet. 2012;34(2):74-79
DOI 10.1590/S0100-72032012000200006
PURPOSE: To analyze the prevalence of insulin resistance, according to different biochemical and anthropometric measurements in women with polycystic ovary syndrome. METHODS: A total of 189 patients with polycystic ovary syndrome were retrospectively analyzed. Insulin resistance diagnosis was performed using fasting insulin, HOMA-IR, QUICKI, insulin sensibility index and glucose/fasting insulin ratio. Body mass index and lipid accumulation product were used. Data were analyzed statistically by descriptive statistics, ANOVA, Tukey post-test, and Pearson's correlation. RESULTS: The polycystic ovary syndrome patients had a mean age of 24.9±5.2 and a mean body mass index of 31.8±7.6. The percentage of obese patients was 57.14%. Among the methods of insulin resistance investigation, the insulin sensibility index was the technique that most detected (56.4%) the presence of insulin resistance in women with polycystic ovary syndrome. The insulin resistance was detected in 87% of obese patients. The fasting glucose/fasting insulin ratio and insulin sensibility index were strongly correlated with lipid accumulation product. CONCLUSION: The prevalence of insulin resistance varied according to the method used, and it was greater the higher the body mass index. Lipid accumulation product was also related to insulin resistance.
Summary
Rev Bras Ginecol Obstet. 2011;33(6):310-316
DOI 10.1590/S0100-72032011000600008
PURPOSE: To compare the metabolic characteristics of obese and non-obese young women with polycystic ovary syndrome (POS) from the Brazilian Southeast. METHODS: This was a cross-sectional study conducted on 218 women of reproductive age with a diagnosis of POS - 90 non-obese women (BMI between 18.5 and 29.9 kg/m²), and 128 obese patients (BMI >30 kg/m²) selected at the time of diagnosis. The frequency of insulin resistance (IR), glucose intolerance (GI), metabolic syndrome (MetS) and type 2 diabetes mellitus (DM2) and mean values of total cholesterol (TC), triglycerides (TG), high-density (HDL) and low-density lipoproteins (LDL), were compared between obese and non-obese patients with POS. The two groups were also compared in terms of clinical and hormonal characteristics (follicle stimulating hormone, prolactin, thyroid stimulating hormone, total testosterone, dihydroepiandrostenedione sulfate, and 17-hydroxyprogesterone). Statistical analysis was performed using the SAS 9.0 software. Quantitative variables were compared by the Student´s t-test (data with normal distribution) or by the Mann-Whitney test (non-parametric distribution). Qualitative variables were compared by the Fisher test. The level of significance was set at 5% (p<0.05) in all analyses. RESULTS: The frequency of IR, GI and MetS was significantly higher in obese than non-obese patients with POS (66.7, 29.9, and 63% versus 24.7, 12.2, and 16.4%, respectively). Obese patients had higher TC and TG levels (189.8±35.8 mg/dL and 145.4±71.1 mg/dL, respectively) than non-obese patients (172.1±38.4 mg/dL and 99.3±54 mg/dL, respectively). Both groups had mean HDL levels below 50 mg/dL. CONCLUSIONS: Young obese women with POS have a higher frequency of IR, GI and MS than non-obese. However, the occurrence of metabolic disorders is elevated also in the non-obese patients, suggesting that the presence of the syndrome may favor the development of metabolic comorbidities with potential medium- and long-term repercussions.