Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(3):192-192
DOI 10.1590/S0100-72032001000300013
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(4):193-200
DOI 10.1590/S0100-72031999000400003
Purpose: to evaluate the efficacy of cytology and colposcopy-directed biopsy to distinguish preclinical invasive cervical carcinoma from intraepithelial lesions. Patients and Methods: 441 patients submitted to conization, hysterectomy and Wertheim-Meigs operation from 1978 to 1995 in the University Hospital "Clementino Fraga Filho", Federal University of Rio de Janeiro, Cervical Pathology Outpatient Clinic. We estimated sensitivity, specificity, predictive values, likelihood ratio and confidence intervals of each study, which were divided into four classes: 1) normal and inflammatory; 2) mild and moderate dysplasias; 3) severe dysplasia and carcinoma in situ; 4) microcarcinoma and invasive carcinoma. Biopsies were analyzed as a whole and separated in accordance with the type of the colposcopic result (satisfactory and unsatisfactory). Results: cytology has shown sensitivity of 50%, specificity of 89%, positive predictive value of 63% and negative predictive value of 82%. The likelihood ratios were 4.4 for stromal invasion diagnosis, 0.7 for severe dysplasia and carcinoma in situ, 0.1 for mild and moderate dysplasia, 2.2 for normal and inflammatory report and 0.6 for the negative results for invasion as a whole. Satisfactory colposcopic guided biopsy white a visible lesion showed sensitivity of 59%, specificity of 100% positive predictive value of 100% and negative predictive value of 83%. Likelyohood ratios were: tending to infinity for invasion, 0.5 for severe dysplasia and carcinoma in situ, zero for mild and moderate dysplasia, zero for negative and inflammatory and 0.4 for all negative results for invasion.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(4):193-198
DOI 10.1590/S0100-72031998000400004
The patients who do not adjust to the metabolic changes of pregnancy and those with previous alterations in carbohydrate metabolism show a significant increase in perinatal morbidity and mortality. In order to contribute to a better prenatal management of diabetic patients, the authors reviewed 60 cases of diabetes during pregnancy, assisted at the Department of Obstetrics and Gynecology, Faculty of Medicine of Ribeirão Preto, University of São Paulo. The sample was divided into two groups: one with prenatal care according to the Department protocol, and referred to this center for pregnancy resolution, and the other without appropriate prenatal care. In the group with prenatal care according to the Department protocol the complications observed were related to prematurity. The group without appropriate care showed 3 cases of congenital malformations, 3 cases of prematurity, 1 case of severe neonatal hypoglycemia, 1 case of macrossomia, 1 case of intrauterine growth retardation and 1 neonatal death. Comparing the groups, it became clear that the appropriate prenatal care is essential for the diabetic pregnant patient, but also that a reference center, such as this Obstetrical and Gynecological Department, must be fully integrated with the regional health centers, in order to offer assistance before and during gestation to the diabetic patients.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(3):193-200
DOI 10.1590/S0100-72032003000300008
PURPOSE: to evaluate the diagnostic procedures used in women with Pap smear result of atypical glandular cells. PATIENTS AND METHODS: a prospective study with 159 women with atypical glandular cells was carried out between January and December 2000. All women were submitted to a new colpocytology and to colposcopy. Directed biopsy was performed in 50 cases, endocervical curettage in 21 and conization in 75. The performance of the diagnostic procedures was described by estimating the sensitivity, specificity, predictive values and likelihood ratio, considering histological results as gold standard. RESULTS: the histological evaluation showed 51 intraepithelial squamous lesions, 29 low grade and 22 high grade. Five women presented in situ adenocarcinoma and six patients presented invasive neoplasias. Colpocytology alone showed sensitivity and specificity of 88.5 and 39%, respectively, and colposcopy alone, 74 and 42%. The association of colpocytology with colposcopy increased the sensitivity to 98.4%, with a significantly lower specificity of 10%. Endocervical curettage showed low sensitivity (25%). CONCLUSION: the presence of atypical glandular cells on colpocytology was associated with preinvasive and invasive cervical lesions in 62.2% of the cases with histological evaluation. Repeating colpocytology and performing colposcopy allowed to select the women who needed histological evaluation. Conization was an adequate procedure when examination continued to show morphologic alterations.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(4):193-193
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(3):193-200
DOI 10.1590/S0100-72032004000300004
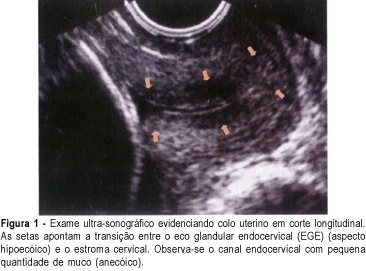
PURPOSE: to verify the prevalence of two sonographic findings, the cervical gland area (CGA) feature and the cervical length of less than 20 mm, and to compare these with the risk for premature delivery in pregnant women between 21 and 24 weeks' gestation. METHOD: this was a prospective, cross-sectional study in which 361 women were consecutively examined by transvaginal ultrasonography. Müllerian or other malformations, multiple gestations, fetal death, olygo- or polyhydramnios, marginal placenta previa, and conization, cerclage, amputation or other surgical procedures in the cervix, prior to or during pregnancy, were exclusion criteria. After the abdominal ultrasonographic morphological examination, we used transvaginal ultrasonography to measure the cervical length and to observe the presence of hyper- or hypoechoic area next to the endocervical canal, a feature characteristic of endocervical epithelium glands which is called CGA (cervical gland area). Qualitative variables are expressed as absolute and relative frequency. Quantitative variables are expressed as mean, median, standard deviation, minimum, and maximum values. Association between qualitative variables was detected by the c² test or by the Fisher exact test. For each variable, the relative risk and the 95% confidence interval (CI) were calculated. Logistic regression analysis was used to calculate the predictive values for premature delivery. Significance level was 95% (alpha = 5%), with descriptive (p) values equal or lower than 0.05 considered significant. RESULTS: spontaneous preterm delivery occurred in 5.0% of the patients. Cervical length was up to 20 mm in 3.3% of all studied patients and in 27.8% of those who delivered spontaneously before the end of the pregnancy. Absence of the CGA was detected in 2.8% of all patients and in 44.4% of the women who eventually developed spontaneous preterm labor. There was a statistically significant association of absence of CGA with short cervical length (p<0.001). Absence of CGA was strongly associated with spontaneous preterm delivery (relative risk of 28.57, 95% CI 14.40-56.68). CONCLUSION: the absent CGA feature is a new morphological ultrasonographic parameter that is useful in the prediction of spontaneous preterm delivery in single gestations. Our results show that the parameter can be used as an indicator of risk for premature delivery, to be confirmed by future research.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(2):194-200
To analyze the existing scientific literature to find out if the coronavirus disease 2019 (COVID-19) pandemic has an effect on gynecological health.
We performed an integrative review of articles published between April 2020 and April 2021 on the PubMed, SciELO, and LILACS databases, using COVID-19 and the following relevant terms: Menstrual change; Ovarian function; Violence against women; Contraception; HPV; Mental health; and Urogynecology.
Among the eligible studies found, editorials and primary research articles, which describe the dynamics between severe acute respiratory syndrome coronavirus (SARS-CoV-2) infection (the cause of the COVID-19 pandemic) and gynecological health, were included.
Through qualitative synthesis, data were extracted from the included publications and from guidelines of national and international societies of gynecology.
The 34 publications included in the present study showed that some factors of the SARS-CoV-2 infection, and, consequently, the COVID-19 pandemic, might be associated with menstrual abnormalities, effects on contraception, alterations in steroid hormones, changes in urogynecological care, effects on women’s mental health, and negative impact on violence against women.
The COVID-19 pandemic has significantly impacted the health of women. The scientific community encourages the development of recommendations for specialized care for women and strategies to prevent and respond to violence during and after the COVID-19 pandemic.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):194-199
Changes in bleeding patterns could influence the decisions of healthcare professionals to change the levonorgestrel-releasing intrauterine system (LNG-IUS) before 7 years of use, the recommended period of extended use. We evaluated changes in the bleeding patterns of users of the 52 mg LNG-IUS at the end of use of the first (IUS-1) and during the second device (IUS-2) use.
We performed an audit of the medical records of all women who used two consecutive LNG-IUSs at the Family Planning clinic. We evaluated the sociodemographic/gynecological variables, the length of use, and the bleeding patterns reported in the reference periods of 90 days before removal of the IUS-1 and at the last return in use of IUS-2. We used the McNemar test to compare bleeding patterns. Statistical significance was established at p < 0.05.
We evaluated 301 women aged (mean ± SD) 32 (±6.1) years, with lengths of use of 68.9 (±16.8) and 20.3 (±16.7) months for the IUS-1 and IUS-2, respectively. No pregnancies were reported. Bleeding patterns varied significantly among women who used the IUS-2 for ≥ 7 months to 6 years when compared the bleeding patterns reported in IUS-1 use. Eighty-nine out of 221 (40%) women maintained amenorrhea and infrequent bleeding; 66 (30%) evolved to bleeding patterns with light flow, and 66 (30%) maintained or evolved to heavy flow patterns (p = 0.012). No differences were observed among the 80 women with ≤ 6 months of use.
Changes in bleeding patterns occur during the use of LNG-IUS and should not be decisive for the early replacement of the device.