You searched for:"Rui Alberto Ferriani"
We found (48) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(8):673-673
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(12):692-696
To evaluate the effects of nutritional counseling on the dietary habits and anthropometric parameters of overweight and obese adolescentswith polycystic ovary syndrome (PCOS).
This was a prospective, longitudinal and auto-controlled study. Thirty adolescents aged 13-19 years-old, diagnosed with PCOS received nutritional counseling and were followed-up for 6 months. After the follow-up period, the results were evaluated through body weight, body mass index (BMI) and waist circumference (WC).
Sixty-percent of the adolescents adhered to the nutritional counseling and, of these, 50% lost weight. Adolescents who lost weight changed their dietary habits by adopting hypocaloric diets and eating more meals per day, as per nutritional counseling. The waist circumference (WC) decreased significantly, although the body weight decreased non-significantly after adoption of a hypocaloric diet.
Although there was no significant weight loss, there was a considerable reduction in theWCassociated with hypocaloric diets and with eating a greater number of meals per day.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(12):715-720
DOI 10.1590/S0100-72032006001200005
PURPOSE: to investigate the effects of previous bilateral tubal sterilization on the outcome of in vitro fertilization. METHODS: retrospective study of 98 consecutive in vitro fertilization cycles. Fifty-five women with previous tubal sterilization without any other infertility factor (TL group) were compared with 43 women with infertility due only to mild male factor (MI group. Age, cancellation rate per induction cycle, response to ovulation induction (number of days of ovulation induction, total amount of gonadotrophin units used, number of follicles and oocytes retrieved), fertilization and cleavage rates, number of transferred embryos and clinical pregnancy per transfer cycle were the variables considered. RESULTS: the cycle discontinuation rate due to poor response, results of ovulation induction, fertilization and cleavage rates, number of transferred embryos and the occurrence of clinical pregnancy were similar in both groups. Considering solely the variable age in TL group, we observed that patients older than 35 years required higher gonadotrophin doses during ovulation induction (2445 versus 2122 IU), presented lower response with fewer follicular growth (11.3 versus 15.8) and less oocytes retrieved (6.1 versus 8.5) compared to younger women (34 years old or less). CONCLUSIONS: tubal sterilization did not interfere with in vitro fertilization outcomes. We observed a worse response to ovulation induction in women older than 35 years, who had previous tubal sterilization.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(9):727-733
DOI 10.1590/S0100-72032004000900009
PURPOSE: to evaluate the results of ovulation hyperinduction followed by in vitro fertilization (IVF) in women with polycystic ovary syndrome (POS), as compared to normal cycle women. METHODS: a controlled retrospective study conducted on 36 women with POS (POS group) and on 44 women with infertility due to mild male factor (control group), submitted to IVF from 1997 to 2003. Subject ages ranged from 18 to 36 years. Ovulation hyperinduction was obtained with recombinant follicle-stimulating hormone and a gonadotrophin-releasing hormone agonist. The analyzed variables were the follicles with a mean diameter of 14 to 17 mm and the follicles with diameters of 18 mm or above on the day of human chorionic gonadotrophin administration, percentage of follicles >18 mm, the number of retrieved oocytes, fertilization rate, cleavage rate, incidence of ovarian hyperstimulation syndrome (OHS), clinical pregnancy rate, and abortion rate. The variables were analyzed by the unpaired t test, Fisher exact test and Mann-Whitney test, with level of significance set at p<0.05. RESULTS: the POS group presented a larger number of retrieved follicles, most of them measuring 14 to 17 mm in diameter, compared to the control group (64.8 vs 53.9%), a lower fertilization rate (59.43 vs 79.57%) and a higher incidence of OHS (38.9 vs 9.1%). The number of retrieved oocytes, cleavage rates, pregnancy rates per embryo transfer, abortion rates and live born rates did not differ between groups. CONCLUSION: the success of IVF is impaired in women with POS due to their larger number of retrieved follicles of reduced diameter, reduced fertilization rate and high OHS rates.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(2):81-89
The present study aimed to analyze cardiac autonomic modulation via spectral and symbolic analysis of heart rate variability (HRV) in women with polycystic ovary syndrome (PCOS) who were subjected to two consecutive tilt tests.
A total of 64 women were selected and divided into 2 groups: control (without PCOS), and PCOS. Concentrations of follicle-stimulating hormone, luteinizing hormone, prolactin, estradiol, homocysteine, sex hormone-binding globulin, thyroid stimulating hormone, fasting insulin, testosterone, androstenedione, and 17-hydroxyprogesterone levels, triglycerides, free androgen index (FAI), and homeostasis assessment model (HOMA-IR) were assessed. Cardiac autonomic modulation was evaluated by spectral and symbolic analyses during two consecutive tilt tests (two moments) and supine moments before, between and after (three moments) the tilt tests.
Women with PCOS had higher fasting insulin, HOMA-IR indexes, testosterone and FAI. Additionally, we observed that the PCOS group had greater sympathetic autonomic cardiac modulation in supine 2, tilt 1, and supine 3 moments compared with controls.
Women with PCOS had higher autonomic sympathetic cardiac modulation even after a second tilt test. No adaptation to this provocative test was observed. Spectral analysis was more sensitive for identifying differences between groups than the symbolic analysis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):811-819
The present study aimed to investigate the physical performance of handgrip strength (HGS) in women with polycystic ovary syndrome (PCOS).
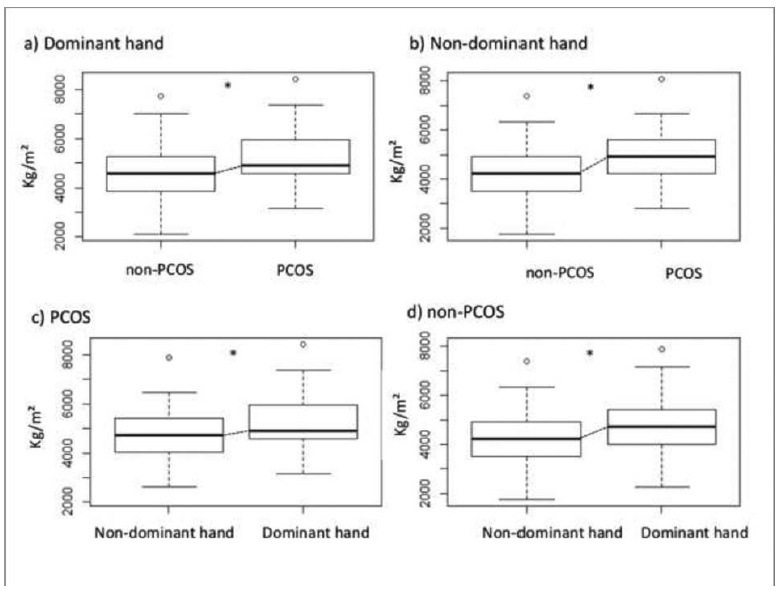
A case-control study that included 70 women with PCOS and 93 agematched healthy women aged between 18 and 47 years with body mass index (BMI) between 18 Kg/m2-39.9 Kg/m2. The serum levels of total testosterone, androstenedione, insulin, estradiol, thyroid-stimulating hormone (TSH), prolactin, sex hormonebinding globulin (SHBG), and 17-hydroxyprogesterone (17-OHP) were measured. The free androgen index (FAI) and the homeostatic model assessment of insulin resistance (HOMA-IR) were calculated. The body composition regions of interest (ROIs) were assessed by dual-energy X-ray absorptiometry (DXA), and the handgrip strength (HGS) was evaluated for both the dominant and the non-dominant hands with a manual Sammons Preston (Bolingbrook, IL, US) bulb dynamometer.
Women with PCOS had high serum levels of total testosterone (p < 0.01), androstenedione (p = 0.03), and insulin (p < 0.01), as well as high FAI (p < 0.01) and HOMA-IR (p = 0.01) scores. Compared with the non-PCOS group, the PCOS group had greater total lean mass in the dominant hand (p < 0.03) and greater HGS in both the dominant and the non-dominant hands (p < 0.01). The HGS was correlated with lean mass (p < 0.01).
Women with PCOS have greater HGS. This may be associated with age and BMI, and it may be related to lean mass. In addition, the dominance effect on muscle mass may influence the physical performance regarding HGS in women with PCOS.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(2):85-90
DOI 10.1590/S0100-72031999000200005
Purpose: to present a profile of endometriosis, stages and results of treatment among the patients seen in our Service. Methods: the medical records of 155 patients with endometriosis treated during the period from 1991 to 1996 according to a preestablished protocol were examined. Results: mean patient age was 31 years, most patients were white, with regular menstrual cycles. The most frequently observed symptoms were dysmenorrhea, pelvic pain and infertility and were mild in most of the cases. The diagnostic methods utilized were laparoscopy or echography. There was agreement between echography and laparoscopy in 96% of cases. Laparotomy was required in 28% of cases for diagnostic elucidation and/or treatment. Endometrioma was detected in 37% of the cases and endometriosis was confirmed in only 74% of the biopsies from the lesion by anatomopathological examination. There was a significant improvement with clinical treatment regardless of the drug used, with improved symptoms in approximately 50% of the patients. Assisted fertilization was performed in 34 patients, consisting of in vitro fertilization (IVF) for 80% of them, with a 27% pregnancy/transfer rate. Conclusions: the diagnostic method of choice should be laparoscopy, although echography presented a high rate of agreement. Anatomopathological examination of the lesions should be used as an adjuvant method in the diagnosis since it is not confirmatory in all of the cases. Clinical treatment with assisted reproductive technologies is a good therapeutic option, especially with the use of IVF.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):89-94
DOI 10.1590/S0100-72032000000200005
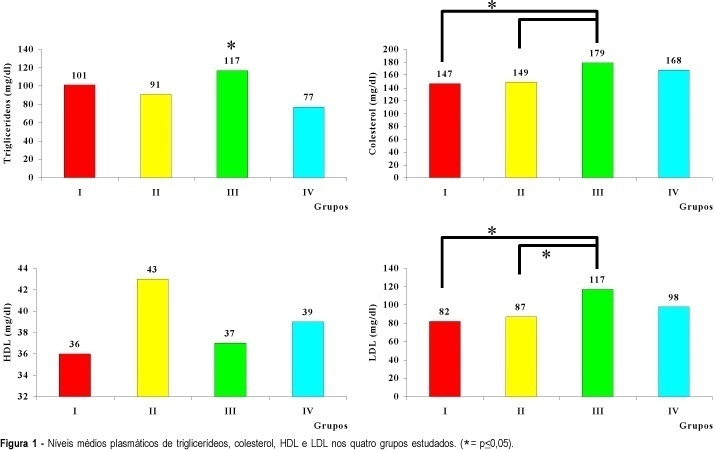
Purpose: to evaluate the lipid profile (cholesterol, triglycerides, HDL and LDL) of women with polycystic ovary syndrome (PCO) and compare it to that of women with ovulatory menstrual cycles. Methods: the patients were divided into two groups, obese and nonobese, based on body mass index, so that it would be possible to determine the joint effect of PCO and obesity on the lipid metabolism of the studied women. We studied 117 women divided into 4 groups: group I (PCO--obese), n = 33; group II (PCO--nonobese), n = 27; group III (control--obese), n = 28; group IV (control--nonobese), n = 29. Results: cholesterol levels were elevated (179 mg/dl) in obese patients with ovulatory cycles (group III) compared to group I (147 mg/dl) and group II (149 mg/dl), as also were triglyceride levels (117 mg/dl) compared to group IV (77 mg/dl) and LDL levels (117 mg/dl) compared to group I (82 mg/dl). Conclusion: these data suggest that alterations in lipid profile are related to obesity only.