You searched for:"Edward Araujo Júnior"
We found (58) results for your search.Summary
Rev Bras Ginecol Obstet. 2021;43(4):317-322
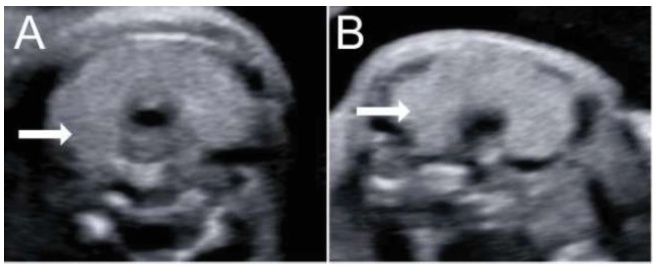
Fetal thyroid complications in pregnancy are uncommon, and are commonly related to the passage of substances through the placenta. The excessive iodine intake during the pregnancy is a well-known mechanism of fetal thyroid enlargement or goiter, and invasive procedures have been proposed for the treatment of fetal thyroid pathologies. In the present report, we demonstrate two cases from different centers of prenatal diagnosis of fetal thyroid enlargement and/or goiter in three fetuses (one pair of twins, wherein both fetuses were affected, and one singleton pregnancy). The anamnesis revealed the ingestion of iodine by the patients, prescribed from inadequate vitamin supplementation. In both cases, the cessation of iodine supplement intake resulted in a marked reduction of the volume of the fetal thyroid glands, demonstrating that conservative treatmentmay be an option in those cases. Also, clinicians must be aware that patients may be exposed to harmful dosages or substances during pregnancy.
Summary
Rev Bras Ginecol Obstet. 2006;28(5):317-317
Summary
Rev Bras Ginecol Obstet. 2016;38(7):348-355
To identify the epidemiological risk factors for congenital anomalies (CAs) and the impact of these fetal malformations on the perinatal outcomes.
This prospective cohort study comprised 275 women whose fetuses had CAs. Maternal variables to establish potential risk factors for each group of CA and perinatal outcomes were evaluated. The primary outcome was CA. Secondary outcomes included: fetal growth restriction (FGR); fetal distress (FD); premature rupture of membranes (PROM); oligohydramnios or polyhydramnios; preterm delivery (PTD); stillbirth; cesarean section; low birth weight; Apgar score < 7 at the 1st and 5th minutes; need for assisted ventilation at birth; neonatal infection; need for surgical treatment; early neonatal death; and hospitalization time. Chi-square (x2) test and multilevel regression analysis were applied to compare the groups and determine the effects of maternal characteristics on the incidence of CAs.
The general prevalence of CAs was of 2.4%. Several maternal characteristics were associated to CAs, such as: age; skin color; level of education; parity; folic acid supplementation; tobacco use; and history of previous miscarriage. There were no significant differences among the CA groups in relation to FGR, FD, PROM, 1-minute Apgar score > 7, and need for assisted ventilation at birth. On the other hand, the prevalence of the other considered outcomes varied significantly among groups. Preterm delivery was significantly more frequent in gastrointestinal tract/abdominal wall defects. The stillbirth rate was increased in all CAs, mainly in isolated fetal hydrops (odds ratio [OR]: 27.13; 95% confidence interval [95%CI]: 2.90-253.47). Hospitalization time was higher for the urinary tract and congenital heart disease groups (p < 0.01). Neonatal death was significantly less frequent in the central nervous system anomalies group.
It was possible to identify several risk factors for CAs. Adverse perinatal outcomes were presented in all CA groups, and may differ according to the type of CA considered.
Summary
Rev Bras Ginecol Obstet. 2020;42(6):369-370
Summary
Rev Bras Ginecol Obstet. 2001;23(6):377-382
DOI 10.1590/S0100-72032001000600006
Purpose: to evaluate a group of pregnant women with human papillomavirus (HPV) infection, analyzing age, gestational age, number of gestations and cytological findings. Methods: in the period from July 1993 to December 1998, 245 pregnant patients seen in our service presented cytological alterations compatible with HPV infection, associated or not with cervical intraepithelial neoplasia (CIN) grade 1. Clinical data were related to age, gestational period (first or second half), number of gestations and cytological finding of Trichomonas vaginalis, Candida sp and clue cells. The control group consisted of 386 pregnant patients seen during the same period and without cytological signs of HPV infection. In the statistical analysis, chi² (chi-square) test was used with Yates correction and a significance level lower than 0.05. Results: HPV infection was more frequent among pregnant women younger than 20 years old (45.3% versus 28.2%, p<0.001). The most frequent cytological finding, among the pregnant women with HPV infection, was the presence of clue cells, compared to the controls (21.6% versus 12.4%, p<0.02). Clue cells were more frequent in pregnant women with HPV infection in the second half of gestation and older than 20 years (27% versus 12.2%, p<0,01). The difference regarding number of gestations was not significant. Conclusion: HPV infection was more frequent among pregnant women younger than 20 years old. Clue cells and HPV were the most frequent cytological findings in pregnant women older than 20 years and in the second half of gestation.
Summary
Rev Bras Ginecol Obstet. 2020;42(7):420-426
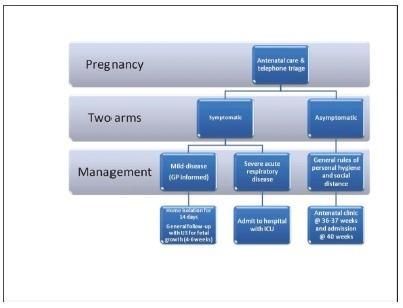
Since the World Health Organization (WHO) declared coronavirus infection (COVID-19) a Public Health Emergency of International Concern in January 2020, there have been many concerns about pregnant women and the possible effects of this emergency with catastrophic outcomes inmany countries. Information on COVID-19 and pregnancy are scarce and spread throughout a fewcase series, with no more than 50 cases in total. The present review provides a brief analysis of COVID-19, pregnancy in the COVID-19 era, and the effects of COVID-19 on pregnancy.
Summary
Rev Bras Ginecol Obstet. 2019;41(7):425-431
To evaluate the relationship between vitamin D receptor (VDR) gene polymorphism (FokI [rs10735810]) and serum vitamin D concentration in gestational diabetes mellitus (GDM).
A prospective case-control study that recruited healthy pregnant women (control group) (n = 78) and women with GDM (GDM group) (n = 79), with no other comorbidities. Peripheral blood samples were collected in the 3rd trimester of gestation, and all of the pregnant women were followed-up until the end of the pregnancy and the postpartum period. Serum vitamin D concentrations were measured by high-performance liquid chromatography (HPLC). For genomic polymorphism analysis, the genomic DNA was extracted by the dodecyltrimethylammonium bromide/ cetyltrimethylammonium bromide (DTAB/CTAB) method, and genotyping was performed by the polymerase chain reaction - restriction fragment length polymorphism (PCR-RFLP) technique, using the restriction enzyme FokI. The Student-t, Mann- Whitney, chi-squared, and Fischer exact tests were used for the analysis of the results.
There was no significant difference between the pregnant women in the control and GDM groups regarding serumvitamin D levels (17.60 ± 8.89 ng/mL versus 23.60 ± 10.68 ng/mL; p = 0.1). Also, no significant difference was detected between the FokI genotypic frequency when the 2 groups were compared with each other (p = 0.41).
There was no association between the FokI polymorphism and the development of GDM, nor was there any change in serum vitamin D levels in patients with GDM.