Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(2):93-97
DOI 10.1590/S0100-72032001000200006
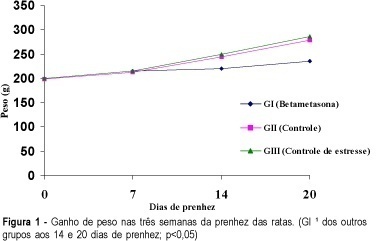
Purpose: to analyze the effect of betamethasone on the pregnancy of rats. Methods: thirty pregnant rats were divided into three groups of ten animals each. Group I -- the animals received betamethasone IM (1 mg/kg body weight, in 0.5 ml distilled water) on the 11th, 12th, 18th and 19th day of pregnancy. Group II -- the rats received distilled water (0.5 ml) IM on the 11th, 12th, 18th and 19th day of pregnancy. Group III - the rats did not receive any drug or vehicle. The animals were weighed on days 0, 7, 14 and on the 20th of pregnancy, and on the last day of weighing, the animals were sacrificed. The number of implantations, resorptions, fetuses, placentas, malformations, maternal and fetal mortality as well as the weight of the fetuses and placentas were obtained and analyzed. Results: our results show that the rats treated with betamethasone gained significantly less weight. Their fetuses had an average weight of 3.2 g compared with 3.75 g in the control group. The results regarding placental weight were 0.36 g vs 0.48 g, respectively. All these differences were statistically significant. Conclusions: betamethasone had a negative effect on the gain of weight of matrices, fetuses and placentas when administered repeatedly and continuousy after the second half of pregnancy.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(2):93-100
DOI 10.1590/S0100-72032008000200008
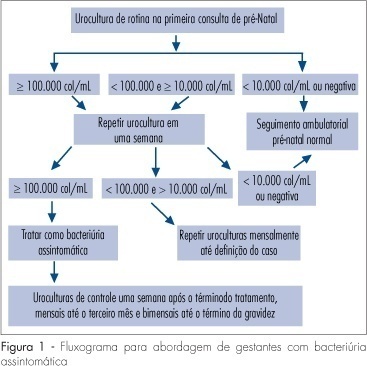
Several factors cause urinary tract infection (UTI) to be a relevant complication of the gestational period, aggravating both the maternal and perinatal prognosis. For many years, pregnancy has been considered to be a factor predisposing to all forms of UTI. Today, it is known that pregnancy, as an isolated event, is not responsible for a higher incidence of UTI, but that the anatomical and physiological changes imposed on the urinary tract by pregnancy predispose women with asymptomatic bacteriuria (AB) to become pregnant women with symptomatic UTI. AB affects 2 to 10% of all pregnant women and approximately 30% of these will develop pyelonephritis if not properly treated. However, a difficult to understand resistance against the identification of AB during this period is observed among prenatalists. The diagnosis of UTI is microbiological and it is based on two urine cultures presenting more than 10(5) colonies/mL urine of the same germ. Treatment is facilitated by the fact that it is based on an antibiogram, with no scientific foundation for the notion that a pre-established therapeutic scheme is an adequate measure. For the treatment of pyelonephritis, it is not possible to wait for the result of culture and previous knowledge of the resistance profile of the antibacterial agents available for the treatment of pregnant women would be the best measure. Another important variable is the use of an intravenous bactericidal antibiotic during the acute phase, with the possibility of oral administration at home after clinical improvement of the patient. At our hospital, the drug that best satisfies all of these requirements is cefuroxime, administered for 10-14 days. Third-generation cephalosporins do not exist in the oral form, all of them involving the inconvenience of parenteral administration. In view of their side effects, aminoglycosides are considered to be inadequate for administration to pregnant women. The inconsistent insinuation of contraindication of monofluorinated quinolones, if there is an indication, norfloxacin is believed to be a good alternative to cefuroxime. In cases in which UTI prophylaxis is indicated, chemotherapeutic agents are preferred, among them nitrofurantoin, with care taken to avoid its use at the end of pregnancy due to the risk of kernicterus for the neonate.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2011;33(2):93-98
DOI 10.1590/S0100-72032011000200007
PURPOSE: to estimate the prevalence and risk factors associated with seropositivity for Toxoplasma gondii in pregnant women. METHODS: a cross-sectional retrospective study based on the records of women screened for toxoplasmosis by the Pregnancy Protection Program in 2008, living in Goiânia (GO). These records were connected to records from the database of the National Information System on Live Births from the State of Goiás. The process occurred in three phases, with 10,316 records being paired for analysis, among the 12,846 initial records. The following variables were evaluated in this process: woman's name, age, date of birth, estimated date of delivery, date of infant birth and household information. Anti-Toxoplasma gondii antibodies were detected with the Q-Preven Toxo IgG and IgMin tests in dried blood samples collected on filter paper. The χ2 test and χ2 test for trend were used for data analysis, and the odds ratio (OR) was used to estimate the chance of association between exposure and outcome. RESULTS: the prevalence of infection was 67.7%, with 0.7% of the samples presenting anti-Toxoplasma gondii IgM and IgG reagents. Out of these, only three did not undergo confirmatory testing in venous blood. The median interval between the screening and the new collection of venous blood was of 12.5 days, and from screening to confirmatory test and avidity it was of 20 days. The variables associated with exposure were: age 20-30 years, OR=1.6 and >31 years, OR=1.8; brown skin color, OR=1.4, and black skin color, OR=1.6; and education of 8-11 years, OR=0.7, and >12 years of education, OR=0.6. CONCLUSION: a high prevalence of infection was estimated among the studied pregnant women. The associated factors that were found found should be considered during prenatal care, along with educational activities for the prevention of infection and assessment of serological status of seronegative pregnant women.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(10):930-937
To determine whether a rescue strategy using dydrogesterone (DYD) could improve the outcomes of frozen embryo transfer cycles (FET) with low progesterone (P4) levels on the day of a blastocyst transfer.
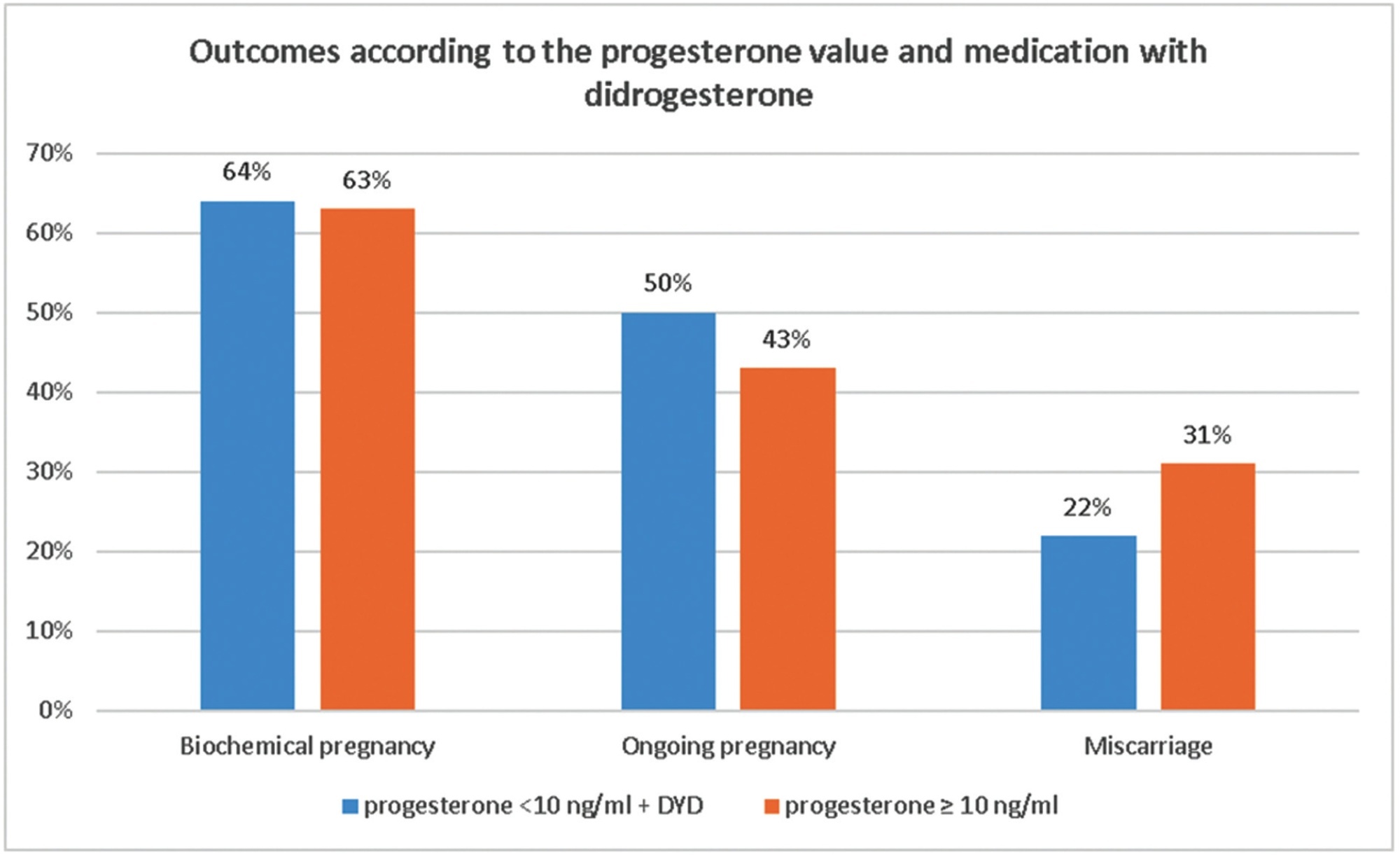
Retrospective cohort study including FET cycles performed between July 2019 and October 2020 following an artificial endometrial preparation cycle using estradiol valerate and micronized vaginal P4 (400 mg twice daily). Whenever the serum P4 value was below 10 ng/mL on the morning of the planned transfer, DYD 10 mg three times a day was added as supplementation. The primary endpoint was ongoing pregnancy beyond 10 weeks. The sample was subdivided into two groups according to serum P4 on the day of FET: low (< 10 ng/mL, with DYD supplementation) or normal (above 10 ng/mL). We performed linear or logistic generalized estimating equations (GEE), as appropriate.
We analyzed 304 FET cycles from 241 couples, 11.8% (n = 36) of which had serum P4 below 10 ng/mL on the FET day. Baseline clinical data of patients was comparable between the study groups.
Our results indicate that DYD 10 mg three times a day administered in women who perform FET with P4 serum levels < 10 ng/mL, allows this group to have pregnancy rates beyond 12 weeks at least as good as those with serum levels above 10 ng/mL.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(12):932-939
To study maternal anxiety in pregnant women without comorbidities in the context of the COVID-19 outbreak in Brazil and to study maternal knowledge and concerns about the pandemic.
This is a secondary analysis from a national multicenter cross-sectional study performed in 10 cities, from June to August, 2020, in Brazil. Interviewed postpartum women, without medical or obstetrical comorbidities, were included in the present subanalysis. A structured questionnaire and the Beck Anxiety Inventory (BAI) were applied.
Out of the 1,662 women, 763 (45.9%) met the criteria for the current analysis and 16.1% presented with moderate and 11.5% with severe maternal anxiety. Moderate or severe maternal anxiety was associated with high school education (odds ratio [OR]:1.58; 95% confidence interval [CI]:1.04–2.40). The protective factor was cohabiting with a partner (OR: 0.46; 95%CI: 0.29–0.73). There was a positive correlation between the total BAI score and receiving information about care in the pandemic (rpartial 0.15; p < 0.001); concern about vertical transmission of COVID-19 (rpartial 0.10; p = 0.01); receiving information about breastfeeding (rpartial 0.08; p = 0.03); concerns about prenatal care (rpartial 0.10; p = 0.01), and concerns about the baby contracting COVID-19 (rpartial 0.11; p = 0.004). The correlation was negative in the following aspects: self-confidence in protecting from COVID-19 (rpartial 0.08; p = 0.04), having learned (rpartial 0.09; p = 0.01) and self-confidence in breastfeeding (rpartial 0.22; p < 0.001) in the context of the pandemic.
The anxiety of pregnant women without medical or obstetrical comorbidities was associated to high school educational level and not living with a partner during the COVID-19 pandemic. Self-confidence in protecting against COVID-19 and knowledge about breastfeeding care during the pandemic reduced maternal anxiety.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(10):938-944
To assess the association between two colposcopic indices, the Swede score and the 2011 International Federation of Cervical Pathology and Colposcopy (IFCPC) Nomenclature as well as to determine the efficacy of the Swede score with cutoffs of 7 and 8.
In the present cross-sectional pilot study, 34 women who had at least 1 colposcopy-directed biopsy due to abnormal cytology were enrolled. The colposcopic findings were scored by both the Swede score and the 2011 IFCPC Nomenclature and were compared with each other. The Kappa coefficient and the McNemar test were used. Accuracy, sensitivity, specificity, and positive and negative predictive values (NPV and PPV, respectively) were calculated, as well as the effectiveness with cutoffs of 7 and 8 in identifying cervical intraepithelial neoplasm (CIN) 2+ when using the Swede score.
The correlation between the 2 colposcopic indices was 79.41%. The Kappa coefficient and the McNemar p-value were 0.55 and 0.37, respectively. The IFCPC Nomenclature had sensitivity, specificity, accuracy, PPV, and NPV of 85.71, 55.00, 67.64, 57.14, and 84.61%, respectively. The Swede score had sensitivity, specificity, accuracy, PPV, and NPV of 100, 63.15, 79.41, 68.18, and 100%, respectively. A Swede score cutoff of 7 for CIN 2+ detection had a specificity of 94.73%, while with a cutoff of 8 it increased to 100%. The sensitivity for both values was 60%. The PPV and NPV for cutoffs of 7 and 8 were 90 and 75 and 100 and 76%, respectively.
Although both colposcopic indices have good reproducibility, the Swede score showed greater accuracy, sensitivity, and specificity in identifying CIN 2 + , especially when using a cutoff of 8.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(2):94-98
DOI 10.1590/S0100-72032010000200008
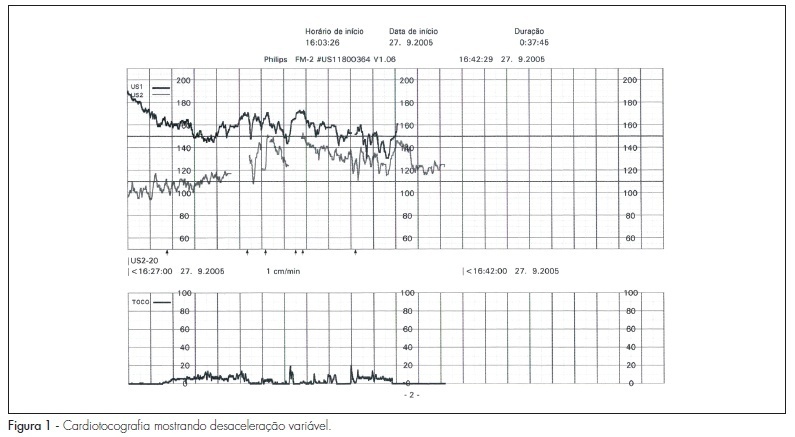
Monoamniotic twin pregnancies are very rare, but they are associated with high fetal morbidity and mortality. There is much controversy regarding the follow-up and obstetric procedures towards prenatal diagnosis of intertwined umbilical cords. In this article, we describe a case of monoamniotic pregnancy with diagnosis of intertwined umbilical cords, and we discuss aspects related to the follow-up and obstetric procedures through a brief literature review.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(2):94-99
DOI 10.1590/SO100-720320150005206
The aim of this study was to compare the performance of two human papillomavirus (HPV) genotyping techniques, Linear Array and PapilloCheck, in women with high-grade squamous intraepithelial lesion (HSIL).
A total of 88 women with cytological diagnosis of HSIL were recruited at 2 reference centers in cervical pathology in Salvador, Bahia, Brazil, from July 2006 to January 2009. After the cytological diagnosis of HSIL, cervix cells were collected to determine the HPV genotype and a biopsy was obtained under colposcopic vision for histopathological analysis. After the confirmation of CIN2+ by histopathology, HPV genotyping was performed on 41 women by the Linear Array and PapilloCheck methods.
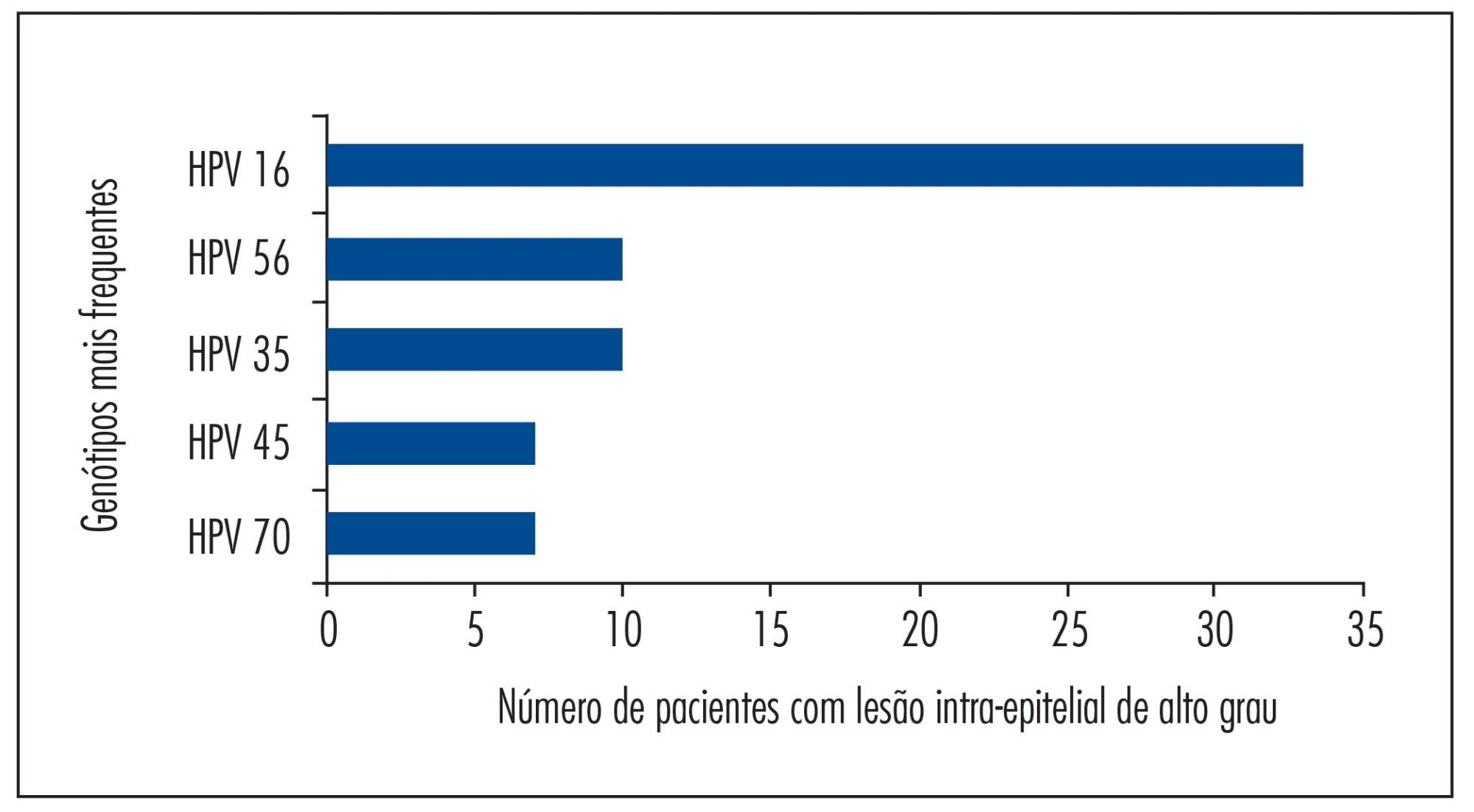
Both tests showed an overall concordance rate for HPV detection of 97.2% (35/36). Of the 36 valid samples, 35 (97.2%) were positive in both tests and 1 (2.8%) was discordant, with the Linear Array indicating the presence of multiple types. The most prevalent HPV genotypes detected by the Linear Array technique were HPV 16, HPV 56, HPV 35, HPV 45, and HPV 70; and those detected by the PapilloCheck technique were HPV 16, HPV 56, HPV 11, HPV 35, and HPV 42. A similar rate of infection with multiple HPV types was observed with the two tests (72.5% with the Linear Array and 75.0% with the PapilloCheck).
Linear Array genotyping assay and PapilloCheck showed equivalent performance for the detection of oncogenic HPV types in women with HSIL, with PapilloCheck having the advantage of being a method that avoids subjectivity when reading the HPV genotypes.