You searched for:"Rui Alberto Ferriani"
We found (49) results for your search.Summary
Rev Bras Ginecol Obstet. 2008;30(8):413-419
DOI 10.1590/S0100-72032008000800007
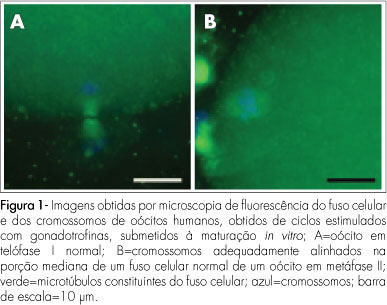
PURPOSE: to evaluate the meiotic spindle and the chromosome distribution of in vitro mature oocytes from stimulated cycles of infertile women with endometriosis, and with male and/or tubal infertility factors (Control Group), comparing the rates of in vitro maturation (IVM) between the two groups evaluated. METHODS: fourteen patients with endometriosis and eight with male and/or tubal infertility factors, submitted to ovarian stimulation for intracytoplasmatic sperm injection have been prospectively and consecutively selected, and formed a Study and Control Group, respectively. Immature oocytes (46 and 22, respectively, from the Endometriosis and Control Groups) were submitted to IVM. Oocytes presenting extrusion of the first polar corpuscle were fixed and stained for microtubules and chromatin evaluation through immunofluorescence technique. Statistical analysis has been done by the Fisher's exact test, with statistical significance at p<0.05. RESULTS: there was no significant difference in the IVM rates between the two groups evaluated (45.6 and 54.5% for the Endometriosis and Control Groups, respectively). The chromosome and meiotic spindle organization was observed in 18 and 11 oocytes from the Endometriosis and Control Groups, respectively. In the Endometriosis Group, eight oocytes (44.4%) presented themselves as normal metaphase II (MII), three (16.7%) as abnormal MII, five (27.8%) were in telophase stage I and two (11.1%) underwent parthenogenetic activation. In the Control Group, five oocytes (45.4%) presented themselves as normal MII, three (27.3%) as abnormal MII, one (9.1%) was in telophase stage I and two (18.2%) underwent parthenogenetic activation. There was no significant difference in meiotic anomaly rate between the oocytes in MII from both groups. CONCLUSIONS: the present study data did not show significant differences in the IVM or in the meiotic anomalies rate between the IVM oocytes from stimulated cycles of patients with endometriosis, as compared with controls. Nevertheless, they have suggested a delay in the outcome of oocyte meiosis I from patients with endometriosis, shown by the higher proportion of oocytes in telophase I observed in this group.
Summary
Rev Bras Ginecol Obstet. 2004;26(6):429-433
DOI 10.1590/S0100-72032004000600002
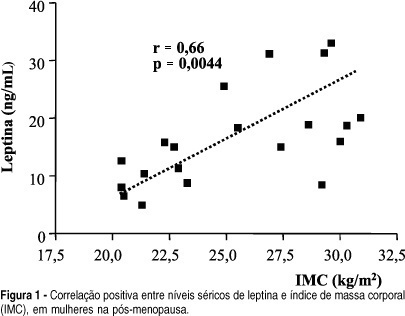
OBJECTIVE: to correlate serum leptin concentration with bone mineral density (BMD) in postmenopausal women. METHODS: twenty-two healthy postmenopausal women were included in the present study. BMD was measured by dual energy X-ray absorptiometry at the lumbar spine and femoral neck. Serum leptin concentrations were determined using an immunoradiometric assay. Statistical analysis was performed by ANOVA and Dunn and Pearson's correlation tests. RESULTS: mean BMD values were 0.898 ± 0.140 g/cm² at the lumbar spine and 0.760 ± 0.152 g/cm² at the femoral neck. Mean serum leptin concentration was 17.2 ± 9.4 ng/ml and no significant differences were observed among women with normal BMD, osteopenia and osteoporosis (18.6 ± 7.8, 18.9 ± 9.9 and 15.6 ± 10.6, respectively; p > 0.05). No significant correlations were observed between serum leptin levels and BMD measurements at the lumbar spine and femoral neck, when the whole sample was considered and when patients were divided into groups with osteoporosis and/or osteopenia and a control group. We observed a positive significant correlation between serum leptin levels and body mass index (BMI) (r = 0.66; p = 0.0044). CONCLUSIONS: there was no direct correlation between leptin and BMD in postmenopausal women, although we observed positive significant correlation between leptin and BMI. This fact indicates a possible indirect effect of leptin on bone metabolism.
Summary
Rev Bras Ginecol Obstet. 2010;32(9):447-453
DOI 10.1590/S0100-72032010000900006
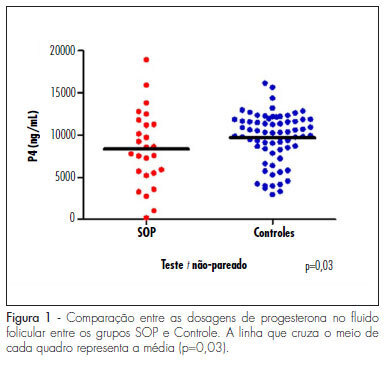
PURPOSE: to evaluate the concentration of steroid hormones in follicular fluid (FF) of small (10-14 mm) and large (> 18 mm) follicles of women with polycystic ovary syndrome (PCOS) submitted to controlled ovarian hyperstimulation (COH) and in vitro fertilization (IVF) cycles. METHODS: a case-control study was conducted on 13 infertile women with PCOS (17 cycles) and 31 infertile women due to male factor - Control Group (31 cycles). FF was aspirated individually and divided into four groups: G1 (FF of small follicles of the Control Group), G2 (FF of small follicles of the PCOS group), G3 (FF of large follicles of the Control Group) and G4 (FF of large follicles of the PCOS group). Estrogen, progesterone and β-hCG were determined by chemiluminescence, and testosterone and androstenedione by radioimmunoassay. The unpaired t-test was used to compare the hormone determinations in the FF of the PCOS and Control Groups, and the four groups were compared by ANOVA. Fisher's exact test was used to compare the pregnancy rates. RESULTS: the small follicles of the two groups had lower progesterone levels (8,435±3,305 ng/mL) than large follicles (10,280±3,475 ng/mL), p-value <0.01. The progesterone levels of all follicles of group PCOS (8,095±4,151 ng/mL) were lower than Control (9,824±3,128 ng/mL), p-value =0.03. Testosterone differed between G1 (326.6±124.4 ng/dL) and G3 (205.8±98.91 ng/dL), p-value <0.001, and between G3 (205.8±98.91 ng/dL) and G4 (351.10±122.1ng/dL), p-value <0.001. Small follicles had higher testosterone levels (508.9±266 ng/dL) than large follicles (245.10±123 ng/dL), p-value <0.0001. The pregnancy rates did not differ between the PCOS (5/13, 38.5%) and the Control groups (9/31, 40.9%), p-value =072. CONCLUSIONS: women with PCOS had high testosterone concentrations in the FF, regardless of the stage of follicle development, and reduced progesterone levels, suggesting that paracrine factors may inhibit the secretion of the latter by follicular cells. The pregnancy rates showed that treatment with COH and IVF is a good option for women with infertility secondary to PCOS.
Summary
Rev Bras Ginecol Obstet. 2021;43(6):457-466
Abnormalities in the eutopic endometrium of women with endometriosis may be related to disease-associated infertility. Although previous RNA-sequencing analysis did not show differential expression in endometrial transcripts of endometriosis patients, other molecular alterations could impact protein synthesis and endometrial receptivity. Our aim was to screen for functional mutations in the transcripts of eutopic endometria of infertile women with endometriosis and controls during the implantation window.
Data from RNA-Sequencing of endometrial biopsies collected during the implantation window from 17 patients (6 infertile women with endometriosis, 6 infertile controls, 5 fertile controls) were analyzed for variant discovery and identification of functional mutations. A targeted study of the alterations found was performed to understand the data into disease’s context.
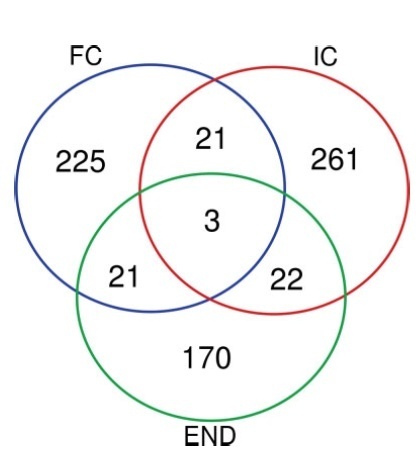
None of the variants identified was common to other samples within the same group, and no mutation was repeated among patients with endometriosis, infertile and fertile controls. In the endometriosis group, nine predicted deleterious mutations were identified, but only one was previously associated to a clinical condition with no endometrial impact. When crossing the mutated genes with the descriptors endometriosis and/or endometrium, the gene CMKLR1 was associated either with inflammatory response in endometriosis or with endometrial processes for pregnancy establishment.
Despite no pattern of mutation having been found, we ponder the small sample size and the analysis on RNA-sequencing data. Considering the purpose of the study of screening and the importance of the CMKLR1 gene on endometrial
Summary
Rev Bras Ginecol Obstet. 2016;38(9):465-470
Infertility has a high prevalence in the general population, affecting 5 to 15% of couples in reproductive age. The assisted reproduction techniques ( ART ) include in vitro manipulation of gametes and embryos and are an important treatment indicated to these couples. It is well accepted that the implantation rate is positively influenced by the morphology of transferred embryos. However, we question if, apart from the assessment of embryo morphology, the number of produced embryos per cycle is also related to pregnancy rates in the first fresh transfer cycle.
To evaluate the clinical pregnancy rate according to the number of formed embryos and the transfer of top quality embryos ( TQEs ).
In a retrospective cohort study, between January 2011 and December 2012 , we evaluated women who underwent intracytoplasmic sperm injection (ICSI), aged < 40 years, andwith at least 1 formed embryo fresh transferred in cleavagestage. These women were stratified into 3 groups according to the number of formed embryos (1 embryo, 2-3 and ≥ 4 embryos). Each group was divided into 2 subgroups according to the presence or not of at least 1 transferred TQE (1 with TQE; 1 without TQE; 2-3 with TQE, 2-3 without TQE; ≥4with TQE; ≥4withoutTQE). The clinicalpregnancy rateswerecomparedineach subgroup based on the presence or absence of at least one transferred TQE.
During the study period, 636 women had at least one embryo to be transferred in thefirst fresh cycle (17.8% had 1 formed embryo [32.7% with TQEversus 67.3% without TQE], 42.1% of women had 2-3 formed embryos [55.6% with TQE versus 44.4% without TQE], and 40.1%ofpatientshad ≥4 formedembryos[73.7%withTQEversus26.3%withoutTQE]).The clinical pregnancy rate was significantly higher in the subgroup with ≥4 formed embryos with at least 1 transfered TQE (45.2%) compared with the subgroup without TQE (28.4%).
Having at least two available embryos and at least one TQE for embryo transfer are predictors of the pregnancy rates.
Summary
Rev Bras Ginecol Obstet. 2017;39(9):488-495
To evaluate the preferences of women and men regarding female pubic hair depilation and identify possible reasons for these preferences.
This is a cross-sectional study of men and women over 18 years old who were invited by the official blog of our institution to respond anonymously to an online and self-administered questionnairemade by the researchers. The analyses weremade using the Statistical Analysis System (SAS, SAS Inc., Cary, NC, US) software, version 9.3, and contingency tables were used to verify the distribution of variables. The univariate statistical analysis was performed using the Pearson chi-squared test, and the differences for values of p < 0.05 were considered significant.
We obtained data from 69,920 subjects (52,787 women and 17,133 men). Themean age was 31.9 years formen, and 28.5 years for women. Most women (64.3%) and men (62.2%) preferred complete removal of female pubic hair, and this preference wasmore pronounced in younger women andmen. Most women reported performing depilation at home (55.8%), with 44.4% using hot wax and 40.1% using a razor blade. About half of the women (44.7%) and men (50.1%) reported sexual activity, having intercourse 2 to 3 times per week. The frequency of intercourse and sexual satisfaction in women correlated with total pubic hair removal.
Most Brazilian women and men prefer the complete removal of female pubic hair, especially those who are younger andmore sexually active.Women who are satisfied with the appearance of their own genitalia have a stronger preference for complete removal of pubic hair.
Summary
Rev Bras Ginecol Obstet. 2012;34(11):524-529
DOI 10.1590/S0100-72032012001100008
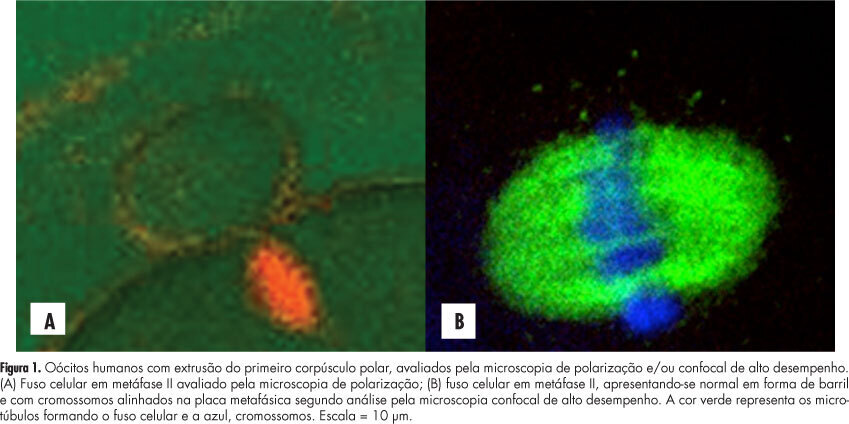
PURPOSE: To evaluate the concordance between polarization microscopy and confocal microscopy techniques in the evaluation of the meiotic spindle of human oocytes matured in vivo. METHODS: Prospective study that evaluated oocytes with the first polar extruded body obtained from infertile women who had undergone ovarian stimulation for intracytoplasmic sperm injection. The oocytes with the first polar extruded body were evaluated by polarization microscopy and were then immediately fixed and stained for microtubule and chromatin evaluation by high-performance confocal microscopy. We determined the correlation of polarization microscopy with confocal microscopy in the detection of meiotic oocyte anomalies, and we also evaluated the percentage of oocytes with a visible and non-visible cell spindle by polarization microscopy and with meiotic normality and abnormalities by confocal microscopy. Confidence intervals, Kappa's index and concordance between the methodologies were calculated, considering immunofluorescence microscopy analysis as the golden-standard for evaluating normal spindle and oocyte chromosome distribution. RESULTS: We observed that 72.7% of metaphase II oocytes with a nonvisible meiotic spindle by polarization microscopy showed no meiotic abnormalities by confocal analysis and 55.6% of metaphase II oocytes with a visible meiotic spindle by polarization microscopy were found to be abnormal oocytes by the confocal analysis. Only 44.4% of oocytes with a visible meiotic spindle by polarization microscopy were found to be normal by confocal analysis. Concordance between the methods was 51.1% (Kappa: 0.11; 95%CI -0.0958 - 0.319). CONCLUSIONS: The low correlation between polarization microscopy and confocal microscopy in the assessment of oocyte meiotic spindle suggests that visualization of the meiotic spindle of human oocytes at metaphase II by polarization microscopy is not a good indicator of oocyte meiotic normality.
Summary
Rev Bras Ginecol Obstet. 2021;43(1):54-60
Scientific information on the impact of the new coronavirus (SARS-CoV-2) on the health of pregnant women, fetuses and newborns is considered of limited confidence, lacking good-quality evidence, and drawing biased conclusions. As a matter of fact, the initial impressions that the evolution of COVID-19 was no different between pregnant and non-pregnant women, and that SARS-CoV-2 was not vertically transmitted, are confronted by the documentation of worsening of the disease during pregnancy, poor obstetric outcomes, and the possibility of vertical transmission. The present article aims to compile the data available on the association of COVID-19 and reproductive events, from conception to birth.