Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(9):562-568
The present comprehensive review aims to show the full extent of what is known to date and provide a more thorough view on the effects of SARS-CoV2 in pregnancy.
Between March 29 and May, 2020, the words COVID-19, SARS-CoV2, COVID- 19 and pregnancy, SARS-CoV2 and pregnancy, and SARS and pregnancy were searched in the PubMed and Google Scholar databases; the guidelines from well-known societies and institutions (Royal College of Obstetricians and Gynaecologists [RCOG], American College of Obstetricians and Gynecologists [ACOG], International Society of Ultrasound in Obstetrics & Gynecology [ISUOG], Centers for Disease Control and Prevention [CDC], International Federation of Gynecology and Obstetrics [FIGO]) were also included.
The COVID-19 outbreak resulted in a pandemic with > 3.3 million cases and 230 thousand deaths until May 2nd. It is caused by the SARS-CoV2 virus and may lead to severe pulmonary infection and multi-organ failure. Past experiences show that unique characteristics in pregnancy make pregnant women more susceptible to complications from viral infections. Yet, this has not been reported with this new virus. There are risk factors that seem to increase morbidity in pregnancy, such as obesity (body mass index [BMI] > 35), asthma and cardiovascular disease. Current reports describe an increased rate of pretermbirth and C-section. Vertical transmission
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(12):563-567
DOI 10.1590/S0100-72032012001200006
PURPOSE: To investigate the relationship between periodontitis and osteoporosis, using a case-control study about periodontal status of postmenopausal women. METHODS: A total of 99 postmenopausal women were divided into three groups: normal bone (Gn, n=45), osteopenia (Gpenia, n=31) and osteoporosis (Gporosis, n=23). The categorization of bone mass was measured by dual energy absorptiometry with X-rays in the lumbar spine (L2 - L4), by assessing bone mineral density. Clinical attachment level (CAL), gingival bleeding index (GI), plaque index (PI), and probing depth (PD) were determined in all participants by a single examiner. The data were submitted to BioEstat 2.0 software through parametric analysis of variance (ANOVA) and the Bonferroni test, with the level of significance set at 5%. RESULTS: Women with osteoporosis presented the highest percentage of periodontal disease, with higher average CAL (2.6±0.4 mm) and PD (2.8±0.6 mm), GI (72.8±25.9 mm) and PI (72.9±24.2 mm). Statistical analysis revealed a significant difference in periodontal situation between Gn and Gporosis (p=0,01) and between Gpenia and Gporosis (p=0,03). CONCLUSION: Osteoporosis may have an influence on periodontal condition, based on the relation between periodontitis and osteoporosis in postmenopausal women.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(11):563-569
DOI 10.1590/S0100-72032010001100008
PURPOSE: to evaluate the evolution of adequacy of the care process among pregnant users of the Brazilian Single Health System (SUS, acronym in Portuguese) and to consolidate a methodology for monitoring the prenatal care. METHODS: this is a multiple time series study with auditing of prenatal cards of pregnant women who were attended for prenatal care in a city of the Brazilian Southeast (Juiz de Fora, Minas Gerais) in the initial semesters of 2002 and 2004 (370 and 1,200 cards, respectively) and gave birth using SUS services in term pregnancies (p < 0.05). A three complementary level sequence was respected: utilization of prenatal care (beginning and number of visits) at level 1; utilization of prenatal care and obligatory clinical-obstetric procedures during prenatal visits (assessment of blood pressure (BP), weight, uterine fundal height (FH), gestational age (GA), fetal heart rate (FHR) and fetal presentation) at level 2; and utilization of prenatal care, obligatory clinical-obstetric procedures and basic laboratory tests, according to the Humanization Program of Prenatal Care and Birth (PHPN, acronym in Portuguese) (ABO/Rh, hemoglobin/hematocrit (Hb/Htc), VDRL, glycemia and urinalisys) at level 3. RESULTS: it was confirmed the high prenatal care coverage (99%), the increased mean number of visits per pregnant woman (6.4 versus 7.2%) and the decreased gestational age at the time of the first visit (17.4 versus 15.7 weeks). The proper registration of procedures and exams (exceptions: fetal presentation and blood typing) has significantly increased: BP (77.8 versus 83.9%); weight (75.4 versus 83.5%); FH (72.7 versus 81.3%); GA (58.1 versus 71.5%); FHR (79.5 versus 86.7%); Hb/Htc (14.9 versus 29%), VDRL (11.1 versus 20.7%), glycemia (16.5 versus 29%) and urinalisys (13.8 versus 29.8%). As a result, there was significant (p < 0.001) improvement of the adequacy between 2002 and 2004: 27.6 versus 44.8% (level 1); 7.8 versus 15.4% (level 2); 1.1 versus 4.5% (level 3). This trend was also noted in care provided by the majority of the municipal services/teams. CONCLUSIONS: the persistence of low adequacy, despite good coverage and PHPN implementation, confirmed the need to increase health managers, professionals and users' compliance with the rules and routines of care, including the institutionalization of a monitoring program of prenatal care.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(9):563-569
To describe a case of vesicouterine fistula and to review the literature related to this condition.
For the review, we accessed the MEDLINE, BIREME and LILACS databases; the references of the searched articles were also reviewed.
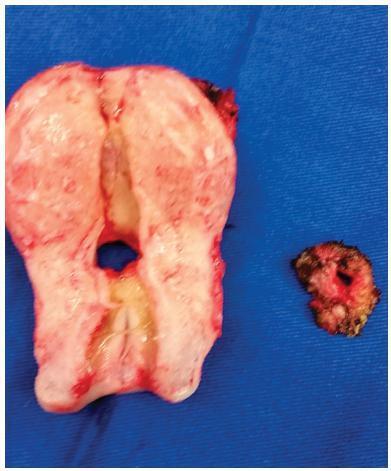
A 38-year-old woman, in the 1st day after her 3rd cesarean, presented heavy hematuria, which was considered secondary to a difficult dissection of the bladder. A total of 6 months after delivery, she failed to resume her regular menstrual cycles and presented cyclic menouria and amenorrhea. At this time, she had two episodes of urethral obstruction by blood clots. She remained without a correct diagnosis until about two years postdelivery, when a vesicouterine fistula was confirmed through cystoscopy. A surgical correction through open abdominal route, coupled with hysterectomy, was performed. After the surgery, the symptoms disappeared. The review showed a tendency of change in the relative frequency of the different types of genitourinary fistulae. Vesicovaginal fistulae, usually caused by inadequate care during labor, are becoming less frequent than those secondary tomedical procedures, such as vesicouterine fistulae. The most common cause of this latter kind of fistula is cesarean section, especially repeated cesarean sections. The diagnosis is confirmed through one or more imaging exams, or through cystoscopy. The most common treatment is surgical, and the routes are: open abdominal, laparoscopic, vaginal or robotic. There are some reports of success with the conservative treatment.
Vesicouterine fistulae are becoming more common because of the increase in the performance of cesarean sections, and the condition must be considered a possible complication thereof.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(7):563-571
DOI 10.1590/S0100-72032004000700009
PURPOSE: to measure changes and predictors of changes in mammographic density of climacteric women, before and one year after hormone replacement therapy. METHODS: seventy climacteric women of 45 years or more participated in the study. They were followed-up at a Climacteric Outpatient Service. All of them used regularly either estrogenic or estroprogestative HRT for one year. They were submitted to one basal mammography and another at the end of the first year. HRT schedules could be different from each other, although with the same bioequivalence. Mammographic density was evaluated blindly at the beginning and at the end of the treatment. Age, ovarian function, time since menopause, body mass index, waist/hip ratio, age at menarche, age at first pregnancy, and smoking were evaluated as well. Mammographic density was classified according to the American College of Radiology BI-RADS system into one of the following four parenchymal patterns: A) entirely liposubstituted breasts, B) liposubstituted breasts with disperse glandular parenchyma, C) heterogeneously dense breasts, and D) extremely dense breasts. We proposed a subdivision of each category in to A e A1, B e B1, C and C1, D and D1 in order to identify smaller variations in mammographic density. Therefore, we attributed initial and final scores of 1-8 to each of the patients according to the mammographic density before and after HRT, corresponding to categories A to D1. The proportions of women that presented increase, decrease and no variation in mammographic density after 1 year of HRT were calculated. In addition, we estimated initial to final score variation using the paired t-test of the Statistical Package for Social Sciences (SPSS). RESULTS: mammographic density increased in 22.9%, decreased in 7.1% and did not change in 70% of the studied cases. A significant difference was observed between the score means before (2.2±1.82) and after HRT (2.5±1.9) (p=0.019). The androgenic distribution of body fat was associated with a denser mammographic pattern. CONCLUSIONS: an increase in mammographic density was shown in women undergoing HRT, and was most pronounced in women with androgenic fat distribution. Additional studies must be carried out in order to evaluate if this increment in mammographic density could impair the mammographic screening of breast cancer.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(11):564-575
The overactive bladder (OAB) has a significant negative impact on the quality of life of patients. Antimuscarinics have become the pharmacological treatment of choice for this condition. The objective of this systematic review and meta-analysis is to examine the evidence from randomized clinical trials about the outcomes of the antimuscarinic drugs available in Brazil on OABs. We searched MEDLINE and the Cochrane Central Register of Controlled Trials from the inception of these databases through to September 2015. The primary outcome measures were the mean decrease in urge urinary incontinence episodes and the mean decrease in the frequency of micturition. The results suggest that there is a moderate to high amount of evidence supporting the benefit of using anticholinergic drugs in alleviating OAB symptoms when compared with placebo. It is still not clear whether any of the specific drugs that are available in Brazil offer advantages over the others. These drugs are associated with adverse effects (dry mouth and constipation), although they are not related to an increase in the number of withdrawals.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(9):564-574
To assess the efficacy of non-surgical treatment for adenomyosis.
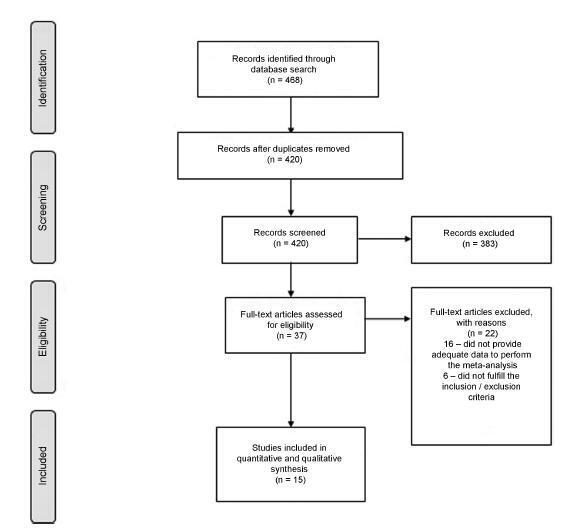
A search was performed by two authors in the Pubmed, Scopus, and Scielo databases and in the grey literature from inception to March 2018, with no language restriction.
We have included prospective randomized studies for treating symptomaticwomen with adenomyosis (abnormal uterine bleeding and/or pelvic pain) diagnosed by ultrasound or magnetic resonance imaging.
Studies were primarily selected by title and abstract. The articles that were eligible for inclusion were evaluated in their entirety, and their data was extracted for further processing and analysis.
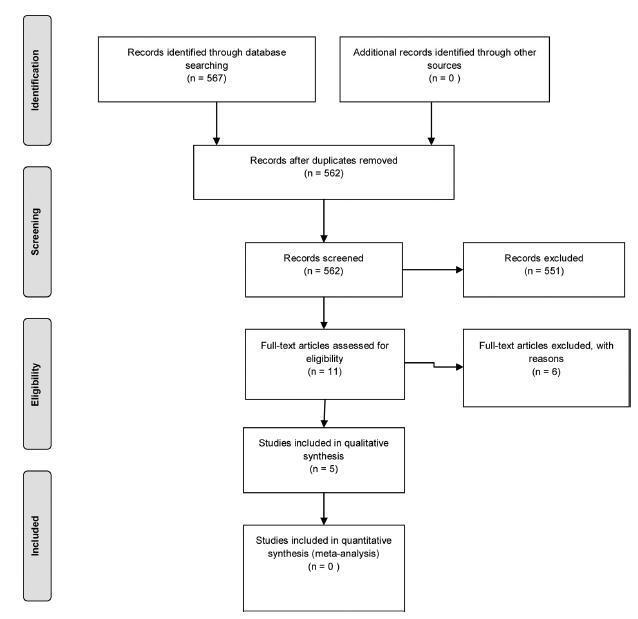
From567retrieved records only 5 remained for analysis. The intervention groups were: levonorgestrel intrauterine system (LNG-IUS)(n= 2), dienogest (n= 2), and letrozole (n= 1). Levonorgestrel intrauterine system was effective to control bleeding when compared to hysterectomy or combined oral contraceptives (COCs). One study assessed chronic pelvic pain and reported that LNG-IUS was superior to COC to reduce symptoms. Regarding dienogest, it was efficient to reduce pelvic pain when compared to placebo or goserelin, but less effective to control bleeding than gonadotropin-releasing hormone (GnRH) analog. Letrozolewas as efficient asGnRHanalog to relieve dysmenorrhea and dyspareunia, but not for chronic pelvic pain. Reduction of uterine volumewas seen with aromatase inhibitors, GnRH analog, and LGN-IUD.
Levonorgestrel intrauterine system and dienogest have significantly improved the control of bleeding and pelvic pain, respectively, in women with adenomyosis. However, there is insufficient data from the retrieved studies to endorse eachmedication for this disease. Further randomized control tests (RCTs) are needed to address pharmacological treatment of adenomyosis.