Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(7):560-569
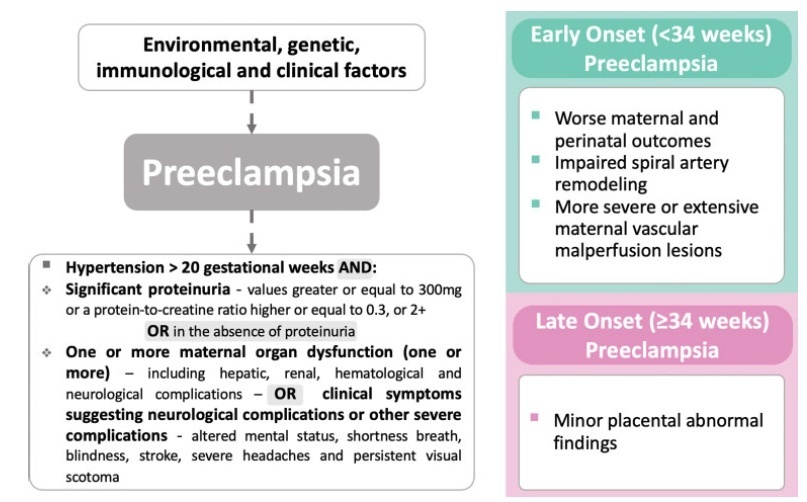
Preeclampsia (PE) is a pregnancy complication associated with increased maternal and perinatal morbidity and mortality. The disease presents with recent onset hypertension (after 20 weeks of gestation) and proteinuria, and can progress to multiple organ dysfunction, with worse outcomes among early onset preeclampsia (EOP) cases (<34 weeks). The placenta is considered the root cause of PE; it represents the interface between the mother and the fetus, and acts as a macromembrane between the two circulations, due to its villous and vascular structures. Therefore, in pathological conditions, macroscopic and microscopic evaluation can provide clinically useful information that can confirm diagnosis and enlighten about outcomes and future therapeutic benefit.
To perform an integrative review of the literature on pathological placental findings associated to preeclampsia (comparing EOP and late onset preeclampsia [LOP]) and its impacts on clinical manifestations.
Cases of EOP presented worse maternal and perinatal outcomes, and pathophysiological and anatomopathological findings were different between EOP and LOP placentas, with less placental perfusion, greater placental pathological changes with less villous volume (villous hypoplasia), greater amount of trophoblastic debris, syncytial nodules, microcalcification, villous infarcts, decidual arteriolopathy in EOP placentas when compared with LOP placentas. Clinically, the use of low doses of aspirin has been shown to be effective in preventing PE, as well asmagnesium sulfate in preventing seizures in cases of severe features.
The anatomopathological characteristics between EOP and LOP are significantly different, with large morphological changes in cases of EOP, such as
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(10):560-568
To characterize the most common peripheral and central neurological disorders during pregnancy.
Original research and review of the literature on neurological complications during pregnancy. We searched for keywords related to the topic on different databases.
Pregnancy involves physiological changes that can trigger peripheral neurological and/or central nervous system pathologies, which can sometimes be associated with hypertensive disorders. A definitive diagnosis of neurological disorders can be made according to the trimester of pregnancy and the clinical findings. Carpal tunnel syndrome and peripheral facial palsy are common peripheral neurological disorders, more frequent in the second half of pregnancy. Central nervous disorders are more complex and a precise diagnosis must be made in order to improve perinatal outcomes, provide correct management and treatment and to prevent acute and long-term complications.
It is possible to achieve a precise diagnosis,management and treatment of neurological disorders during pregnancy, but these require a multidisciplinary approach, crucial to improve perinatal outcomes.

Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(6):560-566
To identify the barriers to provide to women and adequately train physicians on therapeutic abortions in public hospitals in Peru.
Descriptive cross-sectional survey-based study. We invited 400 obstetrics and gynecology specialists from 7 academic public hospitals in Lima and 8 from other regions of Peru. Expert judges validated the survey.
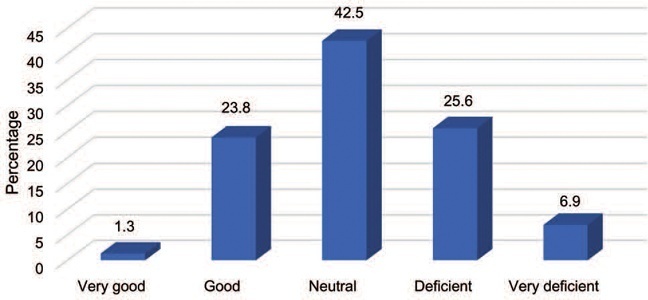
We collected survey results from 160 participants that met the inclusion criteria. Of those, 63.7% stated that the hospital where they work does not offer abortion training. Most of the participants consider that the position of the Peruvian government regarding therapeutic abortion is indifferent or deficient. The major limitations to provide therapeutic abortions included Peruvian law (53.8%), hospital policies (18.8%), and lack of experts (10.6%).
Most surveyed physicians supported therapeutic abortions and showed interest in improving their skills. However, not all hospitals offer training and education. The limited knowledge of the physicians regarding the law and institutional policies, as well as fear of ethical, legal, and religious repercussions, were the main barriers for providing abortions.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(9):560-560
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(9):560-561
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(9):561-566
DOI 10.1590/S0100-72032001000900003
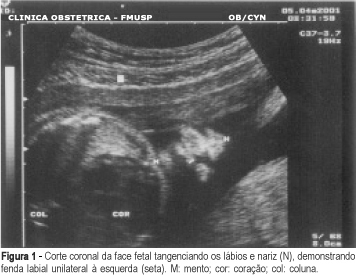
Purpose: to evaluate fetuses with facial cleft as to type of lesion, associated malformations and aneuploidies. Method: the following parameters were evaluated: maternal age and previous history, gestational age at diagnosis, lesion side, type of lesion, presence of associated malformations and aneuploidies, mortality rate and postnatal follow-up. Results: forty fetuses had facial cleft, 18 (45%) cases had cleft lip, 19 (47.5%) had cleft lip and palate, and 3 (7.5%) cases presented with cleft palate. Isolated facial cleft was observed in 10 fetuses (25%), all of them unilaterally located. Aneuploidies were identified in 10/30 (33.33%) of the patients with associated malformations. Cleft lip and palate was more often seen in this group (18/30 - 60%), followed by bilateral lesion (8/30 - 26.7%) and median cleft (10/30 - 33.3%). Conclusion: facial clefts are considered excellent signs for the presence of associated malformations and fetal aneuploidies. Fetuses with facial cleft must be referred to specialized centers in order to have specialized ultrasound and genetic analysis which can provide the best prenatal counseling for these cases. Isolated facial cleft was associated with very good prognosis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(9):561-561
DOI 10.1590/S0100-72031999000900012
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(9):561-561