You searched for:"Geraldo Rodrigues de Lima"
We found (29) results for your search.Summary
Rev Bras Ginecol Obstet. 1998;20(9):533-536
DOI 10.1590/S0100-72031998000900007
Purpose: to evaluate the effects of tamoxifen (TAM) on plasma levels of estradiol, progesterone, prolactin, luteinizing hormone (LH), follicle-stimulating hormone (FSH) and steroid hormone-binding globulin (SHBG) when given to premenopausal women in the doses of 10 and 20 mg/day for 22 days. Patients and Methods: a randomized double-blind study was performed with 43 premenopausal eumenorrheic women. The patients were divided into three groups: A (N = 15, placebo); B (N = 15, TAM 10 mg/day) and C (N = 13, 20 mg/day). They started taking an oral dose of TAM or placebo on the very first day of the menstrual cycle. Two hormone determinations were performed, both on the 22nd day of the menstrual cycle: the first in the cycle that preceded the use of the drug and the second, in the following cycle, after 22 days of using the medication. We used the Levine and Student tests in order to evaluate the homogeneity of the sample and the variation of the hormone determinations respectively. Results:serum levels of estradiol, progesterone and SHBG increased significantly in groups B and C. In group C, we also observed increase in serum level of FSH (p < 0.0045) and a fall in prolactin level (p < 0.0055). Conclusions: TAM promoted a significant increase in serum concentrations of estradiol, progesterone and SHBG either in the doses of 10 or 20 mg/day. However, significant increase in FSH and decrease in prolactin were obtained only with the dose of 20 mg/day.
Summary
Rev Bras Ginecol Obstet. 2006;28(1):54-62
DOI 10.1590/S0100-72032006000100010
Female lower urinary tract symptoms are nonspecific and a clinical evaluation is required to establish the correct diagnosis. Such evaluation should consist of a structured micturition history or questionnaire, physical examination, micturition diary, pad test, and urodynamic evaluation. Urodynamic investigation was developed as an extension of patient history and physical examination in order to reveal the etiology of the patient's complaints. The goal of the present article is to review clinical and subsidiary diagnosis of urinary incontinence.
Summary
Rev Bras Ginecol Obstet. 2002;24(8):547-552
DOI 10.1590/S0100-72032002000800008
Purpose: to evaluate the estrogenic effects of soy phytoestrogens in postmenopausal patients. Method: we selected postmenopausal patients from the Climacteric Service of the Gynecology Department of the Federal University of São Paulo - Escola Paulista de Medicina. The patients were divided into two groups: GI (n=40) received daily 100 mg isoflavone (3 x 33.3 mg/day); and GCtr (n=40) received daily placebo. We included in this study the Kuppermann menopausal index, physical examination and the biochemical determination of total and fractions of cholesterol, triglycerides, estradiol, FSH e LH. We also performed sonographic examination to measure endometrial thickness. To compare baseline and after treatment values of both groups, the nonparametric Kruskal-Wallis test was used for the Kuppermann index, while the t test was performed for other data. Results: evaluation of the Kupperman Menopausal Index, 80% patients of GI showed a decrease in the total score, while the improvement of symptoms in GCtr was 12,5%. The analysis of total cholesterol levels showed that 35 patients of GI had levels above 200 mg/dL, and only 13 of GCtr presented similar levels. The body mass index reduction occurred in GI and the control group showed no changes. We also verified that echo endometrial thickness and FSH levels were similar to baseline values. However the values of estrogen increased after isoflavone treatment. Conclusion: we concluded that 100 mg/day isoflavone may be an alternative treatment for attenuating the climacteric symptoms in 80% of isoflavone users and that it reduced total cholesterol.
Summary
Rev Bras Ginecol Obstet. 2002;24(9):573-577
DOI 10.1590/S0100-72032002000900002
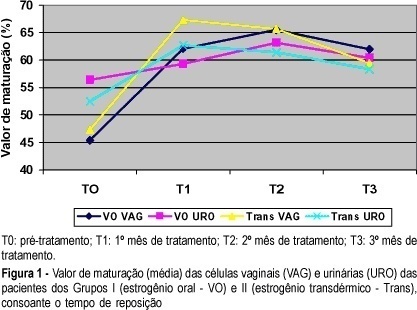
Objective: to study the effects of oral or transdermal estrogen replacement on the lower urinary tract and vagina in postmenopausal women. Methods: we studied 25 postmenopausal women evaluating the oral or transdermic estrogen replacement effects on the vaginal cells and urinary sediment during 3 months. The patients were randomly distributed into 2 groups: Group I, n = 14, treated orally with 0.625 mg equine conjugated estrogen plus 5 mg medroxyprogesterone acetate, daily for 3 months; Group II, n = 11, treated transdermally with 50 mug 17-ß-estradiol, once a week, plus 5 mg medroxyprogesterone. Daily, for 3 months, urinary samples were collected from the first miction in the morning after urogenital antisepsis into sterile tubes. The sample was centrifuged and the sediment was smeared. Vaginal and urinary smears were then fixed in absoluted alcohol and stained by the method of Shorr. Results: the patients who used the oral route presented maturation of the vaginal cells (from 45.4 to 65.5% after 2 months of treatment, maintaing 62% afterwards) but this did not occur with urinary cells (56.4 before treatment versus 60.4% at the end of the period). The transdermal route promoted maturation of vaginal and urinary cells. Conclusion: we have concluded that transdermal estrogens have satisfactory effects both on vaginal and urethral sites. However, with the oral route we did not find the expected results in the urinary tract in all cases.
Summary
Rev Bras Ginecol Obstet. 2000;22(9):585-591
DOI 10.1590/S0100-72032000000900008
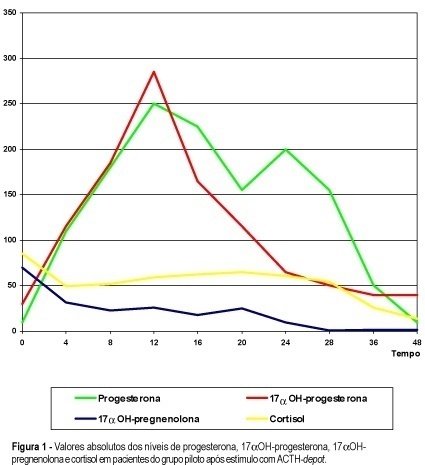
Purpose: to test the adrenal function by a potent stimulus to its reticular layer verifying 3beta-hydroxysteroid dehy-drogenase (3beta-HSD) and 21-hydroxylase (21OH) enzymatic activities. Methods: plasma concentrations of 17alphaOH-pregneno-lone, 17alphaOH-progesterone, cortisol, progesterone, androstenedione, dehydroepiandrosterone (DHEA), dehydroepiandrosterone sulfate (SDHEA) and free testosterone were determined in 39 women, 13 of whom were normal (2 of them used in a pilot study) and 26 had idiopathic hirsutism, 0, 12 and 24 h after injection of ACTH-depot. Results: among hirsute women, we identified different responses that could diagnose any blockage in the steroid pathways leading to the diagnosis of a mild/moderate decreased adrenal function. The 17alphaOH-pregnenolone concentrations varied from 2.0 to 24.6 ng/mL, cortisol values increased from 2.1 to 45.3 and 38.4 mug/dL, 17alphaOH-progesterone levels varied from 50.7 to 346 and 218 ng/mL and progesterone increased from 0.3 to 4.4 and 2.2 ng/mL. Among the reticular layer hormones a rise of SDHEA from 274.7 to 495.5 and 505.8 mg/dL, and of androsterone from 1.1 to 4.0 and 4.5 ng/mL was observed, the levels of free testosterone increased from 1.3 to 1.8 and 2.7 pg/mL and the DHEA levels from 2.4 to 4.7 and 8.5 ng/mL. One patient showed 3beta-HSD deficiency and two others a possible 21OH deficiency. Conclusions: these findings suggest that the ACTH-depot test could be used to exclude the adrenal gland as the possible source of hyperandrogenism in women with idiopathic hirsutism.
Summary
Rev Bras Ginecol Obstet. 2006;28(10):596-600
DOI 10.1590/S0100-72032006001000005
PURPOSE: To analyze gestation evolution and deliveries after myoma treatment by embolization of the uterine arteries. METHODS: In the initial evaluation, 112 patients submitted to embolization of uterine arteries were included for treatment of myoma. From those, only nine wanted to be submitted to conservative treatment in order to keep their reproductive capacity. This procedure was indicated to the nine patients, since they were not susceptible to a conservative surgical treatment. They were submitted to embolization of the uterine arteries with particles of polyvinyl alcohol or embospheres with diameters ranging from 500 to 700 µm, and they have evolved without intercurrence. RESULTS: During the follow-up of these patients, there was a good clinical response with significant reduction in the uterus and myoma volumes. Four of them got pregnant, two had an early abortion and two evolved normally till the end of gestation with a term delivery. One of these had twins. CONCLUSION: Embolization of the uterine arteries is an option for the treatment of uterine myoma, and presents good clinical and anatomical results, allowing patients to preserve their reproductive capacity.
Summary
Rev Bras Ginecol Obstet. 2000;22(10):609-613
DOI 10.1590/S0100-72032000001000002
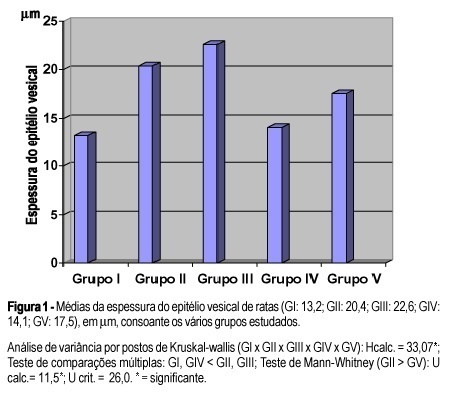
Purpose: the effects of corticosteroids on the female urinary tract are not well understood, specially in climacteric women with or without estrogen replacement therapy. We studied the effects of corticosteroids on the blood vessels and epithelium of the bladder and urethra of female rats. Method: fifty-four female rats were used, divided into five groups. Group I - ten castrated female rats; Group II - eleven castrated female rats which receivedintraperitoneally 15 mg/kg weight prednisolone, for 26 days; Group III - twelve castrated female rats which received the same amount of corticosteroid, during the same time, and subcutaneously 10 mg/kg 17 beta-estradiol, in the last five days before they were sacrificed; Group IV - eleven castrated rats which received placebo for 26 days; and Group V - no castrated female rats which received the same dose of corticosteroid during the same time as in Group II. Results: we observed an average of 1.8 vessels in the bladder of the castrated group which received corticosteroid, a similar number to that of those which received corticosteroid and estrogen, compared with 0.8 vessel in the placebo group. Regarding the urethra, 0.7 vessel was observed in the group which received corticosteroid, as compared with 0.9 vessel in the group treated with corticosteroid associated with estrogen and 0.4 in the placebo group. Regarding the mucous membrane, the vesical epithelium thickness of 14.1 mm in the placebo group increased to 20.6 mm in that with corticosteroid and to 22.6 mm in that with corticosteroid plus estrogen. The urethral epithelium thickness of 12.4 mm in the placebo group increased to 15.1 mm in the group with corticosteroid and to 16.7 mm in that with corticosteroid plus estrogen. Conclusion: corticosteroids significantly increased the vascularization and the thickness of the vesical and urethral epithelia of castrated female rats.