Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):435-435
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(8):435-435
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(8):435-435
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(7):435-441
DOI 10.1590/S0100-72032000000700006
Purpose: to describe sociodemographic characteristics of a group of climacteric women in order to discover the frequency and the variables associated with obesity and android profile of body fat distribution. Methods: an observational study was carried out in 518 patients aged 45 to 65 years, in a climacterium outpatient clinic. Age, color, menopausal status, duration of menopause, physical activity, smoking status, diet, alcohol intake, personal and family antecedents of arterial hypertension, diabetes mellitus, cardiovascular disease, dyslipidemia and obesity were considered. Body mass index and the waist/hip ratio were the dependent variables. For the statistical analysis Wilcoxon test, Pearson's correlation coefficient, with a 5% level of significance, and multivariate analysis using regression model were used. Results: more than two thirds of the participants were nonobese with an android profile and postmenopausal. One fourth had physical activity and were smokers; half reported an inadequate diet and one fifth were alcoholics. Patients with an android profile presented higher mean age than women with gynecoid pattern. Personal antecedents of obesity, arterial hypertension, diabetes and family history of diabetes were related to obesity and android pattern. Postmenopausal status was significantly associated with the android profile. Conclusions: the majority of the participants were nonobese with an android profile, white, postmenopausal, sedentary, neither smokers nor alcoholics. The main factors related to obesity and android pattern were personal antecedents of obesity, arterial hypertension, diabetes, family history of diabetes and particularly, postmenopausal status with android profile.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(8):435-438
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(4):435-441
Antenatal recognition of severe cases of congenital diaphragmatic hernia (CDH) by ultrasound (US) and magnetic resonance imaging (MRI) may aid decisions regarding the indication of fetal endoscopic tracheal occlusion.
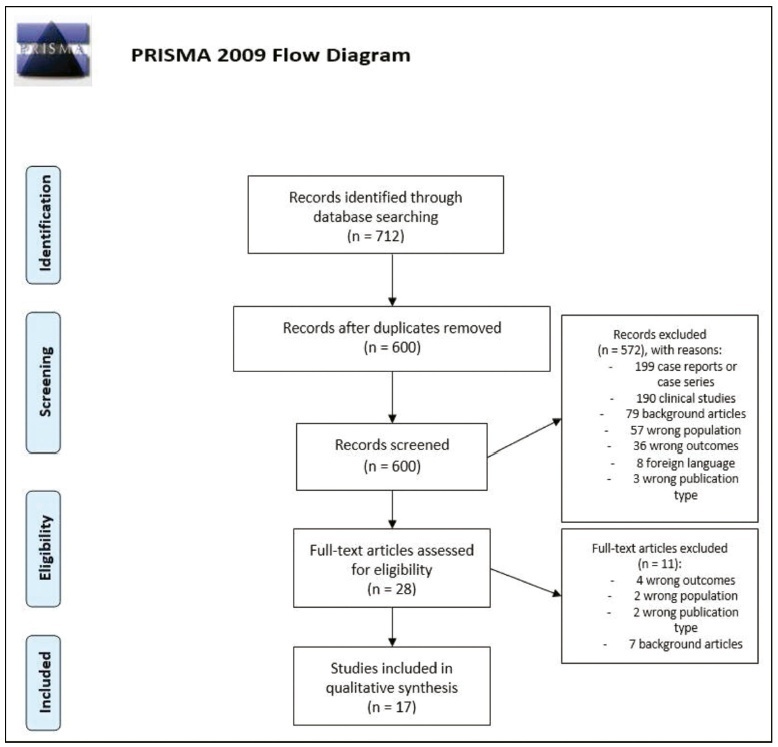
An integrative review was performed. Searches in MEDLINE and EMBASE used terms related to CDH, diagnosis, MRI, and US. The inclusion criteria were reviews and guidelines approaching US and MRI markers of severity of CDH published in English in the past 10 years.
The search retrieved 712 studies, out of which 17 publications were included. The US parameters were stomach and liver positions, lung-to-head ratio (LHR), observed/expected LHR (o/e LHR), and quantitative lung index. The MRI parameters were total fetal lung volume (TFLV), observed/expected TFLV, relative fetal or percent predicted lung volumes, liver intrathoracic ratio, and modified McGoon index. None of the parameters was reported to be superior to the others.
The most mentioned parameters were o/e LHR, LHR, liver position, o/e TFLV, and TFLV.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(8):435-435
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(9):436-442
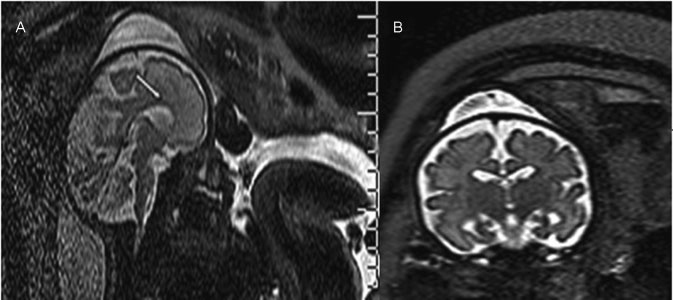
Ventriculomegaly (VM) is one the most frequent anomalies detected on prenatal ultrasound. Magnetic resonance imaging (MRI) may enhance diagnostic accuracy and prediction of developmental outcome in newborns.
The aim of this study was to assess the correlation between ultrasound and MRI in fetuses with isolated mild and moderate VM. The secondary aim was to report the neurodevelopmental outcome at 4 years of age.
Fetuses with a prenatal ultrasound (brain scan) diagnosis of VM were identified over a 4-year period. Ventriculomegaly was defined as an atrial width of 10- 15 mm that was further divided as mild (10.1-12.0 mm) and moderate (12.1-15.0 mm). Fetuses with VM underwent antenatal as well as postnatal follow-ups by brain scan and MRI. Neurodevelopmental outcome was performed using the Griffiths Mental Development Scales and conducted, where indicated, until 4 years into the postnatal period.
Sixty-two fetuses were identified. Ventriculomegaly was bilateral in 58% of cases. A stable dilatation was seen in 45% of cases, progression was seen in 13%, and regression of VM was seen in 4.5% respectively. Fetal MRI was performed in 54 fetuses and was concordant with brain scan findings in 85% of cases. Abnormal neurodevelopmental outcomes were seen in 9.6% of cases.
Fetuses in whom a progression of VM is seen are at a higher risk of developing an abnormal neurodevelopmental outcome. Although brain scan and MRI are substantially in agreement in defining the grade of ventricular dilatation, a low correlation was seen in the evaluation of VM associated with central nervous system (CNS) or non-CNS abnormalities.