Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(9):427-431
DOI 10.1590/S0100-72032013000900008
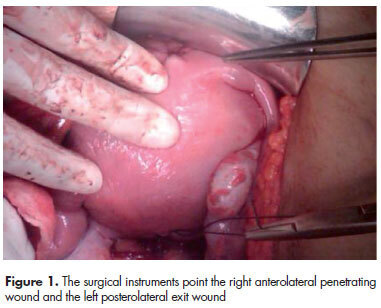
Crime and violence have become a public health problem. Pregnant women have not been the exception and gunshot injuries occupy an important place as a cause of trauma. An important fact is that pregnant women, who suffer trauma, are special patients because pregnancy causes physiological and anatomical changes. Management of these patients should be multidisciplinary, by the general surgeon, the obstetrician and the neonatologist. However, even trauma referral centers could neither have the staff nor the ideal training for these specific cases. In this context we present the following case.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(7):427-435
We performed a systematic review to assess the effectiveness and safety of Tribulus terrestris to treat female sexual dysfunction (FSD).
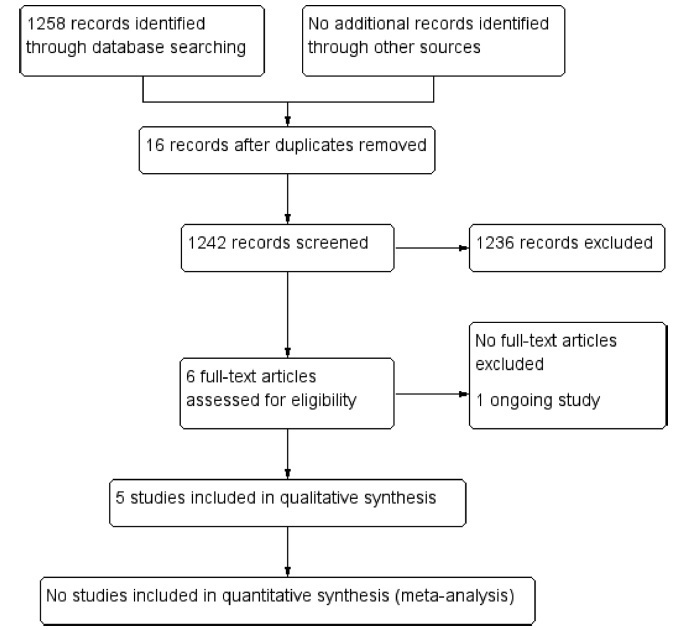
We performed unrestricted electronic searches in the MEDLINE, CENTRAL, EMBASE, LILACS, CINAHL, PsycINFO,WHO-ICTR, Clinicaltrials.gov and OpenGrey databases. Selection of studies We included any randomized controlled trials (RCTs) that compared T. terrestris versus inactive/active interventions. After the selection process, conducted by two reviewers, 5 RCTs (n = 279 participants) were included.
Data extraction was performed by two reviewers with a preestablished data collection formulary.
Due to lack of data and clinical heterogeneity, we could not perform meta-analyses. The risk of bias was assessed by the Cochrane Risk of Bias (RoB) tool, and the certainty of evidence was assessed with Grading of Recommendations, Assessment, Development and Evaluations (GRADE).
After 1 to 3 months of treatment, premenopausal and postmenopausal women randomized to T. terrestris had a significant increase in sexual function scores. Three months of treatment with T. terrestris showed a significant increase in the serum testosterone levels of premenopausal women. There was no report of serious adverse events, and none of the studies assessed health-related quality of life. The certainty of the evidence was very low, whichmeans that we have very little confidence in the effect estimates, and future studies are likely to change these estimates.
MoreRCTs are needed to supportor refute the use of T. terrestris. The decision to use this intervention should be shared with the patients, and the uncertainties around its effects should be discussed in the clinical decision-making process. Number of Protocol registration in PROSPERO database: CRD42019121130
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(8):427-427
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(8):427-427
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(8):428-434
DOI 10.1590/S0100-72032007000800008
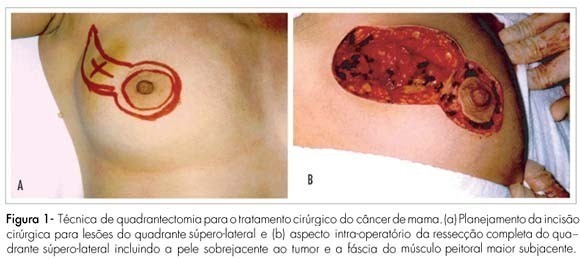
The surgical strategy for breast cancer treatment has changed considerably over the last decade. The breast conserving surgery (BCS) is the standard treatment for early stage breast cancer nowadays. With the current population breast cancer screening programs and the emerging use of systemic neoadjuvant therapy, an increasing number of patients have been eligible to BCS. However, several specific factors must be considered for the therapeutic planning for these patients. This review provides a surgical methodology overview for the BCS in breast carcinoma.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(9):428-435
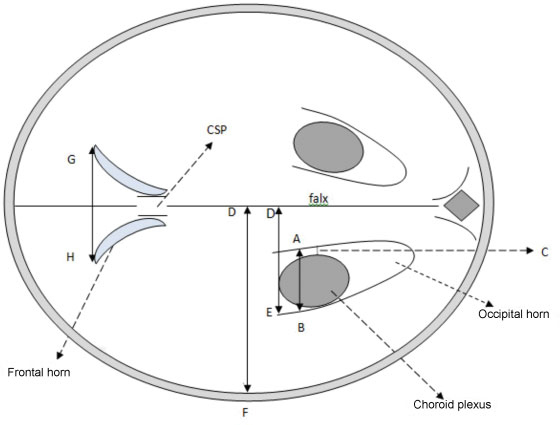
This study was done to evaluate the normal fetal cerebral lateral ventricle dimensions with transabdominal ultrasonography. The atrial width (AW), ventricle-tochoroid measurement (V-C), ventricle-to-hemisphere ratio (VHR), and combined anterior horn measurement (CAHM) were taken.
This was a cross-sectional study involving 400 normal singleton pregnant subjects whose gestational ages were between 14 and 40 weeks. Transabdominal sonography was performed to obtain the values of the fetal cerebral lateral ventricle (FCLV) parameters. Data were reported as mean standard deviation (SD) for continuous variables. The degrees of correlation between FCLV parameters and the estimated gestational age (EGA) were obtained using Pearson's correlation. Regression equations were used to generate the reference limits for the FCLV measurements.
The values of AW, V-C measurements and CAHM increased with advancing gestation. The mean values of the AW, V-C and CAHM from 14 to 40 weeks increased from 6.60 0.94 mm to 9.75 0.07 mm (R2 = 0.114), 0.80 0.00 mm to 1.90 0.14 mm (R2= 0.266), and 6.95 0.06 mm to 23.07 4.02 mm (R2= 0.692) respectively, while the mean VHR decreased from 61.20 1.60% to 42.84 2.91% (R2 = 0.706) over the same period.
The AW, V-C, and CAHM increase, while VHR decreases with advancing gestation.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(9):428-433
DOI 10.1590/SO100-720320150005283
Evaluation of maternal, obstetrics e neonatal features in both spontaneous preterm births (PTB) with or without preterm premature rupture of membranes (PPROM).
Retrospective study of single fetus pregnancies with PTB between 2003 and 2012. Inclusion criteria: PTB associated with ou without PPROM. Exclusion criterias: PTB by medical indication due to fetal/maternal disease and all non accessible or incomplete clinical files. Different characteristics were compared between two groups of PTB: spontaneous PTB without PPROM (sPTB) versus PPROM. Kolmogorov-Smirnov, Levene, χ2, t Student and Mann-Withney tests were used for statistical analysis.
From 2,393 PTB of single fetus, 1,432 files were analysed, from which 596 were sPTB and 836 PPROM. The socioeconomic conditions were similar in both groups. Multiparity (50.7versus 40.3%), personal history of previous PTB (20.8 versus 10.2%), cervical length (18.2 versus 27.2 mm), lower body index mass (23.4 versus 24.3 kg/m2) and higher infectious parameters (Protein C Reactive: 2.2 versus 1.2 mg/L; Leukocytes: 13.3 versus 12.4x109) were more frequent in PBTs (p<0,001). Neonatal outcomes, specially neurologic outcomes (4.7 versus 2.8%, p<0,001), were worst in PBTs.
PTB with or without PPROM has a complex etiology. From all evaluated features in our study, only maternal thinness, multiparity with a previous PTB, the cervical length and worst systemic infections parameters were significant in sPTB. This group also showed worst neonatal outcomes, specially on neurological outcomes.