Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(6):377-382
DOI 10.1590/S0100-72032001000600006
Purpose: to evaluate a group of pregnant women with human papillomavirus (HPV) infection, analyzing age, gestational age, number of gestations and cytological findings. Methods: in the period from July 1993 to December 1998, 245 pregnant patients seen in our service presented cytological alterations compatible with HPV infection, associated or not with cervical intraepithelial neoplasia (CIN) grade 1. Clinical data were related to age, gestational period (first or second half), number of gestations and cytological finding of Trichomonas vaginalis, Candida sp and clue cells. The control group consisted of 386 pregnant patients seen during the same period and without cytological signs of HPV infection. In the statistical analysis, chi² (chi-square) test was used with Yates correction and a significance level lower than 0.05. Results: HPV infection was more frequent among pregnant women younger than 20 years old (45.3% versus 28.2%, p<0.001). The most frequent cytological finding, among the pregnant women with HPV infection, was the presence of clue cells, compared to the controls (21.6% versus 12.4%, p<0.02). Clue cells were more frequent in pregnant women with HPV infection in the second half of gestation and older than 20 years (27% versus 12.2%, p<0,01). The difference regarding number of gestations was not significant. Conclusion: HPV infection was more frequent among pregnant women younger than 20 years old. Clue cells and HPV were the most frequent cytological findings in pregnant women older than 20 years and in the second half of gestation.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(7):379-383
Perineal trauma is a negative outcome during labor, and until now it is unclear if the maternal position during the second stage of labormay influence the risk of acquiring severe perineal trauma. We have aimed to determine the prevalence of perineal trauma and its risk factors in a low-risk maternity with a high incidence of upright position during the second stage of labor.
A retrospective cohort study of 264 singleton pregnancies during labor was performed at a low-risk pregnancymaternity during a 6-month period. Perineal trauma was classified according to the Royal College of Obstetricians and Gynecologists (RCOG), and perineal integrity was divided into three categories: no tears; first/ second-degree tears + episiotomy; and third and fourth-degree tears. A multinomial analysis was performed to search for associated factors of perineal trauma.
From a total of 264 women, there were 2 cases (0.75%) of severe perineal trauma, which occurred in nulliparous women younger than 25 years old. Approximately 46% (121) of the women had no tears, and 7.95% (21) performed mediolateral episiotomies. Perineal trauma was not associated with maternal position (p = 0.285), health professional (obstetricians or midwives; p = 0.231), newborns with 4 kilos or more (p = 0.672), and labor analgesia (p = 0.319). The multinomial analysis showed that white and nulliparous presented, respectively, 3.90 and 2.90 times more risk of presenting perineal tears.
The incidence of severe perineal trauma was low. The prevalence of upright position during the second stage of labor was 42%. White and nulliparous women were more prone to develop perineal tears.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(6):379-386
Several factors might affect the health and the quality of life of women who had a severe maternal morbidity (SMM) or a maternal near-miss (MNM) episode. The objective of the present study was to explore the perspectives of the professionals on the repercussions of SMM or of MNM after interviewing women who survived such episodes.
Selected cases that captured the attention of professionals were reported. The professionals built individually 10 narratives, which were analyzed with the technique of content analysis.
According to the perspectives of the professionals, women surviving a severe maternal condition and their families experienced clinical and psychosocial consequences. Some cases portrayed the intense psychological distress in mourning for the loss of the fetus or of their reproductive capacity and changes in family dynamics generating emotional overload, depression, and gender violence.
The analysis of narratives may offer an idea on the complexity of the perception of care by professionals and on the need for an interdisciplinary follow-up of women surviving an SMM or an MNM episode.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(8):379-383
DOI 10.1590/S0100-72032013000800008
PURPOSE: It was to determine the prevalence of Chlamydia trachomatis and the risk factors associated with infection in endocervical specimens from women seen in outpatient Obstetrics and Gynecology. METHODS: Samples of endocervical secretion of 200 women treated at the University Hospital of the Federal University of Rio Grande were analyzed for the presence of C. trachomatis by polymerase chain reaction (PCR) using primers that amplify CT05/CT06 281 base pairs of the main outer membrane protein of C. trachomatis. All participants completed a pre-coded and self-report questionnaire. Data were analyzed with the SPSS 17.0 software; for multivariate analysis it was used Poisson regression. RESULTS: Of the 200 women who were included in the study, the prevalence of infection with C. trachomatis was 11% (22 patients) and these 55 (27.5%) were positive for HPV. Risk factors associated with infection by C. trachomatis were: 8 years or less of schooling (p<0.001), family income below the poverty level (p=0.005), first intercourse at age 15 or less (p=0.04) and being a carrier of the virus HIV (p<0.001). After multivariate analysis, only the variables of schooling or less than eight years (PR 6.0; 95%CI 1.26 - 29.0; p=0.02) and presence of HIV (RP 14.1; 95%CI 3.4 - 57.5; p<0.001) remained statistically significant. CONCLUSIONS: The prevalence of C. trachomatis in endocervical specimens by PCR was 11%. The factors associated with a higher infection by C. trachomatis were lower education and being HIV positive.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(8):379-383
DOI 10.1590/S0100-72032008000800002
PURPOSE: to verify the association of osteoporosis with periodontal disease. METHODS: the study has included 39 postmenopausal women divided in three groups according to bone mass categories, through evaluation of mineral bone density (MBD), measured by X-ray double emission absorbimetry in the lumbar area (L1-L4): ): normal bone; osteopenia and osteoporosis. In all the participants the Clinical Insertion Level (CIL) index has been determined at the research onset and after one year, by the same examiner. The periodontal situation data have been submitted to statistical analysis with the paired t-Student test. RESULTS: the periodontal exam has shown that postmenopausal women in the osteopenia presented lower CIL at the initial periodontal clinical exam (2.1±1.1 mm), while the ones in the normal bone showed less teeth support tissue loss after one year (3.1±1.6 mm). The statistical analysis has shown that there was no significant difference for the periodontal situation in the normal bone, but there was significant statistical difference for the osteopenia and osteoporosis patients, when CIL values from both evaluation periods were compared. CONCLUSIONS: it is concluded that postmenopausal osteoporosis may be a possible risk factor for periodontal disease.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(7):379-379
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(7):379-379
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(1):38-42
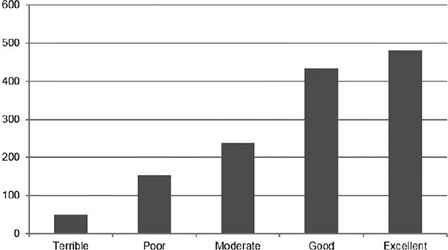
Pain is the primary limitation to performing hysteroscopy. We aimed to evaluate the predictive factors of low tolerance to office hysteroscopic procedures. Methods Retrospective cohort study of the patients who underwent office hysteroscopy from January 2018 to December 2020 at a tertiary care center. Pain tolerance to office-based hysteroscopy was subjectively assessed by the operator as terrible, poor, moderate, good, or excellent. Categorical variables were compared with the use of the Chi-squared test; an independent-samples t-test was conducted to compare continuous variables. Logistic regression was performed to determine the main factors associated with low procedure tolerance.
A total of 1,418 office hysteroscopies were performed. The mean age of the patients was 53 ± 13.8 years; 50.8% of women were menopausal, 17.8% were nulliparous, and 68.7% had a previous vaginal delivery. A total of 42.6% of women were submitted to an operative hysteroscopy. Tolerance was categorized as terrible or poor in 14.9% of hysteroscopies and moderate, good, or excellent in 85.1%. A terrible or poor tolerance was more frequently reported in menopausal women (18.1% vs. 11.7% in premenopausal women, p = 0.001) and women with no previous vaginal delivery (18.8% vs. 12.9% in women with at least one vaginal birth, p = 0.007). Low tolerance led more often to scheduling a second hysteroscopic procedure under anesthesia (56.4% vs. 17.5% in reasonable-to-excellent tolerance, p < 0.0005).
Office hysteroscopy was a well-tolerated procedure in our experience, but menopause and lack of previous vaginal delivery were associated with low tolerance. These patients are more likely to benefit from pain relief measures during office hysteroscopy.