You searched for:"Heitor Ricardo Cosiski Marana"
We found (13) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(9):549-552
DOI 10.1590/S0100-72031999000900008
Purpose: to evaluate the correlation between clinical and surgical staging of patients with vulvar carcinoma, according to the "Federação Internacional de Ginecologia e Obstetrícia" (FIGO 95). Methods: the authors studied 66 consecutive cases of vulvar carcinoma from 1977 to 1997. All patients were clinically staged to verify size and localization of the lesion as well as inguinal lymph node involvement and invasion of other organs. Forty-four patients were submitted to surgical treatment and 34 could be staged according to FIGO 95. Results: among the 34 patients staged through surgery, 17 (50%) showed agreement between clinical and surgical staging. Thus, in 17 patients the staging was different and in these the surgical staging was higher than the clinical in 13 cases and lower in 4 cases. We found in the clinical staging I, 2 cases that were surgical stage II and 1 case that was surgical stage III. Conclusion: the surgical staging could detect lymph node metastasis in patients with clinically negative nodes, as well as exclude false-positive cases. The clinical staging was not accurate for patients with vulvar carcinoma.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(2):67-74
DOI 10.1590/S0100-72032008000200004
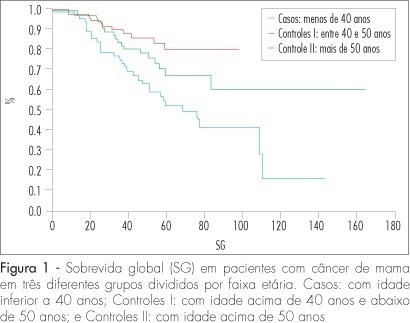
PURPOSE: to compare the epidemiologic and clinical characteristics, and the follow-up of breast cancer in women diagnosed under and over 40 years of age. METHODS: a retrospective study, case-control type, with analysis of information obtained from medical records of patients attended from January 1994 to June 2004. Cases of intraductal carcinoma and at stage IV were excluded. Three groups were formed: patients under 40 years old at the diagnosis (n=72); patients between 40 and 50 (n=68) and patients over 50 (n=75). Data about age at the moment of diagnosis, lesion largest diameter, clinical stage, type, histological grade, presence of hormonal receptors and state of the lymph nodes were collected and analyzed. The chi2 test was used for qualitative variables. For quantitative variables without normal distribution (such as number of axillary nodes with metastasis and follow-up duration), the Kruskal-Wallis' test was used. For delineating the curves of free-of-disease and global survival, the log-rank test was used. RESULTS: there was no difference among the groups in the stage distribution, concerning the tumoral differentiation grade or in the distribution of histological types, and in the estrogen receptor and c-erb-B2 expression. Difference was found in the RP expression, which was less frequent in the group of patients under 40, than in the group of patients over 50 (36.2% versus 58.4%) respectively. There was no difference among the groups in the mean tumoral diameter (5.1, 4.7 and 5 cm, respectively). There was also no difference among the groups, concerning the rate of axillary lymph node metastasis (63.9, 46.9 and 50%, respectively). The average follow-up was 54 months for all the groups. Disease recurrence occurred in 22.6% of patients under 40 years old, in 60% of patients between 40 and 50, and in 22.6% of patients over 50, with a significant difference among groups (p<0.0001). Death caused by the disease was higher among patients under 40 (46.9%) than among patients between 40 and 50 (26.9%) and over 50 (22.6%), p=0.0019. The logistic analysis showed that "age under 40" and the "presence of more than one metastatic axillary node" were independent death risk factors. CONCLUSIONS: age under 40 is an independent risk factor for breast cancer. The traditional prognostic indicators, such as stage, tumoral diameter, axillary involvement and presence of hormonal receptors are not associated with the disease evolution.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(8):672-673
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):79-87
DOI 10.1590/S0100-72032000000200004
Purpose: to assess the esthetic results and personal satisfaction of patients submitted to conservative surgery for cancer of the breast. The study was conducted on 44 patients with breast cancer diagnosed at the mastology outpatient clinic of HCFMRP-USP from January 1990 to December 1994, who fulfilled inclusion criteria according to a previously established protocol. The study consisted of analysis of the esthetic results after conservative treatment of breast cancer and analysis of the degree of patient satisfaction, with a comparison of the morphometry of the treated breast to that of the normal breast. The results were obtained on the basis of five previously established parameters using the esthetic evaluation score proposed by Westreich¹. Methods: of the 44 patients studied, 10 had been submitted to neoadjuvant chemotherapy (CT) because they presented locally advanced tumors, and 2 because of an unfavorable tumor/breast ratio for conservative treatment. Mean follow-up time was 65 months. All 27 patients followed-up at the outpatient clinic received a convocation letter. An evaluation questionnaire was applied to the 20 patients who came to the clinic, followed by breast measurement. Fifteen of these patients had been submitted to surgery with separate incisions and 5 to surgery with a single incision. Results: according to morphometry, the results were classified as excellent in 17 cases (85%), as good in two (10%), and as poor in only one case (5%), an evaluation comparable to the subjective evaluation made by the patients themselves. Considered separately, both measurement "A" (distance from the manubrium of the sternum to the nipple) and measurement "B" (distance from the cranial articulation of the xyphoid appendix to the nipple) showed a greater discriminative power than the measurements as a whole, since with these measurements the cases classified as poor by the patients would have also been classified as poor according to these same criteria separately (A and/or B). Conclusion: there was a significant difference in esthetic results between surgical treatment with a single incision or separate incisions, with the separate incision providing better results. There was high agreement between the classification made by the patients and the morphometric results obtained by us.