You searched for:"Gustavo Salata Romão"
We found (13) results for your search.Summary
Rev Bras Ginecol Obstet. 2012;34(12):575-581
DOI 10.1590/S0100-72032012001200008
PURPOSE: To compare serum anti-Mullerian hormone (AMH) levels on the seventh day of ovarian stimulation between normal and poor responders. METHODS: Nineteen women aged ≥35, presenting with regular menses, submitted to ovarian stimulation for assisted reproduction were included. Women with endometriosis, polycystic ovarian syndrome or those who were previously submitted to ovarian surgery were excluded. On the basal and seventh day of ovarian stimulation, a peripheral blood sample was drawn for the determination of AMH, FSH and estradiol levels. AMH levels were assessed by ELISA and FSH, and estradiol by immunochemiluminescence. At the end of the stimulation cycle patients were classified as normal responders (if four or more oocytes were obtained during oocyte retrieval) or poor responders (if less than four oocytes were obtained during oocyte retrieval or if the cycle was cancelled due to failure of ovulation induction) and comparatively analyzed by the t-test for hormonal levels, length of ovarian stimulation, number of follicles retrieved, and number of produced and transferred embryos. The association between AMH and these parameters was also analyzed by the Spearman correlation test. RESULTS: There was no significant difference between groups for basal or the seventh day as to AMH, FSH and estradiol levels. There was a significant correlation between seventh day AMH levels and the total amount of exogenous FSH used (p=0.02). CONCLUSIONS: AMH levels on the seventh day of the ovarian stimulation cycle do not seem to predict the pattern of ovarian response and their determination is not recommended for this purpose.
Summary
Rev Bras Ginecol Obstet. 2022;44(6):621-628
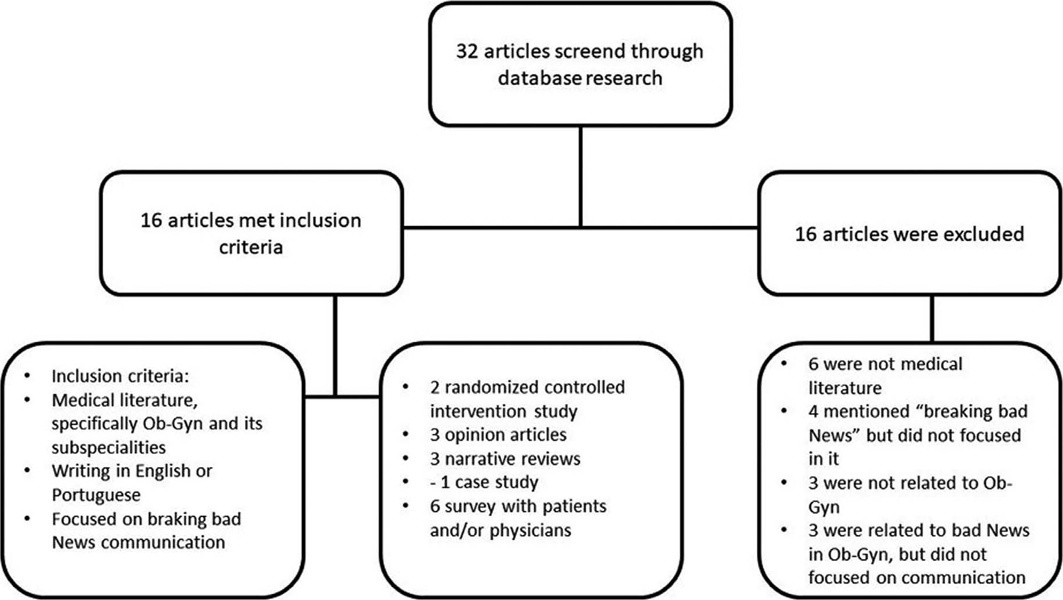
Breaking bad news is common in obstetrics and gynecology (ob-gyn). However, it is difficult, and few doctors receive training on how to deal with this situation. This narrative review aims to gather, analyze, and synthesize part of the knowledge on the area, focused on Ob-Gyn. Among the 16 selected articles, two are randomized controlled intervention studies, and most studies refer to obstetrics. The results found by us pointed out that simulation, feedback/debriefing, lectures, and protocols could improve doctors’ performance in communicating bad news. For patients, the context and how the information is transmitted seem to impact more than the content of the news. Ob-Gyn doctors could benefit from specific protocols and education, given the specialty’s particularities. There is a lack of evidence about the most effective way to conduct such training. Finding validated ways to quantify and classify studies’ results in the area, which would allow for the objective analysis of outcomes, is one of the biggest challenges concerning this topic.
Summary
Rev Bras Ginecol Obstet. 2005;27(2):64-68
DOI 10.1590/S0100-72032005000200004
PURPOSE: to determine the frequency of Mycoplasma hominis and Ureaplasma urealyticum infection, and relate it to the associated clinical variables of infertile women. METHODS: transversal study involving 322 infertile women, submitted to collection of endocervix swab for research of Mycoplasma hominis and Ureaplasma urealyticum infecction, from October 2002 to May 2004. All patients were submitted to a basic infertility investigation protocol. As control, a historical series of 51 non-pregnant women previously investigated as for the studied infectious agents, was used. RESULTS: the frequency of Mycoplasma hominis and Ureaplasma urealyticum infection was 4.9% in the infertile women and 13.8% in the control group. Among the infertile patients, a relationship between the presence of the two agents and changes in the histerosalpingography result (OR: 3.20; IC 95%: 1.05-9.73), presence of dyspareunia (OR: 10.72; IC 95%: 3.21-35.77) and vaginal discharge (OR: 8.5; IC 95%: 2.83-26.02), besides endocervical culture positive for Escherichia coli (OR: 6.09; IC 95%: 4.95-52.25) was observed. CONCLUSION: Mycoplasma hominis and Ureaplasma urealyticum infection rate is low in infertile patients and is associated with reproductive sequels.
Summary
Rev Bras Ginecol Obstet. 2004;26(9):727-733
DOI 10.1590/S0100-72032004000900009
PURPOSE: to evaluate the results of ovulation hyperinduction followed by in vitro fertilization (IVF) in women with polycystic ovary syndrome (POS), as compared to normal cycle women. METHODS: a controlled retrospective study conducted on 36 women with POS (POS group) and on 44 women with infertility due to mild male factor (control group), submitted to IVF from 1997 to 2003. Subject ages ranged from 18 to 36 years. Ovulation hyperinduction was obtained with recombinant follicle-stimulating hormone and a gonadotrophin-releasing hormone agonist. The analyzed variables were the follicles with a mean diameter of 14 to 17 mm and the follicles with diameters of 18 mm or above on the day of human chorionic gonadotrophin administration, percentage of follicles >18 mm, the number of retrieved oocytes, fertilization rate, cleavage rate, incidence of ovarian hyperstimulation syndrome (OHS), clinical pregnancy rate, and abortion rate. The variables were analyzed by the unpaired t test, Fisher exact test and Mann-Whitney test, with level of significance set at p<0.05. RESULTS: the POS group presented a larger number of retrieved follicles, most of them measuring 14 to 17 mm in diameter, compared to the control group (64.8 vs 53.9%), a lower fertilization rate (59.43 vs 79.57%) and a higher incidence of OHS (38.9 vs 9.1%). The number of retrieved oocytes, cleavage rates, pregnancy rates per embryo transfer, abortion rates and live born rates did not differ between groups. CONCLUSION: the success of IVF is impaired in women with POS due to their larger number of retrieved follicles of reduced diameter, reduced fertilization rate and high OHS rates.
Summary
Rev Bras Ginecol Obstet. 2022;44(9):819-820