Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(7):358-365
DOI 10.1590/S0100-72032007000700006
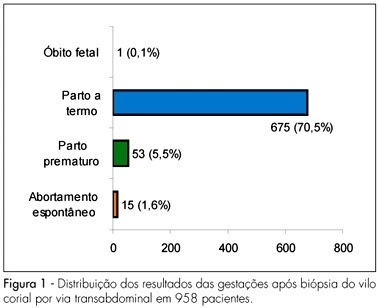
PURPOSE: to evaluate fetal maternal complications after chorionic villus sampling (CVS) for prenatal diagnosis of genetic disorders in pregnant women of Salvador (BA), Brazil. METHODS: case-series study of 958 pregnancies with high risk for chromosomal abnormality submitted to CVS transabdominal between the ninth to the 24th week of gestation, using an ultrasound-guided 18G 3½ spinal needle, from 1990 to 2006. The variables for the analysis of immediate complications were uterine cramps, subchorionic hematoma, accidental amniotic cavity punction, pain in the punction area, amniotic fluid leakage, abdominal discomfort, fetal arrhythmias and vaginal bleeding, and of late complication, abdominal pain, vaginal bleeding, amniotic fluid leakage, infection and spontaneous miscarriage. Premature labor, obstetrical complications (abruption placenta and placenta previa) and newborn malformation were also studied. Qui-square, Student’s "t" or Mann-Whitney tests were used for the statistical analysis; the significance level was 5%. RESULTS: maternal mean age was 36.3±4.9 years old. Immediate complications ware found in 182 (19%) cases (uterine cramp in 14%, subchorionic hematoma in 1.8% and accidental amniotic cavity punction in 1.3%). Late complications were found in 32 (3.3%) cases (vaginal bleeding in 1.6%, abdominal pain in 1.4%, amniotic fluid leakage in 0.3% and spontaneous miscarriage in 1.6% cases). There was no case of abruption placentae, placenta previa or fetal malformation. CONCLUSIONS: CVS is a simple and safe procedure. CVS should be performed in high risk pregnant patients who need prenatal diagnosis of fetal chromosomal abnormalities.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(6):358-364
DOI 10.1590/S0100-72032006000600007
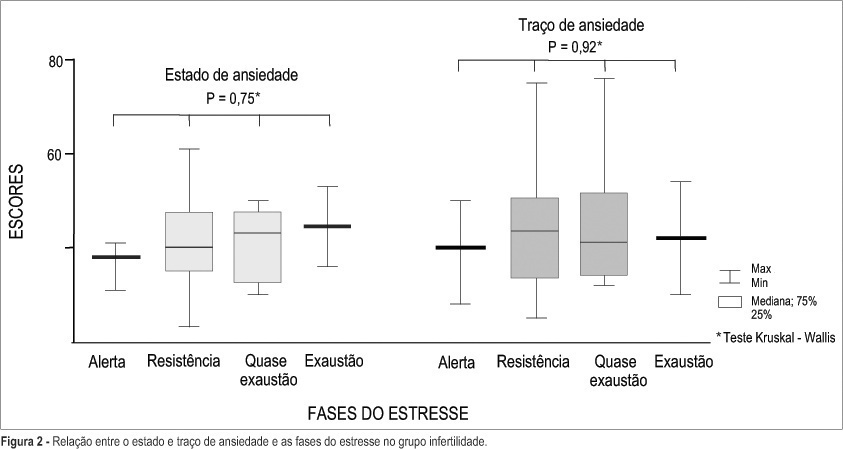
PURPOSE: to assess the frequency of stress and anxiety levels in infertile women, in order to obtain data for specific psychological intervention. METHODS: a cross-sectional study involving 152 infertile (mean age 30.3±5.4 years), and 150 healthy control women (25.7±7.9 years). All patients were evaluated with the Lipp's Inventory of Stress Symptoms and the State-Trait Anxiety Inventory. Considered dependent variables were: stress frequency and anxiety scores (state and trait). Statistical analysis was performed by the chi2 and Mann-Whitney tests, and logistical regression to test associations between response variables and considered risk factors. Statistical significance was defined as p<0.05. RESULTS: the stress was more frequent in the infertile group than in the control group (61.8 and 36.0%, respectively); however, no significant differences were observed between groups in relation to stress phases and predominant symptoms. With respect to anxiety, there were no significant differences between infertile and control groups as to median state scores (39.5 and 41.0, respectively) and anxiety trait scores (44.0 and 42.0, respectively). Factors significantly associated with greater risk for high anxiety scores in the infertile group were: unawareness of the causal factor, diagnostic phase investigation, and lack of children from other marriages. CONCLUSIONS: it can be concluded that infertile women are more vulnerable to stress; however, they are capable of adapting themselves to stressful events without serious physical or psychological compromise.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(7):359-359
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(5):359-364
DOI 10.1590/S0100-72032003000500009
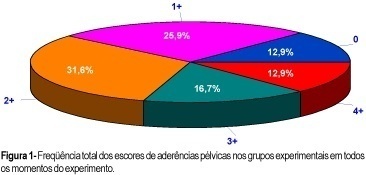
PURPOSE: to evaluate the degree of pelvic adhesions in function of time and the different substances used in its prophylaxis. MATERIAL AND METHODS: prospective study with 120 female, albino, virgin Wistar rats, 3 to 4 months of age, weighing approximately 250 g, randomly divided into 10 groups of 12 animals each: control, without lesion; lesions and without treatment; lesions + 0.9% physiologic saline, lesions + Ringer lactate; lesions + 32% dextran 70; lesions + Ringer lactate/heparin; lesions + Ringer lactate/dexamethasone; lesions + Ringer lactate/hydrocortisone/dexamethasone/ampicillin; lesions + Ringer lactate/albumin, and lesions + 1% carboxymethylcellulose. The animals were anesthetized and two types of lesions (scarification and electrocauterization) were performed in the uterine horns, followed by treatment with the solutions, intraperitoneally, to prevent pelvic adhesions. On the 7th, 14th and 28th postoperative days, moments M1, M2 and M3, respectively, the presence of adhesions was evaluated in 4 rats of each group. The methods applied to the quantification of the adhesions were based on Cohen's classification, with scores varying from 0 to 4+ according to the amount, characteristics and location of the adhesions. Statistical analysis was performed by parametric tests for analysis of variance and the Kruskal-Wallis test. RESULTS: the best treatments for prevention of pelvic adhesions in female rats were Ringer lactate/dexamethasone (score 1+ prevalence), 32% dextran 70 to (score 2+ prevalence) and Ringer lactate/hydrocortisone/dexamethasone/ampicillin (score 2+ prevalence). The postoperative period, represented by moment M3, and the surgical technique, predominantly with score 0, influenced adhesiolysis and maintenance of pelvic adhesions in female rats. CONCLUSIONS: the prevention of pelvic adhesions in female rats begins with the surgical process at a smaller extent of tissue damage. The use of prophylactic substances (solutions) had a varied effectiveness, since some were more efficient than others.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(6):359-360
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(6):359-359
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(8):359-365
DOI 10.1590/SO100-720320150005415
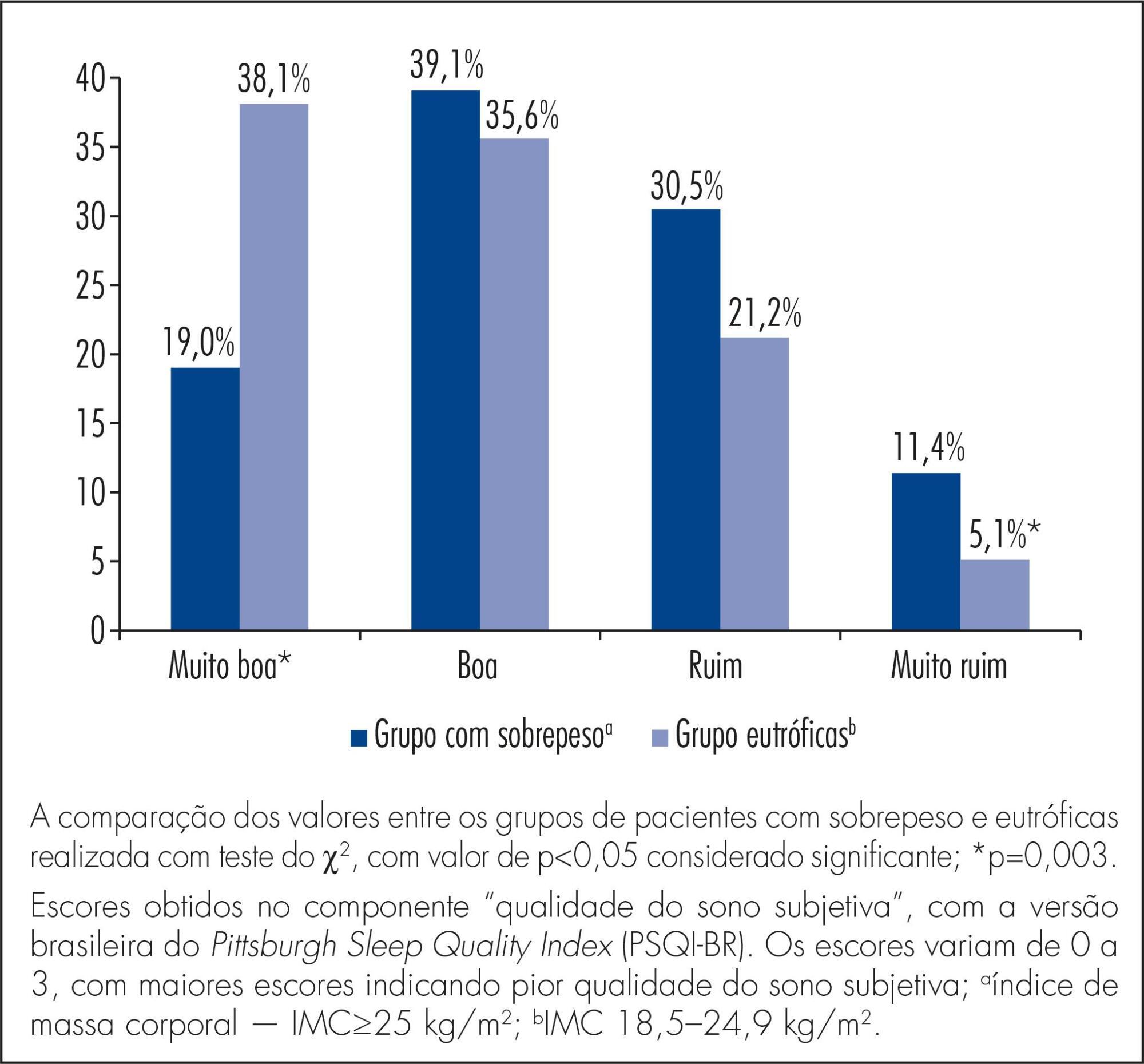
To compare sleep quality of overweight versus normal weight women in the second and third trimesters of pregnancy.
A cross-sectional study involving 223 women with 14 or more weeks of pregnancy, 105 of them overweight (pre-pregnancy body mass index - BMI - ≥25.0 kg/m2) and 118 of normal weight (BMI 18.5-24.9 kg/m2), attending the prenatal care clinic. The Brazilian version of the Pittsburgh Sleep Quality Index (PSQI-BR) questionnaire was used to evaluate sleep quality. The Student t-test and the chi-square test were used to compare differences between groups and a p value <0.05 was considered statistically significant.
Most of the participants (67.7%) were poor sleepers (total score >5); this proportion was significantly higher among overweight (80/105) versus normal weight (67/118) women (76.2 versus 56.8%, p=0,004). During the second trimester, this difference did not reach statistical significance (72.5 versus 53.7%, respectively, p=0.06) but mean total PSQI-BR scores were significantly higher among overweight participants (7.0±3.8 versus 5.5±3.2, p=0.02). In the 2nd trimester, overweight women also had higher scores for sleep latency (1.4±1.0 versus 1.0±0.9, p=0.02) and subjective sleep quality (1.3±0.8 versus 0.8±0.8, p=0.02). In the third trimester, the proportion of women with poor sleep quality was significantly higher in the overweight group, but did not reach statistical significance (79.6 versus 60.8%, p=0.06). During this period, total mean scores were similar for women with and without excess weight (9.4±4.2 versus 8.3±4.6, p=0.2). However, overweight women had higher mean scores for sleep disturbance (2.3±0.7 versus 2.0±0.8, p=0.04).
Overweight women had a poorer sleep quality than normal weight women in the second and third trimesters of pregnancy.