Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(7):352-357
DOI 10.1590/S0100-72032007000700005
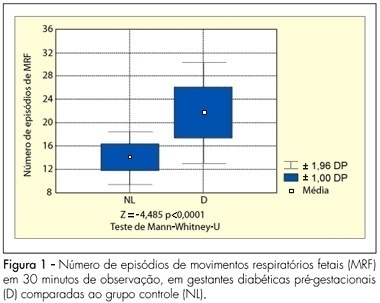
PURPOSE: to analyze the pattern of fetal breathing movements (FBM) in diabetic pregnant women in the third trimester of pregnancy. METHODS: sixteen pregestational diabetic and 16 nondiabetic (control group) pregnant subjects were included fulfilling the following criteria: singleton, between 36-40 weeks of gestation, absence of other maternal diseases and absence of fetal anomalies. The fetal biophysical profile (FBP) was performed to evaluate the following parameters: fetal heart rate, FBM, fetal body movements, fetal tone and amniotic fluid index. The FBM was evaluated for 30 minutes, period when the examination was integrally recorded in VHS video for posterior analysis of the number of FBM episodes, the duration of each episode and the fetal breathing movements index (BMI). The BMI was calculated by the formula: (interval of time with FBM/total time of observation) x 100. At the beginning and in the end of the FBP maternal glucose levels were checked. The results were analyzed by the Mann-Whitney U-test and the Fisher exact test, adopting a level of significance of 5%. RESULTS: the glucose levels demonstrated significantly superior average in the diabetic group (113.3±35.3 g/dL) in relation to the normal group (78.2±14.8 g/dL, p<0.001). The average of the amniotic fluid index was higher in the group of the diabetic cases (15.5±6.4 cm) when compared with controls (10.6±2.0 cm; p=0.01). The average of the number of FBM episodes was superior in the diabetic ones (22.6±4.4) in relation to controls (14.8±2.3; p<0.0001). The average of the BMI in the diabetic patients (54.6±14.8%) was significantly higher than that in the control group (30.5±7.4%, p<0.0001). CONCLUSIONS: the elevated blood glucose levels can be associated with a different pattern in the FBM of diabetic mothers. The use of this parameter of the FBP, in the obstetric practice, must be considered with concern in diabetic pregnancies.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(4):352-359
To assess homocysteine (Hcy) levels in the three trimesters of pregnancy in women with fetal growth restriction (FGR) and to evaluate the role of Hcy as a possible predictor of FGR.
A total of 315 singleton pregnant women were included in the present prospective cohort study and were monitored since the 1st trimester of pregnancy before delivery. Newborns were monitored for the first 7 days of life. Patients who had risk factors for FGR were excluded. Fetal growth restriction was defined according to uterine fundal height (< 10 percentile), ultrasound fetometry (< 5 percentile), and anthropometry of newborns (<5 percentile). The concentrations of Hcy were detected at between 10 and 14, between 20 and 24, and between 30 and 34 weeks of pregnancy by enzyme-linked immunosorbent assay (ELISA). Receiver operating characteristics (ROC) curve test and diagnostic odds ratio (DOR) were performed to evaluate the results of ELISA.
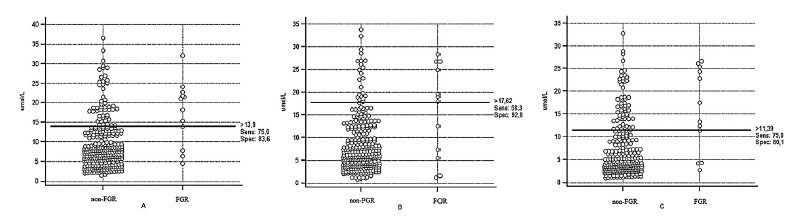
The concentration of Hcy in patients with FGR was 19.65 umol/L at between 10 and 14 weeks, compared with 9.28 umol/L in patients with normal fetal growth (p<0.0001). The optimal cut-off level for Hcy in the 1st trimester of pregnancy was>13.9 umol/L with AUC 0.788, sensitivity of 75%, specificity of 83.6%, and DOR of 15.2.
Assessment of serum Hcy concentration may be used as a predictor of FGR, with the highest diagnostic utility in the 1st trimester of pregnancy.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):353-356
DOI 10.1590/S0100-72032005000600010
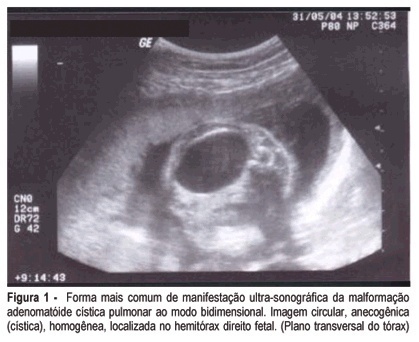
Fetal cystic adenomatoid malformation is a pulmonary developmental anomaly arising from an overgrowth of the terminal respiratory bronchioles. This is such a rare malformation, that is not always thought of as a diagnostic possibility. We present a case of pulmonary cystic adenomatoid malformation and emphasize the importance of early diagnosis and therapeutic possibilities. We also present its evolution after prenatal placement of a catheter for continuous drainage.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(5):353-358
DOI 10.1590/S0100-72032003000500008
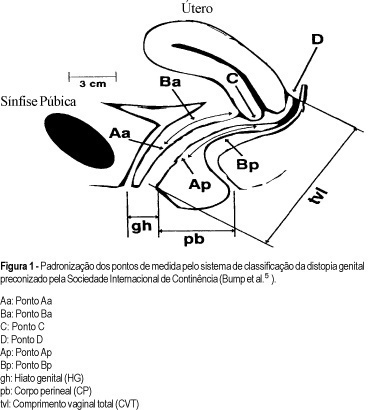
PURPOSE: to determine interobserver reliability of site-specific measurements and stages according to the proposed International Continence Society prolapse terminology document. METHODS: we analyzed 51 women during urogynecological investigation performed at the Urogynecology and Vaginal Surgery Sector of UNIFESP / EPM. We recorded the locations of point-specific measures proposed by the International Continence Society (ICS). They are: two in the anterior vaginal wall, two in the superior vagina, two in the posterior vaginal wall, genital hiatus, perineal body and total vaginal length. Then we recorded the stage of genital prolapse. Women underwent pelvic examinations by two investigators, each blinded to the results of the other's examination. The reproducibility of the nine site-specific measurements and the summary stage were analyzed using Pearson's correlation coefficient and the median measurements were compared by the paired-t test. RESULTS: there were substantial and highly significant correlations for each of the nine measurements. Correlation coefficient for point Aa was 0.89 (p<0.0001), point Ba 0.90 (p<0.0001), point C 0.97 (p<0.0001), point Ap de 0.72 (p<0.0001), point Bp 0.84 (p<0.0001), point D 0.91 (p<0.0001), genital hiatus 0.65 (p<0.0001), perineal body 0.66 (p<0.0001) e total vaginal length 0.73 (p<0.0001). We also did not note differences between the means of measurements by the two examiners. Staging was highly reproducible (r=0.81, p<0.0001). ln no subject did the stage vary by more than one; in 86,2%, stages were identical. CONCLUSIONS: there is a good reproducibility of measures using the system proposed by the International Continence Society prolapse terminology document.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(8):353-358
DOI 10.1590/SO100-720320150005338
To investigate the association between genetic, behavioral, biological and medical risk factors and the occurrence of preterm birth.
A retrospective case-control study was conducted. The real-time polymerase chain reaction was used to analyze the influence of the rs12473815 polymorphism of the follicle stimulating hormone receptor gene (FSHR) and the rs1942836 polymorphism of the progesterone receptor gene (PGR). Other proposed risk factors were assessed using validated or specifically developed questionnaires and analysis of electronically recorded medical data. A total of 157 patients were included (45 cases who went into labor before 37 weeks of pregnancy and 112 controls who went into labor after 37 and before 42 weeks of pregnancy).
The genotypes CT of rs12473815 and CT and CC of rs1942836 were associated with a higher chance of premature delivery. There was an association between preterm birth and alcohol intake when consumption occurred 2 or more times per month. Low pre-pregnancy body mass index was a predictor of spontaneous preterm birth, while high body mass index reduced this likelihood.
The results suggest that excessive alcohol intake, a low level of pre-pregnancy body mass and the risk alleles of rs12473815 and rs1942836 polymorphisms of the FSHR and PGR genes, respectively, influence the occurrence of preterm birth.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(6):353-363
DOI 10.1590/S0100-72032000000600006
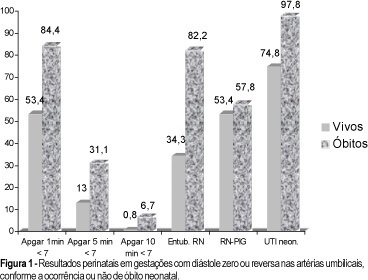
Purpose: to study the prognostic parameters for perinatal death in pregnancies with absent or reversed end-diastolic flow velocity on umbilical artery dopplervelocimetry. Methods: two hundred and four pregnancies were retrospectively reviewed. The methods used were cardiotocography, fetal biophysical profile, amniotic fluid index and dopplervelocimetry of ductus venosus, fetal aorta, middle cerebral artery, umbilical arteries and uterine artery. The logistic regression model was applied to one hundred and seventy cases in order to determine the most accurate variable for predicting perinatal death. Results: the mortality rates were: 28 cases of intrauterine fetal death (13.7%) and 45 neonatal deaths (22.1%). A statistically significant correlation was found between death and the studied variables. The perinatal death rate in the group with birth weight below 1,000 g was 74.7%, and in the group with gestational age at delivery below 31 weeks it was 66.3%. By logistic regression, birth weight was the most accurate variable for predicting perinatal death, and a probability curve for death according to this variable was obtained. Conclusions: absent or reversed end-diastolic flow velocity in the umbilical arteries is a severe fetal condition, where the risk of perinatal death is mainly related to birth weight and a gestational age at delivery below 31 weeks.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(6):353-357
DOI 10.1590/S0100-72031999000600009
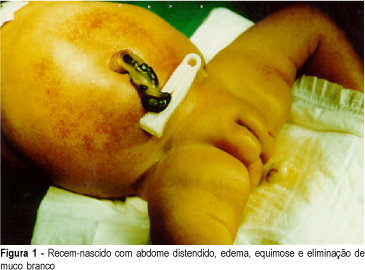
Introduction: meconium peritonitis as result of fetal intestinal perforation has a low incidence (1:30,000 deliveries) and high mortality (50% or more). Prenatal ultrasound findings include fetal ascites and intra-abdominal calcifications. Evidence suggests that prenatal diagnosis can improve postnatal prognosis. Case Report: R.C.M.S., 22 years, II pregnancy O para, presented ultrasound (12/02/98) with diagnosis of fetal ascites. Investigation for hydrops fetalis was performed and immune and nonimmune causes were excluded. Severe fetal ascites persisted on subsequent ultrasound examinations, without calcifications. Vaginal delivery occurred at 36 weeks (01/02/99), with polyhydramnios. Female neonate weighing 2,670 g, with signs of respiratory distress, abdominal distension and petechiae. Abdominal distension worsened progressively, with palpation of a petrous tumor in the right upper quadrant and elimination of white mucus at rectal examination. Radiological findings (01/04/99) were disseminated abdominal calcifications, intestinal dilatation and absence of gas at rectal ampulla. Exploratory laparotomy was indicated with diagnosis of meconium peritonitis. A giant meconium cyst and ileal atresia were observed and lysis of adhesions and ileostomy were performed. Initial postoperative evolution was satisfactory but was subsequently complicated by sepsis and neonatal death occurred (01/09/99). Conclusion: meconium peritonitis should be remembered at differential diagnosis of fetal ascites. In the present case, surgical indication could be anticipated if prenatal diagnosis were established, with improvement of neonatal evolution.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2009;31(7):353-360
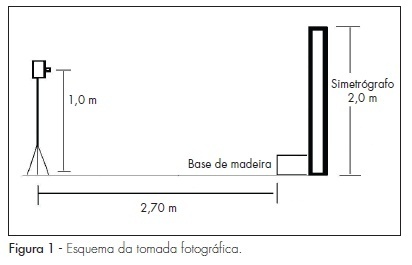
DOI 10.1590/S0100-72032009000700006
OBJECTIVE: to evaluate by photogrammetry, postural changes in women with chronic pelvic pain. METHODS: thirty women with complaint of chronic pelvic pain and 37 without it, in a total of 67 women, were evaluated. The evaluation was realized through anamnesis, fixed markers in defined anatomical sites, and frontal, posterior, left and right lateral photographies. Photo analysis has been done by the software CorelDraw®, version 11.0. Quantitative values for postural analysis of the ankle, the knee in the saggittal plan, pelvis, lumbar lordosis, thoracic kyphosis, adducted/abducted scapula, shoulders, head and third finger on the floor test were obtained. The qualitative variables studied were the knee (varus, valgus or normal), the presence or not of winged scapula and leveling of shoulders. The Statistical Package for Social Sciences, version 16.0 was used for the statistical analyses. Fisher's exact test and Monte-Carlo method were used to compare the qualitative variables, and for the quantitative data, t or Mann-Whitney test was used. The comparisons among continuous data, corrected for possible confusion variables were realized by the univariate covariance analysis. Significance level was established at 0.05 or 5%. RESULTS: there were significant differences between cases and controls for protruded head (47.5 and 52.0º, respectively; p<0.0001) and for protruded shoulders (1.9 and 1.6 cm, respectively; p=0.03). The other variables did not show significant differences. CONCLUSIONS: based on these results, attention to head and shoulder posture, to antalgic postures and to the emotional factor is recommended. Women with chronic pelvic pain should be treated, taking into consideration individual muscle-skeletal changes, and social and emotional conditions.