Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(5):337-343
DOI 10.1590/S0100-72032003000500006
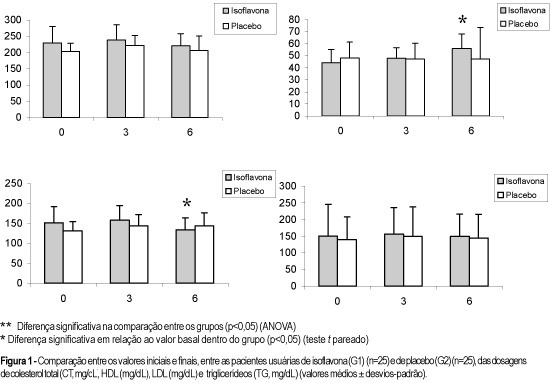
PURPOSE: to evaluate the effects of soy germ isoflavone on menopausal symptoms and blood lipids in postmenopausal women. METHODS: a prospective study was performed on 50 women, randomly divided into two groups: 25 women on soy germ isoflavones (60 mg/day, capsules) (G1) and 25 women on placebo (G2). Inclusion criteria: women with hot flushes and FSH >40 mIU/mL, non-vegetarian, non-smoker, non-Asiatic, not in use of hormone replacement therapy and without disease of the gastrointestinal tract. For six months, the menopausal Kupperman index (MKI) and hormonal and lipid profiles were assessed. For statistical analysis, ANOVA, t test and the non-parametric Kruskal-Wallis and Mann-Whitney tests were used. RESULTS: the median MKI values, initially similar in both groups, decreased in G1 at two and four months (MKI = 14 and 9, respectively), and in G2 at two months (MKI = 15) (p<0.01). At six months, isoflavone was significantly superior to placebo in reducing hot flushes (44 versus 12%, respectively). At the end of the study, in the isoflavone group, an increase in estradiol levels (from 16,8±7.3 to 18,0±6.7 ng/dL) (p<0.05) was observed, with no alteration in FSH, LH and vaginal cytology; there was also a reduction of 11.8% in LDL (from 151.5±39.2 for 133,6±26.4 mg/dL) and a HDL increase of 27.3% (from 44.0±11.3 to 56.0±11.9 mg/dL) (p<0.05). CONCLUSIONS: soy germ isoflavone induced favorable effects on menopausal symptoms and lipid profile, showing to be an interesting option for alternative therapy in postmenopausal women.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(5):337-341
DOI 10.1590/S0100-72032002000500008
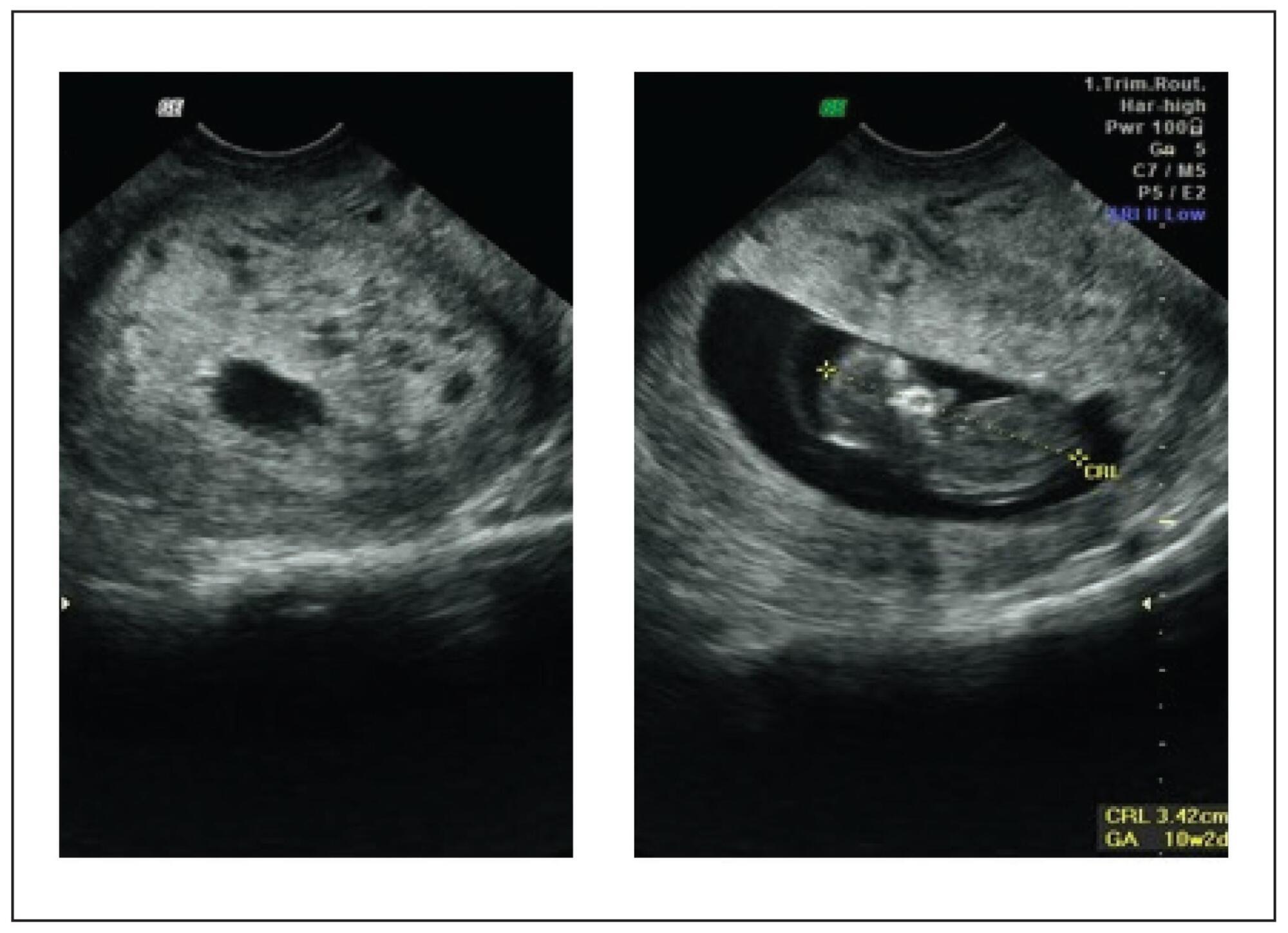
Purpose: to evaluate pregnancy outcome after laparoscopic tubal anastomosis. Method: from December 1998 to December 2001, 26 patients with bilateral tubal ligation who underwent laparoscopic tubal anastomosis were prospectively evaluated. Patients' age ranged from 28 to 37 years. The follow-up period ranged from 150 to 425 days and tubal patency (evaluated by hysterosalpingography) and pregnancy outcome were evaluated. Results: laparoscopic tubal reversal was performed in 23 patients. Bilateral reversal was attempted in all except two patients. The operation time ranged from 95 to 155 minutes and all patients were discharged on the following morning. Tubal patency was confirmed in 15 patients (15/23). Pregnancy rate was 56.5% (13/23), without ectopic pregnancies. Nine patients got pregnant in up to four months and four in up to nine months after discontinuing the use of condom. Conclusion: in selected cases, laparoscopic tubal reversal can be performed in patients who had been submitted to tubal sterilization and desire new pregnancies. Patient selection as well as meticulous surgical technique are key factors in achieving satisfactory pregnancy rates.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(6):338-346
To discuss the implementation and contributions of the External Quality Monitoring in the city of Rio de Janeiro and to analyze the performance of the main providers of cervical cytopathology in this city from September 2013 to March 2017, here referred to as “Alpha laboratory” and “Beta laboratory.”
Observational, cross-sectional, retrospective study using information from the Cervical Cancer Control Information System (SISCOLO, in the Portuguese acronym), municipal coordinationmodule, External QualityMonitoring report. The proportions of false positives, false negatives, unsatisfactory samples and rejected samples were estimated. The agreement among the observers was analyzed through the Kappa index and the reduction of disagreements in the period for each laboratory studied, comparing the results of each cycle.
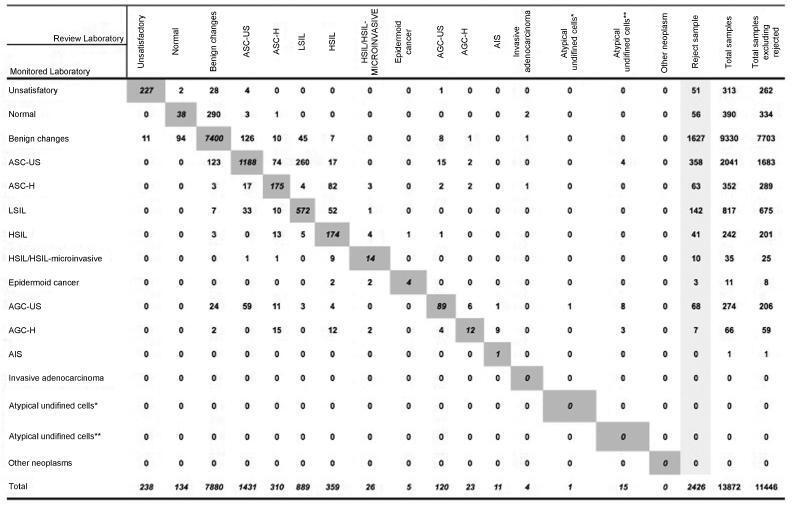
A total of 19,158 examinations were selected, of which 19,130 (99.85%) were monitored, 16.649 (87, 03%) were reviewed by the External Quality Monitoring Unit, 2,481 (12,97%) were rejected and 441 (2,65%) were considered unsatisfactory. The “Beta laboratory” presented excellent concordance in all cycles; the “Alpha laboratory” had good concordance in the first two cycles (K = 0.76 and 0.79), becoming excellent in the following four cycles. The average Kappa index was 0.85, with median of 0.86. The percentage of diagnostic disagreement was 6.63% of the reviewed exams, of which 5.38% required a change of conduct
External Quality Monitoring is an exercise in diagnostic improvement, and its implementation was fundamental to ensure the reliability of the cytopathological exams in the city of Rio de Janeiro.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(4):339-340
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(6):339-345
DOI 10.1590/S0100-72032000000600004
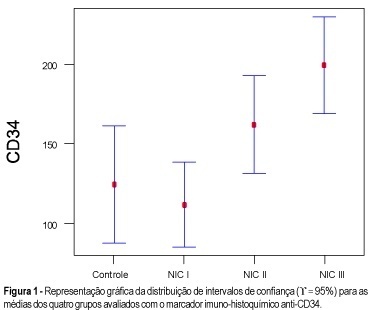
Purpose: to quantify the vessels and epithelial proliferation, applying immunohistochemical staining with anti-CD34 as well as anti-PCNA markers, in intra-epithelial neoplasia of the uterine cervix. Methods: in the present study, 16 patients with CIN III, 16 with CIN II, 21 with CIN I and 11 with normal cervix (control group) were investigated. Slide analysis was performed at the same time by two observers, in 10 consecutive sites using 100X and 400X magnification, both in the highest vascularization (CD34) and proliferative activity sites (PCNA). Results: the means obtained with the use of anti-PCNA in intraepithelial neoplasias were: 78.2% (CIN III), 52.1% (CIN II), 33.3% (CIN I) and 4.6% (control group), while 199.1 vessels (CIN III), 162.0 vessels (CIN II), 111.7 vessels (CIN I) and 124.4 vessels (control group) were quantified using anti-CD34 as a vascular marker. Conclusion: the results showed that both markers, anti-PCNA and anti-CD34, are useful for investigating proliferative and angiogenic activity, respectively. However, anti-PCNA showed better and more accurate results than anti-CD34 in differentiating intraepithelial neoplasias.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(7):339-343
DOI 10.1590/S0100-720320150005318
We report here a case of gestational trophoblastic neoplasia after spontaneous normalization of human chorionic gonadotropin in a patient with a partial hydatidiform mole. This is the second occurrence of this event to be reported and the first one with proven immunohistochemical evidence. Besides showing the treatment for this pregnancy complication, this case report discusses the possibility of reducing the duration of post-molar follow-up, as well as strategies for early recognition of gestational trophoblastic neoplasia after spontaneous remission of molar pregnancy.