Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(6):272-277
DOI 10.1590/SO100-720320150005301
To evaluate the ovarian response after cyclophosphamide use (CPM) in patients
with systemic lupus erythematosus (SLE) and to correlate the age and cumulative
dose findings with changes in menstrual cycle and/or progression to ovarian
failure (OF).
This was a cross-sectional, retrospective study of 50 patients with a diagnosis
of SLE who used CFM with a clinical follow-up of at least 1 year. Included were
patients aged 12-40 years, who had undergone chemotherapy for SLE control and who
had regular menstrual cycles before the beginning of CPM treatment. Patients who
discontinued follow-up, who were followed up for less than one year or who had
irregular/absent menses before the beginning of CPM treatment were excluded. All
women studied were submitted to an interview and a questionnaire containing
questions about the pattern of the menstrual cycle before and after therapy, and
about the gestational periods and contraception. We asked if the patients had been
instructed about the side effects and consequences of CFM. Statistical analysis
was performed using the Student t-test and the Mann Whitney, χ2 and
nonparametric Kolmogorov-Smirnov tests.
The mean age of the patients included in the study was 30.8 years and the mean
age at the time of use of CPM was 25.3 years. After CFM, 24% of patients stopped
menstruating, 28% returned to regular cycles and 48% continued to have irregular
cycles. It was found that the patients who developed OF had longer disease
duration (12.3 years) than those who did not develop it (8.9 years). Thirteen
patients became spontaneously pregnant after CFM; however, 66% progressed to
abortion. The mean age of the patients who used CFM and developed OF was 28.1
years. Amenorrhea occurred in 50% of those aged 31-40 years, in 22.2% of those
aged 21-30 years and in 7.7% of those aged 12-20 years. Our study showed no
statistical correlation between cumulative dose and OF, although cumulative doses
greater than 11grams tended to promote some type of menstrual irregularity.
SLE disease duration, age at the time of treatment and the highest cumulative
doses are important predictors of OF after therapy with CFM. Pregnancy in lupus
patients is more likely to evolve with abortion after the use of chemotherapy. It
was seen that a small proportion of patients were aware of all the implications of
the drug. Therefore, additional studies should be conducted for further knowledge
and awareness of the importance of contraception and the preservation of ovarian
tissue on the part of the medical community.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(3):272-279
To evaluate whether colposcopy-directed biopsy is necessary to increase the accuracy of diagnosing cervical intraepithelial lesions in relation to colposcopy.
We performed a retrospective, observational study by analyzing medical records obtained fromHospital de Clínicas do Paraná fromFebruary 2008 to February 2018. Patients with results of Pap tests, colposcopy, colposcopy-directed biopsy, and surgical procedures (high-frequency surgery or cold conization) were included. Data such as quadrants involved during colposcopy and age differences were also analyzed.
A total of 299 women were included. Colposcopy was found to have an accuracy rate of 76.25% (95% confidence interval [CI], 71.4-81.1). Among the highest-grade lesions, the accuracy rate was 80.5% (95% CI, 75.7-85.3). The accuracy rates for biopsy were 79.6% (95% CI, 75-84.2) and 84.6% (95% CI, 80-89.1) for the highest-grade lesions. High-grade lesions were accurately confirmed in 76.9% and 85% of patients with 1 and 2 or more affected quadrants, respectively. For women younger than 40 years, the accuracy rates were 77.6% and 80.8% for colposcopy and biopsy, respectively. For women 40 years or older, the accuracy rates were 72.5% and 76.3% for colposcopy and biopsy, respectively.
There is no difference between the accuracy of colposcopy and that of biopsy in diagnosing cervical intraepithelial lesions in relation with the result of conization. The patients who received the greatest benefit when biopsy was not performed were those with high-grade lesions at colposcopy, a lesion involving 2 or more quadrants, and those younger than 40 years.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(5):272-288
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(5):273-280
Pituitary apoplexy refers to a rare clinical syndrome consisting of signs and symptoms that occur due to rapid expansion of the contents of the sella turcica. It can occur spontaneously or associated with pituitary tumors. It can have a broad clinical spectrum, but usually presents with severe headache, visual impairment and hypopituitarism. Sudden onset of symptoms associated to imagiologic confirmation makes the diagnosis. Surgical treatment is advised when there is important compression of the optic tract. We present a case report and a review of the literature on pituitary apoplexy in pregnancy. The cases were reviewed to obtain information on maternal characteristics, clinical presentation, diagnostic studies, therapeutic modalities and maternal and fetal outcomes. Our review found 36 cases of pituitary apoplexy in pregnancy. Most of the cases occurred in the second trimester of pregnancy and headache was the most frequent symptom at presentation. Surgical therapy was required in more than half of the patients. In what respect maternal and fetal outcomes, there were 3 cases of preterm delivery and one case of maternal death. Our clinical case and literature review reinforces the importance of an early diagnosis to avoid potential adverse consequences.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(5):273-277
DOI 10.1590/S0100-72031999000500005
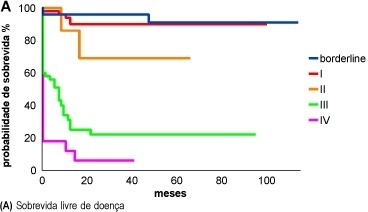
Purpose: to determine some epidemiological, diagnostic and prognostic aspects in women with borderline and invasive epithelial ovarian tumors. Methods: the charts of 198 women treated at CAISM/UNICAMP from 1986 to 1996 were revised. For statistical assessment, chi², Fisher's exact and t Student's tests were used when appropriate, followed by survival curves by the Kaplan-Meyer method, compared by the log-rank test. The mean follow-up was 50 months (11 to 168). Results: the overall rate of borderline tumors was 12% (24 cases), and for invasive carcinoma, 88% (174 cases). The mean age of the patients with borderline tumors was significantly lower than that of those with invasive carcinoma (43 ± 14.8 years vs. 52 ± 12.6 years, p<0.002). The most frequent histologic types were the serous (81 cases: 41%) and the mucinous (46 cases: 23%) tumor. The women with borderline tumors had their diseases diagnosed in earlier stages when compared with the invasive carcinoma patients (p<0.0001). The frozen biopsy, performed on 77 patients, showed a high agreement with the paraffin fixed tissue in the invasive carcinoma cases. However, in borderline tumors, the rate of failure was higher (13%) and the major rate of failure was in mucinous tumors. Regarding prognosis, the survival rate was significantly higher in borderline tumors (p<0.001). Conclusions: women with epithelial ovarian tumors were younger, presented the disease at earlier stages, and had a better prognosis when compared with those with invasive carcinoma.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(5):273-280
DOI 10.1590/S0100-72031998000500007
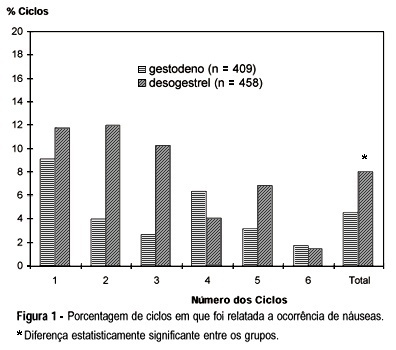
An open-label comparative study was conducted in nine centers in Brazil to evaluate the tolerability and cycle control of two low-dose oral contraceptives containing 20 mg ethynylestradiol/75 mg gestodene and 20 mg ethynylestradiol/150 mg desogestrel, during six treatment cycles. A total of 167 healthy sexually active women were enrolled (77 in the gestodene group and 90 in the desogestrel group) and 138 completed the six-cycle treatment period. A lipid and hemostatic profile was performed for a subgroup of first users. A total of 867 cycles were evaluated. Irregular bleeding did not occur in 95.4% of the cycles evaluated with gestodene and in 91.9% with desogestrel. Tolerability was good with both preparations but there was significantly more nausea in the desogestrel group. Cycle control was good with both preparations with a significantly lower incidence of irregular bleeding with gestodene when all cycles were considered. There were no clinically significant changes in the hemostatic profile. Lipid profile showed a trend to be more favorable after six cycles of treatment with both preparations. Women in the gestodene group did not present changes in the mean weight; in the desogestrel group there was a significant mean weight increase of 1 kg after six cycles of treatment. Compliance with treatment was good with both preparations. Results of this study demonstrated that low-dose preparations containing gestodene or desogestrel combined with 20 mg of ethynylestradiol are well-tolerated oral contraceptives that provide good cycle control.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(4):273-276

Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(6):273-281
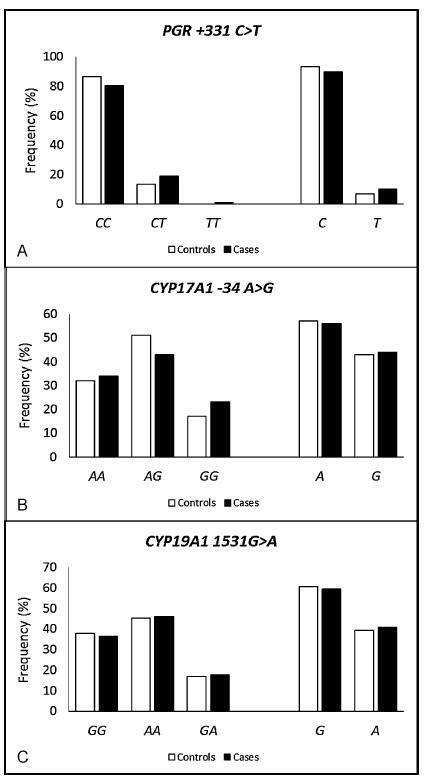
To evaluate the magnitude of the association of the polymorphisms of the genes PGR, CYP17A1 and CYP19A1 in the development of endometriosis.
This is a retrospective case-control study involving 161 women with endometriosis (cases) and 179 controls. The polymorphisms were genotyped by real-time polymerase chain reaction using the TaqMan system. The association of the polymorphisms with endometriosis was evaluated using the multivariate logistic regression.
The endometriosis patients were significantly younger than the controls (36.0±7.3 versus 38.0±8.5 respectively, p = 0.023), and they had a lower body mass index (26.3±4.8 versus 27.9±5.7 respectively, p = 0.006), higher average duration of the menstrual flow (7.4±4.9 versus 6.1±4.4 days respectively, p = 0.03), and lower average time intervals between menstrual periods (25.2±9.6 versus 27.5±11.1 days respectively, p = 0.05). A higher prevalence of symptoms of dysmenorrhea, dyspareunia, chronic pelvic pain, infertility and intestinal or urinary changes was observed in the case group when compared with the control group. The interval between the onset of symptoms and the definitive diagnosis of endometriosis was 5.2±6.9 years. When comparing both groups, significant differences were not observed in the allelic and genotypic frequencies of the polymorphisms PGR + 331C > T, CYP17A1 -34A > G and CYP19A1 1531G > A, even when considering the symptoms, classification and stage of the endometriosis. The combined genotype PGR + 331TT/CYP17A1 -34AA/CYP19A11531AA is positively associated with endometriosis (odds ratio [OR] = 1.72; 95% confidence interval [95%CI] = 1.09-2.72).
The combined analysis of the polymorphisms PGR-CYP17A1-CYP19A1 suggests a gene-gene interaction in the susceptibility to endometriosis. These results may contribute to the identification of biomarkers for the diagnosis and/or prognosis of the disease and of possible molecular targets for individualized treatments.