You searched for:"Rosiane Mattar"
We found (46) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo53
To evaluate the risk factors for postpartum hemorrhage (PPH) according to the Robson Classification in a low-risk maternity hospital.
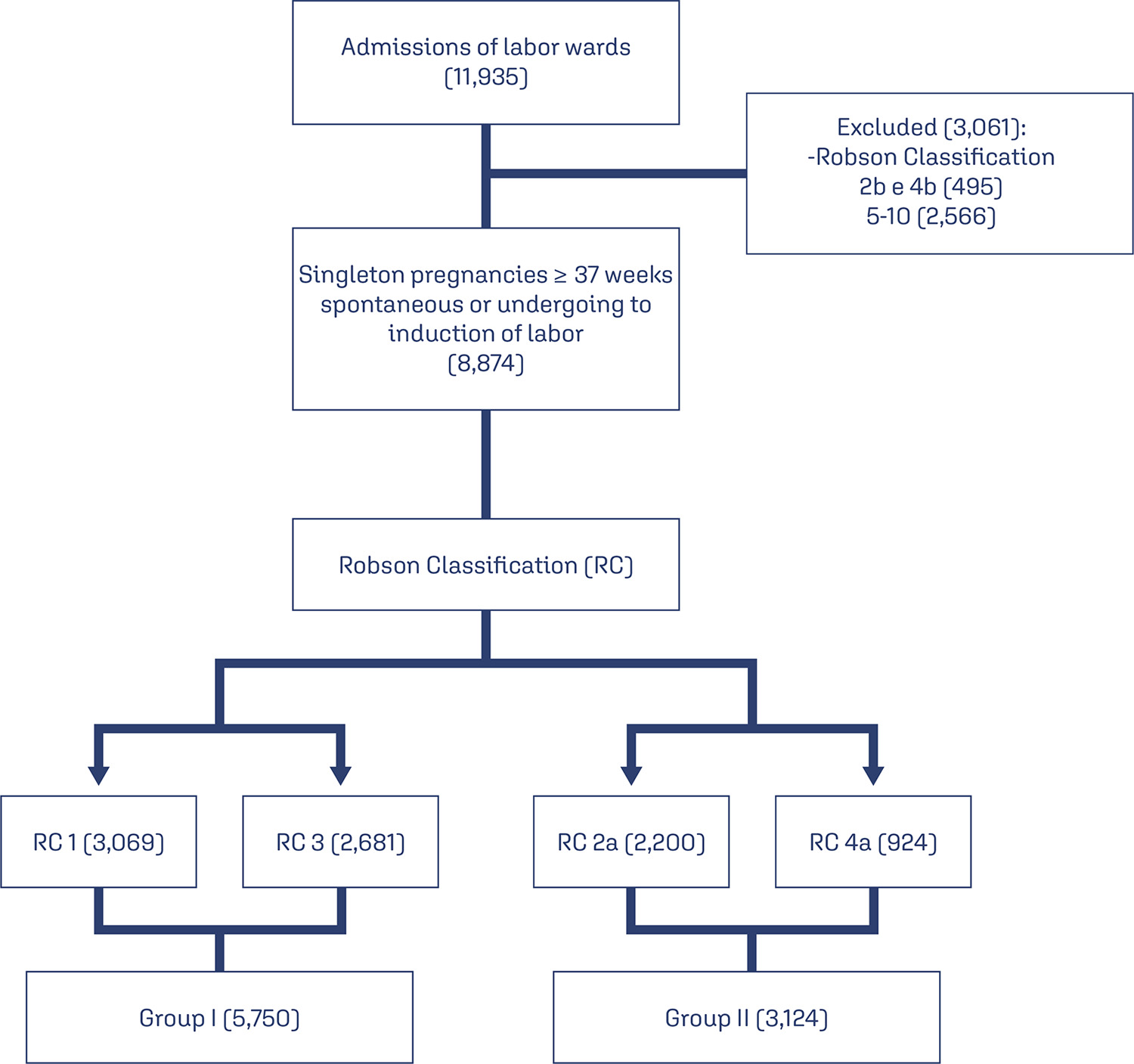
We conducted retrospective cohort study by analyzing the medical records of pregnant women attended in a low-risk maternity hospital, during from November 2019 to November 2021. Variables analyzed were: maternal age, type of delivery, birth weight, parity, Robson Classification, and causes of PPH. We compared the occurrence of PPH between pregnant women with spontaneous (Groups 1 and 3) and with induction of labor (2a and 4a). Chi-square and Student t-tests were performed. Variables were compared using binary logistic regression.
There were 11,935 deliveries during the study period. According to Robson’s Classification, 48.2% were classified as 1 and 3 (Group I: 5,750/11,935) and 26.1% as 2a and 4a (Group II: 3,124/11,935). Group II had higher prevalence of PPH than Group I (3.5 vs. 2.7%, p=0.028). Labor induction increased the occurrence of PPH by 18.8% (RR: 1.188, 95% CI: 1.02-1.36, p=0.030). Model including forceps delivery [x2(3)=10.6, OR: 7.26, 95%CI: 3.32-15.84, R2 Nagelkerke: 0.011, p<0.001] and birth weight [x2(4)=59.0, OR: 1.001, 95%CI:1.001-1.001, R2 Nagelkerke: 0.033, p<0.001] was the best for predicting PPH in patients classified as Robson 1, 3, 2a, and 4a. Birth weight was poor predictor of PPH (area under ROC curve: 0.612, p<0.001, 95%CI: 0.572-0.653).
Robson Classification 2a and 4a showed the highest rates of postpartum hemorrhage. The model including forceps delivery and birth weight was the best predictor for postpartum hemorrhage in Robson Classification 1, 3, 2a, and 4a.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo39i
This study aims to create a new screening for preterm birth < 34 weeks after gestation with a cervical length (CL) ≤ 30 mm, based on clinical, demographic, and sonographic characteristics.
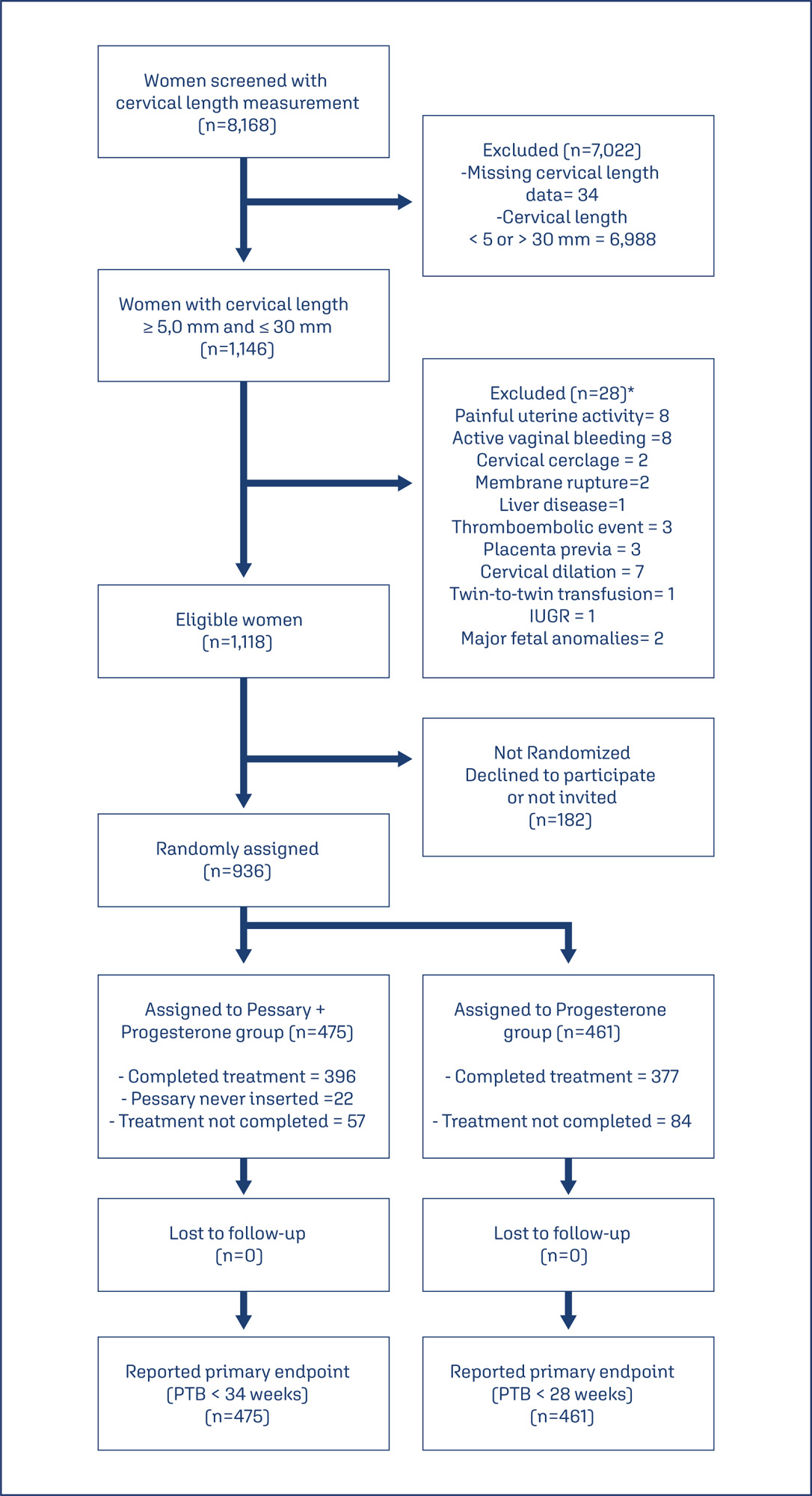
This is a post hoc analysis of a randomized clinical trial (RCT), which included pregnancies, in middle-gestation, screened with transvaginal ultrasound. After observing inclusion criteria, the patient was invited to compare pessary plus progesterone (PP) versus progesterone only (P) (1:1). The objective was to determine which variables were associated with severe preterm birth using logistic regression (LR). The area under the curve (AUC), sensitivity, specificity, and positive predictive value (PPV) and negative predictive value (NPV) were calculated for both groups after applying LR, with a false positive rate (FPR) set at 10%.
The RCT included 936 patients, 475 in PP and 461 in P. The LR selected: ethnics white, absence of previous curettage, previous preterm birth, singleton gestation, precocious identification of short cervix, CL < 14.7 mm, CL in curve > 21.0 mm. The AUC (CI95%), sensitivity, specificity, PPV, and PNV, with 10% of FPR, were respectively 0.978 (0.961-0.995), 83.4%, 98.1%, 83.4% and 98.1% for PP < 34 weeks; and 0.765 (0.665-0.864), 38.7%, 92.1%, 26.1% and 95.4%, for P < 28 weeks.
Logistic regression can be effective to screen preterm birth < 34 weeks in patients in the PP Group and all pregnancies with CL ≤ 30 mm.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(1):1-2
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(3):101-104
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(2):103-107
DOI 10.1590/S0100-72032003000200005
PURPOSE: to study the causes and associated factors of fetal death. METHODS: epidemiological descriptive study, composed of 190 cases of fetal loss amongst 11,825 pregnant women that gave birth at the two only hospitals (Casa de Saúde Divino Espírito Santo and Hospital Nossa Senhora Auxiliadora) of Caratinga City, in the State of Minas Gerais, Brazil, in the period from January 1, 1995 to April 30, 2000. The variables were the number of pregnancies, the timing of the pregnant women at the time of hospitalization, the occurrence of fetal death in relation to delivery and the cause of fetal death. Since there were no comparative groups, tables, percentages and arithmetical means were applied, following the guidelines of the Course of Statistics, of the "Universidade Federal de São Paulo". RESULTS: among the 189 pregnant women with fetal death, 77 were primigravidal and 76 had already been pregnant 2 to 5 times. The gestational age in 113 women was from 20 to 37 weeks. In relation to parturition, the fetal loss occurred during the antepartum period in 164 of 190 dead fetuses. The most frequently noticed death causes were: abruptio placentae in 35 cases, fetal anomaly in 12 cases, and hypertension syndrome in 8 cases. Nervertheless, there was no explanation for the etiology of 117 cases of fetal death. CONCLUSION: stillbirth has frequently been observed among the primigravidae (40.74%), in preterm period (59.79%), and in the antepartum period (86.31%). Among fetal death causes, the most frequent was a abruptio placentae (18.42%), and in 61.57% of the cases the fetal death could not be explained.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(2):104-108
Summary
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(12):1083-1089
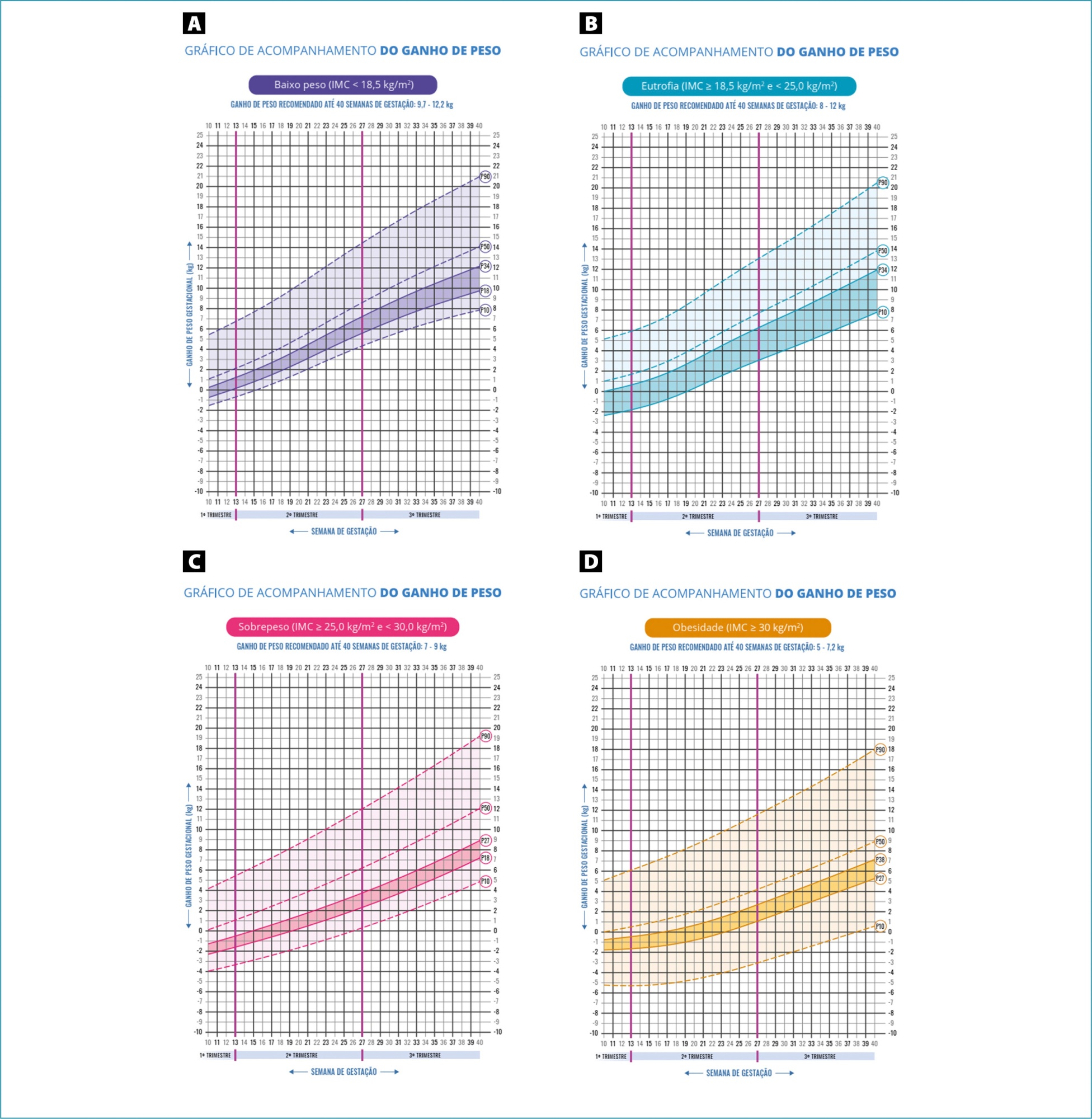
To compare the efficacy of quadratus lumborum (QL) block and intrathecal morphine (M) for postcesarean delivery analgesia.
Thirty-one pregnant women with ≥ 37 weeks of gestation submitted to elective cesarean section were included in the study. They were randomly allocated to either the QL group (12.5 mg 0.5% bupivacaine for spinal anesthesia and 0.3 ml/kg 0.2% bupivacaine for QL block) or the M group (12.5 mg bupivacaine 0.5% and 100 mcg of morphine in spinal anesthesia). The visual analog scale of pain, consumption of morphine and tramadol for pain relief in 48 hours, and side effects were recorded.
Median pain score and/or pain variation were higher in the morphine group than in the QL group (p = 0.02). There was no significant difference in the consumption of morphine or tramadol between groups over time. Side effects such as pruritus, nausea, and vomiting were observed only in the morphine group.
Quadratus lumborum block and intrathecal morphine are effective for analgesia after cesarean section. Patients undergoing QL block had lower postoperative pain scores without the undesirable side effects of opioids such as nausea, vomiting, and pruritus.