You searched for:"Daniela Angerame Yela"
We found (19) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):101-106
DOI 10.1590/S0100-72032000000200007
Purpose: to evaluate the prevalence of anticardiolipin antibody in women with stillbirth. Patients and Methods: this was a cross-sectional study performed from May 1998 to September 1999 at the Maternity of the University of Campinas and at the Hospital and Maternity Leonor Mendes de Barros, in Brazil, which evaluated 109 pregnant women hospitalized with the diagnosis of intrauterine fetal death and gestational age of 20 or more weeks. These women underwent some laboratory examinations to identify the cause of fetal death, including anticardiolipin antibody evaluation performed through the determination of IgG and IgM serum levels. IgG and IgM results are expressed as GPL and MPL units, respectively, and, in both cases, results above 10 units are considered positive. The statistical procedures used were the mean and standard deviation estimates, Student's t test, Fisher test and chi². Results: the prevalence of anticardiolipin positivity was 18.3%. The women were predominantly young, with a mean age around 27 years. The main identified causes of fetal death were: hypertension (26.1%), hemorrhage during the third trimester (9.9%) and fetal malformation (8.1%). One third of the cases had no identified causes of fetal death. However, considering the 20 positive cases for anticardiolipin antibody, the proportion of unidentified causes decreased to 29%. Conclusions: it is important to investigate the presence of anticardiolipin antibodies among women with intrauterine fetal death with the purpose of clarifying the causes of stillbirth. If the diagnosis of antiphospholipid syndrome is confirmed, it is necessary to counsel and treat these women regarding future pregnancies.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(11):1014-1020
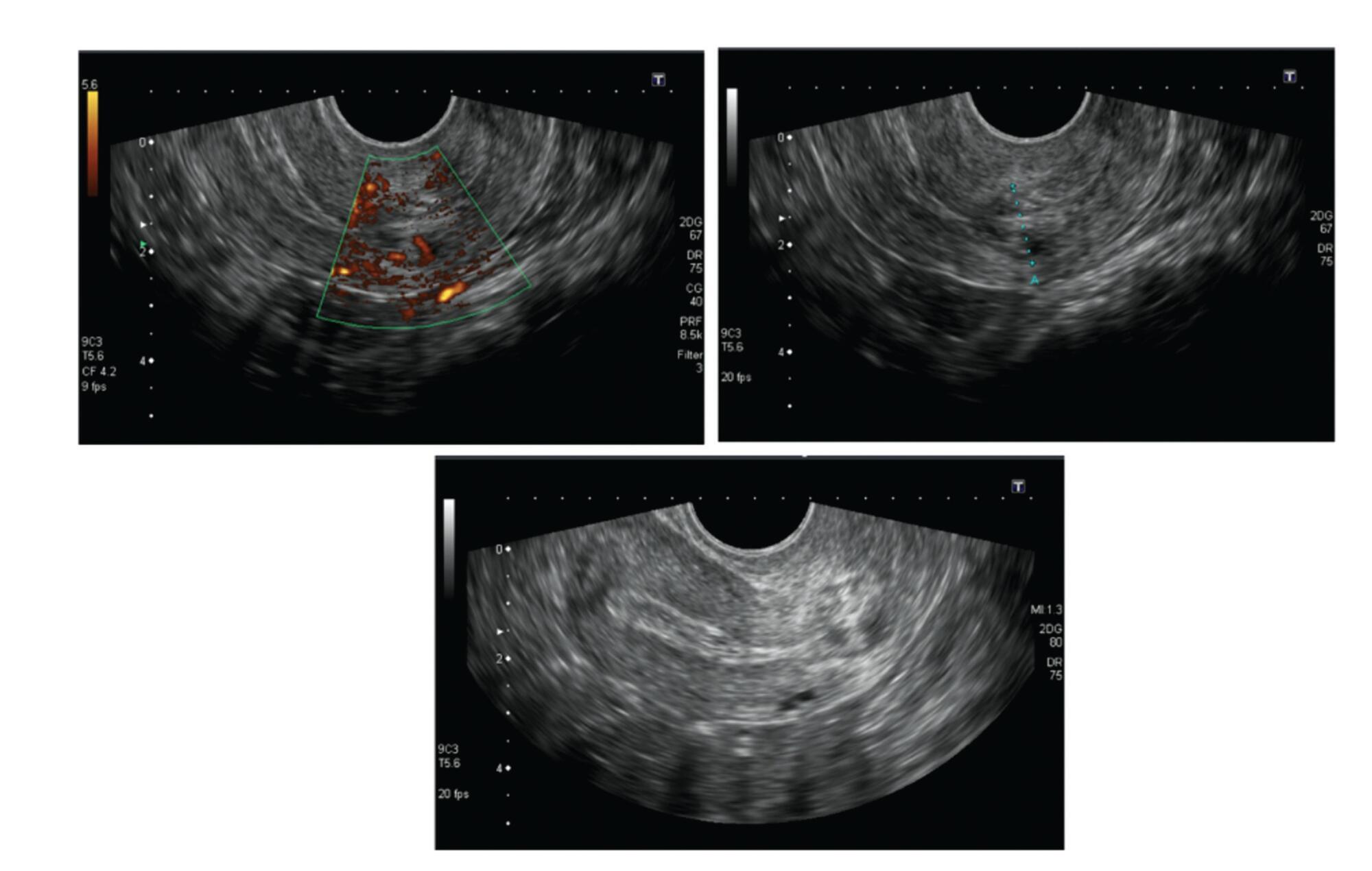
Cervical pregnancy is challenging for the medical community, as it is potentially fatal. The treatment can be medical or surgical; however, there are no protocols that establish the best option for each case. The objective of the present study was to describe the cases of cervical pregnancy admitted to a tertiary university hospital over a period of 18 years.
A retrospective study based on a review of the medical records of all cervical pregnancies admitted to the Women's Hospital at Universidade Estadual de Campinas, Southeastern Brazil, from 2000 to 2018.
We identified 13 cases of cervical pregnancy out of a total of 673 ectopic pregnancies; only 1 case was initially treated with surgery because of hemodynamic instability. Of the 12 cases treated conservatively, 7 were treated with single-dose intramuscular methotrexate, 1, with intravenous and intramuscular methotrexate, 1, with intravenous methotrexate, 1, with 2 doses of intramuscular methotrexate, and 2, with intra-amniotic methotrexate. Of these cases, one had a therapeutic failure that required a hysterectomy. Two women received blood transfusions. Four women required cervical tamponade with a Foley catheter balloon for hemostasis. There was no fatal outcome.
Cervical pregnancy is a rare and challenging condition from diagnosis to treatment. Conservative treatment was the primary method of therapy used, with satisfactory results. In cases of increased bleeding, cervical curettage was the initial treatment, and it was associated with the use of a cervical balloon for hemostasis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(2):137-144
The present study aims to evaluate the profile of endometrial carcinomas and uterine sarcomas attended in a Brazilian cancer center in the period from 2001 to 2016 and to analyze the impact of time elapsed fromsymptoms to diagnoses or treatment in cancer stage and survival.
This observational study with 1,190 cases evaluated the year of diagnosis, age-group, cancer stage and histological type. A subgroup of 185 women with endometrioid histology attended in the period from 2012 to 2017 was selected to assess information about initial symptoms, diagnosticmethods, overall survival, and to evaluate the influence of the time elapsed from symptoms to diagnosis and treatment on staging and survival. The statistics used were descriptive, trend test, and the Kaplan- Meier method, with p-values < 0.05 for significance.
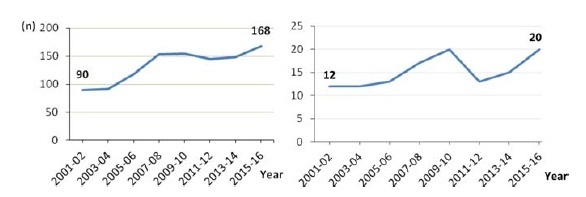
A total of 1,068 (89.7%) carcinomas (77.2% endometrioid and 22.8% nonendometrioid) and 122 (10.3%) sarcomas were analyzed, with an increasing trend in the period (p < 0.05). Histologies of non-endometrioid carcinomas, G3 endometrioid, and carcinosarcomas constituted 30% of the cases. Non-endometrioid carcinomas and sarcomas weremore frequently diagnosed in patients over 70 years of age and those on stage IV (p < 0.05). The endometrioid subgroup with 185 women reported 92% of abnormal uterine bleeding and 43% diagnosis after curettage. The average time elapsed between symptoms to diagnosis was 244 days, and between symptoms to treatment was 376 days, all without association with staging (p = 0.976) and survival (p = 0.160). Only 12% of the patients started treatment up to 60 days after diagnosis.
The number of uterine carcinoma and sarcoma cases increased over the period of 2001 to 2016. Aggressive histology comprised 30% of the patients and, for endometrioid carcinomas, the time elapsed between symptoms and diagnosis or treatment was long, although without association with staging or survival.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(3):183-190
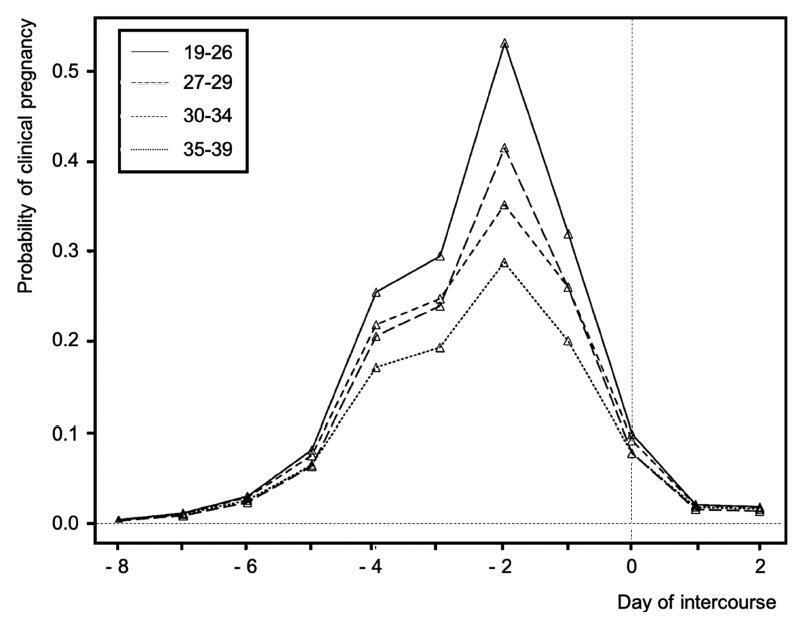
Considering that myths and misconceptions regarding natural procreation spread rapidly in the era of easy access to information and to social networks, adequate counseling about natural fertility and spontaneous conception should be encouraged in any kind of health assistance. Despite the fact that there is no strong-powered evidence about any of the aspects related to natural fertility, literature on how to increase the chances of a spontaneous pregnancy is available. In the present article, the Brazilian Federation of Gynecology and Obstetrics Associations (FEBRASGO, in the Portuguese acronym) Committee on Endocrine Gynecology provides suggestions to optimize counseling for non-infertile people attempting spontaneous conception.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(5):224-228
This study analyzed the effectiveness of the thyroid-stimulating hormone (TSH) as a predictor of insulin resistance (IR) and its association with the clinical and metabolic parameters of women with polycystic ovary syndrome (PCOS) without overt hypothyroidism.
A cross-sectional study was performed. Women with PCOS and without overt hypothyroidism (n = 168) were included.
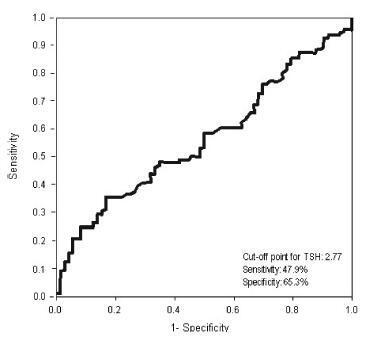
Receiver operating characteristic (ROC) curve was used to determine the cut-off point for TSH that would maximize sensitivity and specificity for a diagnosis of IR using homeostatic model assessment of insulin resistance (HOMA-IR)≥ 2.71. Clinical and metabolic parameters were compared as a function of the TSH cut-off limit and the presence of IR.
Thyroid-stimulating hormone ≥ 2.77 mIU/L was associated with a diagnosis of IR, with sensitivity of 47.9% and specificity of 65.3%. There were no differences in clinical, hormonal or metabolic parameters between TSH < 2.77 and TSH of 2.77 - 10 mIU/L.
In women with PCOS without overt hypothyroidism, TSH ≥2.77 mIU/L is associated with IR; however, with poor sensibility, showing TSH to be a poor predictor of IR in this population. No clinical or metabolic alterations were found that would justify a change in clinical management. Thus, the IR should be investigated in all women with PCOS irrespective of TSH level.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(5):275-280
Gender incongruence is defined as a condition in which an individual self-identifies and desires to have physical characteristics and social roles that connote the opposite biological sex. Gender dysphoria is when an individual displays the anxiety and/or depression disorders that result from the incongruity between the gender identity and the biological sex. The gender affirmation process must be performed by a multidisciplinary team. The main goal of the hormone treatment is to start the development of male physical characteristics by means of testosterone administration that may be offered to transgender men who are 18 years old or over. The use of testosterone is usually well tolerated and improves the quality of life. However, there is still lack of evidence regarding the effects and risks of the long-term use of this hormone. Many different pharmacological formulations have been used in the transsexualization process. The most commonly used formulation is the intramuscular testosterone esters in a short-term release injection, followed by testosterone cypionate or testosterone enanthate. In the majority of testosterone therapy protocols, the male physical characteristics can be seen in almost all users after 6 months of therapy, and themaximum virilization effects are usually achieved after 3 to 5 years of regular use of the hormone. To minimize risks, plasmatic testosterone levels should be kept within male physiological ranges (300 to 1,000 ng/dl) during hormonal treatment. It is recommended that transgender men under androgen therapy be monitored every 3 months during the 1st year of treatment and then, every 6 to 12 months.
Summary
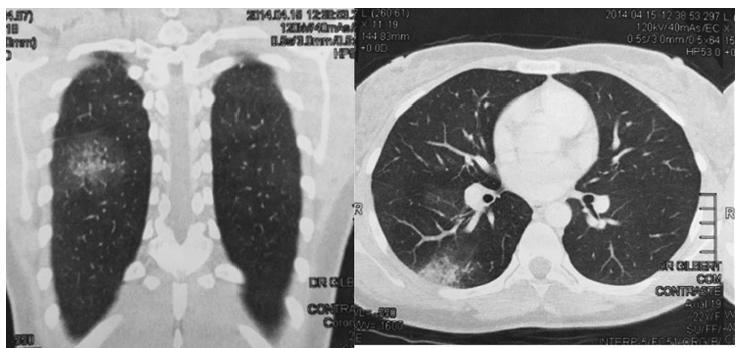
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(5):300-303
Thoracic endometriosis syndrome is a rare condition that includes four entities: catamenial pneumothorax, catamenial hemothorax, catamenial hemoptysis and lung nodules. We describe the case of a 23-year-old woman with complaints of hemoptysis during menstrual period in the two years prior to the appointment. Initially, a treatment for tuberculosis was established with no success. Further investigation showed a 4 mmnodule in the right lung, and the transvaginal ultrasonography indicated the presence of deep endometriosis. Considering the occurrence of symptoms only during menses, an empirical therapy was instituted with remission of the complaints.