You searched for:"Cristina Laguna Benetti-Pinto"
We found (23) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS07
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS05
Summary
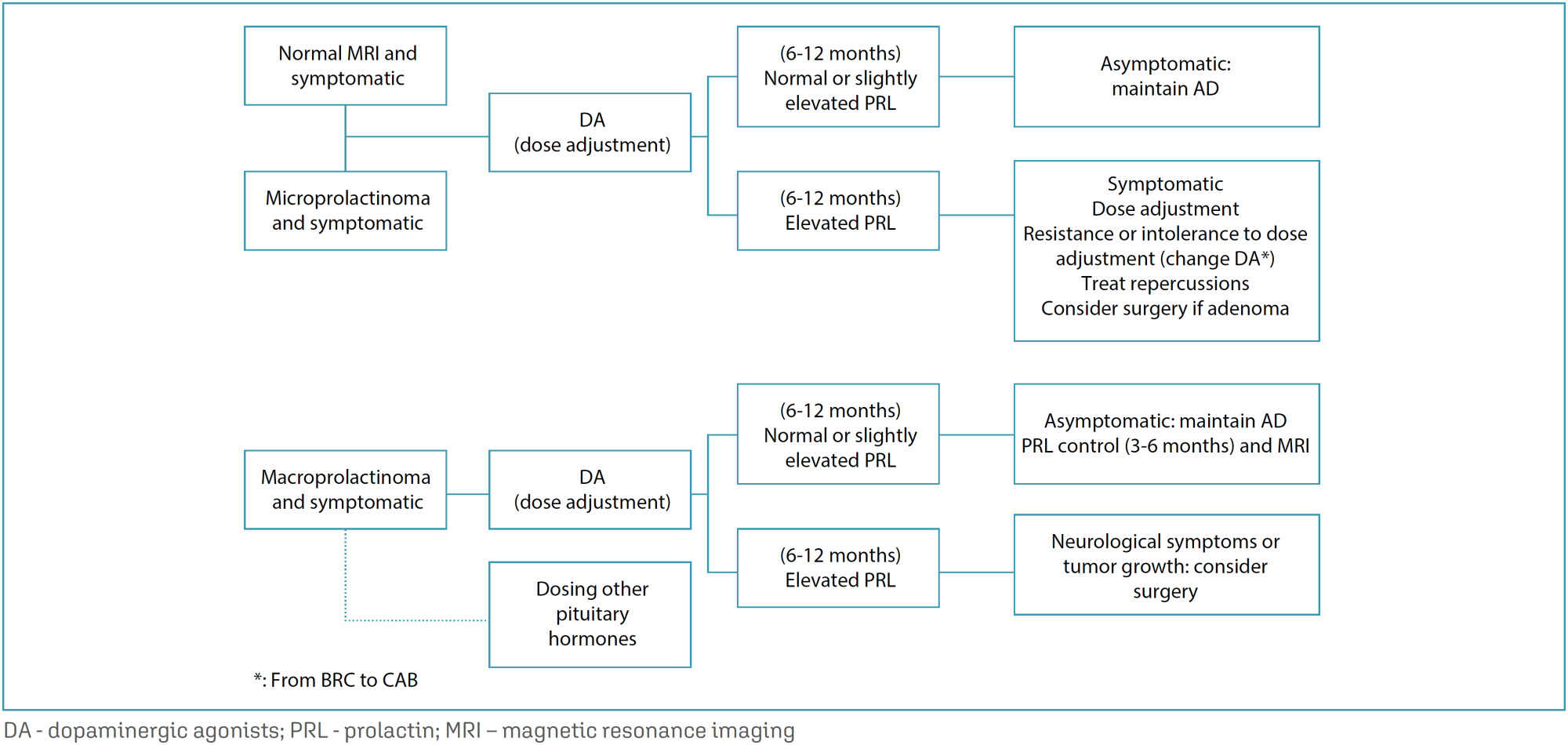
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS04
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(1):1-2
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(2):169-177
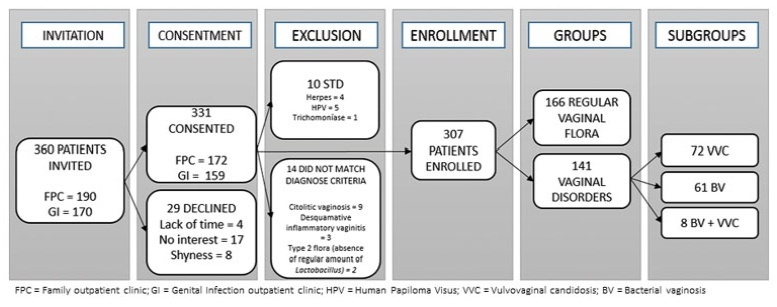
To evaluate genital hygiene among women with and without bacterial vaginosis (BV) and/or vulvovaginal candidiasis (VVC).
A cross-sectional study of reproductive-aged women who underwent gynecological and laboratory tests and fulfilled a genital hygiene questionnaire.
This study evaluated 166 healthy controls and 141 women diagnosed with either BV (n=72), VVC (n=61), or both (n=8). The use of intimate soap and moist wipes after urination was more frequent among healthy women (p=0.042 and 0.032, respectively). Compared to controls, bactericidal soap was more used by women with BV (p=0.05).
Some hygiene habits were associated to BV and/or VVC. Clinical trials should address this important issue in women’s health.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(3):183-190
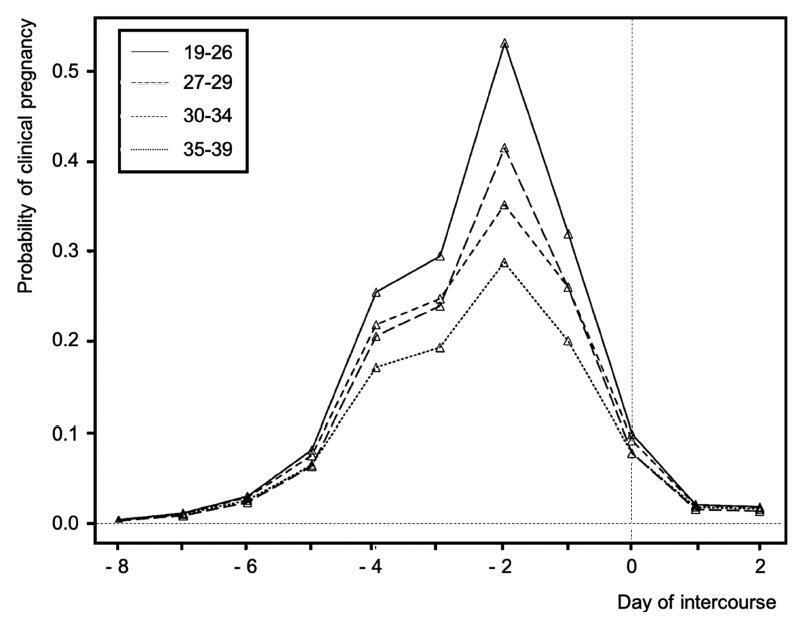
Considering that myths and misconceptions regarding natural procreation spread rapidly in the era of easy access to information and to social networks, adequate counseling about natural fertility and spontaneous conception should be encouraged in any kind of health assistance. Despite the fact that there is no strong-powered evidence about any of the aspects related to natural fertility, literature on how to increase the chances of a spontaneous pregnancy is available. In the present article, the Brazilian Federation of Gynecology and Obstetrics Associations (FEBRASGO, in the Portuguese acronym) Committee on Endocrine Gynecology provides suggestions to optimize counseling for non-infertile people attempting spontaneous conception.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(5):224-228
This study analyzed the effectiveness of the thyroid-stimulating hormone (TSH) as a predictor of insulin resistance (IR) and its association with the clinical and metabolic parameters of women with polycystic ovary syndrome (PCOS) without overt hypothyroidism.
A cross-sectional study was performed. Women with PCOS and without overt hypothyroidism (n = 168) were included.
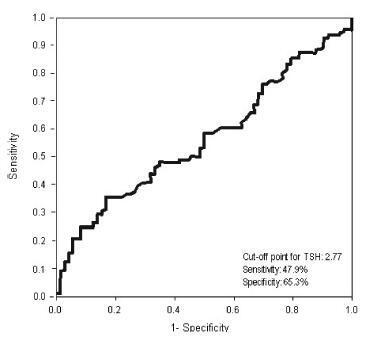
Receiver operating characteristic (ROC) curve was used to determine the cut-off point for TSH that would maximize sensitivity and specificity for a diagnosis of IR using homeostatic model assessment of insulin resistance (HOMA-IR)≥ 2.71. Clinical and metabolic parameters were compared as a function of the TSH cut-off limit and the presence of IR.
Thyroid-stimulating hormone ≥ 2.77 mIU/L was associated with a diagnosis of IR, with sensitivity of 47.9% and specificity of 65.3%. There were no differences in clinical, hormonal or metabolic parameters between TSH < 2.77 and TSH of 2.77 - 10 mIU/L.
In women with PCOS without overt hypothyroidism, TSH ≥2.77 mIU/L is associated with IR; however, with poor sensibility, showing TSH to be a poor predictor of IR in this population. No clinical or metabolic alterations were found that would justify a change in clinical management. Thus, the IR should be investigated in all women with PCOS irrespective of TSH level.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(5):275-280
Gender incongruence is defined as a condition in which an individual self-identifies and desires to have physical characteristics and social roles that connote the opposite biological sex. Gender dysphoria is when an individual displays the anxiety and/or depression disorders that result from the incongruity between the gender identity and the biological sex. The gender affirmation process must be performed by a multidisciplinary team. The main goal of the hormone treatment is to start the development of male physical characteristics by means of testosterone administration that may be offered to transgender men who are 18 years old or over. The use of testosterone is usually well tolerated and improves the quality of life. However, there is still lack of evidence regarding the effects and risks of the long-term use of this hormone. Many different pharmacological formulations have been used in the transsexualization process. The most commonly used formulation is the intramuscular testosterone esters in a short-term release injection, followed by testosterone cypionate or testosterone enanthate. In the majority of testosterone therapy protocols, the male physical characteristics can be seen in almost all users after 6 months of therapy, and themaximum virilization effects are usually achieved after 3 to 5 years of regular use of the hormone. To minimize risks, plasmatic testosterone levels should be kept within male physiological ranges (300 to 1,000 ng/dl) during hormonal treatment. It is recommended that transgender men under androgen therapy be monitored every 3 months during the 1st year of treatment and then, every 6 to 12 months.