You searched for:"Juliana Straehl"
We found (2) results for your search.Summary
Rev Bras Ginecol Obstet. 2012;34(6):274-277
DOI 10.1590/S0100-72032012000600006
PURPOSE: This study aimed to evaluate the results of neovaginoplasty by a modified McIndoe-Bannister technique and by the non-surgical Frank technique. METHODS: This retrospective study was conducted on a convenience sample of 25 women with vaginal agenesis undergoing surgical or conservative treatment at an Infant-Pubertal Gynecology Outpatient Clinic. Data were obtained from the medical records. Fifteen women underwent the surgical McIndoe-Bannister modified technique Surgical Group, and 10 women underwent the non-surgical Frank technique Frank Group. The following parameters were considered for comparative analysis between the two samples: vaginometry, surgical and non-surgical complications, and sexual satisfaction after treatment. Sexual satisfaction was assessed by a simple question: How is your sex life? RESULTS: There were differences related to vaginal length before and after performing exercises in both Frank Group (initial vaginal length 2.4±2.0 cm versus 6.9±1.1 cm after treatment, p<0.0001) and Surgical Group (initial vaginal length 0.9±1.4 cm versus 8.0±0.8 cm after treatment, p<0.0001). Increased vaginal length was observed in Surgical Group compared to Frank Group (Frank Group=7.0±0.9 cm versus Surgical Group=8.0±0.8 cm, p=0.0005). Forty percent of Surgical Group women had surgical complications versus no complications with the Frank technique. All women reported to be satisfied with their sexual life. CONCLUSION: The present data indicate that both the surgical and Frank techniques are effective for the treatment of vaginal agenesis, resulting in the construction of a vagina that pewrmits sexual intercourse and sexual satisfaction. The favorable aspects of the Frank technique are related to its low cost and to the low rates of major complications.
Summary
Rev Bras Ginecol Obstet. 2017;39(6):282-287
The views of infertile couples regarding oocyte donation by third parties and adoption are unknown, as these may be interpreted as a final closure of the available options for conception. This study aimed to determine the acceptance of oocyte donation, oocyte reception, and child adoption of infertile women who submitted to assisted reproductive technology (ART) treatment
Sixty-nine women who were under treatment for infertility and submitted to ART procedures were included in this cross-sectional study. They were evaluated using semi-structured questionnaires administered during ovulation induction in a treatment cycle. Marital status, religion, years of schooling, occupation, type of infertility, age, duration of infertility, number of previous ART cycles, mean oocyte number per cycle, and mean number of embryos per cycle had no influence on a woman’s acceptance of oocyte donation or oocyte reception.
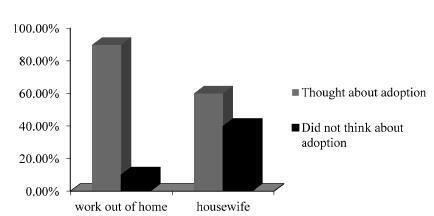
More than 90% of the patients thought that the subject of “adoption” should be brought up during their ART treatments, although they preferred to discuss this topic with psychologists, not doctors. Women with occupations were more willing to consider adoption.
The opinions of these patients on these issues seem to be based on personal concepts and ethical, religious, and moral values. Women preferred to discuss adoption with psychologists rather than doctors.