You searched for:"André Luis Ferreira Santos"
We found (7) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS12
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS10
•The negative impact of infectious diseases and their immunoprevention during the different stages of a woman’s life requires a broad approach including adolescence, adulthood, pregnancy and the postmenopausal phase.
•Immunization of pregnant women should be a priority for the protection of the maternal-fetal dyad, especially in regions with high rates of infections preventable by immunization.
•Brazil has one of the most comprehensive vaccination programs in the world – the National Immunization Program (Programa Nacional de Imunizações, PNI) – that serves all age groups: newborns, children, adolescents, adults, pregnant women and older adults, as well as groups with special needs, such as adolescents, pregnant and older adult women.
•However, vaccination coverage remains below ideal for all available vaccines, especially among adolescents and pregnant women, and Febrasgo is committed to collaborating with the PNI to combat vaccine hesitancy.
•The gynecologist/obstetrician is the reference physician for women, therefore the access to information and updates regarding all vaccines recommended for their patients is extremely important for this professional, aiming at the greatest possible protection.
•The objective of this Febrasgo Position Statement is to bring an update to women’s vaccination schedule, covering some vaccines that are available, including new approved vaccines and those in the commercialization phase.
•This work is a compilation of the First Febrasgo Scientific Immunization Forum held in the city of São Paulo in October 2023 with the objective to update recommendations for vaccines in use and new innovative vaccines soon to be available.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(6):631-635
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(2):150-154
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(3):140-145
To describe the referral for colposcopy in a Hospital in Brazil and the relative frequency of patients who benefited from it, considering the correct indications for the examination and its final diagnoses.
A retrospective study was performed in the colposcopy service database of the Hospital Universitário de Taubaté, Taubaté, state of São Paulo, Brazil. The frequency validated in the analysis of the medical records of women referred for clinical indication or cytological alteration, attended from March 2015 to March 2017. The population selected and analyzed included 256 results that were correlated to the cytological, clinical data and the result of the colposcopy.
Of the women referred, 45% presented out of the age of screening according to the guidelines of cervical cancer screening, 8.6% being adolescents and young adults < 25 years old, and 36.4% of the patients being ≥ 65 years old. A total of 50% of the patients had no indication of colposcopy, that is, normal cytologies, benign changes, ectopia, cervicitis, atypical squamous cells of indeterminate significance (ASC-US) and low-grade intraepithelial lesion (LSIL) without persistence and normal clinical appearance. A total of 39.84% who underwent colposcopy had high-grade lesion or cancer results, thus benefiting from the adequate referral.
Most (60.16%) of the patients referred to the colposcopy service did not benefit from the referral for results without changes, such as negative colposcopies, histologies with no cervical intraepithelial neoplasm (CIN) or only CIN 1, or were out of the age for screening. These findings therefore demonstrate a significant number of unnecessary and inadequate referrals.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(6):457-462
DOI 10.1590/S0100-72032004000600006
OBJECTIVE: to assess the ability of Pap smear and hybrid capture II (HCII) to detect clinically significant cervical lesions (CIN2/3) in women referred to hospital due to atypical squamous cells of unknown significance (ASCUS) or low-grade squamous intraepithelial lesions (LSIL). METHODS: a cross-sectional study comprising 161 women referred to the Taubaté University Hospital due to ASCUS/LSIL, between August 2000 and September 2002. All women responded to a questionnaire regarding sociodemographic and reproductive characteristics and were subjected to gynecological examination with specimen collection for Pap test and HCII, along with colposcopy and eventual cervical biopsy. The relationship between HCII results and age, use of condom, oral hormonal contraception, and smoking were evaluated by the chi-square test. The sensitivity, specificity, positive and negative predictive values of both Pap test and HCII were calculated. All calculations were performed within 95% confidence intervals. RESULTS: sixty-seven percent of the women that tested positive for HPV were less than 30 years old. Pap smear and HCII showed the same 82% sensitivity in detecting CIN2/3 when the threshold for a positive Pap result was ASCUS, LSIL or HSIL. Pap smear specificity and positive predictive values were substantially increased when only HSIL results were considered as positive (from 29 to 95% and 12 to 50%, respectively). These figures were superior to those of HCII, but at the expense of an expressive loss of sensitivity (from 82% to 41%). CONCLUSIONS: our results substantiate the potential of HCII in detecting CIN2/3 among women referred due to ASCUS/LSIL.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(5):365-370
DOI 10.1590/S0100-72032003000500010
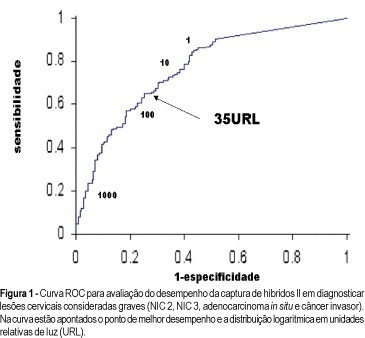
PURPOSE: to assess the performance of hybrid capture II (HCII) HPV viral load in predicting the grade of cervical lesions. METHODS: between August 2000 to November 2002, 309 women admitted due to an abnormal Pap smear result were recruited. Histological disease confirmation was done in all women and cervical intraepithelial neoplasia (CIN) grade 2 or above was considered as severe disease. HCII was done for high-risk HPV types and viral load was estimated in relative light units (RLU). Receiver operating characteristics analysis was used to test the performance of HCII. RESULTS: histological findings included 140 (45.3%) cervicitis or CIN 1 and 199 (54.7%) CIN 2/3, in situ adenocarcinoma or invasive cancer. The best cutoff for HCII in detecting severe disease was 35 RLU, showing a sensitivity of 69% and a specificity of 70%. Association of high-grade cervical lesions at Pap smear and HCII at 35 RLU showed a positive predictive value of 88.2% in diagnosis of CIN 2 or above. On the other hand, 95.7% of the women with low grade lesion at cytology and HCII below 1 RLU presented no severe histological disease. CONCLUSIONS: the best performance of HCII in diagnosing CIN 2 or above was found at 35 RLU. Association of cytology and HCII in different settings provided very high positive and negative predictive values.