Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(10):930-937
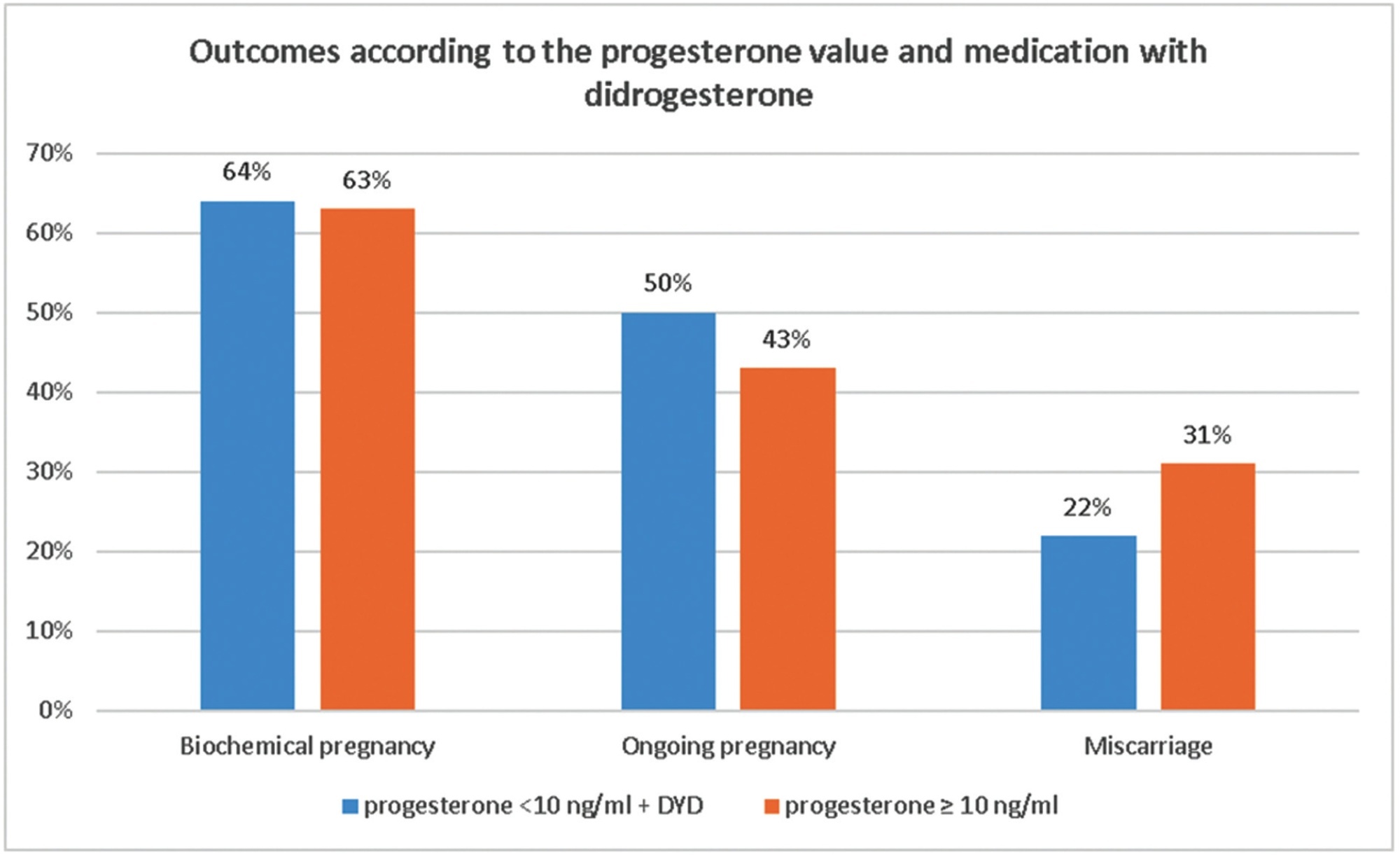
To determine whether a rescue strategy using dydrogesterone (DYD) could improve the outcomes of frozen embryo transfer cycles (FET) with low progesterone (P4) levels on the day of a blastocyst transfer.
Retrospective cohort study including FET cycles performed between July 2019 and October 2020 following an artificial endometrial preparation cycle using estradiol valerate and micronized vaginal P4 (400 mg twice daily). Whenever the serum P4 value was below 10 ng/mL on the morning of the planned transfer, DYD 10 mg three times a day was added as supplementation. The primary endpoint was ongoing pregnancy beyond 10 weeks. The sample was subdivided into two groups according to serum P4 on the day of FET: low (< 10 ng/mL, with DYD supplementation) or normal (above 10 ng/mL). We performed linear or logistic generalized estimating equations (GEE), as appropriate.
We analyzed 304 FET cycles from 241 couples, 11.8% (n = 36) of which had serum P4 below 10 ng/mL on the FET day. Baseline clinical data of patients was comparable between the study groups.
Our results indicate that DYD 10 mg three times a day administered in women who perform FET with P4 serum levels < 10 ng/mL, allows this group to have pregnancy rates beyond 12 weeks at least as good as those with serum levels above 10 ng/mL.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(10):915-924
To assess obstetric/puerperal/neonatal outcomes in an inflammatory bowel disease (IBD) population and to analyze disease characteristics that may be associated to adverse outcomes.
Retrospective descriptive analysis including 47 pregnant womn with IBD (28 with Crohn's disease – CD and 19 with ulcerative colitis – UC) who delivered between March 2012 and July 2018 in a tertiary hospital. We reviewed clinical records to extract demographic information, previous medical history, disease subtype, activity, severity, treatment, and obstetric, puerperal, and neonatal outcome measures.
Obstetric and neonatal complications (composite outcomes) occurred in 55.3% and 14.6% of the IBD population, respectively, and were more frequent in UC patients. Preterm birth (PTB), preeclampsia, anemia, low birth weight (LBW), and neonatal death were also more frequent in UC patients. The rate of postpartum hemorrhage (PPH) was 14.9%, and it was higher in CD patients. Women with active IBD had more obstetric/neonatal adverse outcomes (fetal growth restriction and LBW in particular) and cesarean sections. Patients with medicated IBD had less obstetric/neonatal complications (PTB and LBW in specific) and cesarean sections but more PPH.
Women with IBD may have an increased risk of obstetric/puerperal/neonatal adverse outcomes. Ulcerative colitis patients had more obstetric and neonatal complications, whereas PPH was more frequent if CD patients. Other disease characteristics were considered, which allowed a better understanding of their possible influence. Although more research is needed, this work reinforces the importance of adequate surveillance to allow prompt recognition and treatment of complications.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(10):909-914
To evaluate the iodine sufficiency of pregnant women assisted in a University Hospital of Minas Gerais, and to correlate the urinary concentrations of maternal iodine with the fetal thyroid hormone levels at birth.
Urinary iodine concentrations from 30 pregnant women with a singleton pregnancy and gestational age lower than 20 weeks were analyzed. Occasional samples of the mothers' urine were collected for the urinary iodine concentration dosage, and these were correlated with the newborns' thyroid-stimulating hormone (TSH) levels.
The median iodine urinary concentration of this study's pregnant women population was 216.73 mcg/l, which is proper for the group, following the World Health Organization (WHO). No cases of neonatal hypothyroidism were reported in the study, which corroborates the iodine sufficiency in this population sample.
This study shows that despite the increased demand for iodine from pregnant women and the Brazilian Health Regulatory Agency (ANVISA) recommendation of 2013 for reduction of salt iodization levels, the population of pregnant women attended in the prenatal ambulatory of normal risk from the Federal University of Minas Gerais is considered sufficient in iodine. As a higher sample is necessary for the confirmation of these findings, it is too early to recommend the universal supplementation of iodine for Brazilian pregnant women, and more studies must be carried out, considering that iodine supplementation for pregnant women in an area of iodine sufficiency is associated to the risks of the fetus's excessive exposure to iodine.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(9):830-837
To use the Robson Ten Group Classification (RTGC) to analyze cesarean section (CS) rates in a Honduran maternity hospital, with focus in groups that consider induction of labor.
Cross-sectional study. Women admitted for childbirth (August 2017 to October 2018) were classified according to the RTGC. The CS rate for each group and the contribution to the overall CS rate was calculated, with further analyses of the induction of labor among term primiparous (group 2a), term multiparous (group 4a), and cases with one previous CS (group 5.1).
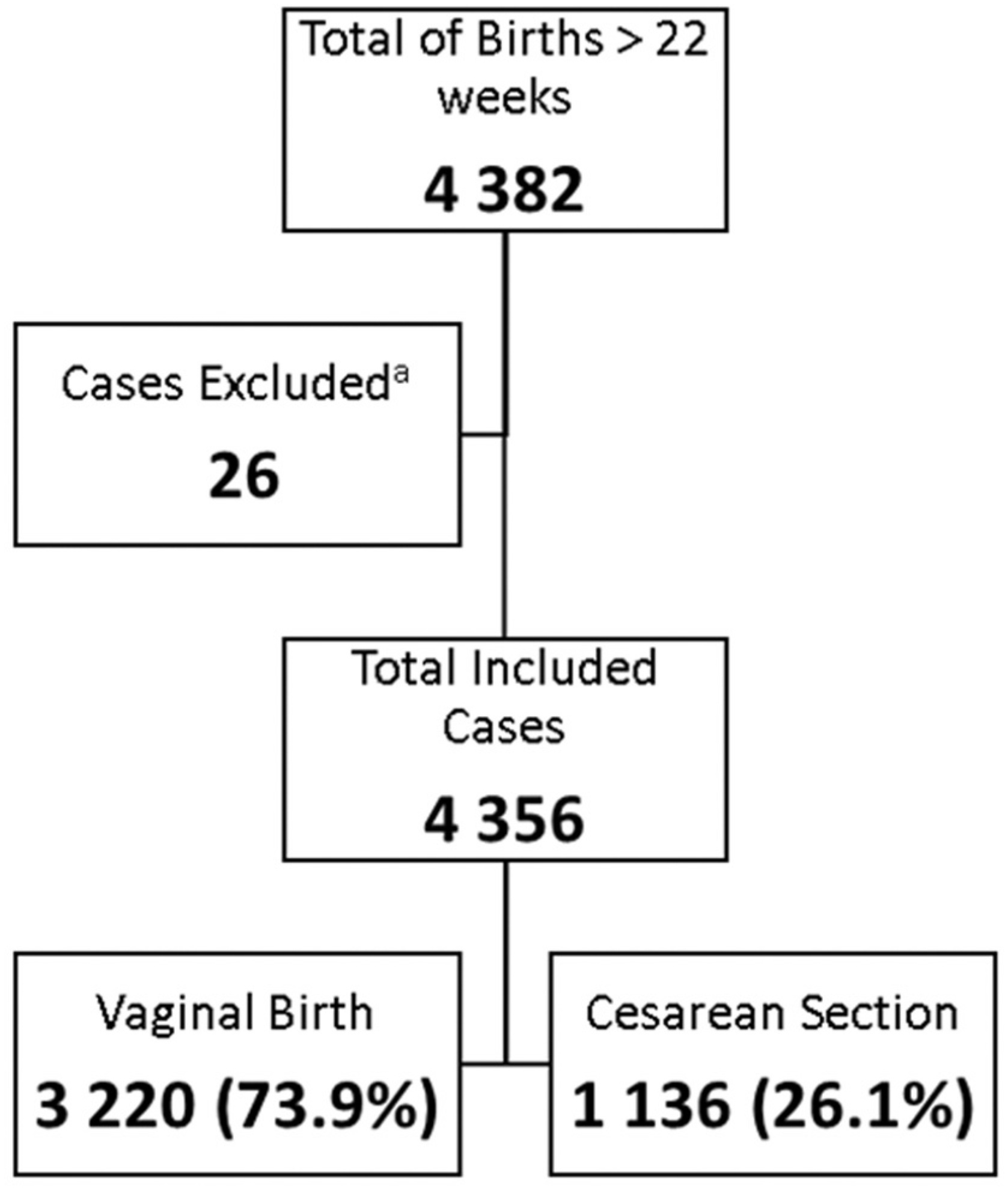
A total of 4,356 women were considered, with an overall CS rate of 26.1%. Group 3 was the largest group, with 38.6% (1,682/4,356) of the cases, followed by Group 1, with 30.8% (1,342/4,356), and Group 5, with 10.3% (450/4,356). Considering the contribution to overall CS rates per group, Group 5 contributed with 30.4% (345/1,136) of the CSs and within this group, 286/345 (82.9%) had 1 previous CS, with a CS rate > 70%. Groups 1 and 3, with 26.6% (291/1,136) and 13.5% (153/1,136), respectively, were the second and third larger contributors to the CS rate. Groups 2a and 4a had high induction success, with low CS rates (18.4 and 16.9%, respectively).
The RTGC is a useful tool to assess CS rates in different healthcare facilities. Groups 5, 1, and 3 were the main contributors to the CS rate, and groups 2 and 4 showed the impact and importance of induction of labor. These findings may support future interventions to reduce unnecessary CS, especially among primiparous and in women with previous CS.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(9):838-844
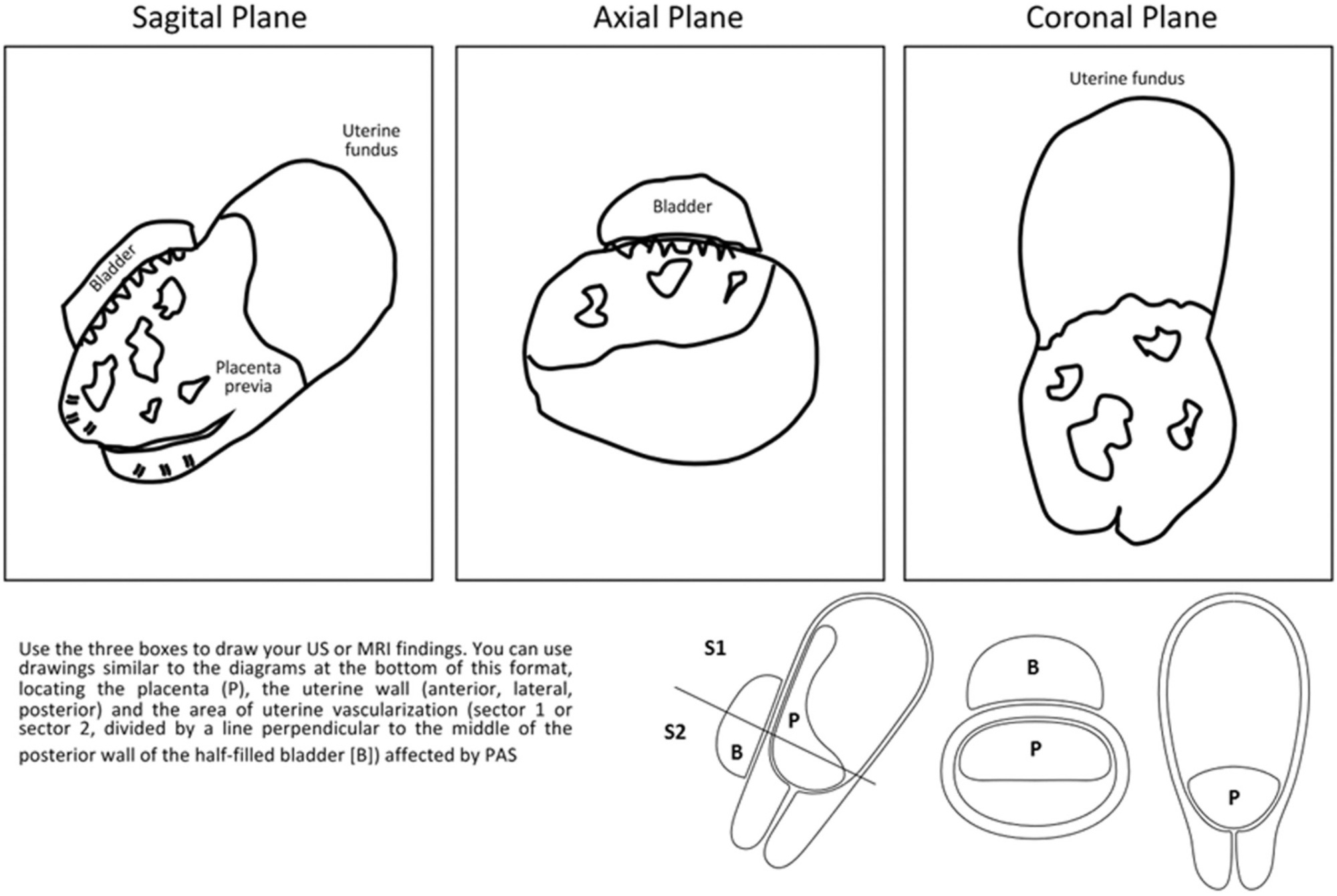
The immediate referral of patients with risk factors for placenta accreta spectrum (PAS) to specialized centers is recommended, thus favoring an early diagnosis and an interdisciplinary management. However, diagnostic errors are frequent, even in referral centers (RCs). We sought to evaluate the performance of the prenatal diagnosis for PAS in a Latin American hospital.
A retrospective descriptive study including patients referred due to the suspicion of PAS was conducted. Data from the prenatal imaging studies were compared with the final diagnoses (intraoperative and/or histological).
A total of 162 patients were included in the present study. The median gestational age at the time of the first PAS suspicious ultrasound was 29 weeks, but patients arrived at the PAS RC at 34 weeks. The frequency of false-positive results at referring hospitals was 68.5%. Sixty-nine patients underwent surgery based on the suspicion of PAS at 35 weeks, and there was a 28.9% false-positive rate at the RC. In 93 patients, the diagnosis of PAS was ruled out at the RC, with a 2.1% false-negative frequency.
The prenatal diagnosis of PAS is better at the RC. However, even in these centers, false-positive results are common; therefore, the intraoperative confirmation of the diagnosis of PAS is essential.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(9):821-829
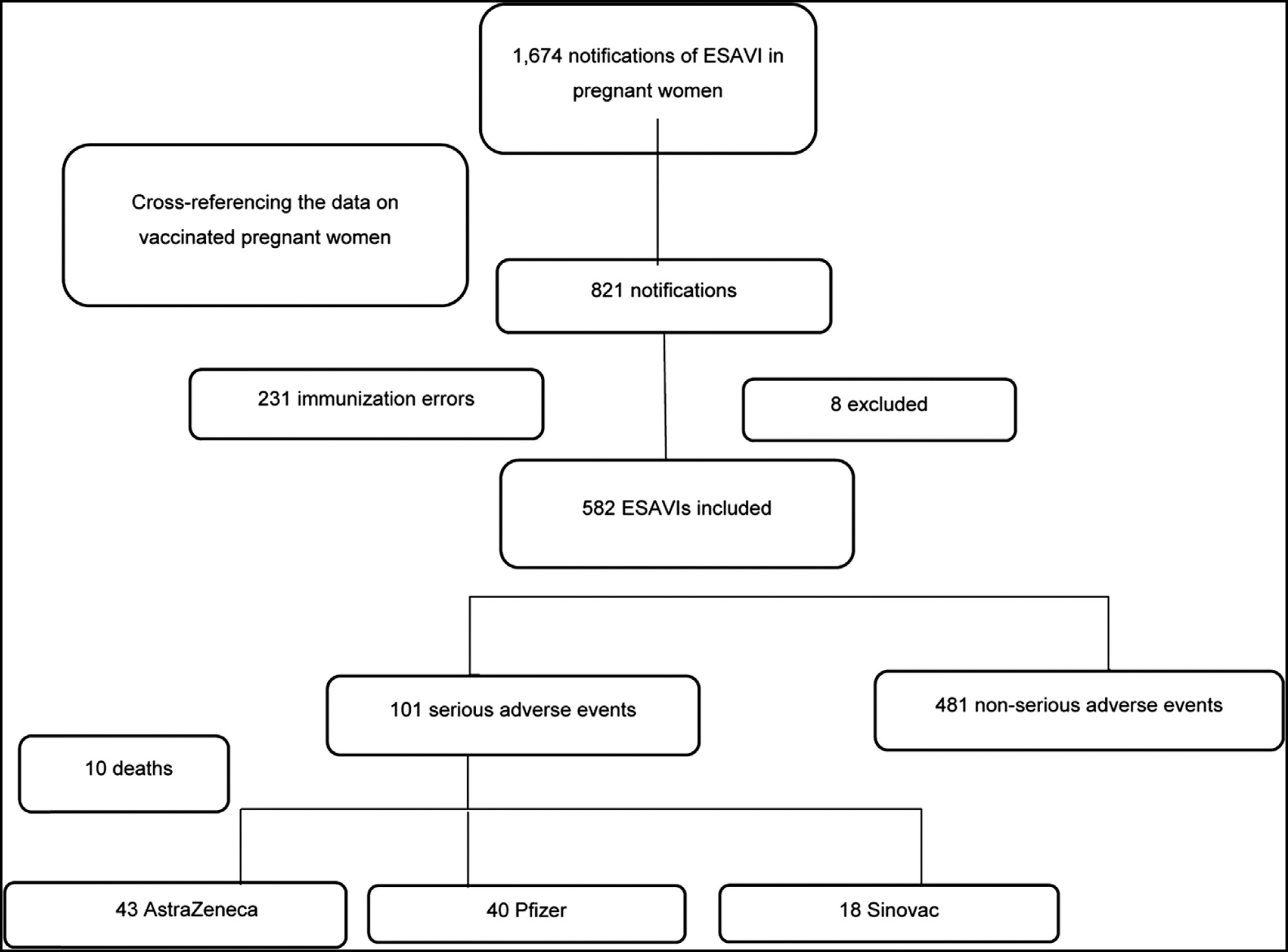
Regulations for the vaccination of pregnant women in Brazil occurred in March 2021. Despite the absence of robust data in the literature on the coronavirus disease 2019 (COVID-19) vaccinations in pregnant women, it is understood that the benefit-risk ratio tends to be favorable when considering the pandemic and the high burden of the disease. However, it is still important to monitor for Events Supposedly Attributable to Vaccination or Immunization (ESAVI) and to draw safety profiles of the different platforms used in pregnant and postpartum women. The present study aims to describe the main characteristics of ESAVIs related to COVID-19 vaccines occurring in pregnant women in the first months of the vaccination campaign in Brazil. During the evaluation period, 1,674 notifications of ESAVIs in pregnant women were recorded, and 582 notifications were included for the analysis. Of the 582 ESAVIs identified, 481 (82%) were classified as non-serious adverse events and 101 (17%) as serious adverse events. Ten deaths were identified, including one death which was considered to be causally related to the vaccine. The other nine maternal deaths had causality C, that is, without causal relationship with the vaccine, and most were due to complications inherent to pregnancy, such as pregnancy-specific hypertensive disorder (PSHD) in 4 cases and 3 due to COVID-19. Despite some limitations in our study, we believe it brings new insights into COVID-19 vaccines in this group and will add to the available evidence.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(10):925-929
Placenta accreta spectrum (PAS) is a cause of massive obstetric hemorrhage and maternal mortality. The application of family-centered delivery techniques (FCDTs) during surgery to treat this disease is infrequent. We evaluate the implementation of FCDTs during PAS surgeries.
This was a prospective, descriptive study that included PAS patients undergoing surgical management over a 12-month period. The patients were divided according to whether FCDTs were applied (group 1) or not (group 2), and the clinical outcomes were measured. In addition, hospital anesthesiologists were surveyed to evaluate their opinions regarding the implementation of FCDTs during the surgical management of PAS.
Thirteen patients with PAS were included. The implementation of FCDTs during birth was possible in 53.8% of the patients. The presence of a companion during surgery and skin-to-skin contact did not hinder interdisciplinary management in any case.
Implementation of FCDTs during PAS care is possible in selected patients at centers with experience in managing this disease.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(9):866-870
Female sterilization is a surgical procedure that aims women to permanently stop the use of conception. The benefits, risks and cost-effectiveness are important issues. The purpose of this study was comparing the applicability, complications and efficacy of salpingectomy versus electrocoagulation and tubal occlusion by laparoscopy in the Ambulatory Surgery Unit.
We performed a retrospective and observational study that included women undergoing laparoscopic sterilization procedures at our Ambulatory Surgery Unit, during three years. Statistical analysis was performed using SPSS, applying the Fisher exact test, the Mann-Whitney test, and Linear Regression.
Two hundred and twenty-one laparoscopic surgical procedures were performed, including 79 (35.7%) bilateral total salpingectomies and 142 (64.3%) electrocoagulation and bilateral tubal occlusion procedures. The majority of the procedures were performed by a resident (n = 162; 73.3%), with 40% (n = 33) of salpingectomies. The surgical time, independently the type of surgeon, was significantly shorter in the tubal occlusion (42.2 vs. 52.7 min, p < 0.001). Safety and efficacy endpoints were not significantly different between the two groups, with a case of pregnancy in tubal occlusion group.
Salpingectomy is a safe and effective alternative comparing with electrocoagulation and tubal occlusion.