Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo46
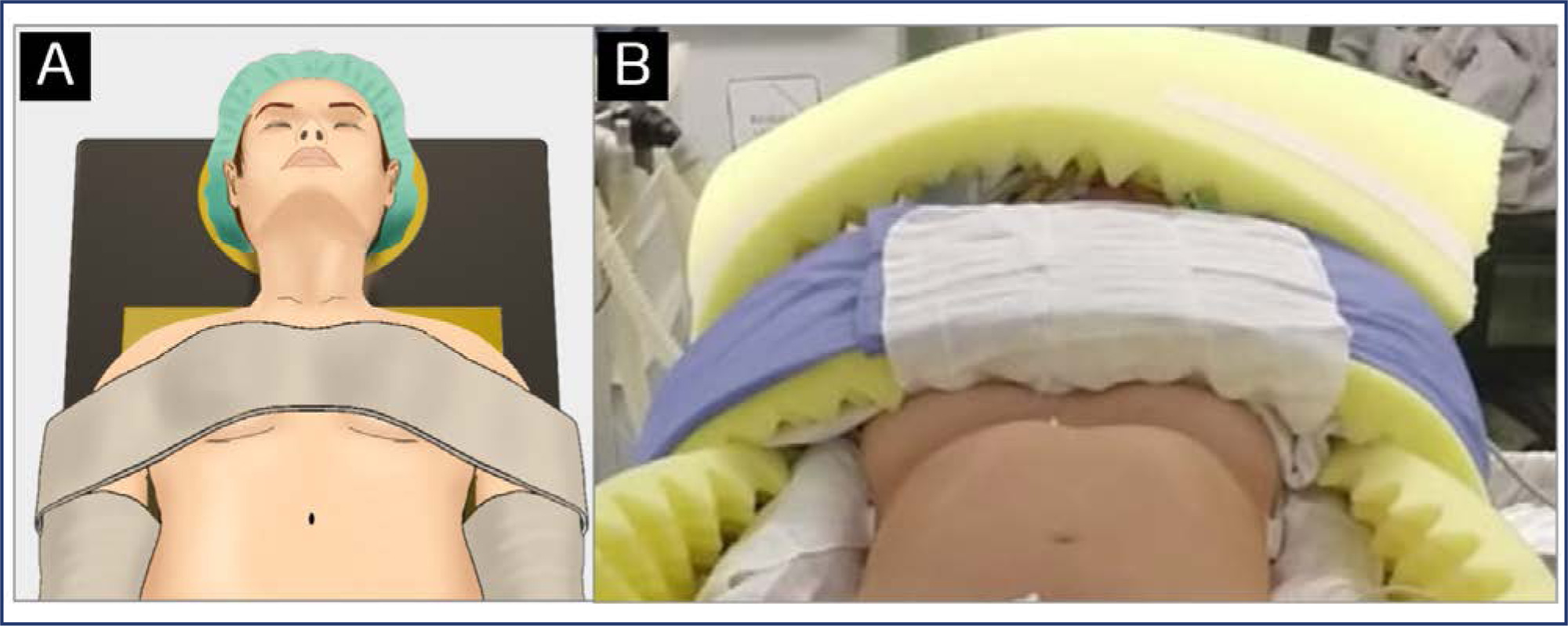
Effective patient positioning is a critical factor influencing surgical outcomes, mainly in minimally invasive gynecologic surgery (MIGS) where precise positioning facilitates optimal access to the surgical field. This paper provides a comprehensive exploration of the significance of strategic patient placement in MIGS, emphasizing its role in preventing intraoperative injuries and enhancing overall surgical success. The manuscript addresses potential complications arising from suboptimal positioning and highlights the essential key points for appropriate patient positioning during MIGS, encompassing what the surgical team should or shouldn't do. In this perspective, the risk factors associated with nerve injuries, sliding, compartment syndrome, and pressure ulcers are outlined to guide clinical practice. Overall, this paper underscores the critical role of precise patient positioning in achieving successful MIGS procedures and highlights key principles for the gynecological team to ensure optimal patient outcomes.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(5):266-272
This study analyzes the role of clinical simulation in internal medical residency programs (IMRP) in Obstetrics and Gynecology (OB/GYN), attributed by the supervisors, in the training of residents in the city of São Paulo (SP).
Cross-sectional descriptive, qualitative, and exploratory approach. Semi-structured interviews were performed with ten supervisors of Medical Residency programs in Obstetrics and Gynecology. Interviews were analyzed by means of content analysis under the thematic modality, starting with the core the role of clinical simulation in Obstetrics and Gynecology Medical Residency Programs.
Supervisors view Clinical simulation as: a complementary tool for the teaching and learning process, a possibility of a safe teaching and learning environment, an opportunity to learn from mistakes, a support for professional practice committed to patient safety, a learning scenario for teamwork, a scenario for reflection on the work process in Obstetrics and Gynecology, a scenario for evaluative processes in the medical residency. Still according to supervisors, Clinical Simulation favors decision-making and encourages the resident participation in activities.
Supervisors recognize Clinical Simulation as a powerful pedagogical tool in the learning process of resident doctors in Obstetrics and Gynecology Residency Programs.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(6):258-264
In the pregnancy-puerperal cycle, women may develop complications that require admission to the Intensive Care Unit (ICU). Thus, special attention to pharmacotherapy is necessary, particularly to potential drug interactions (PDIs) and to the effect of the drugs on the fetus and newborn.
The aim of this study was to determine the profile of PDIs and the potential risk of drugs used during pregnancy and breastfeeding among patients admitted to the ICU.
We conducted an observational, cross-sectional and prospective study, including pregnant and breastfeeding women admitted to the ICU at the Women’s Hospital of a university in the city of Campinas, Brazil, for one year. Online databases were used to identify and classify the PDIs and the potential risk of the drugs used during pregnancy and breastfeeding.
We evaluated 305 prescriptions of 58 women, 31 pregnant and 27 breastfeeding, and 284 (91%) prescriptions presented PDIs. A total of 175 different combinations of PDIs were identified in the prescriptions, and adverse effects caused by the simultaneous use of drugs were not actually observed in the clinical practice. A total of 26 (1.4%) PDIs were classified as contraindicated. We identified 15 (13.8%) drugs prescribed with risk D, and 2 (1.8%) with risk X for pregnant women, as well as 4 (4.9%) drugs prescribed with high risk for breastfeeding women.
This study demonstrates that there is a high incidence of PDIs in prescriptions. Most drugs used by pregnant and breastfeeding women at the ICU did not present serious risks to their fetus and newborns, but sometimes drugs with risk D or X are necessary in the course of the treatment.