Home
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(7):308-313
07-01-2015
DOI 10.1590/S0100-720320150005343
To estimate the likelihood of axillary lymph node involvement for patients with early-stage breast cancer, based on a variety of clinical and pathological factors.
A retrospective analysis was done in hospital databases from 1999 to 2007. Two hundred thirty-nine patients were diagnosed with early-stage breast cancer. Predictive factors, such as patient age, tumor size, lymphovascular invasion, histological grade and immunohistochemical subtype were analyzed to identify variables that may be associated with axillary lymph node metastasis.
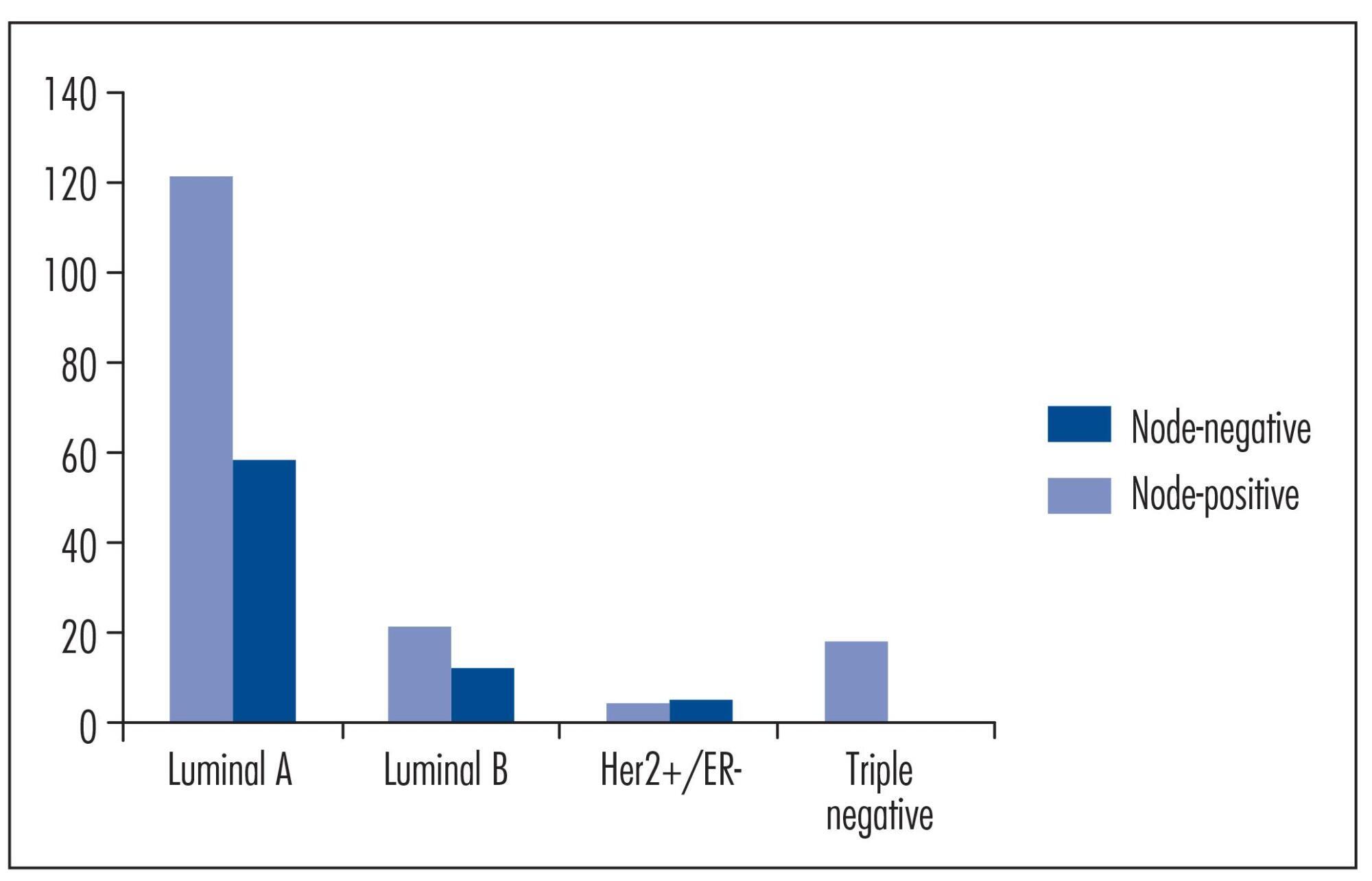
Patients with tumors that are negative for estrogen receptor, progesterone receptor, and HER2 had approximately a 90% lower chance of developing lymph node metastasis than those with luminal A tumors (e.g., ER+ and/or PR+ and HER2-) - Odds Ratio: 0.11; 95% confidence interval: 0.01-0.88; p=0.01. Furthermore, the risk for lymph node metastasis of luminal A tumors seemed to decrease as patient age increased, and it was directly correlated with tumor size.
The molecular classification of early-stage breast cancer using immunohistochemistry may help predicting the probability of developing axillary lymph node metastasis. Further studies are needed to optimize predictions for nodal involvement, with the aim of aiding the decision-making process for breast cancer treatment.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(7):308-313
07-01-2015
DOI 10.1590/S0100-720320150005343
To estimate the likelihood of axillary lymph node involvement for patients with early-stage breast cancer, based on a variety of clinical and pathological factors.
A retrospective analysis was done in hospital databases from 1999 to 2007. Two hundred thirty-nine patients were diagnosed with early-stage breast cancer. Predictive factors, such as patient age, tumor size, lymphovascular invasion, histological grade and immunohistochemical subtype were analyzed to identify variables that may be associated with axillary lymph node metastasis.
Patients with tumors that are negative for estrogen receptor, progesterone receptor, and HER2 had approximately a 90% lower chance of developing lymph node metastasis than those with luminal A tumors (e.g., ER+ and/or PR+ and HER2-) - Odds Ratio: 0.11; 95% confidence interval: 0.01-0.88; p=0.01. Furthermore, the risk for lymph node metastasis of luminal A tumors seemed to decrease as patient age increased, and it was directly correlated with tumor size.
The molecular classification of early-stage breast cancer using immunohistochemistry may help predicting the probability of developing axillary lymph node metastasis. Further studies are needed to optimize predictions for nodal involvement, with the aim of aiding the decision-making process for breast cancer treatment.


Search
Search in:
