Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(10):603-608
12-11-2023
To evaluate the performance of residents in gynecology and obstetrics before and after practicing laparoscopic sutures, to establish when the training shows the best results, in addition to comparing whether being in different years of residency influences this progression.
A prospective cohort study involving 32 medical residents evaluated with a pretest to establish their previous knowledge in laparoscopic suture. This test consisted of knotting two wires, one made of polypropylene and the other of polyglactin, with a blocking sequence of five semi-knots. We set a 30-minute limit to complete the task. Then, the residents held four training meetings, focusing on suture, Gladiator rule, knot, and symmetries, in addition to executing blocking sequences. A second test to establish progress was performed.
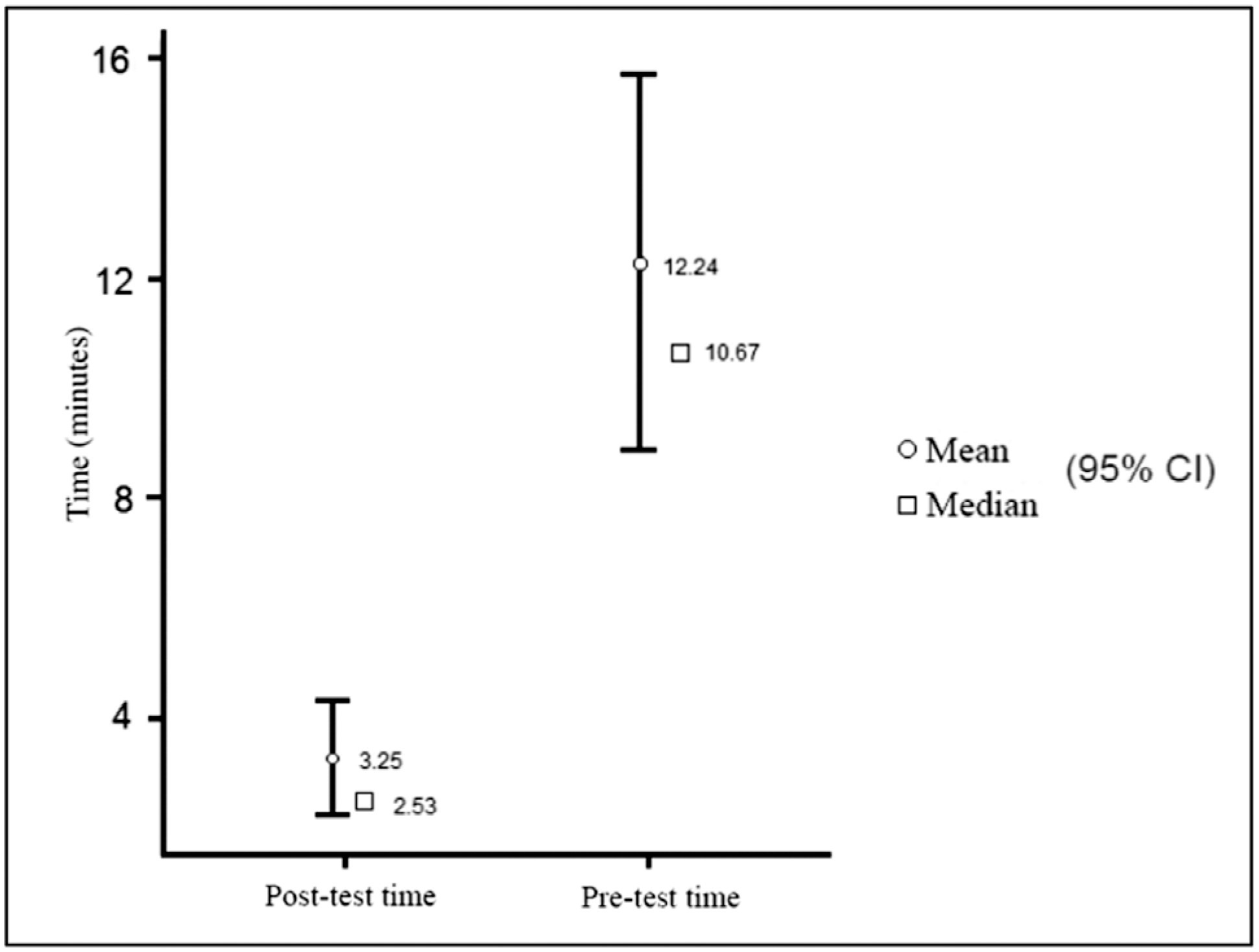
Regarding the time spent to make the stiches using polyglactin wire, a statistically significant time improvement (p< 0.01) was observed, with a 10.67-minute pretraining median (mean 12.24 minutes) and a 2.53-minute posttraining median (mean 3.25 minutes). Regarding the stitches with polypropylene wire, a statistically significant time improvement (p< 0.05) was also observed, with a 9.38-minute pretraining median (mean 15.43 minutes) and a 3.65-minute posttraining median (mean 4.54 minutes). A total of 64.2% of the residents had been able to make the knot with polypropylene previously. One hundred percent were able to complete the task in the posttest.
Model training using the Gladiator rule for laparoscopic suture improves the knotting time with statistically similar performance, regardless of the year of residency, after systematic training.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(2):86-91
02-01-2018
To compare the quality of cervicovaginal samples obtained from basic health units (BHUs) of the Unified Health System (SUS) and those obtained fromprivate clinics to screen precursor lesions of cervical cancer.
It was an intervention study whose investigated variables were: adequacy of the samples; presence of epithelia in the samples, and cytopathological results. A total of 940 forms containing the analysis of the biological samples were examined: 470 forms of women attended at BHUs of the SUS and 470 forms of women examined in private clinics in January and February of 2016.
All the unsatisfactory samples were collected at BHUs and corresponded to 4% of the total in this sector (p < 0.0001). There was a higher percentage of samples containing only squamous cells in the SUS (43.9%). There was squamocolumnar junction (SJC) representativeness in 82.1% of the samples from the private clinics (p < 0.0001). Regarding negative results for intraepithelial lesions and/or malignancies, the percentages obtained were 95.9% and 99.1% (p < 0.0049) in the exams collected in the private system and SUS, respectively. Less serious lesions corresponded to 0.89% of the samples from the SUS and 2.56% of the tests from the private sector; more serious lesions were not represented in the samples obtained from BHUs, whereas the percentage was 1.49% in private institutions.
Unsatisfactory cervical samples were observed only in exams performed at the SUS. There is a need for guidance and training of professionals who perform this procedure to achieve higher reliability in the results and more safety for women who undergo this preventive test.