Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(5):196-202
DOI 10.1590/S0100-72032012000500002
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(4):196-200
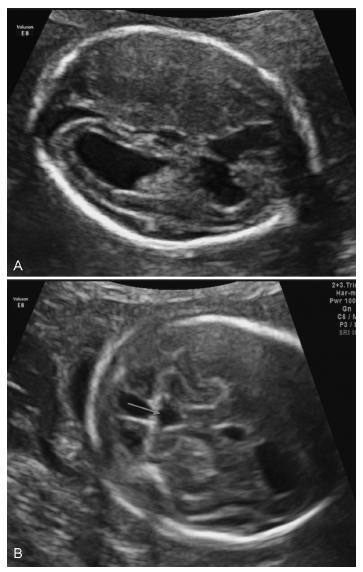
Cytomegalovirus (CMV) is the most common congenital viral infection, causing hearing, visual and psychomotor impairment. Preexisting maternal CMV immunity substantially reduces, but not eliminates, the risk of fetal infection and affectation. This article is about a case of nonprimary maternal CMV infection during pregnancy, with vertical transmission, resulting in severe fetal affectation. Preconceptional analysis indicated maternal CMV past infection. Pregnancy progressed uneventfully until the 20th week ultrasound (US), which revealed cerebral abnormalities: thin and hyperechogenic cerebral cortex with prominent lateral ventricles, bilateral periventricular hyperechogenicities, cerebellar vermis hypoplasia and absent corpus callosum. The MRI suggested these findings were compatible with congenital infection rather than primary brain malformation.
The fetal karyotype was normal. The title of CMV's IgG antibodies almost tripled. Since the first semester,analysisof the polymerasechainreaction(PCR)forCMVDNAintheamniotic fluid was negative. The pregnancy was terminatedat 23weeks. Neuropathologicalfindings at autopsy showed severe brain lesions associated with CMV infection.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2009;31(4):196-202
DOI 10.1590/S0100-72032009000400007
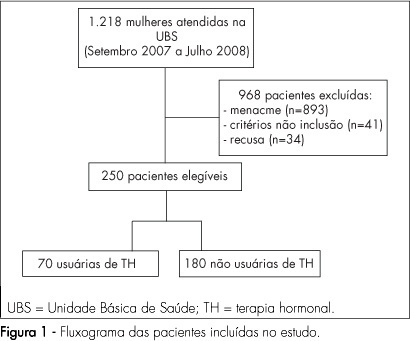
PURPOSE: to evaluate the quality of life of post-menopause women, users and non-users of hormonal therapy (HT), in a Healthcare Unit in Franca, São Paulo, Brazil. METHODS: a clinical transversal study, carried out with 250 post-menopausal women, with ages from 45 to 70 years old, attended to in Healthcare Units, from September 2007 to August 2008. Participants were divided into two groups: HT users (n=70) and non-users (n=180). Women making continuous HT use for at least six months were considered as users. Sociodemographic and clinical characteristics have been evaluated. Blatt-Kupperman's menopausal index has been applied to assess climacteric symptoms, and the Women's Health Questionnaire (WHQ), to assess their quality of life. Fisher's exact test or χ2 and Mann-Whitney and Kruskal-Wallis's tests have been used for the statistical analysis. RESULTS: no significant difference has been found in the comparison of groups, concerning age, menarche, menopause, parity and body mass index. It has been seen that 67.2% of the women were married, 83.2% had attended primary school and 53.2% were housewives, with no difference between the groups. HT users reported lower frequency of climacteric symptoms (BKMI) with moderate and marked intensity, as compared to non-users (p<0.001). Even though HT users presented lower average score in cognitive deficit (p<0.001), vasomotor symptoms (p=0.04), sleeping problems (p<0.001), attractiveness (p=0.02) from the WHQ, there has been no difference in the total score, as compared to non-users. CONCLUSIONS: post-menopausal women, HT users and non-users, admitted at Healthcare Units, have not presented differences in global quality of life.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(4):197-203
DOI 10.1590/S0100-72032005000400006
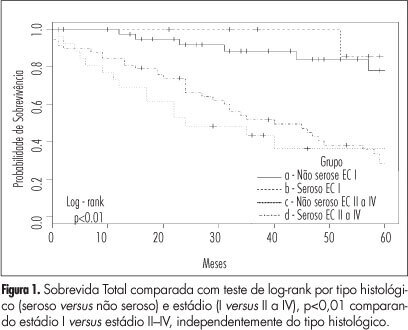
PURPOSE: to apply a severity score to cases of severe maternal morbidity (SMM) and to compare the classification criteria. METHODS: a control-case study was performed as a secondary analysis of cases of SMM in a tertiary level maternity unit for a period of 12-month. A specific score for assessing the degree of severity was applied to cases identified as SMM. Twenty cases of near miss maternal morbidity (higher severity) were compared to 104 control cases (lower severity) of other severe morbidities, regarding risk factors, primary determinants and assistance requirements. Analyses were performed with means and proportions, using Student's t, Wilcoxon and chi2 statistical tests, and estimations of OR and 95% CI. RESULTS: the higher severity (near miss) was identified in 16.1% of cases and the history of abortion was the only factor statistically associated with it (OR=3.41, 95% CI 1.08-10.79). In fact, the indices of assistance complexity were more frequent in the near-miss morbidity group, which also presented less hypertension (30% against 62.5%) and more hemorrhage (35.5% against 10.6%) as primary determinant factors of severe morbidity. CONCLUSIONS: the higher severity of maternal morbidity was associated with a history of abortion and with hemorrhage as a cause. The applied score was able to identify a higher severity subgroup (near miss), which needs more complex professional and institutional care in order to avoid the occurrence of death.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(4):198-201
DOI 10.1590/S0100-72032010000400008
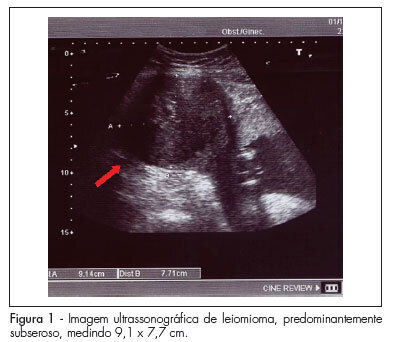
Uterine leiomyomas are characterized as a benign disease and are observed in 2 to 3% of all normal pregnancies. Out of these, about 10% may present complications during pregnancy. We present a case of a pregnant patient sought emergency obstetric care at the 17th week, complaining of severe pain, presenting with painful abdominal palpation and sudden positive decompression. Ultrasonography revealed a myoma nodule measuring 9.1 x 7.7 cm; the patient was hospitalized and medicated, being also submitted to laparotomy and myomectomy due to worsening of her condition. Prenatal care revealed no further abnormalities, with resolution of gestation at 39 weeks. The newborn weighed 3,315 g, with Apgar scores of 9 and 10. In such cases, clinical treatment should always be attempted and surgery should be considered only in selected cases, mainly in the impossibility of conservative treatment or when the patient's clinical features require immediate intervention. In this case, myomectomy was effective against maternal-fetal obstetric complications.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(5):198-204
DOI 10.1590/S0100-7203201400050003
To assess the adherence to a cervical cancer screening program and to identify reported reasons for inadequate screening in women receiving care as part of the Family Health Strategy.
A selective prevalence study on cervical cancer screening in women receiving care as part of the Family Health Strategy in the cities of Duque de Caxias and Nova Iguaçu in the state of Rio de Janeiro, southeastern Brazil, nine years after they participated in a previous study of the Brazilian National Cancer Institute. Only those women who were not diagnosed with CIN II or more severe lesions by histopathology, did not undergo hysterectomy during the study period and still resided in the communities were eligible to participate in the study. Information on exam sites, test results and schedules, sociodemographic characteristics and reported reasons of non-adherence was obtained. Data were collected through interviews and medical record review. The prevalence of adherence to screening was estimated, and the chi-square test was used to compare proportions between the variables studied and their relationship with the reported reasons of non-adherence to screening.
A total of 764 women were interviewed, 70.7% of whom received adequate cervical cancer screening. The reported reasons for inadequate screening included: no risk perception (44.6%), social barriers (26.3%), perceived barriers to action (22.3%) and institutional barriers (21.4%). These reasons were proportionately higher among residents of Nova Iguaçu than among residents of Duque de Caxias (p<0.01), except for institutional barriers (p=0.19).
Although difficulties and barriers were reported, there was good adherence to cervical cancer screening among the women studied. Health providers should receive proper training for complying with the Brazilian Ministry of Health guidelines of regular testing and to facilitate access to screening.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(5):199-204
DOI 10.1590/S0100-72032013000500002
PURPOSE: To determine the prevalence and associated factors of the hospitalization of pregnant women for treatment of urinary tract infection and the repercussions on the health of the newborn, and the absence of a urine exam during the prenatal period. METHODS: A cross-sectional design, where were eligible all mothers of newborns with births occurring between January 1st and December 31, 2010 in Rio Grande (RS). Mothers were interviewed in the two maternity hospitals in the city. Information was collected regarding hospitalization for urinary tract infection, the prenatal assistance and sociodemographic conditions. Statistical analyses were performed by levels and controlled for confounding using Poisson regression. RESULTS: Of the 2,288 women eligible for the study, 2.9% were hospitalized for treatment of urinary tract infection and was higher, after adjustment, in woman with lowest economic status (3.1% the lowest and 2.1% the highest), younger (4.0% in adolescents and 1.8% in those over 30 years), had less education (3.1% had seven years or less of studying and 1.2% had 12 years or more) and did not live with a partner (4.3% living without partner and 2.6% living with partner). Pathologies of the newborn associated with hospitalization, were preterm birth (4.1% in pre-term and 2.7% in those at term) and low birth weight (6.4% in low and 2.6% in those in normal). Of the women who underwent prenatal care, 23.6% had not done the urine test as recommended and, after adjustment, and the risk for not done the test was higher among those with lower socioeconomic status (34.4% in lower and 14.4% in the highest level), less educated (32.3% with seven years or less of studying and 11.0% with 12 years or more) and not living with a partner (32.7% living without partner and 22.0% living with partner). CONCLUSIONS: The high rate of hospitalization reflects the lack of effectiveness of screening for urinary tract infection during pregnancy. The socioeconomic profile of women who required hospitalization and who did not undergo adequate screening of urinary tract infection in prenatal care, demonstrate the need of more careful attention to pregnant women with the features found.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(4):199-205
DOI 10.1590/S0100-72031998000400005
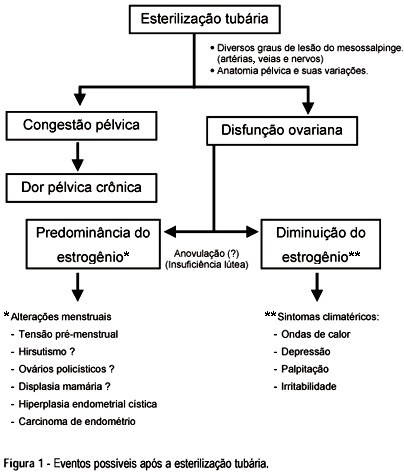
The purpose of the present study was to investigate the menstrual disturbances and the psychological effects of post-tubal sterilization - the so-called post-tubal sterilization syndrome. Does it exist? The authors followed-up prospectively 300 women from the Gynecological Endoscopy and Family Planning Section, Department of Obstetrics and Gynecology, Botucatu Medical School, Universidade Estadual Paulista (UNESP) during one, three and five years after tubal sterilization surgery. Different parameters such as menstrual cycle length, duration of menstrual flow, dysmenorrhea, pelvic pain, regret rates etc, after tubal ligation, were analyzed. Each woman served as her own control. In conclusion, our findings suggest that most women reported no menstrual changes subsequent to sterilization. These findings do not deny or diminish the importance or benefits of tubal sterilization, but serve as a focus for further investigation.