Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(3):136-140
DOI 10.1590/S0100-72032013000300008
Anti-mullerian hormone (AMH) is a glycoprotein produced by granulosa cells of primary, pre-antral and small antral ovarian follicles and its clinical applicability has been recently demonstrated by several studies. Prediction of the response to ovarian stimulation for in vitro fertilization corresponds to the most frequent utilization of AMH in clinical practice, being routinely assessed in many services to identify subgroups of women susceptible to a poor response or to Ovarian Hyperstimulation Syndrome. There are great perspectives that AMH may be applicable to the individual determination of risk for iatrogenic gonadal injury in women with neoplasms who will be submitted to chemotherapy. It is also probable that AMH assessment will be included in protocols for the investigation of amenorrhea and oligomenorrhea, since AMH levels are increased in Polycystic Ovary Syndrome, reduced in premature ovarian failure and normal in other conditions such as hyperprolactinemia and hypogonadotropic hypogonadism. It is possible that AMH will be utilized in the future for the prediction of age at menopause and of reproductive prognosis, providing solid bases for pre-conceptive and contraceptive counseling.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(2):136-136
DOI 10.1590/S0100-72032003000200011
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(2):136-136
DOI 10.1590/S0100-72032003000200010
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(2):136-136
DOI 10.1590/S0100-72032002000200012
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(2):136-136
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(2):136-136
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2011;33(7):137-142
DOI 10.1590/S0100-72032011000700004
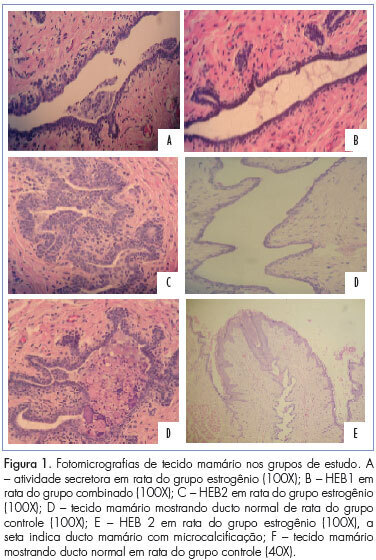
PURPOSE: To evaluate the efect of trimegestone on the histological changes of the mammary tissue of castrated rats. METHODS: Forty-five virgin female Wistar rats were used after oophorectomy. Sixty days after surgery, with hypoestrogenisms confirmed, the experimental rats were randomly assigned to three groups of 15 animals each, when then the specific treatment for each group was started. The control group (C) and experimental groups 1 and 2 respectively received 0.9% saline solution, 17-beta-estradiol and 17-beta-estradiol in combination with trimegestone for 60 consecutive days. After the end of treatment , the inguinal mammary glands were removed, stained with hematoxylin and eosin (HE) for morphometry and examined by immunohistochemistry for the quantification of anti-PCNA antibody in the mammary tissue, followed by euthanasia. The morphometric parameters evaluated were: epithelium cell-proliferation, secretor activity and mammary stroma changes. There were nine deaths during the experiment. The variables were submitted to statistical analysis adopting the 0.05 level of significance. RESULTS:Histological changes were observed in 16/36 rats, mild epithelial hyperplasia in 13/36, moderate epithelial hyperplasia in 3/36, with no cases of severe epithelial hyperplasia. Stromal fibrosis was found in 10/36 and secretory activity in 5/36 rats. All morphometric variables were significant in the estrogen group compared to control (p=0.0361), although there were no difference between the group receiving combined treatment and the controls (p=0.405). The immunohistochemical analysis showed no difference between groups. CONCLUSIONS:The hormones administered to castrated rats, i.e., 17 beta-estradiol alone or in combination with trimegestone, increased the proliferation of breast cells, but this effect appeared to be lower in the combined treatment, the same occurring regarding fibrosis of the mammary stroma.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(3):137-146
Breaking bad news (BBN) is particularly difficult in perinatology. Previous research has shown that BBN skills can be learned and improved when taught and practiced. This project evaluated whether a structured training session would enhance perinatology residents’ skills in BBN.
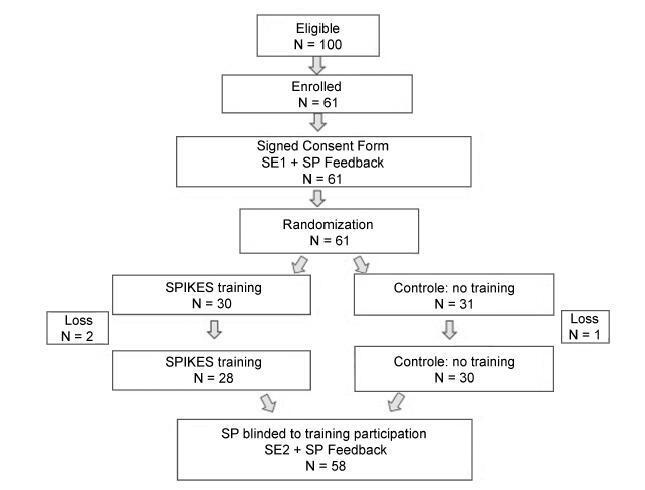
This was a randomized controlled intervention study with year 1 to 4 Perinatology residents from a medical school in Brazil, during the 2014/15 school year. A total of 61 out of 100 (61%) eligible residents volunteered to a structured training program involving communicating a perinatal loss to a simulated patient (SP) portraying the mother followed by the SP’s immediatefeedback,bothvideo recorded. Later, residents were randomly assigned to BBN training based on a setting, perception, invitation, knowledge, emotion and summary (SPIKES) strategy with video reviews (intervention) or no training (control group). All residents returned for a second simulation with the same SP blinded to the intervention and portraying a similar case. Residents’ performances were then evaluated by the SP with a checklist. The statistical analysis included a repeated measures analysis of covariance (RM-ANCOVA). Complementarily, the residents provided their perceptions about the simulation with feedback activities.
Fifty-eight residents completed the program. The simulations lasted on average 12 minutes, feedback 5 minutes and SPIKES training between 1h and 2h30m. There was no significant difference in the residents’ performances according to the SPs’ evaluations (p = 0.55). The participants rated the simulation with feedback exercises highly. These educational activities might have offset SPIKES training impact. Conclusion The SPIKES training did not significantly impact the residents’ performance. The residents endorsed the simulation with feedback as a useful training modality. Further research is needed to determine which modality is more effective.