Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(2):117-123
DOI 10.1590/S0100-72032004000200006
PURPOSE: to assess the natural pregnancy rates in rabbits submitted to bilateral oophorectomy and orthotopic autologous (both intact and sliced) ovarian transplantation without vascular pedicle and to verify the morphofunctional aspects of reimplanted ovaries. METHOD: thirty-two female New Zealand White rabbits were studied. The ovaries were removed and orthotopically replaced without vascular anastomosis. In the control group (GC) (n=8), only laparotomy was carried out. In the RI group (n=8) intact ovaries were reimplanted in both sides. In the RF group (n=8) the ovaries were sliced and orthotopically reimplanted. In the RIF group (n=8), in one side the intact ovary and in the other side the sliced ovary was reimplanted.Three months later, the animals were paired with sexually mature males for copulation. Estradiol, progesterone, follicle stimulating hormone and luteinizing hormone levels were assessed nine months after surgery. Histologic study of the transplanted ovaries, tubes and uteri was carried out, and the number of pregnancies and animals per litter in each group was taken into account as well. The chi² test compared the pregnancy and the litters between the groups. Student's t test compared the hormone determinations. Significance was set at p<0.05. RESULTS: pregnancies occurred in all rabbits of the GC, between the second and third months after copulation, with 6 to 10 animals per litter for animal. In the other groups, the pregnancies occurred between the fifth and eighth postoperative month. Pregnancies occurred in 37.5% of rabbits in group RI, and in 50% of the RF and RIF groups. There was no difference between the number of animals per litter in the reimplanted groups, with 1 to 4 animals per litter for each animal. Hormone levels and histology confirmed the vitality of all ovaries. CONCLUSIONS: intact or sliced orthotopic autologous ovarian transplantation without vascular pedicle is viable in rabbits, and preserves the hormonal and fertile functions.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(3):117-122
DOI 10.1590/S0100-72032013000300005
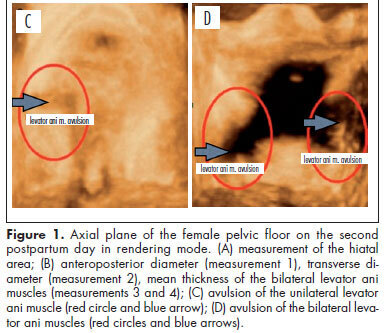
PURPOSE: To evaluate changes to the pelvic floor of primiparous women with different delivery modes, using three-dimensional ultrasound. METHODS: A prospective cross-sectional study on 35 primiparae divided into groups according to the delivery mode: elective cesarean delivery (n=10), vaginal delivery (n=16), and forceps delivery (n=9). Three-dimensional ultrasound on the pelvic floor was performed on the second postpartum day with the patient in a resting position. A convex volumetric transducer (RAB4-8L) was used, in contact with the large labia, with the patient in the gynecological position. Biometric measurements of the urogenital hiatus were taken in the axial plane on images in the rendering mode, in order to assess the area, anteroposterior and transverse diameters, average thickness, and avulsion of the levator ani muscle. Differences between groups were evaluated by determining the mean differences and their respective 95% confidence intervals. The proportions of levator ani muscle avulsion were compared between elective cesarean section and vaginal birth using Fisher's exact test. RESULTS: The mean areas of the urogenital hiatus in the cases of vaginal and forceps deliveries were 17.0 and 20.1 cm², respectively, versus 12.4 cm² in the Control Group (elective cesarean). Avulsion of the levator ani muscle was observed in women who underwent vaginal delivery (3/25), however there was no statistically significant difference between cesarean section and vaginal delivery groups (p=0.5). CONCLUSION: Transperineal three-dimensional ultrasound was useful for assessing the pelvic floor of primiparous women, by allowing pelvic morphological changes to be differentiated according to the delivery mode.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):117-117
DOI 10.1590/S0100-72032000000200010
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):117-117
DOI 10.1590/S0100-72032000000200011
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(3):117-119
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(3):118-121
DOI 10.1590/S0100-72032012000300005
PURPOSE: To report the use of colpotomy for the treatment of ectopic pregnancies. METHODS: This was a retrospective cross-sectional study conducted on all women hospitalized with a clinical-laboratory suspicion of ectopic pregnancy who did not fulfill the criteria for drug treatment with methothrexate, during the period from February 2007 to August 2008. Demographic variables, gynecologic history and characteristics associated with treatment were obtained by reviewing the medical records. RESULTS: Eighteen women were included in the study. Mean age was 27±5.2 years. All patients presented ruptured ectopic pregnancy and all were submitted to partial salpingectomy. Surgical time ranged from 30 to 120 minutes (mean: 64.5 minutes) calculated from the moment when the patient entered the operating room to the moment when she left it. No patient presented postoperative infection. Mean time of hospitalization was 40±14.3 hours. The medications used during the postoperative period were similar in all cases, being based on nonsteroid anti-inflammatory drugs, dipyrone, paracetamol and meperidine, as needed. The diet was reintroduced 8 hours after the end of surgery. CONCLUSIONS: The use of colpotomy in the treatment of ectopic pregnancy showed good results, with the absence of important complications and a short hospitalization time. The basic surgical instruments needed for this procedure are relatively common to all hospitals, and the surgical technique is reproducible.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(2):118-124
To assess the degree of correlation/agreement of maternal-fetal Doppler parameters between normal and growth-restricted fetuses (fetal growth restriction [FGR]).
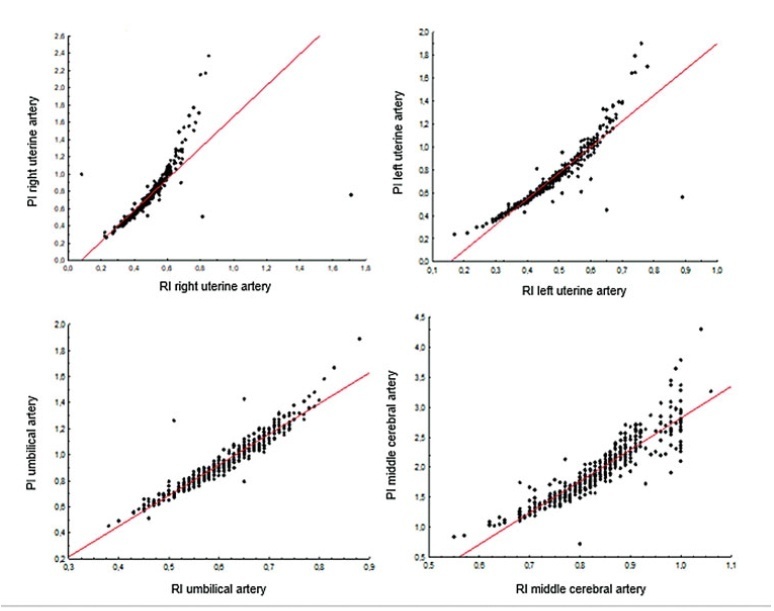
The present observational and retrospective study included 274 singleton pregnancies. The following maternal-fetal Doppler parameters were assessed: uterine artery (UAt), umbilical artery (UA), middle cerebral artery (MCA), cerebroplacental ratio (CPR), and umbilical-cerebral ratio (U/C). The assessment of FGR was based on the Figueiras and Gratacós9 criteria. Spearman correlation coefficients were estimated to assess the correlation between resistance (RI) and pulsatility (PI) indices of Doppler parameters. The agreement between two Doppler parameters was assessed by the Kappa coefficient.
In total, 502 Doppler examinations were included, and FGR was observed in 19 out of 274 fetuses. A strong correlation was observed between RI and PI of UAt, UA, and MCA in all of the samples (p<0.001). Of the 502 Doppler examinations, there was agreement between U/C and CPR percentiles for 480 (95.6%) and disagreement for 22 (4.4%), with Kappa coefficient of 0.26, thereby corresponding to weak agreement. Of the 68 cases with estimated fetal weight ≤ 9th percentile (small for gestational age [SGA]), there was agreement between U/C>1.0 and CPR<5th percentile in 61 (88.4%) and disagreement in 7 (5.8%) with Kappa coefficient of 0.49, thereby corresponding to moderate agreement.
Strong correlation was observed among RI and PI UAt, UA, and MCA Doppler examinations in the present study; however, weak agreement was observed between U/C and CPR in the normal and FGR fetuses. In SGA, U/C and CPR demonstrated moderate agreement.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(3):118-123
DOI 10.1590/S0100-72032014000300005
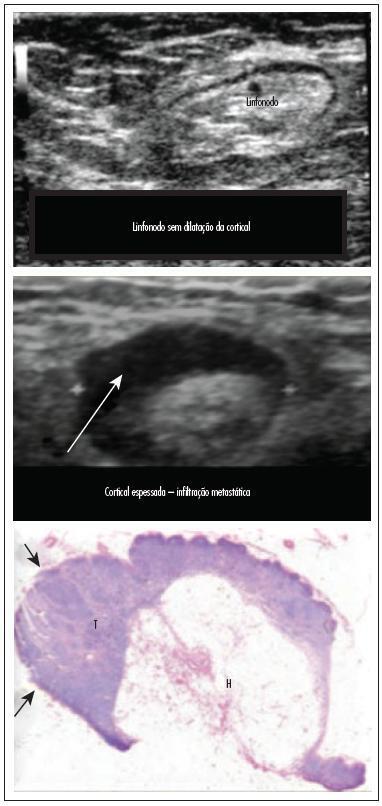
To assess the feasibility and diagnostic accuracy of preoperative ultrasound combined with ultrasound-guided fine-needle aspiration (US-FNA) cytology and clinical examination of axillary lymph node in patients with breast cancer.
In this prospective study, 171 axillae of patients with breast cancer were evaluated by clinical examination and ultrasonography (US) with and without fine needle aspiration (FNA). Lymph nodes with maximum ultrasonographic cortical thickness > 2.3 mm were considered suspicious and submitted to US-FNA.
Logistic regression analysis showed no statistically significant correlation between clinical examination and pathologically positive axillae. However, in axillae considered suspicious by ultrasonography, the risk of positive anatomopathological findings increased 12.6-fold. Cohen's Kappa value was 0.12 for clinical examination, 0.48 for US, and 0.80 for US-FNA. Accuracy was 61.4% for clinical examination, 73.1% for US and 90.1% for US-FA. Receiver Operating Characteristics (ROC) analysis demonstrated that a cortical thickness of 2.75 mm corresponded to the highest sensitivity and specificity in predicting axillary metastasis (82.7 and 82.2%, respectively).
Ultrasonography combined with fine-needle aspiration is more accurate than clinical examination in assessing preoperative axillary status in women with breast cancer. Those who are US-FNA positive can be directed towards axillary lymph node dissection straight away, and only those who are US-FNA negative should be considered for sentinel lymph node biopsy.