Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(11):622-631
Preeclampsia, a multifactorial disease with pathophysiology not yet fully understood, is a major cause of maternal and perinatal morbidity and mortality, especially when preterm. The diagnosis is performed when there is an association between arterial hypertension and proteinuria or evidence of severity. There are unanswered questions in the literature considering the timing of delivery once preterm preeclampsia has been diagnosed, given the risk of developingmaternal complications versus the risk of adverse perinatal outcomes associated with prematurity. The objective of this systematic review is to determine the best timing of delivery for women diagnosed with preeclampsia before 37 weeks of gestation.
Systematic literature review, performed in the PubMed database, using the terms preeclampsia, parturition and timing of delivery to look for studies conducted between 2014 and 2017. Studies that compared the maternal and perinatal outcomes of women who underwent immediate delivery or delayed delivery, in the absence of evidence of severe preeclampsia, were selected.
A total of 629 studies were initially retrieved. After reading the titles, 78 were selected, and their abstracts, evaluated; 16 were then evaluated in full and, in the end, 6 studies (2 randomized clinical trials and 4 observational studies) met the inclusion criteria. The results were presented according to gestational age range (< 34 weeks and between 34 and 37 weeks) and by maternal and perinatal outcomes, according to the timing of delivery, considering immediate delivery or expectant management. Before 34 weeks, thematernal outcomeswere similar, but the perinatal outcomes were significantly worse when immediate delivery occurred. Between 34 and 37 weeks, the progression to severe maternal disease was slightly higher among women undergoing expectant management, however, with better perinatal outcomes.
When there is no evidence of severe preeclampsia or impaired fetal wellbeing, especially before 34 weeks, the pregnancy should be carefully surveilled, and the delivery, postponed, aiming at improving the perinatal outcomes. Between 34 and 37 weeks, the decision on the timing of delivery should be shared with the pregnant woman and her family, after providing information regarding the risks of adverse outcomes associated with preeclampsia and prematurity.

Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(12):623-628
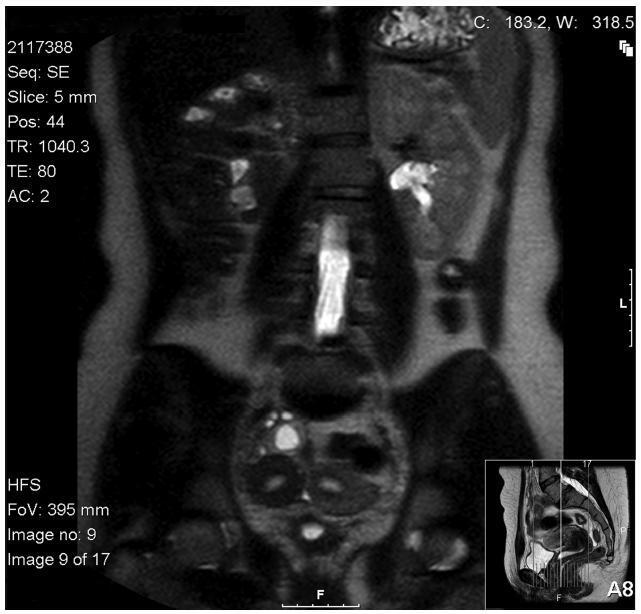
We describe a Herlyn-Werner-Wunderlich syndrome (HWWS) patient with previous history of infertility who got pregnant without treatment and presented a pyometra in the contralateral uterus throughout the gestational period, despite multiple antibiotic treatments. Due to the uterus' congenital anomaly and the possibility of ascending infection with subsequent abortion, this pregnancy was classified as high-risk. We believe that the partial horizontal septum in the vagina may have contributed to the closure of the gravid uterus cervix, thus ensuring that the pregnancy came to term, with an uneventful vaginal delivery.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(9):623-623
Summary
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(12):625-632
DOI 10.1590/S0100-72032007001200005
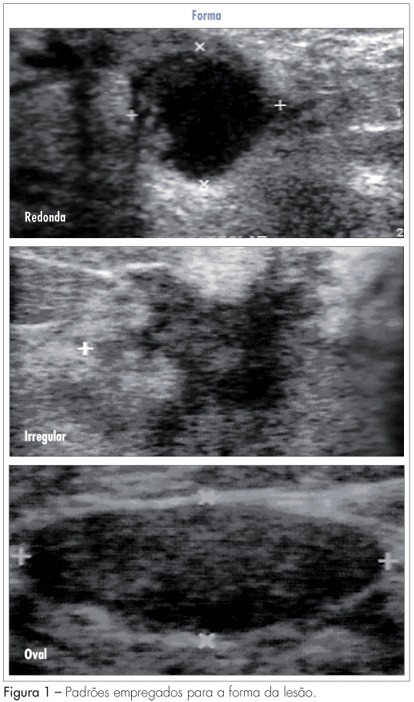
PURPOSE: to analyze which characteristics proposed by the BIRADS lexicon for ultrasound have the greatest impact on distinguishing between benign and malignant lesions. METHODS: ultrasonography features from the third edition of the BIRADS were studied in 384 nodes submitted to percutaneous biopsy from February 2003 to December 2006, at the Medical School of Botucatu. For the ultrasonography, the equipment Logic 5 with a 7.5-12 MHz multifrequential linear transducer was used. The ultrasonography analysis of the node considered the features proposed by the BIRADS lexicon for ultrasound. The data were submitted to statistical analysis by the logistic regression model. RESULTS: the benign lesions represented 42.4% and the malignant, 57.6%. The logistic regression analysis found an odds ratio (OR) for cancer of 7.69 times when the surrounding tissue was altered, of 6.25 times when there were microcalcifications in the lesions interior, of 1.95 when the acoustic effect is shadowing, of 25.0 times when there was the echogenic halo, and of 7.14 times when the orientation was non-parallel. CONCLUSIONS: among the features studied, the lesion limit, represented by the presence or not of the halogenic halo, is the most important differentiator of the benign from the malignant masses.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(10):625-625
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(10):625-625
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(9):625-630
DOI 10.1590/S0100-72032003000900002
PURPOSE: to evaluate the nutritional condition of pregnant adolescents using the pregestational body mass index (BMI) and the BMI at the end of pregnancy and to establish a possible association with the type of delivery and weight of the newborn child. METHODS: in a descriptive retrospective observational study 558 pregnant teenagers as well as their newborns were evaluated in the Obstetrics outpatient clinic of the Universidade Federal de São Paulo, Brazil (UNIFESP-EPM), from January 1998 to December 2000. The sample consisted of pregnant girls who were between 10 and 19 years old at the time of the first prenatal examination, excluding the teenagers who had preexistent disease and those with incomplete data in their records. Thus, the sample consisted of 300 pregnant teenagers. Qualitative variables are presented as absolute and relative frequency and quantitative variables as mean, standard deviation and range. The correlation between maternal variables (pre-pregnancy BMI and final BMI) and parameters of the newborn (type of delivery and weight) was determined by the c² test and the differences were identified by partitioning of the c² values, with the level of significance set at p < 0.05 (a = 0.05). RESULTS: nutritional deviation was detected in 34.7% of the girls, at the beginning of pregnancy. Of these adolescents, 27.7% presented malnutrition, 4% were overweight and 3% were obese. By the end of the gestational period, BMI of 54.3% of them was normal, 1.3% correponded to malnutrition, 27% to overweight and 17.3% to obesity. The mother's nutritional condition (malnutrition, normal, overweight and obesity) did not affect the method of delivery, either vaginal (80.3%) or cesarean section (19.7%). The patients who reached end of pregnancy with BMI corresponding to malnutrition had 75% of neonates under 2.500 g. CONCLUSIONS: the mother's nutritional status was not related to the type of delivery. BMI corresponding to malnutrition at the end of pregnancy was significantly related to more cases of newborn babies under 2.500 g.