You searched for:"Edward Araujo Júnior"
We found (57) results for your search.Summary
Rev Bras Ginecol Obstet. 2016;38(4):189-195
Previous studies have shown that low birth weight (LBW) is associated with cardiovascular risk in late adulthood. Recent studies in adolescents suggest that modifiable factors may have greater influence on increased cardiovascular risk. This study aims to investigate the association between LBW and changes in anthropometric and biochemical risk factors during adolescence in a population with low average socioeconomic status.
In a retrospective double cohort, data of birth weight were extracted from hospital records of children born on the same day between 1992 and 2002. According to the World Health Organization, we classified the children as having LBW or normal birth weight. A total of 172 subjects among children, adolescents and adults were researched. We measured anthropometric and clinical data, lipid profile and glucose after an overnight fasting. The low and normal weight groups were compared using Mann-Whitney U, Fischer exact, Chi-square (2) and Student's t tests.
Pregnant women with preeclampsia delivered more newborns with LBW (p< 0.001). Anthropometric and clinical parameters were similar between groups. No differences were found in the family history of cardiovascular diseases (p= 0.1), family incomes (p= 0.8) and maternal school education (p= 0.8) between groups.
In this study, LBW did not increase cardiovascular disease risk factors in adolescents. We observed absence of association between low birth weight and poor health outcomes among adolescents with low socioeconomic status from an urban city in the Brazilian northeast.
Summary
Rev Bras Ginecol Obstet. 2014;36(5):189-191
DOI 10.1590/S0100-7203201400050001
Summary
Rev Bras Ginecol Obstet. 2008;30(4):190-195
DOI 10.1590/S0100-72032008000400006
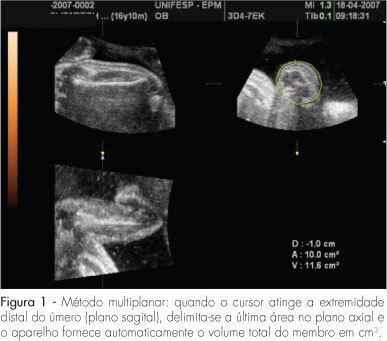
PURPOSE: to evaluate the accuracy of fetal upper arm volume, using three-dimensional ultrasound (3DUS), in the prediction of birth weight. METHODS: this prospective cross-sectional study involved 25 pregnancies without structural or chromosomal anomalies. Bidimensional parameters (biparietal diameter, abdominal circumference and femur length) and the 3DUS fetal upper arm volume were obtained in the last 48 hours before delivery. The multiplanar method, using multiple sequential planes with 5.0-mm intervals, was used to calculate fetal upper arm volume. Polynomial regressions were used to determine the best equation in the prediction of fetal weight. The accuracy of this new formula was compared with Shepard's and Hadlock's formulas. RESULTS: fetal upper arm volume was strongly correlated to birth weight (r=0.83; p<0.005). Linear regression was the best equation [birth weight=681.59 + 43.23 x fetal upper arm volume]. The fetal upper arm volume mean error (0 g), mean absolute error (196.6 g) and mean percent absolute error (6.5%) were lower than using Shepard's formula; however, the difference did not reach significance (p>0.05). Birth weight predicted by fetal upper arm volume had a mean error lower than Hadlock's formula, but this difference was not statistically significant (p>0.05). CONCLUSIONS: the accuracy of fetal upper arm volume obtained through 3DUS is similar to the accuracy of bidimensional ultrasound in the prediction of birth weight. These findings need to be confirmed by larger studies.
Summary
Rev Bras Ginecol Obstet. 2012;34(5):191-195
Summary
Rev Bras Ginecol Obstet. 2016;38(4):201-206
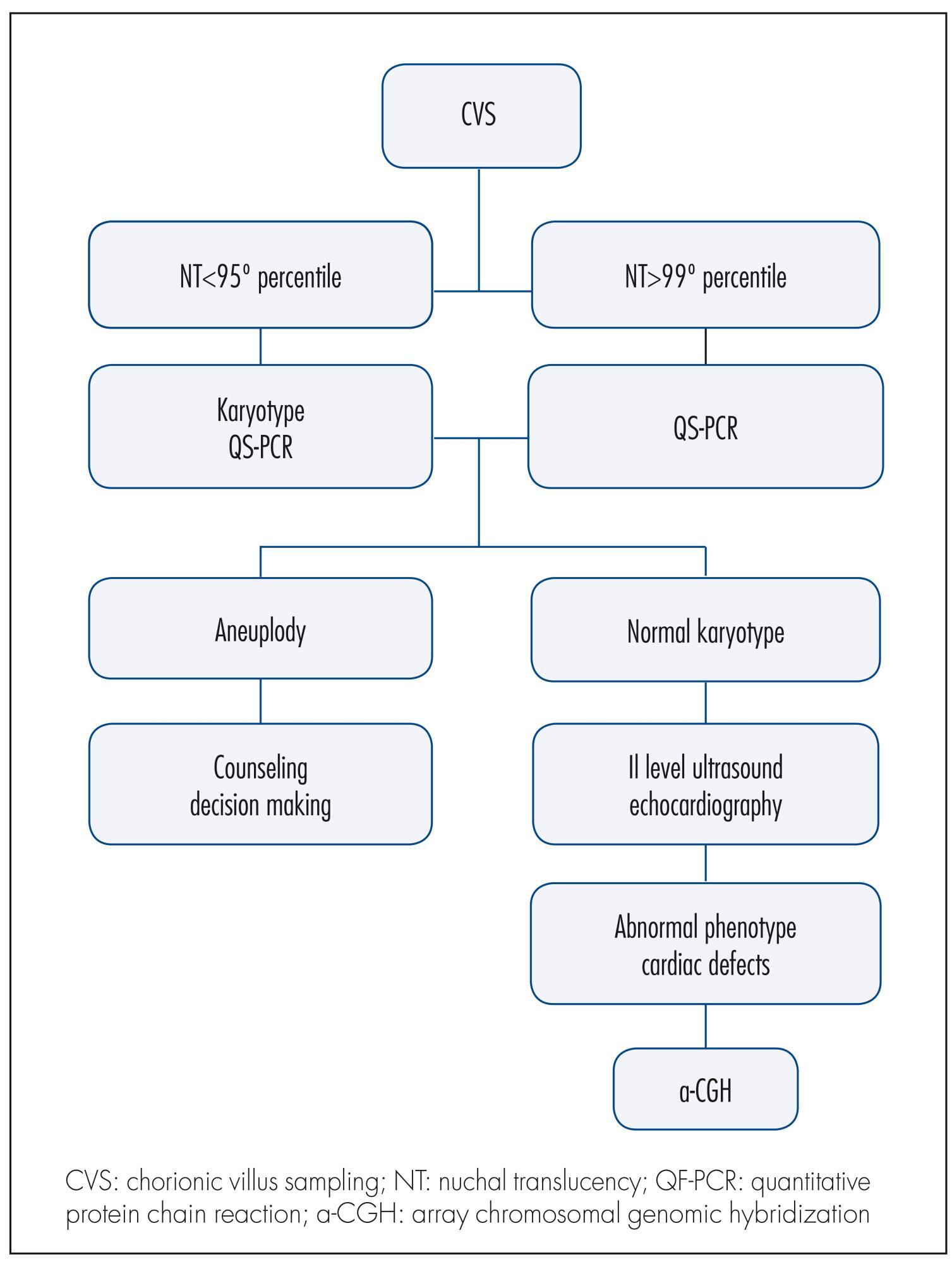
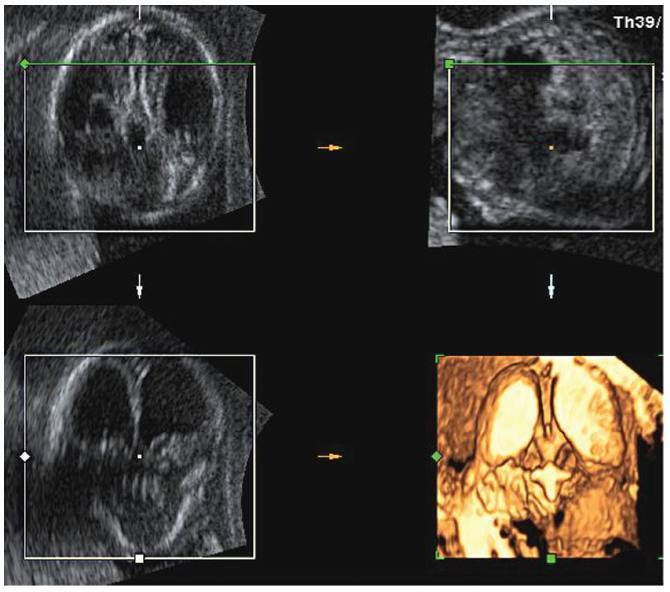
Lissencephaly is a genetic heterogeneous autosomal recessive disorder characterized by the classical triad: brain malformations, eye anomalies, and congenital muscular dystrophy. Prenatal diagnosis is feasible by demonstrating abnormal development of sulci and gyri. Magnetic resonance imaging (MRI) may enhance detection of developmental cortical disorders as well as ocular anomalies. We describe a case of early diagnosis of lissencephaly type 2 detected at the time of routine second trimester scan by three-dimensional ultrasound and fetal MRI. Gross pathology confirmed the accuracy of the prenatal diagnosis while histology showed the typical feature of cobblestone cortex. As the disease is associated with poor perinatal prognosis, early and accurate prenatal diagnosis is important for genetic counseling and antenatal care.
Summary
Rev Bras Ginecol Obstet. 2021;43(3):216-219
To evaluate the seroprevalence of positive markers for syphilis, human immunodeficiency virus (HIV) I and II, human T cell lymphotropic virus (HTLV) I and II, and hepatitis B and C among women undergoing in vitro fertilization (IVF).
We conducted a retrospective analysis among patients who underwent IVF, between January 2013 and February 2016, and who had complete screening records.
We analyzed 1,008 patients who underwent IVF, amounting to 2,445 cycles. Two patients (0.2%) tested positive for HIV I and II and none for HTLV I and II. Three patients (0.3%) had positive screening for syphilis, and two (0.2%) had positive hepatitis C antibody test (anti-HCV). A positive hepatitis B virus surface antigen (HbsAg) test was observed in 4 patients (0.4%), while 47 (4.7%) patients were positive for IgG antibody to hepatitis B core antigen (anti-HbC IgG), and only 1 (0.1%) was positive for IgM antibody to hepatitis B core antigen (anti-HbC IgM). The anti-HbS test was negative in 659 patients (65.3%). Only 34.7% of the patients had immunity against the Hepatitis B virus. Patients with an anti-HbS negative result were older than those with a hepatitis B test (anti-HbS) positive result (36.3 versus 34.9; p<0.001).
The present study showed lower infection rates than the Brazilian ones for the diseases studied in patients undergoing IVF. Only a few patients were immunized against hepatitis B.
Summary
Rev Bras Ginecol Obstet. 2001;23(4):217-221
DOI 10.1590/S0100-72032001000400004
Purpose: to evaluate the influence of pregnancy, habit of smoking, and the contraceptive method in HPV infection and the frequency of cytologic findings in adolescent women with HPV infection. Methods: a total of 54,985 cytologic examinations of patients seen between July, 1993 and December, 1998 were retrospectively analyzed. Of this total, 6,498 (11.8%) examinations were from patients under 20 years old. Of the total of 6,498 cytologic examinations, 326 (5.9%) presented signs of HPV infection, with or without grade I cervical intraepithelial neoplasia (CIN). Patients with diagnosis of grade II and III CIN were excluded. The control group consisted of 333 patients paired by age, without cytological signs of HPV infection. Results: in adolescents, HPV infection was more frequent in oral contraceptive users (16.9% versus 13.8%, p<0.01) and in those who presented with clue cells in cytologic smears (22.4% versus 14.7%, p<0.001). The frequency of HPV infection in couples who used condom was 0% versus 2.1% in the control group (p<0.01). The difference in the number of pregnant women (41.1% versus 44.1%) and smokers (21.8% versus 16.5%) was not statistically significant. Conclusions: HPV infection is more frequent in adolescent women in use of oral contraceptive and with clue cells as cytologic finding. HPV infection did not occur in couples who used condom. Gestation and the habit of smoking did not influence the incidence of HPV infection.
Summary
Rev Bras Ginecol Obstet. 2014;36(5):222-227
DOI 10.1590/S0100-7203201400050007
To identify risk factors for weight retention in women after childbirth.
This was a prospective observational study that followed for six months adult women who delivered at a tertiary center. Were applied a structured questionnaire before hospital discharge and at six weeks and six months after childbirth, through home visits. The outcome was weight retention after childbirth (if risk >7.5 kg). The variables analyzed were: age, skin color, working during pregnancy, income, education, marital status, age at menarche, maternal age at first birth, parity, mode of delivery, birth interval, pre-pregnancy weight, gestational weight gain, percent body fat, and nutritional status. Data were first analyzed by bivariate analysis between prevalence of weight retention at six months and several covariates (p<0.2). We then calculated the Odds Ratio (OR) and their respective gross confidence intervals of 95% (95%CI) and finally performed multivariate logistic regression to control for confounding factors and to estimate the OR and 95%CI.
The frequency of weight retention >7.5 kg by 6 months after delivery was 15%. In bivariate analysis, weight retention was associated with the following variables: age at menarche <12 years (OR=3.7; 95%CI1.1-13.2), gestational weight gain ≥16 kg (OR=5.8; 95%CI 1.8-18.6), percent body fat at baseline >30% (OR=5.0; 95%CI 1.1-23.6), and nutritional status by 6 weeks postpartum >25 kg/m2 (OR=7.7; 95%CI1.6-36.1). In multivariate analysis, only excessive gestational weight gain (OR=74.1; 95%CI 9.0-609.6) remained as a risk factor.
Excessive weight gain during pregnancy should receive special attention in prenatal care in view of its association with weight retention and excess weight in women after childbirth.