You searched for:"Antonio Fernandes Moron"
We found (33) results for your search.Summary
Rev Bras Ginecol Obstet. 2004;26(5):349-354
DOI 10.1590/S0100-72032004000500002
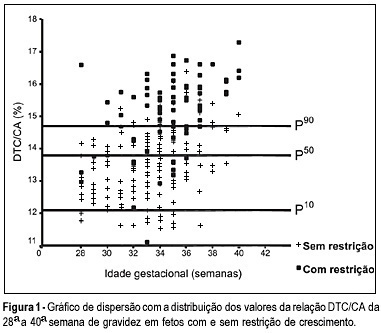
OBJECTIVE: to evaluate the accuracy of both the transverse diameter of the cerebellum (TDC) and of the transverse diameter/abdominal circumference (TDC/AC) ratio in the detection of fetal growth restriction (FGR), in high-risk pregnancies. METHOD: a prospective cross-sectional study was carried out in 260 patients with gestational age between 28 and 40 weeks. The TDC and AC of fetuses were measured through ultrasound and the fetuses with TDC below the 10th percentile or TDC/AC ratio above the 90th percentile (>14.6) were classified as FGR suspects. After birth, the accuracy of the TDC and TDC/AC was evaluated using the neonatal diagnosis of FGR as the gold standard (birth weight <10th percentile). RESULTS: after birth, 79 newborns (30.4%) were classified as small for gestational age. The TDC was appropriate in 74 (93.7%) of these fetuses and small in only 5 (6.3%). The sensitivity (SE), specificity (SP), positive (PPV) and negative (NPV) predictive values and accuracy of the TDC in the prediction of FGR were 6.3, 93.4, 29.4, 69.5, and 67%, respectively. The TDC/AC >14.6 correctly identified 59 of the 79 growth-restricted fetuses, with 27 false-positives and 20 false-negatives, SE of 74.5%, SP of 85.1%, PPV of 68.6%, NPV of 88.5% and 81.9% accuracy. CONCLUSION: the TDC is not a good screening parameter for the detection of FGR while the TDC/AC ratio above the 90th percentile is effective in this detection.
Summary
Rev Bras Ginecol Obstet. 1999;21(7):371-376
DOI 10.1590/S0100-72031999000700002
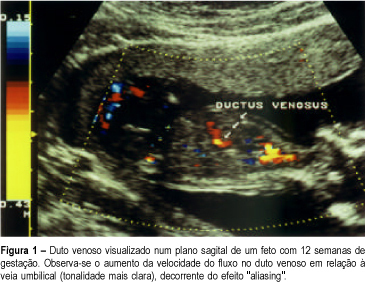
Purpose: to evaluate the possible value of pulsed and color Doppler of ductus venosus blood flow in the screening for chromosomal abnormalities at 10-14 weeks of gestation. Methods: the ductus venosus flow velocity waveforms and the nuchal translucency (NT) thickness were obtained immediately before the chorionic villus sample in 26 pregnancies. We employed the following criteria for the suspicion of chromosomal defects: reverse or absent flow during atrial contraction and NT greater or equal to 3 mm. We calculated the sensitivity, the specificity, the negative and positive predictive value for each of the above items. Results: there were 9 chromosomal abnormalities (3 cases of trisomy 21, 2 cases of trisomy 13, 1 case of trisomy 9, 1 case of trisomy 22, 1 triploidy and 1 monosomy X). Abnormal ductus venosus flow was observed in all cases (sensitivity of 100%). In the normal fetuses (17 cases) only 1 had abnormal flow (specificity of 94%). Concerning NT, the sensitivity and the specificity were 88% and 76%, respectively. Conclusion: our preliminary results suggest that the presence of chromosomal abnormalities may be strongly suspected when an increased NT thickness is associated with an absent or reverse flow in the ductus venosus. We speculated that both methods are valid in the screening of chromosomal defects.
Summary
Rev Bras Ginecol Obstet. 2006;28(7):397-402
DOI 10.1590/S0100-72032006000700004
PURPOSE: to compare the uterine cervix measurements and funneling obtained by two- and three-dimensional transvaginal sonography during pregnancy. METHODS: a prospective, descriptive study, with group comparison, was carried out between April 2004 and February 2005 in 74 pregnant women, who were between the 19th and 24th week of pregnancy, regardless of risk factors for premature delivery. The ultrasound examination of the cervix was carried out only once in the same patient and by only one observer. The measurements of the cervix by two-dimensional ultrasound were made at the time of the test and by three-dimensional ultrasound at intervals of 7 to 15 days after the two-dimensional ultrasound. The measurements of cervical length, funnel width and length were taken by two-dimensional ultrasound in the sagittal plane and by three-dimensional in the sagittal plane as well as in coronal plane. RESULTS: there was no significant difference between the averages of the measurements of the cervix obtained by two- and three-dimensional ultrasound in the sagittal plane (p=0.23); however, there was a difference in the averages of the measurements of the cervix obtained by two-dimensional ultrasound in sagittal plane and three-dimensional ultrasound in the coronal plane (p=0.009) and between three-dimensional ultrasound in the sagittal and coronal planes (p=0.001). The kappa test (0.86) showed no superiority of either the two-dimensional and three-dimensional ultrasound in the visualization of the cervical funnel. No statistically significant difference was observed between the methods when the average of the measurements of funneling was compared (p>0.05). CONCLUSION: there were differences between two-dimensional and three-dimensional ultrasound of cervical length, only using the coronal plane of the three-dimensional ultrasound.
Summary
Rev Bras Ginecol Obstet. 2001;23(7):417-422
DOI 10.1590/S0100-72032001000700002
Purpose: to investigate risk factors associated with accretion in placenta previa (PP) patients. Methods: this was a retrospective case-control study of all the records of patients who delivered between 1986-1998 at Maternidade Escola de Vila Nova Cachoeirinha (São Paulo) with a diagnosis of placenta previa. The groups with and without accretion were compared regarding age, parity, previous history of miscarriage, curettage and cesarean section, type of PP and predominant area of placental attachment. Possible associations between the dependent (accretion) and independent (maternal and placental characteristics) variables were evaluated using the chi² test, univariate and multivariate analyses. Results: reviewing 245 cases of PP, two risk factors were significantly associated with accretion: central placenta previa (odds ratio (OR): 2.93) and two or more previous cesarean sections(OR: 2.54). Based on these data, a predictive model was constructed, according to which a patient with central PP and two more previous cesarean sections has a 44.4% risk for accretion. Conclusions: results of the current study may help obstetricians in the classification of their patients with PP in different risk categories for accretion. This could be useful in preparing for possible delivery complications in those patients considered at a higher risk for accretion.
Summary
Rev Bras Ginecol Obstet. 2003;25(6):425-430
DOI 10.1590/S0100-72032003000600007
PURPOSE: to determine whether prenatal sonographic findings and uterine contractions can predict neonatal motor outcome in fetuses with open spina bifida. METHODS: we evaluated retrospectively 53 fetuses with open spina bifida from 1993 to 2001. These fetuses were born and followed-up at the fetal medicine units of the Hospital São Paulo ("Universidade Federal de São Paulo") and the "Hospital Santa Joana". The influence of the alterations observed through ultrasound scan on neonatal muscular strength (macrocrania, microcrania, level of the spinal column opening, clubfoot and type of fetus position) was evaluated. The influence of uterine contractions on neonatal motor outcome was also evaluated. All deliveries were made through cesarian section. c² and Fisher tests were used for categorical comparisons. A p<0.05 was considered significant. RESULTS: Fifty-three cases of isolated open spina bifida were studied. Alterations of the cranial circumference size and the level of the lesion did not interfere in the neonatal motor perfomance. However, clubfoot and breech position showed to be predictors of an unfavorable neurological prognosis (p<0.05). Twenty-tree (43%) infants had clubfoot. Eighteen (78.3%) of these had abnormal leg movements. No infant in breech presentation (n=10) showed normal motor function. The presence of uterine contractions and the premature membrane rupture, observed in 13 fetuses (87%), were also linked to the alteration of neonatal muscular strength (p<0.05). CONCLUSION: clubfoot and breech presentation are ultrasonographic findings useful in predicting neurological neonatal outcome. Uterine contractions and premature membrane rupture are associated with poor motor neonatal outcome.
Summary
Rev Bras Ginecol Obstet. 2010;32(9):426-432
DOI 10.1590/S0100-72032010000900003
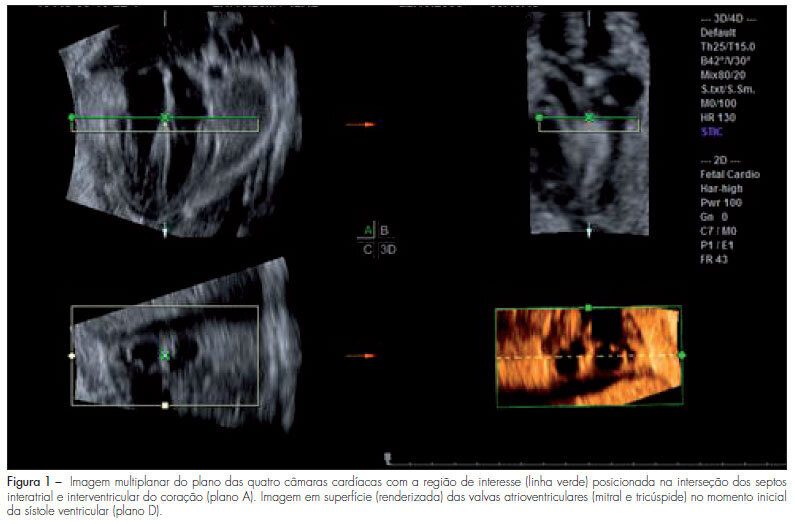
PURPOSE: to evaluate the areas of the atrioventricular valves (tricuspid and mitral) of normal fetuses by the use of three-dimensional ultrasound (3DUS) and the spatiotemporal image correlation (STIC) method. METHODS: a cross-sectional study was conducted on 141 women between the 18th and the 33rd week of pregnancy. Cardiac volumes were measured with a volumetric transabdominal transducer attached to the Voluson 730 Expert equipment. The four chamber plane was used as reference, with the region of interest (ROI) positioned from the ventricles, and the area of the valves was obtained manually. To determine the correlation of the areas with gestational age, scatter plots were constructed and the Pearson correlation coefficient (r) was calculated. Means, medians, standard deviations (SD) and maximum and minimum values were calculated. The simple linear regression model was used to determine reference ranges of valve areas according to the gestational age by the Altman method, with the level of significance set at p<0.05. To calculate the intraobserver reproducibility, we used the intraclass correlation coefficient (ICC) and the Bland-Altman graph. RESULTS: the mitral and tricuspid valve areas were correlated to the gestational age (r=0.80 for the tricuspid and r=0.79 for the mitral valve) and the mean value of the tricuspid and mitral valves increased from 0.22±0.10 cm² and 0.23±0.10 cm² on the 18th week to 0.92±0.29 cm² and 1.08±0.41 cm² on the 33rd of pregnancy, respectively. The intraobserver reproducibility resulted in an ICC=0.993 (95%CI 0.987; 0.996) and the mean difference was 0.01 cm² (SD±0.2 cm² and CI95%±0.4 cm²). CONCLUSION: reference intervals for the areas of the mitral and tricuspid valve between the 18th and the 33rd week of gestation were determined and proved to be highly reproducible.
Summary
Rev Bras Ginecol Obstet. 1998;20(8):449-453
DOI 10.1590/S0100-72031998000800004
Purpose: to determine folate, vitamin B12 and ferritin levels in patients whose fetuses presented neural-tube defects (NTD). Blood folate and vitamin B12 act as cofactors of enzymes involved in DNA biosynthesis. Interruption of this process may block neural-tube closing. Vitamin supplementation with folate may reduce occurrence rates and recurrence of NTD, although there is concern about the fact that this prevention may mask vitamin B12 deficiency. Methods: vitamin B12 and ferritin determinations by enzyme immunoassay with microparticles and folic acid determination using the ion capture method (IMx ABBOTT). Results: the percentage of pregnant women with vitamin B12 deficirncy (serum levels < 150 pg/ml) was 11.8%. There was no case of folate deficiency (serum levels < 3.0 ng/ml) and prevalence of pregnant women with iron store deficiency was 47.1% (serum levels < ng/mg). Conclusions: occording to the results obtained in this study (prevalence of 11.8% of vitamin B12 and 0% of folate deficient pregnant women) we suggest that supplementation should be administered after serum vitamin B12 determination.
Summary
Rev Bras Ginecol Obstet. 2003;25(7):475-479
DOI 10.1590/S0100-72032003000700003
PURPOSE: to study the effects of low-dose oral hormonal contraceptives (OHC) (<30 mg of ethynylestradiol) on the intraerythrocytic folate levels. METHODS: this was a prospective transversal study with 95 patients treated in the Family Planning Clinic of UNIFESP (Federal University of São Paulo). The control group (Condom group) consisted of patients using condom as their exclusive contraceptive method during the last 12 months, and the study groups consisted of patients using low-dose oral hormonal contraceptives, in the following way: OHC 3 group (three to six months of use), OHC 6 group (six to twelve months of use) and OHC 12 group (more than twelve months of use). Intraerythrocytic folate was determined by the ionic capture method. Analysis of variance and c² test were used for statistical analysis. RESULTS: the Condom group showed a rate of 44% of patients with folate lower than 186.0 ng/mL and the users of low-dose oral contraceptives showed a rate of 32% (OHC 3 group), 16% (OHC 6 group) and 31% (OHC 12 group). We did not find in the group using low-dose oral contraceptives a significant reduction in the average level of intraerythrocytic folate compared to the control group and there was no statistically significant difference (p=0.28) regarding time of use. CONCLUSION: we observed reduced levels of intraerythrocytic folate in a significant number (44%) of patients not using low-dose oral hormonal contraceptives. Their rates were similar to the lower limit considered to be normal by most authors, which points to a basal folate deficiency in the studied group. We did not observe any alteration in the level of intraerythrocytic folate in patients using low-dose oral hormonal contraceptives.