Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(11):498-504
DOI 10.1590/SO100-720320150005286
To evaluate the risk factors for morbidity and mortality in an obstetric intensive care unit at a university hospital.
Observational cross-sectional study with 492 pregnant/puerperal women. Patients were admitted to the obstetric intensive care unit over a period of one year, being informed about the proposals of the study and a questionnaire was applied. The analysis was performed using Microsoft Excel 2013 and GraphPad Prism 6. To evaluate risk factors, χ2 tests were used.
The main risk factors to near miss were: non-white race (OR=2.5; PR=2.3); marital status (married women) (OR=7.9; PR=7.1), schooling (primary) (OR=3.1; PR=2.8), being from the countryside (OR=4.6; PR=4.0), low income (OR=70; PR=5.5), gestational hypertensive disorders (OR=16.3; PR=13.2), receiving prenatal care (OR=5.0; PR=4.254) and C-section before labor (OR=39.2; PR=31.2).
The prevalence of near miss was associated with socioeconomic/clinical factors and care issues, revealing the importance of interventions to improve these indicators. Additionally, we suggest a better curriculum insertion of this subject in the discipline of the medical course due to the importance of avoiding the near miss using adequate medical education. The importance of correct prenatal care is emphasized in order to identify potential risks, to provide nutritional support to pregnant women, to treat potential diseases and to establish a maternal immunization program, as well as providing better care regarding the clinical features of the patients, in order to reduce obstetrical and neonatal risk.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(10):499-503
DOI 10.1590/S0100-72032008001000004
PURPOSE: to evaluate the embryo's volume (EV) between the seventh and the tenth gestational week, through tridimensional ultrasonography. METHODS: a transversal study with 63 normal pregnant women between the seventh and the tenth gestational week. The ultrasonographical exams have been performed with a volumetric abdominal transducer. Virtual Organ Computer-aided Analysis (VOCAL) has been used to calculate EV, with a rotation angle of 12º and a delimitation of 15 sequential slides. The average, median, standard deviation and maximum and minimum values have been calculated for the EV in all the gestational ages. A dispersion graphic has been drawn to assess the correlation between EV and the craniogluteal length (CGL), the adjustment being done by the determination coefficient (R²). To determine EV's reference intervals as a function of the CGL, the following formula was used: percentile=EV+K versus SD, with K=1.96. RESULTS: CGL has varied from 9.0 to 39.7 mm, with an average of 23.9 mm (±7.9 mm), while EV has varied from 0.1 to 7.6 cm³, with an average of 2.7 cm³ (±3.2 cm³). EV was highly correlated to CGL, the best adjustment being obtained with quadratic regression (EV=0.2-0.055 versus CGL+0.005 versus CGL²; R²=0.8). The average EV has varied from 0.1 (-0.3 to 0.5 cm³) to 6.7 cm³ (3.8 to 9.7 cm³) within the interval of 9 to 40 mm of CGL. EV has increased 67 times in this interval, while CGL, only 4.4 times. CONCLUSIONS: EV is a more sensitive parameter than CGL to evaluate embryo growth between the seventh and the tenth week of gestation.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(8):499-504
DOI 10.1590/S0100-72032001000800004
Purpose: to evaluate factors that might influence the results of nonphamacological treatment (verbal guidance) in women with clinical mastalgia. Methods: an uncontrolled study of the experimental type was conducted on a sample of 128 women with a clear history of clinical mastalgia treated with verbal guidance. A visual analogue scale for pain was used before and after treatment to evaluate pain intensity and mastalgia was classified into grade I (mild), grade II (moderate) and grade III (severe) according to pain intensity. The Cardiff Breast Score (CBS), modified, was also used to evaluate the clinical response to treatment. Data were analyzed statistically using the chi² test (Epi-Info 6.04). Results: we noted that factors such as parity, menarche, age at first term delivery and breast-feeding had no significant effect (p=0.19, p=0.31, p=0.80 and p=0.54, respectively) on the results of nonpharmacological treatment (verbal guidance). On the other hand, when age was taken into consideration, 26 patients (78.8%) aged 40 years or older were found to benefi more from verbal guidance, with a significant difference (p=0.01) when compared to younger women. Conclusion: reproductive factors such as parity, menarche, age at first term delivery and breast-feeding did not affect the results of nonpharmacological treatment (verbal guidance), whereas the age factor had a specific and significant effect on the results.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(9):499-504
DOI 10.1590/S0100-72031999000900002
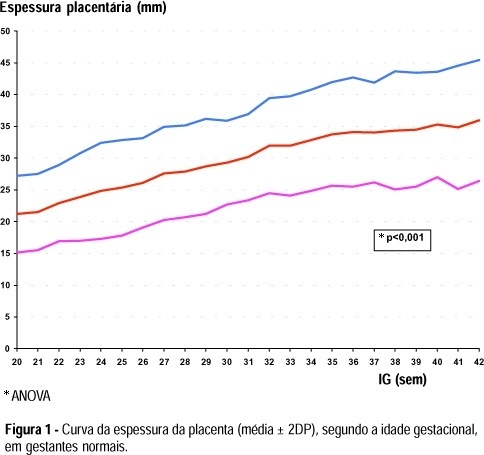
Purpose: to evaluate the ultrasound characteristics of normal pregnancies, according to the placental maturity, local of insertion and thickness, fetal presentation and position during the second half of pregnancy. Methods: a descriptive study was perfomed, including at least 120 measures in each gestational age, in 2,868 normal pregnant women from Campinas, Brazil, studied through routine obstetric ultrasound examinations, with fetal biometry and placental evaluation, applying Grannum, Berkowitz, Hobbins (1979) criteria for placental maturity. Placental thickness was measured at the cord insertion site. Results: grade 0 placentas were more frequent up to 31 weeks and grade I after 32 weeks. Grade II did not appear until 32 weeks and grade III was more frequent after 36 weeks. The placental thickness significantly increased with gestational age and the most frequent placental locations were anterior and posterior. The cephalic presentation was the most frequent all gestational ages, with only 1% of breech presentation at term. The most frequent fetal position was fetal spine left side, followed by right side. Conclusions: the studied factors showed a similar distribution to that expected for normal populations and could be used as a standard for the Brazilian population.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(8):499-499
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(10):499-505
To identify which methods used in the assessment of the ovarian reserve are exclusive or complementary to identify the best response to follicle development.
Retrospective cohort study, involving patients undergoing assisted reproduction treatment at the Instituto de Medicina Reprodutiva e Fetal, from April 2009 to July 2014. Age, biochemical tests, and ultrasound were assessed. The data were analyzed to predict the follicular development and the relation between them, using, for statistical analysis, Statistical Package for Social Sciences software.
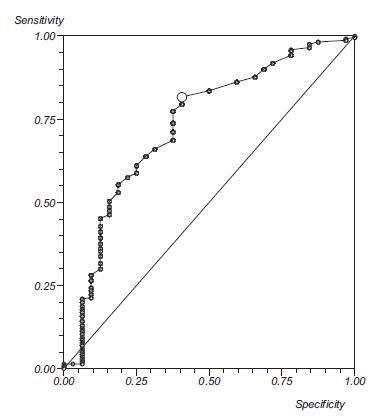
Out of the 293 couples included, 50.2% presented infertility by ovarian factor. Considering the age as the main variable, a significant negative correlation with the volume of both ovaries was observed (right ovary, r = 0.21; left ovary, r =0.22; both p< 0.0001), and with the antral follicle count (right ovary, r =0.38; left ovary, r =0.47; both p< 0.0001). Considering the antral follicle count as the main variable, a significant positive correlation with the total recruited oocytes was observed. When we correlated the antral follicle count with the recruited follicles larger than 18 mm, we observed that, with a cutoff of 12 antral follicles, there is a positive predictive value of 99%, and an area under the ROC curve of 0.76.
We concluded from our study that age and antral follicle count are effective predictors of ovarian response in cycles of assisted reproduction. The ovarian volume, as well as the anti-Müllerian hormone dosage, seem to be adequate markers of the ovarian reserve.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(11):499-504
DOI 10.1590/S0100-72032012001100004
PURPOSE: To detect the presence of Human Cytomegalovirus (HCMV) and Herpes Simplex Virus type 2 (HSV-2) DNA in cervical samples from women assisted in a primary health care clinic in the city of Coari, Amazonas, Brazil. METHODS: Participated in this study 361 sexually active women between 18 and 78 years. They were been assisted in a Basic Health Care Clinic for routine gynecological exam. The cervical samples were collected using endocervical brush. The viruses were detected using real-time Polymerase Chain Reaction (PCR) technique. RESULTS: Mean age was 36.4 years (standard deviation (SD)=13.4). HCMV DNA was found in cervical samples from 30 women (8.3%; IC95% 5.8 - 11.8) and HSV 2 DNA in 2 women (0.6%; IC95% 0.1 - 2.2). Two women related being HIV positive, one of them infected with HCMV. There were no statistically significant associations between infections by the pathogens studied and socioeconomic, clinical or behavioral variables. CONCLUSIONS: The prevalence of the HCMV infection found in the sample points to the need for screening of the virus during pregnancy and surveillance in immunocompromised patients. The low prevalence of HSV-2 found is probably due to the fact that cervical sampling is not appropriate for this type of study because of the characteristics of viral biology related to neurovirulence.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(8):499-500