Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(8):494-496
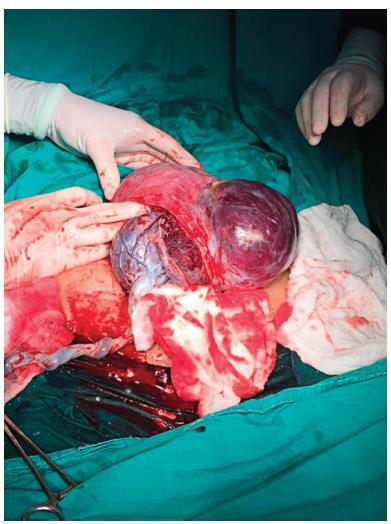
Placenta accreta syndromes are associated with increased maternal mortality and morbidity. Cesarean hysterectomy is usually performed in cases of placenta accreta syndrome. Fertility sparing methods can be applied. In the present study, we report a successful segmental uterine resection method for placenta accreta in the anterior uterine wall in a cesarean section case. A 39-year-old woman underwent an elective cesarean section at 38 + 2 weeks. A placental tissue with an area of 10 cm was observed extending fromthe anterior uterine wall to the serosa, 2 cm above the uterine incision line. The placental tissue was removed with the help of monopolar electrocautery. The uterine incision was continuously sutured. The patient was discharged on the second postoperative day. The placental pathology was reported as placenta accreta. The American College of Obstetricians and Gynecologists (ACOG) generally recommends cesarean section hysterectomy in cases of placenta accreta because removal of placenta associated with significant hemorrhage. Conservative and fertility sparing methods include placenta left in situ, cervical inversion technique and triple-P procedure. There are several studies reporting that segmental uterine resection is performed with and without balloon placement or artery ligation. Segmental uterine resection may be an alternative to cesarean hysterectomy to preserve fertility or to protect the uterus in cases of placenta accreta when there is no placenta previa. received
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(7):494-494
DOI 10.1590/S0100-72032002000700015
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(7):494-494
DOI 10.1590/S0100-72032002000700016
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(11):494-498
DOI 10.1590/S0100-72032012001100003
PURPOSE: To describe trends in prevalence, indicators of care and pregnancy outcomes for women with pre-existing type I or type II diabetes. METHODS: Cohort study of all consecutive singleton pregnancies complicated by pre-existing type I or type II diabetes followed from 2004 to 2011 at a tertiary perinatal care centre (n=194). We collected data from the medical records and described trends in demographics, clinical history, indicators of care before or during pregnancy and glycaemic control. We also studied perinatal outcomes, including gestational age at delivery, mode of delivery, and birthweight. RESULTS: The overall incidence of pregestational diabetes was 4.4 per 1000, with no significant changes throughout the study period. The number of type 2 diabetes cases also remained constant. In 67% of cases delivery occurred after 37 weeks (maximum 80% in 2010 - 11). During this period there was a significant reduction in rates of elective caesarean section (p=0.03) and in the incidence of large infants for gestational age (p=0.04). Indicators of glycaemic control were favorable throughout pregnancy, with no significant trends detected during the study period. However, preconceptional care indicators were substandard, with no significant improvement. CONCLUSIONS: A multidisciplinary approach to diabetic management and obstetric practice contributed to adequate glycaemic control throughout pregnancy and to improved pregnancy outcomes. Preconceptional care remains a key challenge.
Summary
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(9):495-501
DOI 10.1590/S0100-72031998000900002
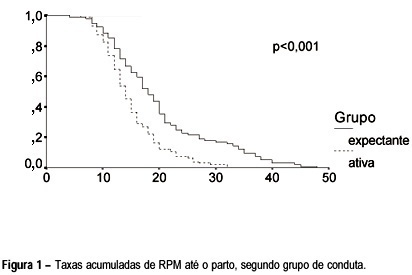
Objective: to compare the expectant versus active management with oxytocin in a Brazilian population of pregnant women with premature rupture of membranes (PROM) at term. Methods: a prospective, randomized and multicenter clinical trial was performed, evaluating variables concerning the time from PROM until the onset of labor and delivery, and maternal and neonatal hospitalization periods. Two hundred pregnant women with PROM at term were selected from four public hospitals in São Paulo state, from November 1995 to February 1997. They were randomly divided into two groups: active management, with oxytocin induction of labor until 6 h of PROM; and expectant management, waiting for the spontaneous onset of labor up to 24 h. The data were analyzed with the Epi-Info and SPSS-PC+ packages, using the statistical c², Student's t and log-rank tests. Results: the results indicate that the differences between the two managements concern to the longer time needed for the expectant management group until onset of labor and delivery, besides the higher number of women and neonates who remained in hospital for more than three days. Conclusions: the time between admission and onset of labor and delivery, and also the latent period were longer in the expectant management group.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(11):495-497
DOI 10.1590/SO100-720320150005473
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(6):495-495