You searched for:"Francisco Herlânio Costa Carvalho"
We found (16) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(6):403-403
DOI 10.1590/S0100-72032001000600010
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(8):446-452
DOI 10.1590/S0100-72032006000800002
PURPOSE: to describe the obstetric outcomes in pregnant adolescents at a tertiary hospital and to compare the maternal and labor outcomes between precocious and late adolescents. METHODS: in a transversal analytical study, 2058 cases were evaluated, considering 322 (15.65%) from the precocious group and 1736 (84.35%) from the late group that delivered at the "Maternidade Escola Assis Chateaubriand/UFC" from January 1, 2000 to December 31, 2000. The clinical complications in the prenatal period, kind of delivery, indications for cesarean section, birth gestational age at birth, birth weight, comparison of birth weight and gestational age, Apgar score at the first and fifth minute, presence of malformations, and neonatal death were analyzed. The exact Fisher and the chi2 tests were used to compare both groups. The prevalence ratio was calculated. RESULTS: from of total of deliveries, 25.95% belonged to adolescents. The average age was 17.19 years. Prenatal visits were made by 88% of the patients, but 60% had an insufficient number of visits. The most frequent clinical situations were preeclampsia (14.72%), anemia (12.97%) and urinary tract infections (6.37%), with no statistical difference between the groups. Thirty-one and three percent of the births were by cesarean section, preeclampsia being the main indication in the two age groups (25 and 23%, respectively). The frequency of an Apgar score less than 7 at the first minute was 19,9% in the precocious adolescent group and 14,2% in the late adolescent group (x²=6,96, p=0.008). There was no statistical difference regarding prematurity rate (20.2 vs 16.1%), low-birth weight infants (12.4 vs 10.4%), low Apgar score at the fifth minute (5.3 vs 3.3%), congenital malformations (3.1 vs 2.7%), and neonatal death (5.3 vs 3.3%). CONCLUSIONS: the precocious and late pregnant adolescents presented similar pregnancy evolution and obstetric outcomes, except for the differences of the first minute Apgar scores.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(7):585-585
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(9):588-592
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(12):594-601
DOI 10.1590/S0100-72032008001200002
PURPOSE: to evaluate factors associated with women's dyslipidemia during menopause. METHODS: case-control study of prevalent cases and controls selected from a dedicated outpatient clinic. From recent biochemical parameters found in patients' files, women have been grouped in 'case' and 'control'. Women who presented any alteration in the blood levels of total cholesterol, LDL-cholesterol, triglycerides and/or HDL-cholesterol were considered as case, and the ones who presented normal levels of them, as control. Data concerning socioeconomic situation, physical activity, etilism and tabagism, anthropometric measurements and food ingestion have been collected and then compared between the groups. Ratios have been compared by the χ2, Fisher's exact test and/or t-Student test, depending on the distribution type. The crude relationship between each factor and the presence of dyslipidemia has been estimated by logistic regression. RESULTS: data have been collected from 84 women aged from 42 to 59 years, as 45 of them were grouped as case (dyslipidemic) and 39 as control (non-dyslipidemic). Age average of cases and controls was 52.1±4.2 and 52.2±4.7 years old, respectively. The sample showed to be homogeneous for the socioeconomic characteristics (income, occupation and schooling), physical activity practice, etilism and tabagism, and food ingestion, with no significant correlation with dyslipidemia. The groups presented an income up to two minimal wages, low schooling level (up to the fourth grade of lower school), and the housewife occupation. Smoking and drinking alcohol was not very frequent. Practicing physical activity was non-existent, thus characterizing a sedentary population. Food ingestion was adequate for carbohydrates, protein, lipids, but not for cholesterol (excessive) and fibers (insufficient), in both groups. Concerning the anthropometric evaluation, there has been an association with dyslipidemia, as the body mass index (BMI) and the waist circumference (WC) were significantly larger in case than in control. The waist-hip ratio has been similar in both groups. Weight excess has been found in most of the cases (73.3%) as almost half of them (44%) presented WC >88 cm, which represents a very increased risk. CONCLUSIONS: it is possible to conclude that, in the studied sample, only the anthropometric measurements have been considered as risk factors associated with dyslipidemia, during post-menopause.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(12):639-646
DOI 10.1590/S0100-72032007001200007
PURPOSE: to compare the effectiveness of low doses of vaginal misoprostol (12.5 versus 25 µg) for induction of labor. METHODS: a double-blind, randomized, controlled clinical trial was performed in Santa Casa de Misericórdia de Sobral, from May 2005 to April 2006. Sixty-two term pregnant women, with intact membranes and with indication for labor induction, were included. They randomly received 25 µg (32) or 12.5 µg (30) of vaginal misoprostol each four hours, until the maximum of eight doses. Mode of delivery, time between induction and delivery, perinatal complications, and maternal side effects were studied. The control variables were maternal and gestational ages, parity and Bishop score. The statistical tests used were average calculations, shunting line-standards and Student t-test (numerical continuous variables), chi2 (categorical variables) and Mann-Whitney test (discrete variables). RESULTS: the two groups, 12.5 and 25 µg, did not differ in relation to the interval of time between the induction onset and delivery (1524 versus 1212 min, p=0.333), in the frequency of vaginal delivery (70 versus 71.8%, p=0.720), Apgar scores below seven at the fifth minute (3,3 versus 6,25%, p=0.533) and tachysystole frequency (3.3 versus 9.3%, p=0.533). The average of total dose administered was significantly higher in the 25 µg group (40 versus 61.2 µg, p=0.03). CONCLUSIONS: vaginal misoprostol in the dose of 12.5 µg was efficient, with collateral effects similar, to the 25 µg of vaginal misoprostol, for induction of labor at term.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(8):641-647
DOI 10.1590/S0100-72032004000800008
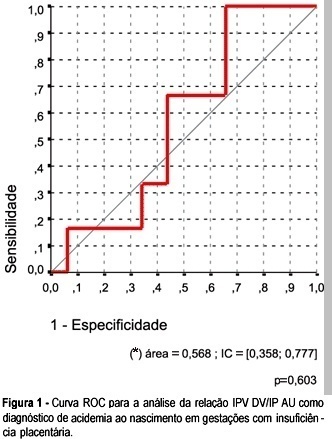
OBJECTIVE: to investigate whether it is possible to predict acidemia at birth in pregnancies with placental insufficiency using venous-arterial indices: pulsatility index for vein (PIV) of the ductus venosus (DV) over PI of the middle cerebral artery (MCA) and PIV of the DV over PI of the umbilical artery, and establish cut-off values for this prediction. PATIENTS AND METHODS: this was a prospective cross-sectional study involving forty-seven patients with placental insufficiency (umbilical artery resistance and pulsatility indices above the 95th percentile for gestational age) who were submitted to Dopplervelocimetry in the last 24 hours before delivery. All pregnancies were singleton, over 26 weeks of age and without structural or chromosome anomalies. Arterial cord blood was obtained for gasometry immediately after birth. Acidemia was defined as umbilical arterial pH < 7.20 in the absence of uterine contractions and pH < 7.15 in the presence of contractions. Metabolic or mixed acidemia at birth were considered pathological. A ROC curve was calculated for the venous-arterial indices: PIV DV/PI umbilical artery (UA) and PIV DV/PI MCA. A cut-off value was established and sensitivity, specificity, accuracy, positive and negative predictive values and positive and negative likelihood ratios were calculated. RESULTS: The DV/UA PI index was not a good predictor of acidemia at birth. The DV/MCA PI index was related to acidemia at birth (area under the curve 0,785, p = 0,004). The cut-off value was: 0,582, sensitivity 66,7%, specificity 77,1 and accuracy 74,5%. CONCLUSION: the PIV DV/PI MCA ratio is adequate for predicting acidemia at birth in pregnancies with placental insufficiency. The cut-off value was: 0,582.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(2):74-80
To evaluate the impact of the presence of criteria for severe maternal morbidity and maternal near miss associated with hypertensive disorders on maternal and perinatal outcomes in a maternity school.
The present is a sub-analysis of a larger study involving 27 centers in Brazil that estimated the prevalence of serious maternal morbidity and near miss. It is an analytical and cross-sectional study with a quantitative approach, involving 928 women who were cared for at Maternidade Escola Assis Chateaubriand (MEAC, in Portuguese), Universidade Federal do Ceará (UFC, in Portuguese), from July 2009 to June 2010. The women were diagnosed with near miss according to the World Health Organization (WHO) criteria. The sample was divided into 2 groups: patients with (n = 827) and without hypertension (n = 101). The results were considered statistically significant when p < 0.05. The Pearson chi-squared and Fisher Exact tests were used for the categorical variables, and the Mann–Whitney U test was used for the continuous variables.
In total, 51 participants with maternal near miss criteria were identified, and 36 of them had hypertensive disorders. Of these, 5 died and were obviously excluded from the near miss final group. In contrast, we observed 867 cases with non-near miss maternal morbidity criteria. During this period, there were 4,617 live births (LBs) in the institution that was studied.
In the severe morbidity/maternal near miss population, the presence of hypertensive complications was prevalent, constituting a risk factor for both the mother and the fetus.