You searched for:"César Eduardo Fernandes"
We found (22) results for your search.Summary
Rev Bras Ginecol Obstet. 2000;22(1):37-41
DOI 10.1590/S0100-72032000000100007
Purpose: to evaluate the effects of tibolone on climacteric symptoms and clinical and metabolic variables. Methods: thirty-four postmenopausal women were treated orally with 2.5 mg tibolone daily for 48 weeks and evaluated as to climacteric complaints, clinical aspects such as weight and blood pressure and lipid profile (total cholesterol, HDL-c, LDL-c, VLDL-c and triglycerides). Results: a significant improvement of climacteric complaints was demonstrated by a significant decrease in the Kupperman index (p<0.001) and the mean number of hot flushes (p<0.001) from the first month of treatment onwards. There was a significant decrease in total cholesterol, triglycerides and VLDL-c (p<0.001). The LDL-c levels presented a slight decrease (not significant). The HDL-c levels showed a significant decrease at week 24. However these levels returned to baseline levels at week 48. With regard to the vital signs no change in body weight and blood pressure was measured. The side effects were mild and temporary, vaginal bleeding, nausea and edema being the most common. Conclusion: tibolone may be considered a safe and efficient option to treat climacteric symptoms in postmenopausal women without significant impact on lipid profile.
Summary
Rev Bras Ginecol Obstet. 2020;42(7):411-414
Summary
Rev Bras Ginecol Obstet. 2021;43(6):425-428
Summary
Rev Bras Ginecol Obstet. 2020;42(1):43-50
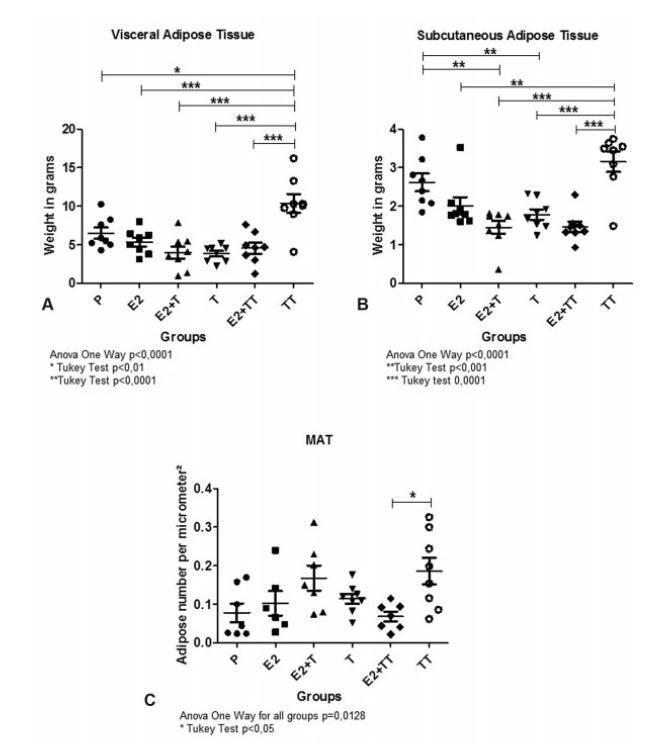
The present article aims to evaluate the impact of testosterone treatment on the expansion of visceral, subcutaneous and intramedullary adipose tissue of ovariectomized rats and the visceral and subcutaneous fat expression of peroxisome proliferator-activated receptors (PPARs) gamma.
In total 48 female Wistar rats were castrated and randomly divided into 6 treatment groups: group E2 was submitted to estradiol 5 μg/day; group T, to testosterone 5 μg/day; group E2+ T, to estradiol 5 μg/day + testosterone 5 μg/day; group TT, to testosterone 30 μg/day; group E2+ TT, to estradiol 5 μg/day+ testosterone 30 μg/day; and placebo was administered to group P. After 5 weeks, the rats were euthanized, the inguinal and visceral adipose tissues were harvested, weighted, and had their PPAR gamma expression evaluated by reverse transcription quantitative polymerase chain reaction (RTqPCR). The right femurs were harvested and histologically prepared to performthe number count of the intramedullary adipocytes.
The expansion of visceral fat tissue was much higher in the TT group when compared with other treated groups (p < 0.001). The TT group also showed a higher expansion of inguinal fat (p < 0.01), and groups E2 +T and E2+ TT presented lower growth compared to the P group (p < 0.01). The number of femur intramedullary adipocytes only showed significant differences between groups TT and E2 + TT (p < 0.05). The expression of PPAR gamma showed no differences among the groups.
The use of testosterone in high doses leads to an important expansion in both visceral and inguinal adipose tissues. Association with estradiol exerts an expansion-repressive effect on the visceral and inguinal adipose tissues.
Summary
Rev Bras Ginecol Obstet. 2019;41(7):449-453
To analyze the effects of estrogen alone or in combination with progestogens and tibolone (TIB) on the expression of the extracellular matrix metalloproteinases 2 and 9 (MMP-2 and MMP-9), of perlecan, and of heparanase (HPSE) of the vascular walls of the carotid arteries.
A total of 30 250-day-old ovariectomized Wistar rats were orally treated for 5 weeks with: a) 1 mg/kg of estradiol benzoate (EB); b) EB + 0.2 mg/kg of medroxyprogesterone acetate (MPA); c) EB + 0.2mg/kg of norethisterone acetate (NETA); d) EB + 2 mg/kg of dydrogesterone (DI); e) 1 mg/kg of TIB; f) placebo (CTR). Following treatment, the expression of mRNA for MMP-2, MMP-9, and HPSE was analyzed by realtime polymerase chain-reaction (PCR), and the expression of MMP-2, of MMP-9, of tissue inhibitor of metalloproteinase 2 (TIMP-2), and of perlecan was quantified by immunohistochemistry in the carotid arteries.
The groups showed significant differences on mRNA HPSE expression (p = 0.048), which was higher in the EB, EB + MPA, and TIB groups. There was no statistically significant difference in mRNA MMP-2 or MMP-9 expression. The immunohistochemical expression of MMP-2, of TIMP-2, of MMP-9, of HPSE, and of perlecan showed no differences between groups.
Estradiol alone or associated with MPA and TIB treatment can increase mRNA HSPE expression of the walls of the carotid arteries in ovariectomized rats.
Summary
Rev Bras Ginecol Obstet. 2019;41(8):476-484
Labor induction does not always result in vaginal delivery, and can expose both the mother and the fetus to the risks inherent to the induction procedure or a possible cesarean section. Transvaginal sonography (TVS) of the cervix is a useful tool to predict prematurity; in the present study, this tool was used to evaluate postterm induction.
We evaluated the ultrasound characteristics of the cervix (cervical length, cervical funneling, internal os dilation, the presence or absence of the cervical gland area [CGA], and the morphological changes of the cervix as a result of applying fundal pressure) before the onset of labor induction among women with postterm pregnancy to identify the possible predictors of failed labor induction. The Bishop score (BS) was used for comparison purposes. Three groups were evaluated: successful versus unsuccessful induction; vaginal delivery versus cesarean delivery (excluding cases of acute fetal distress [AFD]); and vaginal delivery versus cesarean delivery (including cases of AFD). A fourth group including only the primiparous women from the three previous groups was also evaluated.
Based on the studied characteristics and combinations of variables, a cervical length ≥ 3.0 cm and a BS ≤ 2 were the best predictors of induction failure.
Although TVS is useful for screening for induction failure, this tool should not be used as an indication for cesarean section.
Summary
Rev Bras Ginecol Obstet. 2022;44(5):497-502
Construction and validation of the WhatsApp Stress Scale (WASS), a questionnaire designed for physicians that measures how the use of smartphones and related software communication applications affects the quality of life of gynecologists who use this tool to communicate with patients.
The present cross-sectional observational study analyzed 60 gynecologists according to weekly WhatsApp usage time for communication with patients and compared the data with the perception of the doctor on the use of this virtual interaction as a stressor. Physicians were equally divided into three groups:<2hours, 2 to 5 hours, and>5 hours. The authors created a questionnaire in Likert scale format. The study proceeded in three phases: development of the questionnaire items, pretesting, constructing, and validity and reliability testing using factor analysis, Cronbach α coefficient, and paired t-test.
A 9-item instrument using a 5-point Likert scale was created and administered to the participants in 3 different times: T0, T1 (15minutes after the end of T0), and T2 (15 days later). All questionnaire items possessed adequate content validity indices and the internal consistency of the instrument was satisfactory (Cronbach α 0.935; 95% confidence interval [CI]: 0.744-0.989; p=0.0001). No statistically significant differences were observed in the responses between the rounds of testing, indicating good test-retest reliability. A positive association between the high frequency of WhatsApp usage for communication with patients and the stress perceived by the doctor was shown.
The WASS is a valid and reliable instrument for assessing the use of messaging applications to communicate with patients as a stressor perceived by gynecologists.