You searched for:"Antônio Alberto Nogueira"
We found (31) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(1):31-35
DOI 10.1590/S0100-72032008000100006
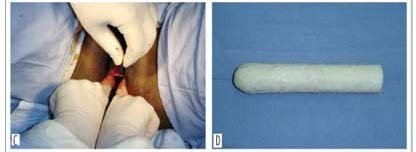
PURPOSE: to evaluate the use of natural latex mold (Hevea brasiliensis) as a modification of McIndoe and Bannister neovaginoplasty in patients presenting Mayer-Rokitansky-Küster-Hauser (MKRH) syndrome. METHODS: we retrospectively included nine patients presenting MKRH syndrome, who had been submitted to McIndoe and Bannister neovaginoplasty modified by the use of natural latex mold. Neovaginal epithelization and depth, coitus occurrence and satisfaction, and surgical complications were evaluated. RESULTS: five weeks after the procedure, eight patients presented an epithelized 7 to 12 cm deep neovagina. There was one case of complete neovaginal stenosis, because of incorrect use of the mold. After at least one year, the others maintained 4 to 8 cm deep neovaginas and capacity for intercourse, with 66.7% satisfaction. One woman presented precocious rectovaginal fistula and late episodes of uretrovaginal fistulae. Two patients presented distal neovaginal stenosis in long-term follow-up. One of these and the patient with fistulae were submitted to a new procedure. CONCLUSIONS: the use of natural latex mold as a modification of classic neovaginoplasty technique allows the creation of neovaginas morphologically and functionally similar to the normal vagina in patients with vaginal agenesis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2011;33(11):323-327
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):401-406
DOI 10.1590/S0100-72032005000700006
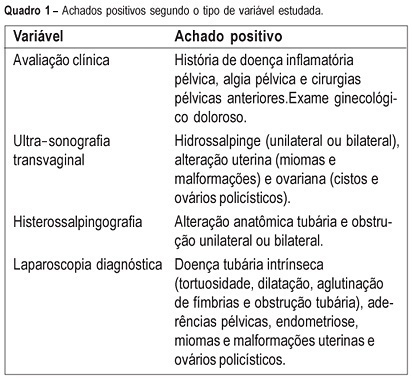
PURPOSE: to evaluate the agreement between noninvasive methods - pelvic pain, transvaginal ultrasound and hysterosalpingography - and the gynecologic endoscopy approach for the diagnosis of tuboperitoneal factors responsible for conjugal infertility. METHODS: this is a cross-sectional study including 149 infertile patients who were submitted to clinical evaluation, transvaginal ultrasound, hysterosalpingography, hysteroscopy, and laparoscopy. In the evaluation of pelvic pain, the following complaints were considered to be abnormal: pelvic pain of the dyspareunia type, dysmenorrhea or acyclic pain, and pain upon mobilization of the cervix and palpation of the adnexa. Ultrasonographic examination was considered to be altered when adnexal or uterine morphological changes (hydrosalpinx, myomas or uterine malformations) were detected. Hysterosalpingography was considered to be abnormal in the presence of anatomical tubal changes and unilateral or bilateral obstruction. The agreement between noninvasive methods and endoscopy was evaluated by kappa statistics. RESULTS: the agreements between pelvic pain, transvaginal ultrasound, and hysterosalpingography and the endoscopic approach were 46.3% (kappa=0.092; CI 95%: -0.043 to 0.228), 24% (kappa=-0.052; CI 95%: -0.148 to 0.043), and 46% (kappa=0.092; CI 95%: -0.043 to 0.228), respectively. When at least one alteration detected by noninvasive methods was considered, the agreement with endoscopic approach was 63% (kappa=-0.014; CI 95%: -0.227 to 0.199). Sensitivity and specificity in predicting alterations on endoscopic approach were 39.5 and 80% in the presence of pelvic pain, 14.5 and 72% in the presence of alteration on transvaginal ultrasound, 39.5 and 80% in the presence of alteration on hysterosalpingography, and 70.2 and 28% in the presence of at least one alteration by noninvasive methods. CONCLUSION: there is a poor diagnostic agreement between the several noninvasive methods and endoscopy in the investigation of conjugal infertility secondary to tuboperitoneal factors.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2009;31(9):425-426
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(9):443-449
to translate and adapt the Patient Satisfaction Questionnaire (PSQ) to Portuguese and to assess its psychometric properties based on internal consistency, test-retest, factor analysis and divergent and convergent construct validities.
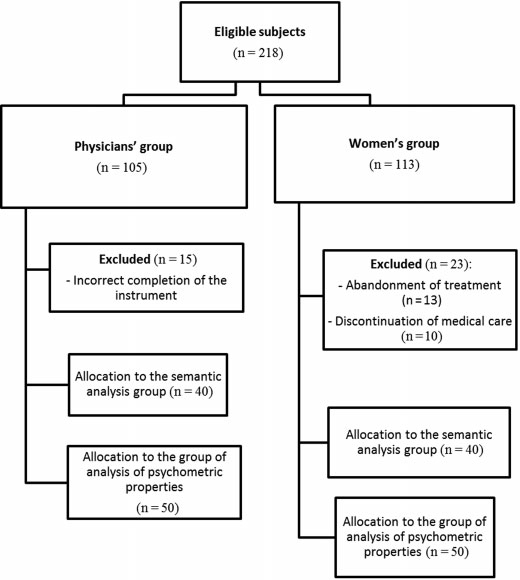
The study involved 218 participants and was approved by the local Research Ethics Committee. All participants gave written informed consent and their anonymity was ensured. The instrument was translated and culturally adapted for use in the Portuguese language. The internal consistency and factorial analysis were assessed by patients and physicians. Convergent and divergent validities were also assessed specifically for the patient group, as well as test-retest reliability. The Portuguese versions of the Patient Health Questionnaire (PHQ-9) and State-Trait Anxiety Inventory (STAI) were used for the analysis of the convergent validity. In addition, we applied a questionnaire of clinical and demographic data for the analysis of the divergent validity.
The adapted version of the PSQ showed good Cronbach’s α and test-retest values, and the results of the convergent construct validity between the PSQ and the PHQ-9 (r = 0.34; p = 0.02) and the STAI (r = 0.47; p = 0.001) were negative, significant and moderate correlations. Divergent validity showed significant correlations only with race and education. The Brazilian Portuguese versionof the PSQ proved to be a valid and reliable instrument, with psychometric properties suitable for the assessment of satisfaction among patients with chronic pelvic pain and their physicians in Brazil. The questionnairemay allow the homogenization of reports on this topic in the international literature.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(1):47-52
Patient autonomy has great importance for a valid informed consent in clinical practice. Our objectives were to quantify thedomains of patient autonomy and to evaluate the variables that can affect patient autonomy in women with chronic pelvic pain.
This study is a cross sectional survey performed in a tertiary care University Hospital. Fifty-two consecutive women scheduled for laparoscopic management of chronic pelvic were included. Three major components of autonomy (competence, information or freedom) were evaluated using a Likert scale with 24 validated affirmatives.
Competence scores (0.85 vs 0.92; p = 0.006) and information scores (0.90 vs 0.93; p = 0.02) were low for women with less than eight years of school attendance. Information scores were low in the presence of anxiety (0.91 vs 0.93; p = 0.05) or depression (0.90 vs 0.93; p = 0.01).
Our data show that systematic evaluation of patient autonomy can provide clinical relevant information in gynecology. Low educational level, anxiety and depression might reduce the patient autonomy in women with chronic pelvic pain.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(1):47-54
DOI 10.1590/S0100-72031999000100008
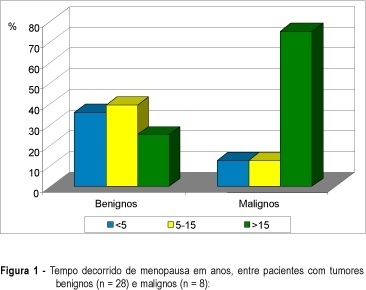
Purpose: to evaluate clinical and ultrasonic findings in patients with pelvic tumors at postmenopause and to correlate them with the final diagnosis. Patients and Methods: thirty-six postmenopausal women with pelvic tumor diagnosis were prospectively evaluated through clinical examination and endovaginal ultrasonography. Clinical follow-up with no surgical procedures was indicated for anechoic cystic tumors with or without thin unique septation and volume under 50 cm³. Needle aspiration was indicated for tumors with the same aspect, and volume of 50 to 100 cm³, whereas exploratory laparotomy was performed in the remaining patients. Diagnosis defined two groups of patients: benign (28) and malignant (8) pathologies. Results: anechoic cystic tumor with or without a thin septum indicates benignity (p = 0.0091). Tumors with solid areas indicate malignancy (p = 0.0024). Ascites correlates with malignancy (p = 0.0278). Heterogeneity, thick capsule, thick septa, and papillary projections predominated in malignancies but without no statistical significance (p > 0,05). Tumor volume indicates malignancy, with a median of 85.2 cm³ in benign tumors and 452.5 cm³ in malignancies (p = 0.0048), with a cutoff at 295 cm³ (sensitivity = 83.3% and specificity = 85.2%). Following this protocol, all malignancies were submitted to surgery and 11 benign tumor patients were treated with a conservative protocol (39.3% of all benign patients). Conclusion: conservative management is an adequate protocol for women with anechoic pelvic tumors with low volume, with or without single thin septum and without ascites. Differentiation between benign and malignant of complex and/or high volume tumors requires complementary investigation.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(7):471-477
DOI 10.1590/S0100-72032002000700007
Purpose: to assess the diagnostic and therapeutic aspects and the complications of symptomatic urinary tract infections (UTI) during pregnancy of patients who were hospitalized. Methods: a total of 136 pregnant women with a clinical diagnosis of pyelonephritis were studied. The studied parameters were: age and parity of patients, gestational age of diagnosis, epidemiologic aspects, laboratory evaluation for UTI, treatment and clinic evolution, prophylaxis and complications. Results: pyelonephritis was diagnosed at the same proportions at all gestational ages. The incidence of UTI was higher among primigravidae. Only 29.3% of the pregnant women had a previous history of UTI; 57.0% were anemic and 93.0% had altered urinalysis. Escherichia coli was the most prevalent uropathogen (75.8% of cases), with low percentages of sensitivity to ampicillin (60.6%) and high percentages of sensitivity to cefuroxime (95,5%). The highest rate of clinical improvement was obtained for the pregnant women treated with cefuroxime (95.7%). Prophylaxis was needed in 11.0% of the patients. Preterm labor occurred in 33.3% of the pregnant women who delivered in our service and preterm delivery occurred in 18.9%. Conclusions: the present results support the need for an early diagnosis and effective treatment of UTI in pregnant women in order to prevent the frequent occurrence of perinatal complications such as premature labor and delivery. We emphasize the need of a periodical evaluation of the pattern of sensitivity of the etiologic agents to the antimicrobials allowed for use during pregnancy, with cefuroxime being adopted as the antibiotic of choice for the treatment of UTI during pregnancy.